Use of Plane X-Ray for Nonoperative Treatment of Intussusception at Resource Limited Settings in Low-and Middle-Income Countries
Article Information
Md. Qumrul Ahsan1,2, Tanvir Kabir Chowdhury3*, Tasmiah Tahera Aziz4, Tahmina Banu4
1Department of Radiology and Imaging, Chattogram Maa- O-Shishu Hospital Medical College, Chattogram, Bangladesh
2Radiology and Imaging, Centre for Specialized Care and Research (CSCR), Chattogram, Bangladesh
3Department of Pediatric Surgery, Chittagong Medical College, Chattogram, Bangladesh
4Chittagong Research Institute for Children Surgery (CRICS), Chattogram, Bangladesh
*Corresponding Author: Dr. Tanvir Kabir Chowdhury, Assistant Professor, Department of Pediatric Surgery, Chittagong Medical College 1, KB Fazlul Kader road, Chattogram 4203, Bangladesh
Received: 11 March 2021; Accepted: 22 March 2021; Published: 25 March 2021
Citation: Md. Qumrul Ahsan, Tanvir Kabir Chowdhury, Tasmiah Tahera Aziz, Tahmina Banu. Use of Plane X-Ray for Nonoperative Treatment of Intussusception at Resource Limited Settings in Low-and Middle-Income Countries. Journal of Radiology and Clinical Imaging 4 (2021): 015-026.
View / Download Pdf Share at FacebookAbstract
Objective: To report an easy and feasible technique of hydrostatic reduction of intussusception using plane x-ray in resource limited setting and summarize the radiological findings.
Method: Records of all patients of hydrostatic reduction between May 2015 and April 2020 were retrospectively evaluated to document patient demography, seasonal variations, type of intussusception, duration of procedure, number of x-ray exposures, reflux of contrast through ileocecal valve, location of intussusception mass, presence of redundant colon and outcome. Hydrostatic reduction was performed with water soluble contrast using intermittent shots of plane x-ray, instead of ultrasound (US) or fluoroscopy guidance.
Results: Among a total of 204 patients, male to female ratio was 1.7:1. Age ranged from 5 days to 16 years (median 10 months). There were more cases during Winter and Spring (110, 53.9%). Right hepatic flexure was the commonest (115, 56.4%) site of obstruction. Hydrostatic reduction was successful in 172 (84.3%) patients. Median duration of the procedure was 27 minutes and, on an average, 8.4 ± 1.7 exposures were needed for one hydrostatic reduction. There was no significant relation of age group and sex with successful hydrostatic reduction but site of obstruction was significantly related with success (p=0.00). There was one (0.5%) recurrence and no mortality.
Conclusion: Hydrostatic reduction using contrast enema under x-ray guidance is a rational alternative to US or fluoroscopy guided reduction in resource limited settings.
Keywords
<p>Intussusception; Non-operative management; Hydrostatic reduction; Contrast; X-ray; Low-and middle-income countries</p>
Intussusception articles; Non-operative management articles; Hydrostatic reduction articles; Contrast articles; X-ray articles; Low-and middle-income countries articles
Intussusception articles Intussusception Research articles Intussusception review articles Intussusception PubMed articles Intussusception PubMed Central articles Intussusception 2023 articles Intussusception 2024 articles Intussusception Scopus articles Intussusception impact factor journals Intussusception Scopus journals Intussusception PubMed journals Intussusception medical journals Intussusception free journals Intussusception best journals Intussusception top journals Intussusception free medical journals Intussusception famous journals Intussusception Google Scholar indexed journals Non-operative management articles Non-operative management Research articles Non-operative management review articles Non-operative management PubMed articles Non-operative management PubMed Central articles Non-operative management 2023 articles Non-operative management 2024 articles Non-operative management Scopus articles Non-operative management impact factor journals Non-operative management Scopus journals Non-operative management PubMed journals Non-operative management medical journals Non-operative management free journals Non-operative management best journals Non-operative management top journals Non-operative management free medical journals Non-operative management famous journals Non-operative management Google Scholar indexed journals Hydrostatic reduction articles Hydrostatic reduction Research articles Hydrostatic reduction review articles Hydrostatic reduction PubMed articles Hydrostatic reduction PubMed Central articles Hydrostatic reduction 2023 articles Hydrostatic reduction 2024 articles Hydrostatic reduction Scopus articles Hydrostatic reduction impact factor journals Hydrostatic reduction Scopus journals Hydrostatic reduction PubMed journals Hydrostatic reduction medical journals Hydrostatic reduction free journals Hydrostatic reduction best journals Hydrostatic reduction top journals Hydrostatic reduction free medical journals Hydrostatic reduction famous journals Hydrostatic reduction Google Scholar indexed journals Low-and middle-income countries articles Low-and middle-income countries Research articles Low-and middle-income countries review articles Low-and middle-income countries PubMed articles Low-and middle-income countries PubMed Central articles Low-and middle-income countries 2023 articles Low-and middle-income countries 2024 articles Low-and middle-income countries Scopus articles Low-and middle-income countries impact factor journals Low-and middle-income countries Scopus journals Low-and middle-income countries PubMed journals Low-and middle-income countries medical journals Low-and middle-income countries free journals Low-and middle-income countries best journals Low-and middle-income countries top journals Low-and middle-income countries free medical journals Low-and middle-income countries famous journals Low-and middle-income countries Google Scholar indexed journals X-ray articles X-ray Research articles X-ray review articles X-ray PubMed articles X-ray PubMed Central articles X-ray 2023 articles X-ray 2024 articles X-ray Scopus articles X-ray impact factor journals X-ray Scopus journals X-ray PubMed journals X-ray medical journals X-ray free journals X-ray best journals X-ray top journals X-ray free medical journals X-ray famous journals X-ray Google Scholar indexed journals Contrast articles Contrast Research articles Contrast review articles Contrast PubMed articles Contrast PubMed Central articles Contrast 2023 articles Contrast 2024 articles Contrast Scopus articles Contrast impact factor journals Contrast Scopus journals Contrast PubMed journals Contrast medical journals Contrast free journals Contrast best journals Contrast top journals Contrast free medical journals Contrast famous journals Contrast Google Scholar indexed journals ultrasound articles ultrasound Research articles ultrasound review articles ultrasound PubMed articles ultrasound PubMed Central articles ultrasound 2023 articles ultrasound 2024 articles ultrasound Scopus articles ultrasound impact factor journals ultrasound Scopus journals ultrasound PubMed journals ultrasound medical journals ultrasound free journals ultrasound best journals ultrasound top journals ultrasound free medical journals ultrasound famous journals ultrasound Google Scholar indexed journals demography articles demography Research articles demography review articles demography PubMed articles demography PubMed Central articles demography 2023 articles demography 2024 articles demography Scopus articles demography impact factor journals demography Scopus journals demography PubMed journals demography medical journals demography free journals demography best journals demography top journals demography free medical journals demography famous journals demography Google Scholar indexed journals Ultrasonography articles Ultrasonography Research articles Ultrasonography review articles Ultrasonography PubMed articles Ultrasonography PubMed Central articles Ultrasonography 2023 articles Ultrasonography 2024 articles Ultrasonography Scopus articles Ultrasonography impact factor journals Ultrasonography Scopus journals Ultrasonography PubMed journals Ultrasonography medical journals Ultrasonography free journals Ultrasonography best journals Ultrasonography top journals Ultrasonography free medical journals Ultrasonography famous journals Ultrasonography Google Scholar indexed journals radiographers articles radiographers Research articles radiographers review articles radiographers PubMed articles radiographers PubMed Central articles radiographers 2023 articles radiographers 2024 articles radiographers Scopus articles radiographers impact factor journals radiographers Scopus journals radiographers PubMed journals radiographers medical journals radiographers free journals radiographers best journals radiographers top journals radiographers free medical journals radiographers famous journals radiographers Google Scholar indexed journals
Article Details
1. Introduction
Intussusception, first described by Barbette in 1674, is the invagination or telescoping of one segment (intussusceptum) into the adjacent segment (intussuscipiens) of intestine [1]. Now-a-days, various non-operative treatment options are available in the world for reduction of intussusception which includes fluoroscopy guided reduction. A recent survey among pediatric radiologists of North America reported that fluoroscopy is used by 96% and 4% used US guidance for reduction; 78% used air enema and 20% preferred liquid enema to reduce intussusception [2]. However, in many low-and middle-income countries (LMICs) non-operative treatment of intussusception is not practiced widely and many patients with intussusception undergo surgery even if they present early. As many as 95% to 100% of patients in some centers underwent surgical treatment for intussusception in these countries [3-8]. Various factors hinder the establishment of non-operative treatment. Ultrasonography (USG) and fluoroscopy are not widely available in the rural hospitals and also in many district hospitals. On the other hand, plane radiography is widely available. A recent long-term study from a tertiary level government referral center in Chattogram, Bangladesh reported successful hydrostatic reduction with contrast under plane radiography guidance [9]. The objectives of the current study are to describe the procedure in a greater detail for the radiologists and radiographers, analyze the radiographic findings and report the outcome at a private investigation center, where majority of the procedures of the earlier study were performed along with patients from other centers. It is expected that finding of the study will encourage centers in the LMICs with resource limited settings to perform more non-operative treatment of intussusception in the absences of traditional well-established methods.
2. Methods and Materials
2.1 Study design
We retrospectively reviewed records of all patients of intussusception who were referred to principal author’s institute for hydrostatic reduction between May, 2015 and April, 2020 (5 years) from different government and private hospitals in and around Chattogram city. Patients in whom presence of intussusception was confirmed by USG and who presented within 3 days of onset of symptoms and did not have any features of peritonitis, gut perforation, severe dehydration or sepsis were selected for hydrostatic reduction. Patients in whom hydrostatic reduction was attempted were included in the study. The risks and benefits of the procedure were explained to the parents and informed consent was obtained. Patient demography, seasonal variations, diagnosis, type of intussusception, duration of procedure, number of x-ray exposures, reflux of contrast through ileocecal valve, outcome, location of intussusception mass, presence or absence of redundant colon, complications, recurrence and mortality were analyzed. The total cost of a single procedure was also assessed.
2.2 Hydrostatic reduction technique
The child was placed on an X-ray table in left lateral position. A well lubricated Foley’s catheter of appropriate size (10 to 18 F) was inserted into the rectum for up to 8-9 cm, and the balloon was gently inflated by 10-20 ml of distilled water. The catheter was clamped and both the buttocks were strapped to prevent leakage of contrast. Patient’s attendants were allowed to hold the buttock and body for immobilization which also helped to reduce apprehension of the child and anxiety of the parents. It also reduced x-ray exposure to radiation workers. 50 ml of non-ionic water-soluble contrast (Iohexol) mixed with 200 ml of normal saline warmed to body temperature was taken in a kidney tray. Then 50 ml of the solution was slowly injected into the rectum through the Foley catheter by a 50-ml syringe such as done during performing contrast enema study of large gut. First exposure was taken for preliminary assessment and to locate the position and site of obstruction by the intussusception mass. Then another 100 ml of contrast mixed solution was inserted into rectum in 2 sessions by a 50 ml syringe with gentle pressure if no resistance was felt. The intussusceptum was usually pushed back towards caecum with this gentle pressure of the solution. The progress of the reduction was observed by another exposure at this time. If the location of contrast had reached up to caecum or at the level of ileo-cecal junction, some contrast solution was withdrawn and gently pushed back several times by the 50 ml syringe through the Foleys catheter. Sometimes, additional 20 ml contrast was given per session depending on progress of reduction at 10-15 minutes interval.
The progress of reduction of intussusception was observed by taking interval spot films and about 200-400 ml contrast mixed solution was required depending on the length of large gut and redundancy of the colon. The criteria for successful reduction were disappearance of the intussusception mass, presence of radio-opaque contrast in the terminal ileum and coming out of yellowish fecal matter in the syringe during withdrawal of the solution. In our observation, the babies had typical cry after arrival in the hospital and during the procedure; but when obstruction was released, the patients became quiet and got into deep sleep on the table. From these x-ray exposures, position of the cecum, redundancy of colon, occurrence of perforation during procedure were also recorded. The procedure was abandoned and the patient was sent for surgery whenever there was back pressure or feel of tightness during insertion of contrast and if the mass failed to progress. After successful reduction the parents were advised to stay in hospital for at least 24 hours for observation. The dose of radiation in a nonionic contrast enema procedure without fluoroscopy is 7 mSv [10, 11]. The FDA lethal dose is 50 mSv. The dose of radiation was reduced by using modern digital equipment and age-specific scanning protocol [12].
2.3 Statistical analysis
Compiled data were coded in unique alphanumeric codes for each variable and subjected to statistical analysis using SPSS version 22. Categorical variables were described as frequency and percentage and continuous variables were expressed as median or mean ± standard deviation. The relation of age, sex, site of obstruction, redundancy of colon, number of x-ray exposures were analyzed using Chi-square or Fisher’s Exact test as appropriate. Difference in age and duration of procedure between patients with or without successful hydrostatic reduction and duration of procedure between obstruction “proximal to transverse colon (TC)” vs “TC and distally” were analyzed using Mann-Whitney U test. P value of less than 0.05 was considered significant. Seasonal variations were analyzed based on Northern Meteorological Seasons which are Winter (December to February), Spring (March to May), Summer (June to August) and Fall (September to November) [13].
3. Results
During this period, hydrostatic reduction was attempted in a total of 204 patients. Among them, 129 were male and 75 were female (ratio 1.72:1). Age ranged from 5 days to 16 years (median 10 months; mean age 17.0 ± 19.5 months). Majority of the patients (93, 45.59%) were between 6 and 12 months of age (Figure 1). Mild seasonal variation was noticed among the patients and a slightly larger number of patients presented during Winter and Spring (Figure 2).
Hydrostatic reduction was successfully performed in 172 (84.3%) patients and it failed in 32 (15.7%) patients. Median duration of the procedure was 27 minutes (mean 32 ± 11 minutes, range 5 to 92 minutes). Median duration in successful reduction was 26.5 minutes and in failed reduction 37 minutes (p=0.11). Among the patients who had failed reduction, more time was spent in cases with obstruction “proximal to TC” (median 40.5 minutes) than in “TC and distally” (median 26 minutes). On the other hand, time consumption in cases of successful reduction were similar between cases with obstruction “proximal to TC” and “TC and distally” (median 27 minutes in both). On an average, 8.4 ± 1.7 exposures were needed for one hydrostatic reduction (range 4 to 14, median 8). Majority of the patients (170, 83.3%) needed 6-10 exposures; 28 (13.8%) needed 11-15 exposures, and 6 (2.9%) needed 1-5 exposures. Number of exposures were similar in both successful and failed reduction (median 8); and also, in obstruction “proximal to TC” and “TC and distally” (median 8). All the patients had ileo-colic intussusception and reflux of contrast through ileo-cecal valve was noticed during reduction in 124 (60.8%) patients. In 48 (23.5%) patients, contrast did not reach ileum, but the mass disappeared and the patient passed stool and became clinically well. There was no case of perforation of gut and there was no mortality. There was one (0.5%) case of recurrence in a 14-month-old girl 6 days after initial successful hydrostatic reduction. She was again managed by hydrostatic reduction. The first reduction required 19 minutes and the second reduction required 17 minutes. She had redundant sigmoid colon and the sigmoid colon was extended up to left hypochondriac region.
Right hepatic flexure was the commonest (115, 56.37%) site of obstruction, followed by TC (39, 19.12%) (Table 1). There was redundancy of colon in 192 (94.1%) patients in this series. Most of them had redundancy of sigmoid colon. There were redundant ascending, transverse and descending colon in 4, 1, and 1 patient, respectively. There was no significant difference in redundancy of colon between patients with or without failed hydrostatic reduction (94.8% vs 90.6%, respectively, p=0.36). There were no significant relations of age group and sex with the success of hydrostatic reduction. However, patient who underwent successful hydrostatic reduction had higher median age than patients with failed reduction (10 months vs 7 months, p=0.02). Site of obstruction was significantly related with success (p=0.00, Table 1). Among 5 patients with level of obstruction at the descending colon, none had successful reduction and among 5 with obstruction at splenic flexure, 2 had failed reduction.
There were many variations of the position of the sigmoid colon noticed during hydrostatic reduction in patients with intussusception. In 50 (24.51%) patients, the curvature of the sigmoid colon was noticed in the umbilical region and in 40 (19.61%) patients it extended to the right lumber region through the right iliac fossa (Table 2). The traditionally described pelvic location was found in 73 (35.8%) children. The total cost of a single procedure was about taka 6000 (71 USD), including the accessories -100 ml contrast: 2300 BDT (27 USD), one Foley catheter of 22G: 120 BDT (1.4 USD), two 50 ml syringe: 50 BDT (0.6 USD), 500 ml normal saline: 65 BDT (0.8 USD), 1 pair of gloves: 60 BDT (0.7 USD), one Lidocaine jelly: 95 BDT (1.1 USD), one toilet tissue: 20 BDT (0.2 USD), private hospital service charge: 3290 BDT (38.7 USD).
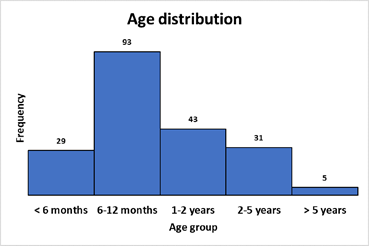
Figure 1: Age distribution of patients with intussusception (N=204).
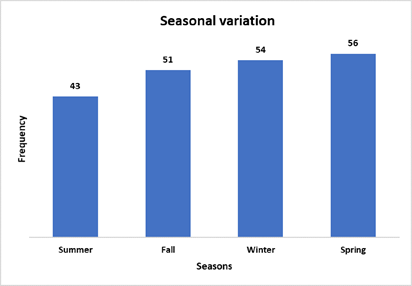
Figure 2: Seasonal variation among patients (N=204).
|
Hydrostatic reduction |
Successful |
Failed |
Total |
% of total patients (N=204) |
Success rate |
p value |
|
Age group |
0.11 |
|||||
|
<6 months |
20 |
9 |
29 |
14.2 |
69.0 |
|
|
6-12 months |
79 |
14 |
93 |
45.6 |
85.0 |
|
|
1-2 years |
37 |
6 |
43 |
21.1 |
86.1 |
|
|
2-5 years |
29 |
2 |
31 |
15.2 |
93.6 |
|
|
>5 years |
5 |
0 |
5 |
2.5 |
100.0 |
|
|
Not available |
2 |
1 |
3 |
1.5 |
66.7 |
|
|
Sex |
0.18 |
|||||
|
Male |
106 |
23 |
129 |
63.2 |
82.2 |
|
|
Female |
66 |
9 |
75 |
36.8 |
88.0 |
|
|
Site of obstruction |
0.00 |
|||||
|
Ileo-cecal junction |
3 |
0 |
3 |
1.5 |
100.0 |
|
|
caecum |
2 |
0 |
2 |
1.0 |
100.0 |
|
|
Ascending colon |
32 |
2 |
34 |
16.7 |
94.1 |
|
|
Rt. hepatic flexure |
99 |
16 |
115 |
56.7 |
86.1 |
|
|
Transverse colon |
32 |
7 |
39 |
19.1 |
82.1 |
|
|
Splenic flexure |
3 |
2 |
5 |
2.5 |
60.0 |
|
|
Descending colon |
0 |
5 |
5 |
2.5 |
0.0 |
|
|
Sigmoid colon |
1 |
0 |
1 |
0.5 |
100.0 |
|
|
Redundancy of colon |
0.29 |
|||||
|
Yes |
163 |
29 |
192 |
94.1 |
84.9 |
|
|
No |
9 |
3 |
12 |
5.9 |
75.0 |
|
|
No of x-ray exposures |
0.06 |
|||||
|
1-5 |
3 |
3 |
6 |
2.9 |
50.0 |
|
|
6-10 |
145 |
25 |
170 |
83.3 |
85.3 |
|
|
11-15 |
24 |
4 |
28 |
13.7 |
85.7 |
|
|
Total |
172 |
32 |
204 |
100.0 |
84.3 |
|
Table 1: Relation of demographic, anatomical and procedural factors with success of hydrostatic reduction.
|
Position of sigmoid flexure |
No |
% |
|
Pelvic |
73 |
35.8 |
|
Umbilical |
50 |
24.5 |
|
RIF and Right Lumber |
40 |
19.6 |
|
RIF |
11 |
5.4 |
|
Left hypochondriac |
9 |
4.4 |
|
Left lumber and umbilical |
5 |
2.5 |
|
Right hypochondriac |
5 |
2.5 |
|
Right lumber |
4 |
2.0 |
|
Epigastric |
2 |
1.0 |
|
Left lumber |
2 |
1.0 |
|
RIF and umbilical |
2 |
1.0 |
|
Left hypochondriac and right lumber |
1 |
0.5 |
*RIF: Right iliac fossa
Table 2: Location of sigmoid flexure (N=204).
4. Discussion
This study shows that hydrostatic reduction of intussusception can be successfully performed using contrast material under plane x-ray guidance with an acceptable success rate. Non-operative reduction is preferred to surgery in patients who present early, in whom the bowel is viable and there are no signs of bowel compromise. This procedure can avoid unnecessary surgery and anesthesia in children with intussusception. Centers who could not establish non-operative treatment by US or fluoroscopy guided reduction, may consider starting this procedure with plane x-ray guidance. Among the methods of non-operative reduction, US and fluoroscopy guided reductions are most popular. USG is operator dependent and it needs a continuous presence of a sonologist [14]. On the other hand, fluoroscopic reduction by contrast enema has the disadvantage of more radiation hazard. Air enema reduction under fluoroscopic guidance also has increasing popularity [15-17]. Unfortunately, among all possible option for non-operative reduction, many centers in the LIMCs could not still adopt any of these and are still performing surgeries for all cases of intussusception. Our finding may encourage these centers to perform non-operative treatment by plane radiography as this is widely available and we had satisfactory success rate.
The median age of 10 months in this study is higher than many reported median ages of 8 months. However, majority of the patients (45.59%) were between 6 and 12 months of age which is the most common age range for occurrence of intussusception. Only 36 (17.65%) patients were more than 2 years of age; among them 29 (80.6%) underwent successful hydrostatic reduction. Although there was no significant difference among age groups with regards to hydrostatic reduction, it was found that median age of patients with successful hydrostatic reduction was significantly higher than patients with failed reduction. In this study, more patients presented during winter and spring. Seasonal variation of intussusception has been reported by other studies. Although it has been suggested that the increased prevalence in Spring or Summer is due to gastroenteritis and in Winter due to more respiratory infections, there are variable reports of seasonal variations [5, 18-21].
The most common site of obstruction in this series was right hepatic flexure (56.37%). This means that these patients were presented early and that is why they were sent for hydrostatic reduction. If the mass advances more distally, it becomes more irreducible and only 4 of the 11 patients in whom the mass was at or distal to splenic flexure underwent successful reduction. The overall success rate in this series was 84.31% which is comparable to success rates of US guided or fluoroscopy guided air enema or hydrostatic reduction. A meta-analysis that compared air vs liquid enema for reduction of intussusception showed that the combined estimate for success rate of air enema was 82.7% and it was 69.6% for hydrostatic reduction. [2] There was also no perforation and only one recurrence (0.49%) in this series. This goes with the very minimum complication rates of non-operative reduction. Rate of perforation and recurrence were reported to be 0.39-0.43% and 6-7.3% in the above-mentioned meta-analysis. It was found that failed reduction of the distal intussusception needed less time (26 minutes) than the intussusceptions proximal to TC (40.5 minutes). It implies that, when the radiographer found that the obstruction was located distally, he did not try more attempts and abandoned the procedure.
Redundancy of colon was not significantly related to failed reduction in this study. This is similar to finding from Ntoulia et al. [22]. However, 94% of the patients in this series had redundant colon. A redundancy or looping of individual or several sections of the colon are far more frequent than was previously assumed [23]. Redundancy of sigmoid colon has been suggested to be related with distal intussusception [24]. Although the relation of intussusception with malrotation of gut is well established, their relation with redundant colon needs further evaluation [25]. Redundancy of sigmoid colon has also been shown to be related to constipation [26-28]. This study also found that location of sigmoid colonic flexure was in the umbilical region in about one-fourth patients. Several studies have shown that the sigmoid colon is often in the right side in the children [27, 29, 30].
Initially, we performed the procedures under fluoroscopic guidance using barium enema and later shifted to plane radiography guidance to reduce radiation exposure. All the procedures in the current series were performed under plane x-ray guidance. At the beginning, we performed the procedures by hanging saline contrast from 3 feet height from a saline stand connected with a rectal Foley catheter. The contrast saline enema from the saline bag was allowed to flow and to exert pressure on intussusceptum. It was time consuming and usually took 2-3 hours to complete. Radiographers showed lack of patience and could not complete the procedure within their duty hour. Parents also used to become worried. It was also difficult to hold the apprehended patient for a long time on the table. Subsequently, we started to give contrast enema directly through the foleys catheter to the rectum by 50 ml syringe with a very slow and gentle pressure. This application method is usually performed by many during diagnostic contrast enema procedure. This technique is easier, less time consuming and parents also became satisfied by observing the improvement within less than half an hour.
Hydrostatic reduction is usually attempted in patients with history of symptoms for less than 24 to 48 hours [31]. In this study, we accepted the patients with symptoms up to 72 hours depending on the condition of the patients. Tareen et al. performed non-operative reduction in patients with up to 10 days of history and they have found that there was no correlation between length of history and non-operative reduction outcome [32]. In our experience, hydrostatic reduction under US guidance was time consuming, needed several settings, and gaseous interference hampered the procedure. There was difficulty in visualization of completion of reduction and assessment of perforation. The current procedure will allow observation of the completion of reduction and occurrence of perforation should these happen [16, 17]. Although, the procedure cost about 71 USD, it was performed at a lower cost of 58 USD for poor patients and 35 USD for the very poor patients from whom only the costs of materials were taken. The cost may be further reduced if it can be performed in a government hospital set-up.
This study has some limitations. The sample size is moderate and the results are from a single center. Since data were collected from a center where only hydrostatic reduction was performed and the patients were admitted in other centers, we could not evaluate the patients for presenting features, etiologies, hospital stay and surgeries performed on them. However, the aim of the study was to report the radiological perspectives of this procedures. We believe, this study will be able to re-emphasize the need and feasibility of non-operative treatment of intussusception in resource limited settings. This procedure is reproducible and easy to perform; and it will save many patients in the LMICs from unnecessary surgery and anesthesia in patients who present early and thereby reduce cost and complications related to these.
5. Conclusion
Contrast enema reduction under plane x-ray guidance was successfully performed in about 84% of the patients and it is a safe alternative of US or fluoroscopy guided non-operative reduction of intussusception in resource limited settings where other established methods cannot be applied.
Declarations
Funding
No funding was used for this research from any funding agency in the public, commercial or not-for-profit sectors.
Conflict of Interest
None.
Availability of Data and Material
Data are available upon reasonable request from the following ORCID ID: https://orcid.org/0000-0002-1661-2111
Authors’ Contributions
Conceptualization: MQA, TB. Data curation: MQA, TKC. Formal analysis: TKC. Methodology: MQA. Supervision: TB. Writing – MQA, TTA. Writing -review and editing: TKC, TB. Approval of final manuscript: MQA, TB.
Ethics Approval
Ethics approval was given by the Institutional Review Board of CMOSH Medical College, Chattogram (Memo: CMOSHMC/IRB/2021/14).
Consent for Participation
Informed consent was taken prior to procedure from parents of the patients who underwent hydrostatic reduction.
Consent for Publication
Not required.
Acknowledgement
The authors thank the radiographers of CSCR Pvt. Ltd., Mr. Dipak Kumar Ghosh and Mr. Tapan Kumar Ghosh for their sincere support in performing hydrostatic reduction since 2003. The authors also gratefully acknowledge the contributions of Pediatric Surgery Department of Chittagong Medical College and all pediatric Surgeons of Chattogram City.
References
- Mensah Y, Glover-Addy H, Etwire V, et al. Ultrasound Guided Hydrostatic Reduction of Intussusception in children at Korle Bu Teaching Hospital: An Initial Experience. GMJ-MedJ 45 (2011): 128-131.
- Sadigh G, Zou KH, Razavi SA, et al. Meta-analysis of Air Versus Liquid Enema for Intussusception Reduction in Children. AJR 205 (2015): 542-549.
- Wakjira E, Sisay S, Zember J, et al. Implementing ultrasound-guided hydrostatic reduction of intussusception in a low-resource country in Sub-Saharan Africa: our initial experience in Ethiopia. Emerg Radiol 25 (2018): 1-6.
- Mpabalwani E, Ngwira B, Cortese MM, et al. Evaluation of Intussusception after Monovalent Rotavirus Vaccination in Africa. N Engl J Med 378 (2018): 1521-1528.
- Satter SM, Aliabadi N, Yen C, et al. Epidemiology of childhood intussusception in Bangladesh: Findings from an active national hospital-based surveillance system, 2012-2016. Vaccine 36 (2018): 7805-7810.
- Clark A, Tate J, Parashar U, et al. Mortality reduction benefits and intussusception risks of rotavirus vaccination in 135 low-income and middle-income countries: a modelling analysis of current and alternative schedules. Lancet Glob Heal 7 (2019): 1541-1552.
- Akello VV, Cheung M, Kurigamba G, et al. Pediatric intussusception in Uganda: differences in management and outcomes with high-income countries. J Pediatr Surg 55 (2020): 530-534.
- Chalya PL, Kayange NM, Chandika AB. Childhood intussusceptions at a tertiary care hospital in northwestern Tanzania: a diagnostic and therapeutic challenge in resource-limited setting. Ital J Pediatr 40 (2014): 1-8.
- Chowdhury TK, Ahsan Q, Chowdhury MZ, et al. Hydrostatic reduction of intussusception with intermittent radiography: an alternative to fluoroscopy or ultrasound- guided reduction in low- income and income countries. World Jnl Ped Surg 4 (2021): e000221.
- Diagnostic Imaging Pathways-About Imaging: Ionizing radiation in Diagnostic Imaging. Imaging Pathways (2019).
- Ogbole GI. Radiation dose in paediatric computed tomography: Risks and benefits. Ann lb Postgr Med 8 (2010): 118-126.
- Lumbreras B, Salinas JM, Gonzalez-Alvarez I. Cumulative exposure to ionising radiation from diagnostic imaging tests: analysis in Spain. BMJ Open 9 (2019): e030905.
- Bikos Konstantin, Kher A. Seasons: Meteorological and Astronomical. Time and Date AS (1995-2021).
- Blane CE, Strouse PJ, Dipietro MA, et al. The effect of screening sonography on the positive rate of enemas for intussusception. Pediatr Radiol 33 (2003): 190-193.
- Daftary G, Harvard Medical Schhol YI, Lieberman G. Intussuceptio: A Guide to Diagnosis and Intervention in children. 2020. Yumpu (2005).
- Wong CWY, Chan IHY, Chung PHY, et al. Childhood intussusception?: 17-year experience at a tertiary referral centre in Hong Kong. Hong Kong Med J 21 (2015): 518-523.
- Del-Pozo G, Albillos JC, Tejedor D, et al. Intussusception in Children: Current Concepts in Diagnosis and Enema Reduction. RadioGraphics 19 (1999): 299-319.
- Gadisa A, Tadesse A, Hailemariam B. Patterns and seasonal variation of intussusception in children?: a retrospective analysis of cases operated in a tertiary hospital in Ethiopia. Ethiop Med J 54 (2016): 9-15.
- Carneiro PMR, Kisusi DM. Intussusception in children seen at Muhimbili National Hospital, Dar es Salaam. East African Med J 81 (2004): 439-442.
- Bhowmick K, Kang G, Bose A, et al. Retrospective Surveillance for Intussusception in Children Aged Less than Five Years in a South Indian Tertiary-care Hospital. J Heal Popul NUTR 27 (2009): 660-665.
- Zhang T, Cui L, Geng X, et al. Epidemiology study of pediatric primary intussusception aged 24 months in pre-rotavirus vaccine era of Jinan, China. Vaccine 37 (2019): 1436-1442.
- Ntoulia A, Tharakan SJ, Reid JR, et al. Failed Intussusception Reduction in Children: Correlation Between Radiologic, Surgical, and Pathologic Findings. AJR 207 (2016): 424-433.
- Moller PF. The Redundant Colon. Acta radiol 6 (1926): 432-457.
- Sullins VF, Jarboe M, Calkins CaM. Acquired Anorectal Disorders. In Eds.: Holcomb GWI, Murphy JP, St. Peter SD. Holcomb and Ashcraft’s Pediatric Surgery, 7th Philadelphia: Elsevier (2015): 616.
- Brereton RJ., Taylor B., Hall CM. lntussuscept ion and intestinal malrotation in infants: Waugh’s syndrome. Br J Surg 73 (1986): 55-57.
- Wood RJ, Levitt MA. Fecal Incontinence and Constipation. In Eds.: George W III, Murphy J Patric, St. Peter SD. Holcomb and Ashcraft’s Pediatric Surgery, 7th Philadelphia: Elsevier (2017): 610.
- Brummer P, Seppala P, Wegelius UNO. Redundant colon as a cause of constipation. Gut 3 (1962): 140.
- Noviello C, Nobile S, Romano M, et al. Functional constipation or redundancy of the colon? Indian J Gastroenetrol 39 (2020): 147-152.
- Fiorella DJ, Donnelly LF. Frequency of Right Lower Quadrant Position of the Sigmoid Colon in Infants and Young Children. Radiology 219 (2001): 91-94.
- Saxena AK, Sodhi KS, Tirumani S. Position of a sigmoid colon in right iliac fossa in children: A retrospective study. J Indian Assoc Pediatr Surg 16 (2011): 93-96.
- Ocal S, Cevik M, Boleken ME, et al. A comparison of manual versus hydrostatic reduction in children with intussusception: Single-center experience. Afr J Paediatr Surg 11 (2014): 184-189.
- Tareen F, Ryan S, Avanzini S. Does the length of the history influence the outcome of pneumatic reduction of intussusception in children? Pediatr Surg Int 27 (2011): 587-589.
