Type 1 Brugada Phenocopy in a Patient with Stubborn Congestive Heart Failure
Article Information
Chao Liu1*, Changjin Li1*, Haoyu Gu1*, Songqun Huang1, Jiang Cao1, Zhifu Guo1#
1Department of Cardiovasology, Changhai Hospital, Shanghai, China
*Corresponding Author: Zhifu Guo, Department of Cardiovasology, Changhai Hospital, Shanghai, China
Received: 26 March 2023; Accepted: 10 April 2023; Published: 13 April 2023
Citation: Chao Liu, Changjin Li, Haoyu Gu, Songqun Huang, Jiang Cao, Zhifu Guo. Type 1 Brugada Phenocopy in a Patient with Stubborn Congestive Heart Failure. Archives of Clinical and Medical Case Reports. 7 (2023): 145-147.
View / Download Pdf Share at FacebookKeywords
Cardiac; Cardiology; Heart Failure
Cardiac articles; Cardiology articles; Heart Failure articles
Cardiac articles Cardiac Research articles Cardiac review articles Cardiac PubMed articles Cardiac PubMed Central articles Cardiac 2023 articles Cardiac 2024 articles Cardiac Scopus articles Cardiac impact factor journals Cardiac Scopus journals Cardiac PubMed journals Cardiac medical journals Cardiac free journals Cardiac best journals Cardiac top journals Cardiac free medical journals Cardiac famous journals Cardiac Google Scholar indexed journals Ultrasound articles Ultrasound Research articles Ultrasound review articles Ultrasound PubMed articles Ultrasound PubMed Central articles Ultrasound 2023 articles Ultrasound 2024 articles Ultrasound Scopus articles Ultrasound impact factor journals Ultrasound Scopus journals Ultrasound PubMed journals Ultrasound medical journals Ultrasound free journals Ultrasound best journals Ultrasound top journals Ultrasound free medical journals Ultrasound famous journals Ultrasound Google Scholar indexed journals Covid-19 articles Covid-19 Research articles Covid-19 review articles Covid-19 PubMed articles Covid-19 PubMed Central articles Covid-19 2023 articles Covid-19 2024 articles Covid-19 Scopus articles Covid-19 impact factor journals Covid-19 Scopus journals Covid-19 PubMed journals Covid-19 medical journals Covid-19 free journals Covid-19 best journals Covid-19 top journals Covid-19 free medical journals Covid-19 famous journals Covid-19 Google Scholar indexed journals Cardiology articles Cardiology Research articles Cardiology review articles Cardiology PubMed articles Cardiology PubMed Central articles Cardiology 2023 articles Cardiology 2024 articles Cardiology Scopus articles Cardiology impact factor journals Cardiology Scopus journals Cardiology PubMed journals Cardiology medical journals Cardiology free journals Cardiology best journals Cardiology top journals Cardiology free medical journals Cardiology famous journals Cardiology Google Scholar indexed journals Tapia Syndrome articles Tapia Syndrome Research articles Tapia Syndrome review articles Tapia Syndrome PubMed articles Tapia Syndrome PubMed Central articles Tapia Syndrome 2023 articles Tapia Syndrome 2024 articles Tapia Syndrome Scopus articles Tapia Syndrome impact factor journals Tapia Syndrome Scopus journals Tapia Syndrome PubMed journals Tapia Syndrome medical journals Tapia Syndrome free journals Tapia Syndrome best journals Tapia Syndrome top journals Tapia Syndrome free medical journals Tapia Syndrome famous journals Tapia Syndrome Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals CT articles CT Research articles CT review articles CT PubMed articles CT PubMed Central articles CT 2023 articles CT 2024 articles CT Scopus articles CT impact factor journals CT Scopus journals CT PubMed journals CT medical journals CT free journals CT best journals CT top journals CT free medical journals CT famous journals CT Google Scholar indexed journals surgery articles surgery Research articles surgery review articles surgery PubMed articles surgery PubMed Central articles surgery 2023 articles surgery 2024 articles surgery Scopus articles surgery impact factor journals surgery Scopus journals surgery PubMed journals surgery medical journals surgery free journals surgery best journals surgery top journals surgery free medical journals surgery famous journals surgery Google Scholar indexed journals Heart Failure articles Heart Failure Research articles Heart Failure review articles Heart Failure PubMed articles Heart Failure PubMed Central articles Heart Failure 2023 articles Heart Failure 2024 articles Heart Failure Scopus articles Heart Failure impact factor journals Heart Failure Scopus journals Heart Failure PubMed journals Heart Failure medical journals Heart Failure free journals Heart Failure best journals Heart Failure top journals Heart Failure free medical journals Heart Failure famous journals Heart Failure Google Scholar indexed journals Cholecystectomy articles Cholecystectomy Research articles Cholecystectomy review articles Cholecystectomy PubMed articles Cholecystectomy PubMed Central articles Cholecystectomy 2023 articles Cholecystectomy 2024 articles Cholecystectomy Scopus articles Cholecystectomy impact factor journals Cholecystectomy Scopus journals Cholecystectomy PubMed journals Cholecystectomy medical journals Cholecystectomy free journals Cholecystectomy best journals Cholecystectomy top journals Cholecystectomy free medical journals Cholecystectomy famous journals Cholecystectomy Google Scholar indexed journals
Article Details
1. Introduction
Brugada syndrome (BrS) is an inherited cardiac ion channelopathy, which can induce malignant arrhythmias and sudden cardiac death (SCD). The BrS ECG is characterized by an abnormal ST-segment elevation of at least 2 mm (0.2 mV) in leads V1-3, including three types. Type-1 manifests a coved pattern, which obtained the most diagnostic significance [1-3]. Brugada phenocopy (BrP) is referred to as a clinical situation that has an identical ECG pattern to congenital BrS but is induced by various other clinical factors. In this report, we describe the case of severe heart failure, in which the Type-1 Brugada pattern was recorded.
2. Case Report
A 71-year-old female was hospitalized with urinary tract infection, accompanied by fatigue and exertional dyspnea complaint for a week. Examination on admission: WBC 11.54×109/L, BNP 2373.76 pg/ml, Crea 515 μmol/L, ECG: sinus rhythm (71 bpm). When the patient was routinely disposed with anti-infection, reinforcement myocardial systole, diuretic, and other symptomatic measures for 7 days, the BNP gradually decreased to 630.69 pg/ml, with discomfort complaint relieved. On the 16th day, the patient has repeated episodes of atrial fibrillation (AF) with rapid ventricular rate (150-160 bpm), accompanied by the symptoms of chest tightness, dyspnea, and orthopnea later, with an abnormal increase of BNP levels to 1950.82 pg/ml. On the 18th day, the patient occurred palpitations again. The ECG (Figure 2) showed the rapid AF (132 bpm) combined with Brugada pattern. The patient never had a similar BrP ECG before, and had no SCD family history. Echocardiography showed that the ejection fraction (EF) was reduced to 47%. The BNP > 6000 pg/ml, NT-pro BNP > 35000 pg/ml, Na+ 139mmol/L, K+ 4.1 mmol /L, Ca2+ 1.99 mmol /L, D-dimer: 1.26 μg/ml (<0.5), cTnI: 0.063 μg/L. The 18-lead ECG retested 4 hours later, showed that the BrP still existed, and no ST-segment mirror changes were observed in leads V7-9. Continuous intravenous recombinant human brain natriuretic peptide (rhBNP), lanatoside C (cedilanid), and diuretic to counter heart failure, as well as anti-infection treatment. 3 days later, the patient’s NT-pro BNP was significantly decreased, the ECG showed sinus rhythm (90 bpm), and the symptoms improved dramatically. The patient was discharged home on the 35th day, with regular follow-ups in the heart failure clinic. Up until now (2 years later), no arrhythmic events have occurred.
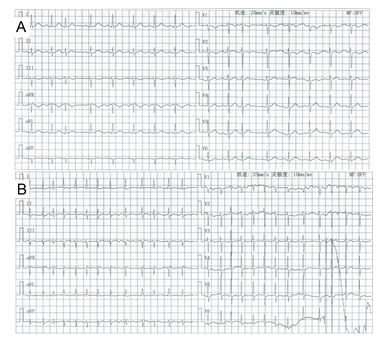
Figure 1: ECG tracings documented. (A) On admission, the 12-lead ECG showed sinus rhythm, without RBBB or ST-segment elevation in leads V1-2. (B) On the 16th day, the 12-lead ECG repeatedly showed episodes of rapid AF, without RBBB or ST-segment elevation in leads V1-2.
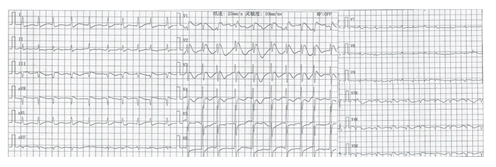
Figure 2: On the 18th day, the 18-lead ECG showed a “coved-like” ST-segment elevation in leads V1-2, combined with rapid AF.
3. Discussion
3.1 BrS and BrP
BrS is an inherited cardiac ion channelopathy with a potential risk of death. However, BrP changes refer to the influence of some specific clinical conditions [4], such as fever, metabolic disorder, mechanical compression, myocardial ischemia, pulmonary embolism, and even some drugs. Nevertheless, it is the most difficult to distinguish the true congenital BrS owing to identical ECG patterns. Patients with only BrP and no family history indicate a low probability of true congenital BrS. Most significantly, patients with BrP obtain a negative induced reaction with sodium channel blockers, while patients with BrS obtain a positive induced reaction [5]. For BrS, the primary goal is to prevent SCD by requiring ICD once definitely diagnosed. For BrP, once the inducement factors are corrected, it disappears. Hence, patients with BrP usually gain a better prognosis than BrS.
3.2 The Differential Diagnosis of Brugada Wave
3.2.1 Electrolyte Disturbance: In hypercalcemia, the accelerated flow velocity of calcium shortened the 2 phases of action potential duration (APD), which could shorten or even make the ST-segment not obvious. Hyperkalemia generally causes some changes in ECG pattern in which a prolonged QTc interval with a peak T wave [6]. However, the patient has normal electrolytes.
3.2.2 Myocardial Infarction: The ECG of anterior myocardial infarction is manifested as an abnormal ST-segment elevation in leads V1-3.In this case, the retested 18-lead ECG showed that ST-segment elevation in V1-2 still existed, but no ST-segment mirror changes were observed in leads V7-9. Combined with no apparently abnormal cTnI, myocardial infarction was not considered.
3.2.3 Right Bundle Branch Block (RBBB): The RBBB ECG is characterized as a broad R wave or rsR’ morphology of QRS complex in leads V1-2, and a broad S wave in leads I, avL, and V5-6. In this case, the ECG showed apparently J point upward and “coved” elevation of ST-segment, while the RBBB commonly presented ST-segment depression without shortening in the lead V1-2.
3.3 The Etiology Analysis of BrP in this Case
In this case, we tend to consider that BrP is caused by myocardial ischemia due to acute heart failure. Repeated and persistent episodes of tachycardia deteriorate cardiac systolic function. Within only 1 day, the level of BNP aggravated sharply from 1950.82 pg/ml to more than 6000 pg/ml, with an obvious change of stubborn and congestive heart failure. Myocardial ischemia is a well-known and published etiology of BrP. In this case, the mechanism could be related to the transient ion channel dysfunction. The outward potassium current (Ito) is increased, and the balance between inward and outward currents is broken, inducing the J-point and ST-segment elevations in leads V1-2 [7].
4. Conclusion
Whether Brugada syndrome or Brugada phenocopy, further examination should be recommended to get a definitive diagnosis and make appropriate therapeutic decisions.
Funding
This work was funded by the National Natural Science Foundation of China (81970278).
References
- Antzelevitch C, Brugada P, Borggrefe M, et al. Brugada syndrome: report of the second consensus conference: endorsed by the Heart Rhythm Society and the European Heart Rhythm Association. Circulation 111 (2005): 659-670.
- Brugada P, Brugada J. Right bundle branch block, persistent ST segment elevation and sudden cardiac death: a distinct clinical and electrocardiographic syndrome. A multicenter report. Journal of the American College of Cardiology 20 (1992): 1391-1396.
- Frustaci A, Priori S, Pieroni M, et al. Cardiac histological substrate in patients with clinical phenotype of Brugada syndrome. Circulation 112 (2005): 3680-3687.
- Anselm D, Gottschalk B, Baranchuk A. Brugada phenocopies: consideration of morphologic criteria and early findings from an international registry. The Canadian journal of cardiology 30 (2014): 1511-1515.
- Anselm D, Baranchuk A. Terminological clarification of Brugada Phenocopy, Brugada Syndrome, and the Brugada ECG pattern: re. Early repolarization pattern in patients with provocable Brugada Phenocopy: a marker of additional arrhythmogenic cardiomyopathy. International journal of cardiology 171 (2014): 288.
- Varga C, Kálmán Z, Szakáll A, et al. ECG alterations suggestive of hyperkalemia in normokalemic versus hyperkalemic patients. BMC emergency medicine 19 (2019): 33.
- Baranchuk A, Nguyen T, Ryu M, et al. Brugada phenocopy: new terminology and proposed classification. Annals of noninvasive electrocardiology: the official journal of the International Society for Holter and Noninvasive Electrocardiology, Inc 17 (2012): 299-314.
