Subclavian Steal Syndrome: An Underrecognized Manifestation of Atherosclerosis - Review of the Current Literature with a Case Report
Article Information
Suryansh Bajaj MD1*, Pranav Sharma MD2, Unnati Bhatia MD3
1Research Fellow, Department of Radiology, Maulana Azad Medical College, New Delhi, India
2Clinical Fellow, Department of Vascular and Interventional Radiology, University of Minnesota Medical Center, MN, USA
3Research Fellow, Department of Internal Medicine, Maulana Azad Medical College, New Delhi, India
*Corresponding Author: Suryansh Bajaj MD, Research Fellow, Department of Radiology, Maulana Azad Medical College
2 Bahadurshah Zafar Marg, New Delhi – 110002, India
Received: 16 July 2021; Accepted: 25 August 2021; Published: 10 September 2021
Citation: Suryansh Bajaj, Pranav Sharma, Unnati Bhatia. Subclavian Steal Syndrome: An Underrecognized Manifestation of Atherosclerosis - Review of the Current Literature with a Case Report. Journal of Radiology and Clinical Imaging 4 (2021): 81-92.
View / Download Pdf Share at FacebookAbstract
Subclavian steal is a term used to describe hemodynamics of blood flow in the branches of subclavian artery in patients with an occlusive or stenotic lesion in the proximal subclavian artery. This leads to a retrograde or reversed flow in the ipsilateral vertebral artery supplied by the contralateral vascular bed due to minimal anterograde pressure in the ipsilateral branch. The occlusive lesion is most commonly due to significant atherosclerotic disease. Most patients remain asymptomatic despite having an occlusive lesion. Subclavian steal syndrome (SSS) is the term used when patients develop symptoms related to poor blood supply in the regions supplied by the vertebral artery (posterior circulation symptoms like transient ischemic attacks, vertigo, and dizziness) and/or the brachial artery (arm claudication). Diagnosis is usually made using Doppler ultrasonography (USG), but other cross-sectional imaging modalities have shown increased prevalence than once thought. Most patients are managed conservatively; however symptomatic patients may need additional endovascular or surgical intervention. Herein, we present a patient of SSS who received subclavian artery stenting followed by complete resolution of symptoms and also review the clinical and management aspects of SSS in detail.
Keywords
Subclavian Steal Syndrome; Atherosclerosis; Stents; Angiography
Subclavian Steal Syndrome articles; Atherosclerosis articles; Stents articles; Angiography articles
Subclavian Steal Syndrome articles Subclavian Steal Syndrome Research articles Subclavian Steal Syndrome review articles Subclavian Steal Syndrome PubMed articles Subclavian Steal Syndrome PubMed Central articles Subclavian Steal Syndrome 2023 articles Subclavian Steal Syndrome 2024 articles Subclavian Steal Syndrome Scopus articles Subclavian Steal Syndrome impact factor journals Subclavian Steal Syndrome Scopus journals Subclavian Steal Syndrome PubMed journals Subclavian Steal Syndrome medical journals Subclavian Steal Syndrome free journals Subclavian Steal Syndrome best journals Subclavian Steal Syndrome top journals Subclavian Steal Syndrome free medical journals Subclavian Steal Syndrome famous journals Subclavian Steal Syndrome Google Scholar indexed journals Atherosclerosis articles Atherosclerosis Research articles Atherosclerosis review articles Atherosclerosis PubMed articles Atherosclerosis PubMed Central articles Atherosclerosis 2023 articles Atherosclerosis 2024 articles Atherosclerosis Scopus articles Atherosclerosis impact factor journals Atherosclerosis Scopus journals Atherosclerosis PubMed journals Atherosclerosis medical journals Atherosclerosis free journals Atherosclerosis best journals Atherosclerosis top journals Atherosclerosis free medical journals Atherosclerosis famous journals Atherosclerosis Google Scholar indexed journals Stents articles Stents Research articles Stents review articles Stents PubMed articles Stents PubMed Central articles Stents 2023 articles Stents 2024 articles Stents Scopus articles Stents impact factor journals Stents Scopus journals Stents PubMed journals Stents medical journals Stents free journals Stents best journals Stents top journals Stents free medical journals Stents famous journals Stents Google Scholar indexed journals Angiography articles Angiography Research articles Angiography review articles Angiography PubMed articles Angiography PubMed Central articles Angiography 2023 articles Angiography 2024 articles Angiography Scopus articles Angiography impact factor journals Angiography Scopus journals Angiography PubMed journals Angiography medical journals Angiography free journals Angiography best journals Angiography top journals Angiography free medical journals Angiography famous journals Angiography Google Scholar indexed journals hemodynamics articles hemodynamics Research articles hemodynamics review articles hemodynamics PubMed articles hemodynamics PubMed Central articles hemodynamics 2023 articles hemodynamics 2024 articles hemodynamics Scopus articles hemodynamics impact factor journals hemodynamics Scopus journals hemodynamics PubMed journals hemodynamics medical journals hemodynamics free journals hemodynamics best journals hemodynamics top journals hemodynamics free medical journals hemodynamics famous journals hemodynamics Google Scholar indexed journals brachial artery articles brachial artery Research articles brachial artery review articles brachial artery PubMed articles brachial artery PubMed Central articles brachial artery 2023 articles brachial artery 2024 articles brachial artery Scopus articles brachial artery impact factor journals brachial artery Scopus journals brachial artery PubMed journals brachial artery medical journals brachial artery free journals brachial artery best journals brachial artery top journals brachial artery free medical journals brachial artery famous journals brachial artery Google Scholar indexed journals ultrasonography articles ultrasonography Research articles ultrasonography review articles ultrasonography PubMed articles ultrasonography PubMed Central articles ultrasonography 2023 articles ultrasonography 2024 articles ultrasonography Scopus articles ultrasonography impact factor journals ultrasonography Scopus journals ultrasonography PubMed journals ultrasonography medical journals ultrasonography free journals ultrasonography best journals ultrasonography top journals ultrasonography free medical journals ultrasonography famous journals ultrasonography Google Scholar indexed journals CT angiography articles CT angiography Research articles CT angiography review articles CT angiography PubMed articles CT angiography PubMed Central articles CT angiography 2023 articles CT angiography 2024 articles CT angiography Scopus articles CT angiography impact factor journals CT angiography Scopus journals CT angiography PubMed journals CT angiography medical journals CT angiography free journals CT angiography best journals CT angiography top journals CT angiography free medical journals CT angiography famous journals CT angiography Google Scholar indexed journals MR angiography articles MR angiography Research articles MR angiography review articles MR angiography PubMed articles MR angiography PubMed Central articles MR angiography 2023 articles MR angiography 2024 articles MR angiography Scopus articles MR angiography impact factor journals MR angiography Scopus journals MR angiography PubMed journals MR angiography medical journals MR angiography free journals MR angiography best journals MR angiography top journals MR angiography free medical journals MR angiography famous journals MR angiography Google Scholar indexed journals Doppler USG articles Doppler USG Research articles Doppler USG review articles Doppler USG PubMed articles Doppler USG PubMed Central articles Doppler USG 2023 articles Doppler USG 2024 articles Doppler USG Scopus articles Doppler USG impact factor journals Doppler USG Scopus journals Doppler USG PubMed journals Doppler USG medical journals Doppler USG free journals Doppler USG best journals Doppler USG top journals Doppler USG free medical journals Doppler USG famous journals Doppler USG Google Scholar indexed journals
Article Details
1. Introduction
Subclavian steal syndrome (SSS) is the phenomenon of reversal of blood flow in a branch of the subclavian artery due to a proximal steno-occlusive lesion in the main vessel [1]. Studies have shown the prevalence of SSS is 0.6-6.4% [2, 3]. With the advancements in the non-invasive diagnostic modalities like Doppler ultrasonography (USG), CT angiography (CTA), and MR angiography (MRA), more asymptomatic cases are being diagnosed to have SSS. The majority of patients are asymptomatic [4, 5].The steno-occlusive lesion in the proximal part of the subclavian artery leads to impedance in the distal blood flow to its branches namely the vertebral artery, the internal mammary artery, and the axillary artery. With a decrease in the pressure of the blood flow, the vertebral artery can receive blood from the contralateral vertebral artery through the basilar artery or from the carotid artery due to increased pressures in those vessels leading to a reversal in the blood flow in the ipsilateral vertebral artery. This can further be accentuated by exercising the ipsilateral arm which increases the blood flow to the exercising arm further decreasing the blood flow to the vertebral artery [6].
2. Case Study
A 71-year-old female presented to the emergency department with noticeable dizziness, vertigo and pain in her left arm, and left hand for the past 9 months. She also reported her left hand getting cold and shaky sometimes. She had no history of stroke or transient ischemic attack. No significantcardiachistory. She had multiple emergency visits in the past due to these symptoms. CT angiography of the head and neck was performed which showed no evidence of intracranial hemorrhage, mass, acute infarct, or intracranial anomaly, however, there was severe stenosis at the origin of left subclavian artery. Further workup with carotid doppler ultrasound revealed new flow reversal in the left vertebral artery, suggestingproximal subclavian stenosis and subclavian steal. Due to her lifestyle being severely impaired by these symptoms, multiple visits to the emergency department for dizziness and posterior circulation issues and having suffered left arm/hand ischemic symptoms she underwent a subclavian angiogram. Angiogram showed patent right subclavian and left common carotid arteries with minimal flow in the left subclavian artery withdelayed filling of the subclavian artery through the left vertebral artery suggesting subclavian steal. The left subclavian artery was catheterized with a 5 French Headhunter catheter and 0.035-in angled Glidewire. A baseline left upper extremity angiogram was performed which showed patent left axillary and brachial arteries with slow flow in the forearm and patent radial and ulnar arteries. Measurements were performed from the subclavian artery origin to the takeoff of the left vertebral artery. Subsequently, a 7mm x 37mm Visiproballoon expandable covered stent was deployed in the left subclavian artery. Post stenting angiogram performed through the sheath showed brisk flow through the left subclavian artery and antegrade filling of the left vertebral artery. Completion angiogram of the left arm and forearm showed improved flow in left upper extremity. The patient was discharged on clopedogril for 3 months. One-month follow-up imaging showed improved symptoms and excellent radiographic results.
2.1 Background
SSS can present with a spectrum of symptoms depending on the circulation involved but is most commonly diagnosed incidentally as most patients remain asymptomatic. A large clinical study that involved 7881 patients over a period of 6 years undergoing a Doppler ultrasonography (USG) of the cervical region showed the presence of SSS in only 514 (6.5%) patients, out of which only 38 (7.4%) patients were symptomatic [3]. Another study demonstrated that only 5.3% of the 168 patients having SSS under study were symptomatic [7]. A majority (>90%) of patients can be found to have a complete or at least a partial reversal of flow once the caliber of the subclavian artery is reduced by 50%, however, only a small fraction of those patients are symptomatic [8]. Depending on the severity, SSS can be divided into grade I (decreased anterograde flow), grade II (intermittent retrograde flow), or grade III (persistent retrograde flow). Surprisingly, grade II patients are more commonly symptomatic than grade III patients [9].
2.2 Clinical presentation
Upper limb symptoms can include exercise-induced claudication, muscle weakness, paraesthesias, limb coolness, and rest pain in severe cases. The involvement of vertebrobasilar circulation can lead to syncope, ataxia, diplopia, vertigo, and other posterior circulation symptoms [4, 9, 10]. Patients with internal mammary bypass graft can show a reversal of blood flow from the coronary circulation to the internal mammary artery while exercising the ipsilateral upper limb due to increased requirement of blood in the arm and can present with unstable angina [11]. Reversible cognitive deficits in patients with bilateral SSS have been reported secondary to chronic cerebral hypoperfusion [12]. The physical examination can often elicit a weak radial pulse in the affected limb and patients also show a difference in the blood pressures (BP) in the two arms. The BP differences in the two arms have been directly related to the incidence and severity of the symptoms and the need for intervention [10]. Studies have suggested additional workup for SSS in patients with a BP difference of >15mmHg in the two arms. it has been shown that average difference of 36.9 mmHg in the BP of the two arms in patients with moderate stenosis of the subclavian vessel (>50%) [13]. Auscultation may also reveal a subclavian or a suboccipitalbruit due to the turbulent flow [14]. The clinical symptoms can involve the ipsilateral arm, vertebrobasilar circulation, or coronary circulation (in patients with internal mammary artery bypass graft) and occurs due to ischemia due to poor perfusion.
2.3 Diagnosis
2.3.1 Doppler USG: SSS can be diagnosed on imaging with color Doppler USG, CTA, and MRA. Doppler USG of the cervical region is widely recognized as the initial screening test and can demonstrate the blood flow characteristics in the vertebral artery, show reversal of blood flow along with decreased and turbulent flow in the affected arm, and accentuated peak flow velocity distal to the occlusive lesion in the subclavian artery [5, 15, 16] (Figure 1). In patients with high clinical suspicion showing an absence of retrograde flow in the vertebral artery, a BP cuff test (hyperemia-ischemia test) can be easily performed at the bedside under sonographic examination to reveal any subclinical occult steal at the early stages. In this test, the BP cuff is inflated around the affected arm at a pressure > 20 mmHg than the systolic pressure to cut off the blood supply to the arm. As the cuff is deflated and the blood is preferentially directed towards the ischemic arm, decreased flow or blood flow reversal can be observed on the USG in the vertebral artery in patients with SSS [17]. Kliewer et al proposed that 4 different types of waveforms could be seen based on the degree of steal present. These were classified according to the velocity at the nadir of mid-systolic notch (Figure 2).
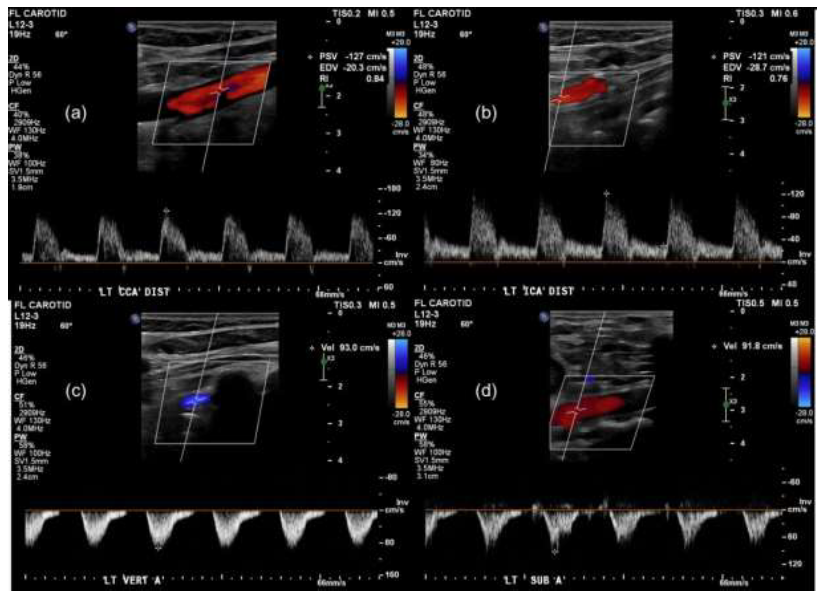
Figure 1: Left carotid doppler ultrasound in 79-year-old female showing antegrade flow in the left common (a) and internal carotid (b) artery and retrograde flow in left vertebral (c) and subclavian (d) arteries.
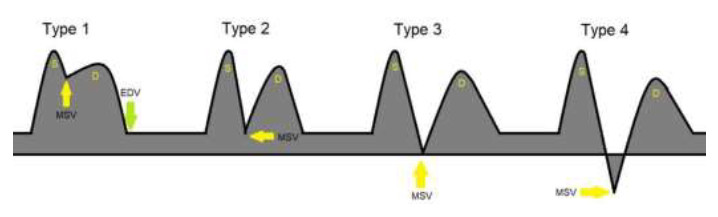
Figure 2: Vertebral artery waveforms depending on the degree of steal: Type 1 demonstrating the mid-systolic velocity (MSV) greater than the end diastolic velocity (EDV). Type 2 demonstrating Mid systolic velocity equal to End diastolic velocity. Type 3 demonstrating Mid systolic velocity equal to End diastolic velocity. Type 4 demonstrating retrograde/inverted Mid systolic velocity.
It was greater than the end-diastolic velocity in type 1 waveform, equal in type 2, at the baseline in type 3, and below the baseline in type 4 [17]. However, there are certain limitations of using Doppler USG. The Sonographic examination may not provide a complete visualization of the subclavian and vertebral arteries. Moreover, the calcification in the atherosclerotic plaque might obstruct the view due to the shadowing effect [18]. Studies have shown that USG cannot accurately differentiate between a severely stenosed vessel from a completely obstructed one [19].
2.4 Cross-sectional imaging
The diagnosis is confirmed on CTA and MRA as these modalities help in better characterization, grading and mapping of the lesion with greater detail of the surrounding soft tissue as well [14]. Additionally, angiographic techniques may also help in the diagnosis of additional subclavian artery pathologies like thrombosis or aneurysm [20]. All patients with uncertain or equivocal findings on USG should undergo CTA or MRA. CTA offers a higher spatial resolution and with advanced processing techniques like maximum-intensity projection and multiplanar reconstruction, the subclavian anatomy and the disease extent can be completely assessed [21, 22] (Figure 3).
Moreover, atherosclerosis in the aortic arch and its other branches can also be assessed (seen as vessel-wall irregularities) along with any intracranial disease (Figure 4). It also provides a detailed visualization of calcifications in the aortic arch and other vessels [23]. However, hemodynamic information cannot be evaluated on CTA. MR imaging can help in evaluating the hemodynamics of the blood flow along with the anatomy of the vascular bed. The blood flow dynamics can be assessed using the phase-contrast technique (to identify the direction of blood flow) and the time-of-flight technique (to identify the anatomy of the vascular blood). Additionally, the time-of-flight technique may also be used without intravenous contrast and thus helps in the diagnosis of SSS especially in patients with renal failure [24, 25]. For the overall assessment, the optimal sequence would include a phase-contrast along with contrast-enhanced MRA. 3-D contrast-enhanced MRA has an even better signal tonoise ratio and provides a higher resolution [26]. Angiography is still considered the gold standard for the diagnosis of SSS and also offers the advantage of being a therapeutic procedure as well (Figure 5). It can also help to elucidate the anatomy and patency of collaterals that are being used in different patients [27].
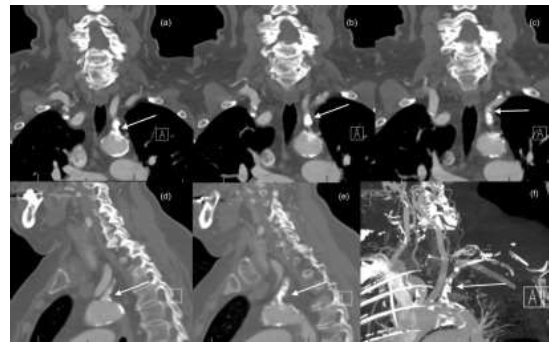
Figure 3: Sequential Coronal (a, b, c), sagittal (c, d) and Maximum Intensity Projection (e) reformatted images of CTA in a 79-year-old female showing severe atherosclerotic narrowing in the left subclavian artery (White arrow).
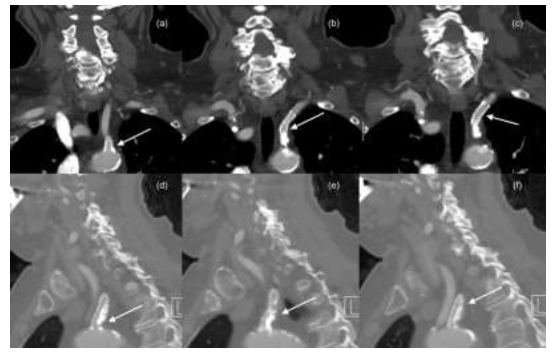
Figure 4: Sequential Coronal (a, b, c) and sagittal (c, d, e) reformatted images of CTA in a 79-year-old female at one month follow-up showing patent left subclavian artery stent (White arrow) with eccentric atherosclerotic plaque pushed towards the posterior wall by the stent.
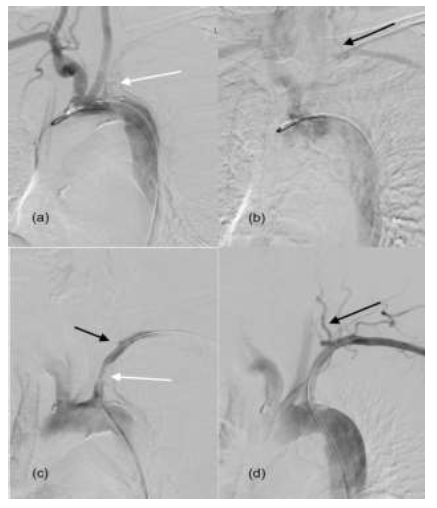
Figure 5: Angiographic images in a 79-year-old female. (a) Aortic angiogram showing opacification of the brachiocephalic artery, left common carotid artery and severe stenosis of the left subclavian artery with faint contrast opacification in the subclavian artery (White arrow) (b) Delayed images on the aortic angiogram showing retrograde flow in the left vertebral artery (black arrow) with delayed opacification of the left subclavian and axillary arteries. (c) Selective catheterization and contrast injection through the sheath at the left subclavian artery ostium shows the area of luminal narrowing and tiny nubbin of contrast reflux in the left vertebral artery (Black arrow). This is used for measurement of the stent. (d) Post stenting left subclavian artery angiogram showing improved luminal diameter of the stenotic segment (White arrow) and antegrade flow in the left vertebral artery (Black arrow).
2.5 Management
2.5.1 Medical: The presence of SSS is highly suggestive of significant atherosclerotic disease in other vascular territories and is associated with an increased risk of total mortality (with a hazard ratio of 1.4) and cardiovascular associated mortality (with a hazard ratio of 1.57) [28]. It warrants a thorough cardiovascular and cerebrovascular workup to look for any significant occlusive atherosclerotic lesions. Asymptomatic patients and patients with mild symptoms are usually managed medically which include aspirin, β-blockers, ACE-inhibitors, and statins, a regimen that is similarly used to manage atherosclerosis in other vascular beds along with lifestyle modification for hypertension, diabetes mellitus, smoking, and alcohol use [29]. It has been shown that only 1.4% of patients with SSS require any therapeutic intervention [3].
2.6 Endovascular and surgical
Traditionally treated with a surgical bypass or a transposition technique, the management of SSS has been completely transformed with endovascular treatment introduced by Kim and Bachman in 1980 [30]. Percutaneous transluminal angioplasty (PTA), or balloon angioplasty, can be performed with or without the placement of stents. PTA has proven to be an excellent alternative to open vascular surgery with a success rate of nearly 95% and comparable long-term patency rates (80-90%) with a much lesser incidence of complications that are seen with surgical options. Previous studies have shown that only 10% of the patients develop restenosis during long-term follow-up and nearly 95% of those lesions can be successfully managed with a repeat PTA [31, 32]. Placement of stents along with PTA can further improve the clinical outcomes in patients with SSS [33]. The algorithm “stent first, then surgery” has garnered immense popularity [34]. Angioplasty without stenting (primary or secondary) was the initial modality tested, with Hebrang et al reporting a technical success rate of 93% and a clinical success rate of 86.5% and 78.8% at 1 and 3 years respectively in a cohort of 52 patients [35]. Despite its early success, this procedure had its share of drawbacks namely a less favorable outcome for a total occlusive disease of the subclavian artery and a considerably high rate of restenosis. Duber et al reported a 57% rate of restenosis or reobstruction in treated patients [36]. To combat this problem, angioplasty with stenting was introduced in the 1900s as a reasonable alternative. The proposed advantages of stenting included prevention of elastic recoil of atherosclerotic lesion and reduction in thrombotic or embolic complications by trapping of the exposed intraluminal plaque [30]. Considerable success was achieved with Sakai et al reporting 89.3% primary and 100% secondary patency rates [37].
However, further randomized controlled clinical trials are required to compare angioplasty with or without stenting to draw a definite conclusion. Irrespective of the technique used, a regular follow-up for 2 years post endovascular therapy is recommended [38]. Drug-eluting stents have also been introduced recently to improve the patency rates. One of the major challenges faced while performing the endovascular treatment is the difficulty in traversing the vessel for the management of chronically occluded subclavian artery. Multiple techniques have been tried to solve this problem, namely bi-directional access, extra-stiff catheters, and an iatrogenically created sub-intimal dissection [30]. Some authors have reported techniques like non-compliant and compliant balloon catheters and distal filters to prevent distal emboli, but that discussion is beyond the scope of this manuscript [39, 40]. Another important thing to consider is the disparity between technical and clinical success with regard to endovascular procedures. This could be due to the fact that the diameter change (morphological parameter) does not always correlate with hemodynamic status (pathophysiological parameter). Soga et al reported the technical success rates for SCA occlusion and stenosis as 100% and 91% respectively, but clinical success rates were shown to be 92% and 80% respectively [41]. A technique to assess hemodynamic status during endovascular therapy for SSS was used by a Chinese study group in 11 patients with SSS undergoing angioplasty with or without stenting. They used a pressure wire to detect the trans-stenosis pressure difference during the procedure, a technique that has been used previously for coronary, renal, and mesenteric vascular beds. They concluded that the pressure difference is closely related to clinical symptoms and degree of steal with values of 6-9 mm of Hg for grade 1 and 2 steals and >10 mm of Hg for ≥grade 3 steal. It was also reported that the gradient of <3 mm of Hg was associated with high post-procedural clinical success [34]. Patients who are not amenable to endovascular treatment require surgical options. The surgical vascular interventions include bypass (axillary-axillary or carotid-subclavian with latter showing lower mortality and recurrence rates) and transposition of SA [38]. Studies have shown that the transposition of SA has the highest long term patency rate (100% at 5 years) [17].
3. Conclusion
SSS is a hemodynamic phenomenon that causes decreased perfusion in the branches of thesubclavian artery and retrograde flow of blood in the vertebral artery due to decreased anterograde flow caused by an occlusive lesion in the subclavian artery. An overwhelming majority of patients remain asymptomatic and those with severe occlusion can present with symptoms involving the vertebrobasilar circulation or ipsilateral arm ischemia. A thorough workup for SSS and other atherosclerotic lesions should be done in all such patients. Most patients can be managed conservatively by medical management. Symptomatic patients are managed with endovascular (PTA with or without stenting) first or surgical management in select cases.
References
- Reivich M, Holling H E, Roberts B, et al. Reversal of blood flow through the vertebral artery and its effect on cerebral circulation. New England Journal of Medicine 265 (1961): 878-885.
- Teng-Yeow Tan, Ulf Schminke, Li-Ming Lien, et al. Subclavian steal syndrome: can the blood pressure difference between arms predict the severity of steal. Journal of Neuroimaging 12 (2002): 131-135.
- Labropoulos N, Nandivada P, Bekelis K. Prevalence and impact of the subclavian steal syndrome. Annals of surgery 252 (2010): 166-170.
- Potter BJ, Pinto DS. Subclavian steal syndrome. Circulation 129 (2014): 2320-2323.
- Georgios Sahsamanis, Georgios Vourliotakis, Konstantinos Pirgakis, et al. Primary Stenting of Right-Sided Subclavian Artery Stenosis Presenting as Subclavian Steal Syndrome: Report of 3 Cases and Literature Review. Annals of vascular surgery 48 (2018): 254. e1-254. e5.
- Lum CF, Ilsen PF, Kawasaki B. Subclavian steal syndrome. Optometry-Journal of the American Optometric Association 75 (2004): 147-160.
- Fields WS, Lemak N A. Joint study of extracranial arterial occlusion: VII. Subclavian steal—a review of 168 cases. Jama 222 (1972): 1139-1143.
- Carl Harper, Paul A Cardullo, Albert K Weyman, et al. Transcranial Doppler ultrasonography of the basilar artery in patients with retrograde vertebral artery flow. Journal of vascular surgery 48 (2008): 859-864.
- Stephen Osiro, Anna Zurada, Jerzy Gielecki, et al. A review of subclavian steal syndrome with clinical correlation. Medical science monitor: international medical journal of experimental and clinical research 18 (2012): RA57.
- Odysseas Kargiotis, Simos Siahos, Apostolos Safouris, et al. Subclavian steal syndrome with or without arterial stenosis: a review. Journal of Neuroimaging 26 (2016): 473-480.
- Schatzl S, Karnik R, Gattermeier M. Coronary subclavian steal syndrome: an extracoronary cause of acute coronary syndrome. Wiener klinische Wochenschrift 125 (2013): 437-438.
- Apostolos Safouris, Anne-Sophie Hambye, Claudine Sculier, et al. Chronic brain hypoperfusion due to multi-vessel extracranial atherosclerotic disease: a potentially reversible cause of cognitive impairment. Journal of Alzheimer's Disease 43 (2015): 23-27.
- Christopher E Clark, Rod S Taylor, Angela C Shore, et al. Association of a difference in systolic blood pressure between arms with vascular disease and mortality: a systematic review and meta-analysis. The Lancet 379 (2012): 905-914.
- Chan-Tack KM. Subclavian steal syndrome: a rare but important cause of syncope. Southern medical journal 94 (2001): 445-447.
- Vecera J, Vojtísek P, Varvarovský I, et al. Non-invasive diagnosis of coronary-subclavian steal: role of the Doppler ultrasound. European Journal of Echocardiography 11 (2010): E34-E34.
- Andrei V Alexandrov, Michael A Sloan, Charles H Tegeler, et al. Practice standards for transcranial Doppler (TCD) ultrasound. Part II. Cliniceral indications and expected outcomes. Journal of neuroimaging 22 (2012): 215-224.
- Kliewer M A, Hertzberg B S, Kim D H, et al. Vertebral artery Doppler waveform changes indicating subclavian steal physiology. American Journal of Roentgenology 174 (2000): 815-819.
- Päivänsalo M, Heikkilä O, Tikkakoski T, et al. Duplex ultrasound in the subclavian steal syndrome. Acta Radiologica 39 (1998): 183-188.
- Sidhu PS. Ultrasound of the carotid and vertebral arteries. British medical bulletin 56 (2000): 346-366.
- Contorni L. The vertebro-vertebral collateral circulation in obliteration of the subclavian artery at its origin. Minerva chirurgica 15 (1960): 268-271.
- Ugur Bozlar, Torel Ogur, Patrick T Norton, et al. CT angiography of the upper extremity arterial system: Part 1—Anatomy, technique, and use in trauma patients. American Journal of Roentgenology 201 (2013): 745-752.
- Rupert W Prokesch 1, Curtis H Coulam, Lawrence C Chow, et al. CT angiography of the subclavian artery: utility of curved planar reformations. Journal of computer assisted tomography 26 (2002): 199-201.
- Ugur Bozlar, Torel Ogur, Minhaj S Khaja, et al. CT angiography of the upper extremity arterial system: part 2—clinical applications beyond trauma patients. American Journal of Roentgenology 201 (2013): 753-763.
- Sheehy N, MacNally S, Smith CS, et al. Contrast-enhanced MR angiography of subclavian steal syndrome: value of the 2D time-of-flight “localizer” sign. American Journal of Roentgenology 185 (2005): 1069-1073.
- Van Grimberge F, Dymarkowski S, Budts W, et al. Role of magnetic resonance in the diagnosis of subclavian steal syndrome. Journal of Magnetic Resonance Imaging: An Official Journal of the International Society for Magnetic Resonance in Medicine 12 (2000): 339-342.
- Teng-Fu Tsao, Kai-Lun Cheng, Chao-Yu Shen, et al. Diagnostic performance of combined contrast-enhanced magnetic resonance angiography and phase-contrast magnetic resonance imaging in suspected subclavian steal syndrome. Canadian Association of Radiologists Journal 67 (2016): 190-201.
- Santschi D R, Frahm C J, Pascale L R, et al. The subclavian steal syndrome: Clinical and angiographic considerations in 74 cases in adults. The Journal of thoracic and cardiovascular surgery 51 (1966): 103-112.
- Victor Aboyans, Aruna Kamineni, Matthew A Allison, et al. The epidemiology of subclavian stenosis and its association with markers of subclinical atherosclerosis: the Multi-Ethnic Study of Atherosclerosis (MESA). Atherosclerosis 211 (2010): 266-270.
- Dharam J Kumbhani, Ph Gabriel Steg, Christopher P Cannon, et al. Adherence to secondary prevention medications and four-year outcomes in outpatients with atherosclerosis. The American journal of medicine 126 (2013): 693-700.
- Vasileios Rafailidis, Xin Li, Ioannis Chryssogonidis, et al. Multimodality imaging and endovascular treatment options of subclavian steal syndrome. Canadian Association of Radiologists Journal 69 (2018): 493-507.
- Jean-Paul P M De Vries, Cara Jager L, Jos C Van den Berg, et al. Durability of percutaneous translum 41 (2005): 19-23.
- Ke-qin Wang, Zhong-gao Wang, Bao-zhong Yang, et al. Long-term results of endovascular therapy for proximal subclavian arterial obstructive lesions. Chinese medical journal 123 (2010): 45-50.
- Aiello F, Morrissey NJ. Open and endovascular management of subclavian and innominate arterial pathology. in Seminars in vascular surgery. Elsevier (2011).
- Da-Wei Chen, Yu-Hai Gao, Jin Shi, et al. Significance of hemodynamic assessment by pressure wire for endovascular therapy of subclavian steal syndrome. Interventional Neuroradiology 26 (2020): 321-328.
- Hebrang A, Maskovic J, Tomac B. Percutaneous transluminal angioplasty of the subclavian arteries: long-term results in 52 patients. AJR. American journal of roentgenology 156 (1991): 1091-1094.
- Christoph Düber, Klaus Jochen Klose, Helmut Kopp, et al. Percutaneous transluminal angioplasty for occlusion of the subclavian artery: short-and long-term results. Cardiovascular and interventional radiology 15 (1992): 205-210.
- Sakai C, Sakai N, Kuroiwa T, et al. Stenting for chronic total occlusion of the proximal subclavian artery. Interventional Neuroradiology 13 (2007): 135-140.
- Luana Antunes Maranha Gatto, Diego do Monte Rodrigues Seabra, Gabriel Angelo Garute Zenatti et al. Endovascular Treatment in the Subclavian Steal Syndrome: Series of 29 Patients. Arquivos Brasileiros de Neurocirurgia: Brazilian Neurosurgery (2021).
- Rami Fakih, Sudeepta Dandapat, Alan Mendez-Ruiz, et al. Combined Transradial and Transfemoral Approach With Ostial Vertebral Balloon Protection for the Treatment of Patients With Subclavian Steal Syndrome. Frontiers in Neurology 11 (2020): 1249.
- Taiki Yamamoto, Tomotaka Ohshima, Kojiro Ishikawa, et al. Feasibility and safety of distal and proximal combined endovascular approach with a balloon-guiding catheter for subclavian artery total occlusion. World neurosurgery, 2017. 100: p. 709. e5-709. e9.
- Yoshimitsu Soga, Yusuke Tomoi, Masahiko Fujihara, et al. Perioperative and long-term outcomes of endovascular treatment for subclavian artery disease from a large multicenter registry. Journal of Endovascular Therapy 22 (2015): 626-633.
