Suicidality and Psychosis Following Vaping Related Lung Injury
Article Information
Samuel K Lin, MD1,2*, Chad Percifield, DO1,2, Zach Hommer, MD1,2, Brad Demijohn, MD1,2, Carol A. Janney, PhD1,2,3
1Pine Rest Christian Mental Health Services, 300 68th Street SE, Grand Rapids, Michigan, USA
2Division of Psychiatry and Behavioral Medicine, Michigan State University College of Human Medicine, Grand Rapids, MI, USA
3Department of Epidemiology and Biostatistics, Michigan State University College of Human Medicine, East Lansing, MI, USA
*Corresponding Author: Samuel K Lin, Pine Rest Christian Mental Health Services, 300 68th Street SE, Grand Rapids, Michigan 49548, USA
Received: 25 June 2022; Accepted: 11 July 2022; Published: 21 July 2022
Citation: Samuel K Lin, Chad Percifield, Zach Hommer, Brad Demijohn, Carol A. Janney. Suicidality and Psychosis Following Vaping Related Lung Injury. Archives of Clinical and Medical Case Reports 6 (2022): 537-540.
View / Download Pdf Share at FacebookAbstract
Background: Vaping-related lung injuries are of great concern, particularly among those who vape tetrahydrocannabinol (THC). Research also indicates that THC use increases the risk of developing psychotic disorders, particularly with use of high potency THC.
Case Presentation: The case of a 20-year-old female with a history of depression and daily vaping of THC is presented. She was medically hospitalized and treated for a vaping-related lung injury, followed by a psychiatric hospitalization for treatment of depression and suicidal ideation. The patient endorsed new-onset psychotic symptoms which required targeted treatment. A second psychiatric hospitalization ensued after an intervening suicide attempt.
Conclusions: Vaping of THC poses clear risks to the physical health of its users, including vaping-related lung injury. Although the patient presented in this case recovered from her lung injury, her subsequent need for psychiatric treatment also highlights the detrimental effects from vaping THC on mental health, ranging from depression to psychotic symptoms and even to suicidality.
Keywords
<p>EVALI; Vaping; THC; Lung injuries; Depression</p>
EVALI articles; Vaping articles; THC articles; Lung injuries articles; Depression articles
EVALI articles EVALI Research articles EVALI review articles EVALI PubMed articles EVALI PubMed Central articles EVALI 2023 articles EVALI 2024 articles EVALI Scopus articles EVALI impact factor journals EVALI Scopus journals EVALI PubMed journals EVALI medical journals EVALI free journals EVALI best journals EVALI top journals EVALI free medical journals EVALI famous journals EVALI Google Scholar indexed journals COVID-19 articles COVID-19 Research articles COVID-19 review articles COVID-19 PubMed articles COVID-19 PubMed Central articles COVID-19 2023 articles COVID-19 2024 articles COVID-19 Scopus articles COVID-19 impact factor journals COVID-19 Scopus journals COVID-19 PubMed journals COVID-19 medical journals COVID-19 free journals COVID-19 best journals COVID-19 top journals COVID-19 free medical journals COVID-19 famous journals COVID-19 Google Scholar indexed journals Vaping articles Vaping Research articles Vaping review articles Vaping PubMed articles Vaping PubMed Central articles Vaping 2023 articles Vaping 2024 articles Vaping Scopus articles Vaping impact factor journals Vaping Scopus journals Vaping PubMed journals Vaping medical journals Vaping free journals Vaping best journals Vaping top journals Vaping free medical journals Vaping famous journals Vaping Google Scholar indexed journals tumors articles tumors Research articles tumors review articles tumors PubMed articles tumors PubMed Central articles tumors 2023 articles tumors 2024 articles tumors Scopus articles tumors impact factor journals tumors Scopus journals tumors PubMed journals tumors medical journals tumors free journals tumors best journals tumors top journals tumors free medical journals tumors famous journals tumors Google Scholar indexed journals THC articles THC Research articles THC review articles THC PubMed articles THC PubMed Central articles THC 2023 articles THC 2024 articles THC Scopus articles THC impact factor journals THC Scopus journals THC PubMed journals THC medical journals THC free journals THC best journals THC top journals THC free medical journals THC famous journals THC Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals CT articles CT Research articles CT review articles CT PubMed articles CT PubMed Central articles CT 2023 articles CT 2024 articles CT Scopus articles CT impact factor journals CT Scopus journals CT PubMed journals CT medical journals CT free journals CT best journals CT top journals CT free medical journals CT famous journals CT Google Scholar indexed journals Lung injuries articles Lung injuries Research articles Lung injuries review articles Lung injuries PubMed articles Lung injuries PubMed Central articles Lung injuries 2023 articles Lung injuries 2024 articles Lung injuries Scopus articles Lung injuries impact factor journals Lung injuries Scopus journals Lung injuries PubMed journals Lung injuries medical journals Lung injuries free journals Lung injuries best journals Lung injuries top journals Lung injuries free medical journals Lung injuries famous journals Lung injuries Google Scholar indexed journals Histology articles Histology Research articles Histology review articles Histology PubMed articles Histology PubMed Central articles Histology 2023 articles Histology 2024 articles Histology Scopus articles Histology impact factor journals Histology Scopus journals Histology PubMed journals Histology medical journals Histology free journals Histology best journals Histology top journals Histology free medical journals Histology famous journals Histology Google Scholar indexed journals Psychosis articles Psychosis Research articles Psychosis review articles Psychosis PubMed articles Psychosis PubMed Central articles Psychosis 2023 articles Psychosis 2024 articles Psychosis Scopus articles Psychosis impact factor journals Psychosis Scopus journals Psychosis PubMed journals Psychosis medical journals Psychosis free journals Psychosis best journals Psychosis top journals Psychosis free medical journals Psychosis famous journals Psychosis Google Scholar indexed journals
Article Details
1. Introduction
E-cigarette vaping associated lung injury (EVALI) was first recognized by the Centers for Disease Control (CDC) in August 2019 after receiving reports from state and local health departments of a novel respiratory disease associated with the use of e-cigarettes [1]. In September 2019, the incidence of the disease peaked, with 116 emergency department (ED) visits/million and 215 hospital admissions/week due to EVALI [1].
As of February 18, 2020, there have been 2,807 EVALI hospitalizations reported to the CDC with 68 deaths [2]. While EVALI pathophysiology is subject to debate, the majority of cases occur in patients reporting vaping tetrahydrocannabinol(THC) [1,3]. THC consumption in adolescence and young adulthood is strongly associated with the development of psychotic disorders, including schizophrenia, and is an established preventable risk factor for psychiatric illness [4,5]. This report presents a case of a previously healthy 20-year-old female with new onset psychosis and suicidality, requiring prolonged inpatient psychiatric treatment following a hospitalization for EVALI. To our knowledge this report is the first known case of psychosis and suicidality reported following EVALI. Patient provided consent and authorization for Pine Rest psychiatrists and researchers to access their health information for this case report.
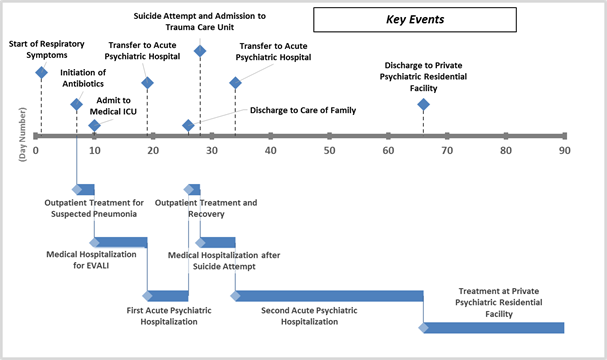
Figure 1: Key events in the patient’s disease progression, treatment and recovery spanning her multiple hospitalizations. The timeline starts at the onset of respiratory symptoms (Day 1). In-text references are made to this timeline throughout the patient case description.
2. Patient Case
Twenty-year-old female received outpatient treatment for suspected pneumonia following one week of symptoms including fever, cough, dyspnea, chest pain, nausea and vomiting (days 1-7), (Figure 1). An outpatient chest x-ray demonstrated bilateral basilar lung infiltrates. Symptoms did not improve with antibiotics. Patient was admitted to the medical intensive care unit 3 days later (day 10) for persistent hypoxia despite breathing treatments in the ED. On admission, repeat chest x-ray and computed tomography with contrast demonstrated worsening bilateral infiltrates (Figures 2 and 3). Labs were consistent with leukocytosis. Patient’s medical history was significant for depression and daily vaping of THC using an electronic cigarette. Outpatient medications including bupropion XL 300 mg daily, lurasidone 60 mg nightly, trazodone 50 mg nightly and amoxicillin-clavulanate 875-125 mg/tablet twice daily, were discontinued and EVALI diagnosis made. During hospitalization (days 10-19), patient received intravenous methylprednisolone per CDC guidelines (days 11-16) and intravenous cefepime for suspected bacterial superinfection. Respiratory support through bilevel positive airway pressure was started and gradually tapered per patient tolerance. Patient was started on a prednisone taper starting at 60 mg daily (day 17) and stabilized and demonstrated improvement in symptoms. On discharge day, patient noted active suicidal thoughts to hospital staff and was subsequently transferred to an inpatient psychiatric hospital for further treatment.
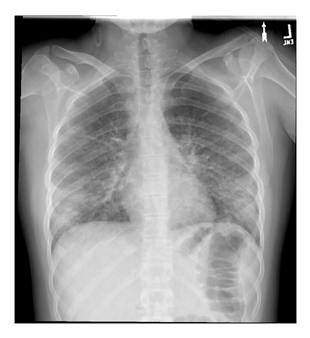
Figure 2: Patient chest x-ray of EVALI with bilateral lung infiltrates.
Courtesy of Bronson Methodist Hospital, Kalamazoo, MI
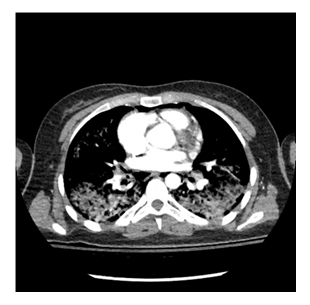
Figure 3: Patient chest computed tomography (CT) with contrast of EVALI with bilateral ground glass opacities.
Courtesy of Bronson Methodist Hospital, Kalamazoo, MI.
On psychiatric hospital admission (day 19), patient described a long history of depression with the current episode precipitated by her mother’s death from opiate overdose four months prior and recent separation from her boyfriend. She endorsed self-medicating her depression over this time with daily THC use. She described suicidal thoughts, history of self-harm by cutting and one previous suicide attempt. She presented with flat affect, disorganized thought patterns and appeared internally preoccupied, although she denied auditory or visual hallucinations. Her primary diagnosis was major depressive disorder, recurrent, severe, with psychotic features, with additional diagnosis of cannabis use disorder, severe. Prednisone taper was continued. Sertraline 25 mg daily was started (day 20) for depression but was discontinued due to facial rash. Due to increasing concern for psychosis, patient was started on olanzapine 2.5 mg nightly (day 24) which resulted in improvement in both psychotic and depressive symptoms. She reported a significant decrease in suicidal thoughts and her father felt that she had markedly improved in her mental state. Given the patient’s apparent improvement, she was determined safe to return home with a plan to follow up with an established outpatient psychiatric provider (day 26).
Upon re-admission to the medical hospital (day 28) following a suicide attempt by stabbing, electrocution, and poisoning two days following discharge from the psychiatric facility, patient reported minimizing her symptoms of depression during the previous psychiatric hospitalization and that she experienced suicidal thoughts throughout that hospitalization. Patient waited for her father to leave for work and then stabbed herself several times in her left breast, abdomen, left wrist and neck. She reported drinking one half bottle of PineSolTM (The Clorox Company, Oakland, CA), and filled a bathtub with water and attempted to electrocute herself by placing cords from electrical appliances in the water. She was found by her father upon returning home and transported to the ED. On presentation, she was somnolent but arousable, tachycardic and hypotensive with blood pressure in the range of 90’s systolic over 50’s diastolic. She was otherwise hemodynamically stable. Exploratory trauma surgery demonstrated a small tracheal laceration and imaging showed a small left pneumothorax. Labs were consistent with anion gap metabolic acidosis, leukocytosis, and hypokalemia. Urine toxicology was positive for cannabinoids, but she denied THC use since before her first medical hospitalization for EVALI. Patient was intubated and monitored in the trauma care unit where she stabilized, and lab abnormalities were corrected. Olanzapine 2.5 mg nightly and the prednisone taper were continued. Following medical stabilization, the patient was again discharged to the inpatient psychiatric facility (day 34).
On the second psychiatric admission, the patient noted worsening suicidal thoughts and demonstrated thought disorganization, paranoia and delusional beliefs. She denied auditory or visual hallucinations. The diagnosis of major depressive disorder, recurrent, severe, with psychotic features was maintained. Olanzapine was discontinued and replaced with quetiapine (day 35) for mood and psychotic symptoms which was titrated to 600 mg nightly. Gabapentin 100 mg was started as needed for anxiety (day 39). Fluoxetine was added for depression (day 48) and titrated to 60 mg daily. Patient demonstrated significant improvement in mood and psychotic symptoms once medications were titrated to effective dosages. Some ongoing passive suicidal thoughts were noted, but the patient’s presentation and affect were significantly improved. She was stable for discharge to continue treatment at a private, long-term residential psychiatric facility (day 66).
3. Discussion
We present the case of a 20-year-old female with a history of daily THC vaping and depression who developed EVALI requiring ICU treatment, with subsequent psychiatric inpatient treatment for suicidal ideation expressed during medical hospitalization. Psychiatrically, the patient was noted to demonstrate new-onset psychotic symptoms in the context of acutely worsening depression and recent lung injury. Patient minimized her symptoms during her first psychiatric hospitalization and attempted suicide by several methods following discharge, resulting in rapid readmission following medical treatment. This onset of psychosis and suicidality is unique, as we are not aware of any previously reported such cases associated with EVALI.
Despite a recent decreasing incidence of acute cases, EVALI continues to be of immense clinical concern as the pathophysiology of the disease remains poorly understood [6]. Theories include lung injury facilitated by acute inflammation, atypical pneumonitis and lipoid or eosinophilic pneumonia [7]. Vitamin E acetate is an additive compound found in e-cigarette solutions that is strongly linked to EVALI, as it has been found in bronchoalveolar lavage fluid in 94% of cases [7]. A related concern is that vaping rates among adolescents and young adults have been increasing. Monitoring the Future Study January 2019 found 41% of high school seniors endorsed vaping of any kind in the past year, compared to 34% in 2016 [8]. In 2019, 21% of high school seniors reported vaping marijuana within the past year as opposed to 10% in 2017 [9]. Considering the increased popularity of vaping THC among adolescents and young adults, there should be continued concern for EVALI as the majority of cases are associated with vaping THC [1,3].
Additionally, there is a well-known link between THC use and the development of psychotic disorders such as schizophrenia, with high potency THC increasing this risk substantially [4,5]. Evidence suggests that those who consume THC are three times as likely as those who do not to develop psychosis, while high potency THC increases this risk sixfold [10]. Drug Enforcement Administration estimates average THC content of vaping solutions at 52% compared to the 13% of cannabis flower [11]. The association between THC use and chronic psychosis is also stronger with heavy or frequent use during adolescence, earlier use, and use of high potency THC [5]. With 9% of 8th grade students reporting ever vaping THC and 4% of seniors reporting near daily use, this population is clearly vulnerable to the development of psychotic disorders secondary to vaping THC [9].
This case highlights concerns associated with vaping high potency THC, and the potential risks vaping poses to both the physical and mental well-being of adolescents and young adults. It serves to further support the literature and understanding of EVALI and its sequelae. The patient’s presentation with significant psychotic symptoms and suicidality in the context of EVALI is novel, warranting further research into the frequency and possible etiology of this phenomenon.
Acknowledgements
Patient provided informed consent for this case report. The medical images were graciously provided by Bronson Methodist Hospital, Kalamazoo, MI.
References
- Krishnasamy VP, Hallowell BD, Ko JY, et al. Update: Characteristics of a Nationwide Outbreak of E-cigarette, or Vaping, Product Use–Associated Lung Injury- United States, August 2019–January 2020. MMWR Morb Mortal Wkly Rep 69 (2020): 90-94.
- CDC, States Update Number of Hospitalized EVALI Cases and EVALI Deaths. Www.cdc.gov, Centers for Disease Control (2020).
- Hartnett KP, Kite-Powell A, Patel MT, et al. Syndromic Surveillance for E-Cigarette, or Vaping, Product Use–Associated Lung Injury. New England Journal of Medicine (2019).
- D'Souza DC, Radhakrishnan R, Sherif M, et al. Cannabinoids and Psychosis. Current Pharmaceutical Design 22 (2016).
- Volkow ND, Swanson JM, Evins AE, et al. Effects of Cannabis Use on Human Behavior, Including Cognition, Motivation, and Psychosis: A Review. JAMA Psychiatry 73 (2016): 292-297.
- Kligerman S, Raptis C, Larsen B, et al. Radiologic, Pathologic, Clinical, and Physiologic Findings of Electronic Cigarette or Vaping Product Use–associated Lung Injury (EVALI): Evolving Knowledge and Remaining Questions. Radiology 294 (2020): 491-505.
- Chand HS, Thivanka M, Wasim M, et al. Pulmonary Toxicity and the Pathophysiology of Electronic Cigarette, or Vaping Product, Use Associated Lung Injury. Frontiers in Pharmacology10 (2020): 1619.
- Monitoring the Future Study: Trends in Prevalence of Various Drugs. Www.drugabuse.gov, National Institute on Drug Abuse.
- Miech RA, Patrick ME, O’Malley PM, et al. Trends in Reported Marijuana Vaping Among US Adolescents, 2017-2019. Jama 323 (2020): 475-476.
- Di Forte M, Quattrone D, Freeman TP, et al. The Contribution of Cannabis Use to Variation in the Incidence of Psychotic Disorder across Europe (EU-GEI): a Multicentre Case-Control Study. Lancet Psychiatry 6 (2019): 427-436.
- Drug Enforcement Administration (DEA). National Drug Threat Assessment Summary. U.S. Department of Justice, DEA (2014).
