Ultrasound Guided Percutaneous Neurolysis for Sciatic Nerve Tethering Post Mid-Hamstring Tendon Repair
Article Information
Yi Ying Heng 1,*, Eamon Koh 2,3, Jeffrey Boyle2
1Royal Perth Hospital, Orthopaedics Department, Perth, WA 6000, Australia
2Fremantle Dockers Football Club, Medical Department, Cockburn Central, WA 6164, Australia
3Envision Medical Imaging, Wembley, WA 6014, Australia
*Corresponding Author: Yi Ying Heng, Royal Perth Hospital, Orthopaedics Department, Perth, WA 6000, Australia
Received: 20 February 2020; Accepted: 04 March 2020; Published: 11 March 2020
Citation: Yi Ying Heng, Eamon Koh, Jeffrey Boyle. Ultrasound Guided Percutaneous Neurolysis for Sciatic Nerve Tethering Post Mid-Hamstring Tendon Repair. Journal of Orthopaedics and Sports Medicine 2 (2020): 35-41.
View / Download Pdf Share at FacebookOrthopaedics articles Orthopaedics Research articles Orthopaedics review articles Orthopaedics PubMed articles Orthopaedics PubMed Central articles Orthopaedics 2023 articles Orthopaedics 2024 articles Orthopaedics Scopus articles Orthopaedics impact factor journals Orthopaedics Scopus journals Orthopaedics PubMed journals Orthopaedics medical journals Orthopaedics free journals Orthopaedics best journals Orthopaedics top journals Orthopaedics free medical journals Orthopaedics famous journals Orthopaedics Google Scholar indexed journals Football articles Football Research articles Football review articles Football PubMed articles Football PubMed Central articles Football 2023 articles Football 2024 articles Football Scopus articles Football impact factor journals Football Scopus journals Football PubMed journals Football medical journals Football free journals Football best journals Football top journals Football free medical journals Football famous journals Football Google Scholar indexed journals Hamstring injuries articles Hamstring injuries Research articles Hamstring injuries review articles Hamstring injuries PubMed articles Hamstring injuries PubMed Central articles Hamstring injuries 2023 articles Hamstring injuries 2024 articles Hamstring injuries Scopus articles Hamstring injuries impact factor journals Hamstring injuries Scopus journals Hamstring injuries PubMed journals Hamstring injuries medical journals Hamstring injuries free journals Hamstring injuries best journals Hamstring injuries top journals Hamstring injuries free medical journals Hamstring injuries famous journals Hamstring injuries Google Scholar indexed journals Sports articles Sports Research articles Sports review articles Sports PubMed articles Sports PubMed Central articles Sports 2023 articles Sports 2024 articles Sports Scopus articles Sports impact factor journals Sports Scopus journals Sports PubMed journals Sports medical journals Sports free journals Sports best journals Sports top journals Sports free medical journals Sports famous journals Sports Google Scholar indexed journals Muscle strain injury articles Muscle strain injury Research articles Muscle strain injury review articles Muscle strain injury PubMed articles Muscle strain injury PubMed Central articles Muscle strain injury 2023 articles Muscle strain injury 2024 articles Muscle strain injury Scopus articles Muscle strain injury impact factor journals Muscle strain injury Scopus journals Muscle strain injury PubMed journals Muscle strain injury medical journals Muscle strain injury free journals Muscle strain injury best journals Muscle strain injury top journals Muscle strain injury free medical journals Muscle strain injury famous journals Muscle strain injury Google Scholar indexed journals Surgery articles Surgery Research articles Surgery review articles Surgery PubMed articles Surgery PubMed Central articles Surgery 2023 articles Surgery 2024 articles Surgery Scopus articles Surgery impact factor journals Surgery Scopus journals Surgery PubMed journals Surgery medical journals Surgery free journals Surgery best journals Surgery top journals Surgery free medical journals Surgery famous journals Surgery Google Scholar indexed journals Bony avulsions articles Bony avulsions Research articles Bony avulsions review articles Bony avulsions PubMed articles Bony avulsions PubMed Central articles Bony avulsions 2023 articles Bony avulsions 2024 articles Bony avulsions Scopus articles Bony avulsions impact factor journals Bony avulsions Scopus journals Bony avulsions PubMed journals Bony avulsions medical journals Bony avulsions free journals Bony avulsions best journals Bony avulsions top journals Bony avulsions free medical journals Bony avulsions famous journals Bony avulsions Google Scholar indexed journals Proximal tendinous avulsions articles Proximal tendinous avulsions Research articles Proximal tendinous avulsions review articles Proximal tendinous avulsions PubMed articles Proximal tendinous avulsions PubMed Central articles Proximal tendinous avulsions 2023 articles Proximal tendinous avulsions 2024 articles Proximal tendinous avulsions Scopus articles Proximal tendinous avulsions impact factor journals Proximal tendinous avulsions Scopus journals Proximal tendinous avulsions PubMed journals Proximal tendinous avulsions medical journals Proximal tendinous avulsions free journals Proximal tendinous avulsions best journals Proximal tendinous avulsions top journals Proximal tendinous avulsions free medical journals Proximal tendinous avulsions famous journals Proximal tendinous avulsions Google Scholar indexed journals Sciatic nerve injury articles Sciatic nerve injury Research articles Sciatic nerve injury review articles Sciatic nerve injury PubMed articles Sciatic nerve injury PubMed Central articles Sciatic nerve injury 2023 articles Sciatic nerve injury 2024 articles Sciatic nerve injury Scopus articles Sciatic nerve injury impact factor journals Sciatic nerve injury Scopus journals Sciatic nerve injury PubMed journals Sciatic nerve injury medical journals Sciatic nerve injury free journals Sciatic nerve injury best journals Sciatic nerve injury top journals Sciatic nerve injury free medical journals Sciatic nerve injury famous journals Sciatic nerve injury Google Scholar indexed journals Rehabilitation articles Rehabilitation Research articles Rehabilitation review articles Rehabilitation PubMed articles Rehabilitation PubMed Central articles Rehabilitation 2023 articles Rehabilitation 2024 articles Rehabilitation Scopus articles Rehabilitation impact factor journals Rehabilitation Scopus journals Rehabilitation PubMed journals Rehabilitation medical journals Rehabilitation free journals Rehabilitation best journals Rehabilitation top journals Rehabilitation free medical journals Rehabilitation famous journals Rehabilitation Google Scholar indexed journals Fibrosis articles Fibrosis Research articles Fibrosis review articles Fibrosis PubMed articles Fibrosis PubMed Central articles Fibrosis 2023 articles Fibrosis 2024 articles Fibrosis Scopus articles Fibrosis impact factor journals Fibrosis Scopus journals Fibrosis PubMed journals Fibrosis medical journals Fibrosis free journals Fibrosis best journals Fibrosis top journals Fibrosis free medical journals Fibrosis famous journals Fibrosis Google Scholar indexed journals Biceps femoris articles Biceps femoris Research articles Biceps femoris review articles Biceps femoris PubMed articles Biceps femoris PubMed Central articles Biceps femoris 2023 articles Biceps femoris 2024 articles Biceps femoris Scopus articles Biceps femoris impact factor journals Biceps femoris Scopus journals Biceps femoris PubMed journals Biceps femoris medical journals Biceps femoris free journals Biceps femoris best journals Biceps femoris top journals Biceps femoris free medical journals Biceps femoris famous journals Biceps femoris Google Scholar indexed journals Chronic pain articles Chronic pain Research articles Chronic pain review articles Chronic pain PubMed articles Chronic pain PubMed Central articles Chronic pain 2023 articles Chronic pain 2024 articles Chronic pain Scopus articles Chronic pain impact factor journals Chronic pain Scopus journals Chronic pain PubMed journals Chronic pain medical journals Chronic pain free journals Chronic pain best journals Chronic pain top journals Chronic pain free medical journals Chronic pain famous journals Chronic pain Google Scholar indexed journals Athletes articles Athletes Research articles Athletes review articles Athletes PubMed articles Athletes PubMed Central articles Athletes 2023 articles Athletes 2024 articles Athletes Scopus articles Athletes impact factor journals Athletes Scopus journals Athletes PubMed journals Athletes medical journals Athletes free journals Athletes best journals Athletes top journals Athletes free medical journals Athletes famous journals Athletes Google Scholar indexed journals Tendon injuries articles Tendon injuries Research articles Tendon injuries review articles Tendon injuries PubMed articles Tendon injuries PubMed Central articles Tendon injuries 2023 articles Tendon injuries 2024 articles Tendon injuries Scopus articles Tendon injuries impact factor journals Tendon injuries Scopus journals Tendon injuries PubMed journals Tendon injuries medical journals Tendon injuries free journals Tendon injuries best journals Tendon injuries top journals Tendon injuries free medical journals Tendon injuries famous journals Tendon injuries Google Scholar indexed journals
Article Details
1. Introduction
Hamstring injuries are the most common muscle strain injury in footballers and other sports where quick accelerations are required [1, 2]. The most common location affected is the long head of biceps femoris myotendinous junction however, the presence of central tendon injury is more clinically significant as it is associated with a prolonged rehabilitation interval [3-5]. Whilst there is no clear consensus on indications for surgery following acute hamstring injury, it has been proposed that operative management should be considered in displaced bony avulsions, proximal tendinous avulsions involving all 3 tendons, proximal 2-tendon avulsions with retraction of > 2cm or persisting pain [2, 6, 7]. These injuries are now increasingly being treated surgically [8, 9].
The results from surgical management of hamstring injuries appear promising, especially when the repair is performed acutely [6, 9, 10]. One of the complications following surgical repair includes sciatic nerve injury, although the true incidence of this complication is unknown and the etiology uncertain [10, 11]. We describe a case of sciatic neural tethering post mid-hamstring tendon repair, and propose percutaneous neurolysis as a viable therapeutic intervention.
2. Case Report
31-year-old male elite Australian Football League footballer with known history of previous hamstring injuries bilaterally. He sustained a complete mid biceps femoris central tendon tear (British Athletics Muscle Injury Grade 4C4 injury) 13cm below the left hamstring origin demonstrated on MRI (Figure 1), and subsequently underwent surgical repair three days later.
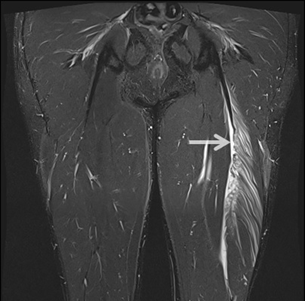
Figure 1: Coronal T2-weighted fat saturated hamstring MRI of a 31-year-old elite AFL footballer with acute left proximal biceps femoris mid-tendon tear at approximately 16 cm below the hamstring origin (arrow).
He recovered well post operatively and completed rehabilitation successfully with a return to play time of 68 days. However, he sustained a further grade 2C4 injury to the more distal left biceps femoris musculotendinous junction and central tendon which required a further 5-week rehabilitation period.
Post re-injury, the patient continued to experience ongoing mid-belly and distal hamstring pain, affecting strength and function. His clinical picture was confounded by his known background of bilateral hamstring syndrome, which had previously responded well to percutaneous neurolysis at the ischial tunnel. However, posterior thigh pain and symptoms of sciatica persisted following neurolysis at the hamstring origin. Subsequent ultrasound of the left mid hamstring muscle belly in the region of surgery showed a band of echogenic perineural fibrosis tethering the nerve to the biceps femoris muscle at the repair site that was visible on previous MRI (Figures 2 and 3a).

Figure 2: Axial T1-weighted left hamstring MRI for recurrent strain injury in rehabilitation at 8 weeks post initial injury showing a fine intermediate signal band (dotted arrow) posterior to the left sciatic nerve (dashed arrow). Note the intermediate signal repaired central tendon (arrow).
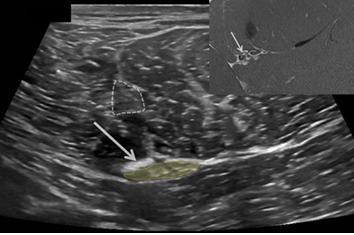
Figure 3a: Transverse ultrasound of the left proximal to mid hamstring muscle at the site of surgical repair. White or echogenic band adhesion (arrow) lies posterior to the left sciatic nerve (yellow shaded area). The repaired central tendon is iso-echoic to surrounding muscle and therefore difficult to distinguish on ultrasound due to ongoing remodeling (dashed line). Inset: MRI image oriented to corresponding ultrasound image.
Percutaneous neurolysis was performed at both the hamstring origin and tendon repair site with 80cc of normal saline and 40mg of triamcinolone acetonide (Figure 3b), and he was able to return to play in 6 days. The patient experienced mild recurrence of mid-thigh symptoms 6 weeks after the previous procedure, and percutaneous neurolysis of the sciatic nerve from the focal area of scarring at the previous site of hamstring tendon repair was performed with 20cc of saline and 5.7mg Betamethasone acetate. Again, he was able to resume playing competitively 5 days after this procedure. The patient underwent further neurolysis of the sciatic nerve again 7 weeks later with 20cc of saline and 2mg dexamethasone, and again a dense posterior band adhesion at the site of previous surgery was hydrodissected from the nerve. The patient had an excellent response to this procedure, with final resolution of symptoms at 6 months post-injury. He has no recurrence of hamstring symptoms at the 2-year mark.
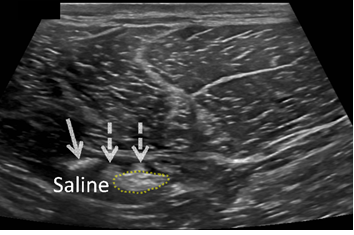
Figure 3b: Transverse ultrasound of the left proximal to mid hamstring muscle at the site of surgical repair during percutaneous neurolysis. Note displacement of the band adhesion (arrow) from the sciatic nerve (yellow dotted line) with some less echogenic peri-sciatic adhesions also evident. There is anechoic or black fluid within the peri-sciatic space post hydro-dissection.
3. Discussion
Due to the prolonged rehabilitation interval associated with biceps femoris central tendon injury and high rates of recurrence, there is a shift in the management protocol of elite athletes to early surgical repair of these tendon injuries [5, 12]. Although literature on surgical intervention remains limited, it has been suggested that non-operative management of proximal hamstring avulsions are associated with ongoing chronic pain, weakness, decreased endurance, reduction in function and difficulty with running [13]. There is even less data for management of mid-tendon injuries however, assuming that there is clinical overlap between proximal and mid-tendon injury these complications of conservative management are unacceptable in the elite sports setting. Therefore, complete biceps femoris central tendon rupture generally mandates surgical repair in many elite athletes and consequently we can expect an increase in the incidence of hamstring surgeries.
Given the proximity of the sciatic nerve to the biceps femoris muscle, the sciatic nerve is at risk both at time of hamstring injury as well as during surgery. There have been various reports of distal sciatic nerve symptoms that develop both acutely and chronically following hamstring avulsion [14, 15], but the incidence of sciatic nerve involvement remains unclear. Literature regarding sciatic nerve injury following hamstring surgery remains exiguous, but it has been suggested that the true incidence of sciatic nerve involvement is likely to be high [11]. In a recent study by Subbu et al., on 112 operative cases, the incidence of local sciatic nerve symptoms was 11%, with 1 patient requiring revision surgery for exploration and neurolysis [10]. Wilson et al proposed the risk of developing new sciatic nerve-related deficit to be 7.5%, with nerve related pain being the most common at 4.5%, and motor weakness (3.0%) and sensory loss (1.5%) being less so [11]. Entrapment of nerve by scar formation following surgery has been theorized as a possible etiology for the postoperative symptoms, although it has never been confirmed [11]. A similar case of nerve entrapment by scar tissue has been published previously, albeit in the setting of repetitive injury rather than surgery, and open surgical release was required for resolution of symptoms [15].
Other causes of sciatic nerve injuries apart from hamstring conditions have been reported in literature, with common entrapments within the deep gluteal space including fibrous bands, piriformis syndrome, ischiofemoral pathology and gluteal disorders [16]. Apart from surgical neurolysis of the sciatic nerve endoscopically [17] or through open surgery [18], image guided injection with corticosteroid has also been proposed as a useful intervention [19, 20], although most articles describe injection to the muscle, with limited studies describing a targeted perineural approach [21, 22] . A recent study by Burke et al, described 38 cases of ultrasound guided perisciatic hydrodissection, and they reported immediate relief of symptoms in 84% of the cases, with 47% of cases reporting sustained relief up to follow up of 33.6days [21]. Ultrasound guided percutaneous hydrodissection has also been described for neurolysis of the lateral femoral cutaneous nerve [23], saphenous nerve [24], and carpal tunnel syndrome [25] to good effect with minimal complications. In a randomized, double-blind control trial on hydrodissection for carpal tunnel syndrome, the authors found improvement in symptoms, and they suggest a cumulative effect of hydrodissection with repeated injections, and possible advantages for postoperative adhesions [25]. For the elite sporting population, percutaneous neurolysis is an appealing choice for intervention, given its effectiveness, low risk profile, and short return to play time, as compared to traditional surgery, which requires a longer recovery period for wound healing and post-operative rehabilitation.
3. Conclusion
Clinicians should have a high suspicion of sciatic nerve tethering due to perineural band adhesions in patients presenting with persisting local and referred pain following hamstring tendon repair. Percutaneous neurolysis can be a useful first-line therapeutic intervention which allows for rapid return to play at the usual level.
References
- Ahmad CS, Redler LH, Ciccotti MG, et al. Evaluation and management of hamstring injuries. Am J Sports Med 41 (2013): 2933-2947.
- Cohen S, Bradley J. Acute proximal hamstring rupture. J Am Acad Orthop Surg 15 (2007): 350-355.
- Connell DA, Schneider-Kolsky ME, Hoving JL, et al. Longitudinal study comparing sonographic and MRI assessments of acute and healing hamstring injuries. AJR Am J Roentgenol 183 (2004): 975-984.
- Patel A, Chakraverty J, Pollock N, et al. British athletics muscle injury classification: a reliability study for a new grading system. Clin Radiol 70 (2015): 1414-1420.
- Pollock N, Patel A, Chakraverty J, et al. Time to return to full training is delayed and recurrence rate is higher in intratendinous (c) acute hamstring injury in elite track and field athletes: clinical application of the British Athletics Muscle Injury Classification. Br J Sports Med 50 (2016): 305-310.
- Cohen SB, Rangavajjula A, Vyas D, et al. Functional results and outcomes after repair of proximal hamstring avulsions. Am J Sports Med 40 (2012): 2092-2098.
- Gidwani S, Bircher MD. Avulsion injuries of the hamstring origin - a series of 12 patients and management algorithm. Ann R Coll Surg Engl 89 (2007): 394-399.
- Harris JD, Griesser MJ, Best TM, et al. Treatment of proximal hamstring ruptures - a systematic review. Int J Sports Med 32 (2011): 490-495.
- van der Made AD, Reurink G, Gouttebarge V, et al. Outcome After Surgical Repair of Proximal Hamstring Avulsions: A Systematic Review. Am J Sports Med 43 (2015): 2841-2851.
- Subbu R, Benjamin-Laing H, Haddad F. Timing of surgery for complete proximal hamstring avulsion injuries: successful clinical outcomes at 6 weeks, 6 months, and after 6 months of injury. Am J Sports Med 43 (2015): 385-391.
- Wilson TJ, Spinner RJ, Mohan R, et al. Sciatic Nerve Injury After Proximal Hamstring Avulsion and Repair. Orthop J Sports Med 5 (2017): 2325967117713685.
- Brukner P, Connell D. Serious thigh muscle strains': beware the intramuscular tendon which plays an important role in difficult hamstring and quadriceps muscle strains. Br J Sports Med 50 (2016): 205-208.
- Wood DG, Packham I, Trikha SP, et al. Avulsion of the proximal hamstring origin. J Bone Joint Surg Am 90 (2008): 2365-2374.
- Carmody C, Prietto C. Entrapment of the sciatic nerve as a late sequela of injury to the hamstring muscles. A case report. J Bone Joint Surg Am 77 (1995): 1100-1102.
- Lohrer H, Nauck T, Konerding, MA. Nerve entrapment after hamstring injury. Clin J Sport Med 22 (2012): 443-445.
- Hernando MF, Cerezal L, Perez-Carro L, et al. Deep gluteal syndrome: anatomy, imaging, and management of sciatic nerve entrapments in the subgluteal space. Skeletal Radiol 44 (2015): 919-934.
- Martin HD, Shears SA, Johnson JC, et al. The endoscopic treatment of sciatic nerve entrapment/deep gluteal syndrome. Arthroscopy 27 (2011): 172-181.
- Benson ER, Schutzer SF. Posttraumatic piriformis syndrome: diagnosis and results of operative treatment. J Bone Joint Surg Am 81 (1999): 941-949.
- Benzon HT, Katz JA, Benzon HA, et al. Piriformis syndrome: anatomic considerations, a new injection technique, and a review of the literature. Anesthesiology 98 (2003): 1442-1448.
- Masala S, Crusco S, Meschini A, et al. Piriformis syndrome: long-term follow-up in patients treated with percutaneous injection of anesthetic and corticosteroid under CT guidance. Cardiovasc Intervent Radiol 35 (2012): 375-382.
- Burke CJ, Walter WR, Adler RS. Targeted Ultrasound-Guided Perineural Hydrodissection of the Sciatic Nerve for the Treatment of Piriformis Syndrome. Ultrasound Q (2018).
- Rosales J, Garcia N, Rafols C, et al. Perisciatic Ultrasound-Guided Infiltration for Treatment of Deep Gluteal Syndrome: Description of Technique and Preliminary Results. J Ultrasound Med 34 (2015): 2093-2097.
- Mulvaney SW. Ultrasound-guided percutaneous neuroplasty of the lateral femoral cutaneous nerve for the treatment of meralgia paresthetica: a case report and description of a new ultrasound-guided technique. Curr Sports Med Rep 10 (2011): 99-104.
- Clendenen S, Greengrass R, Whalen J, et al. Infrapatellar saphenous neuralgia after TKA can be improved with ultrasound-guided local treatments. Clin Orthop Relat Res 473 (2015): 119-125.
- Wu YT, Chen SR, Li TY, et al. Nerve hydrodissection for carpal tunnel syndrome: A prospective, randomized, double-blind, controlled trial. Muscle Nerve 59 (2019): 174-180.
