Scientific Communication in the Storm: the War against the Fakedemic on COVID-19 Vaccines
Article Information
Matteo Maria Cati
Department of Economics, University of Bologna, Bologna, 40126, Italy
*Corresponding author: Matteo Maria Cati, Department of Economics, University of Bologna, Bologna, 40126, Italy.
Received: 13 May 2022; Accepted: 19 May 2022; Published: 31 May 2022
Citation: Matteo Maria Cati. Scientific Communication in the Storm: the War against the Fakedemic on COVID-19 Vaccines. Archives of Microbiology and Immunology 6 (2022): 171-187
View / Download Pdf Share at FacebookAbstract
‘Fake news’ may have a strong impact on human behavior, particularly when it is linked to health issues. The flattening of the pandemic curve due to the COVID-19 vaccine is proof of the urgency of convincing the anti-vax people to change their mind. However, why does a fraction of the population, acting against their own interests, become irrational, and why are they reluctant to receive vaccine injection? This paper, tries to find a plausible answer to that question, introducing the ‘link a fear’ bias. In addition, a method, a more severe version of nudging linked to the introduction of restrictive regulations in the job market, is suggested to convince people to vaccinate.
Keywords
Social and behavioral sciences, public health and policy design in the job market, fake-news, COVID-19 and vaccine
Social and behavioral sciences articles, public health and policy design in the job market articles, fake-news articles, COVID-19 articles and vaccine articles
Article Details
1. Introduction
The past few years have seen an unprecedented increase in the spread of social media [1 - 6], along with clear advantages and disadvantages. Even though social media represents a step toward the formation of a global digital community, it also introduces a dark aspect, which is the ease of creating and distributing ‘fake news’. Although the meaning of 'fake news' is intuitive, it is necessary to be careful, as there is disagreement on its definition. Gelfert (2018) argues that ‘fake news’ “should be reserved for cases of deliberate presentation of (typically) false or misleading claims as news”, while Molina, Sundar, Le, and Lee (2021) consider a broader definition, presenting a taxonomy of online content that includes “false news, polarized content, satire, misreporting, commentary, persuasive information, and citizen journalism”, which, in their opinion can be defined as ‘fake news’. Unfortunately, ‘fake news’ may have a strong impact on human behavior, particularly when it is linked [8, 9] to health issues. A striking example of how harmful misinformation can be on human behavior is given by the myriad of 'fake news' (Burki 2020) that gravitates around the COVID-19 vaccination campaign; pushing a fraction of the population in many countries to not want to be vaccinated. Currently, anti-vax groups are demonstrating in various countries, including in Italy. There is a growing consensus in the scientific community, supported by empirical evidence, that increases in COVID infections and ICU admissions occur predominantly in the unvaccinated part of the population.
Italy is one of the first European countries hit by the COVID-19 pandemic, so it can be considered an experimental laboratory. From the empirical data of the Italian National Bureau of Statistics and the task force of the Italian Health Ministry, it is possible to ascertain that the anti-vax population consists of more than 6 million individuals, representing a significant portion of the overall population of 59.2 million people, who need to be convinced to vaccinate in a short period of time. Furthermore, within the anti-vax population, it is necessary to distinguish, between those who are hesitant/reluctant to vaccinate for a variety of reasons (for example, because they prefer to wait and see what happens to those who have already been vaccinated), but who might change their mind, and those who are anti-vaccine regardless of any other consideration, and who would never change their mind [11]. (For more information, see the review study by [10] and the guide of European Centre for Disease Prevention and Control [11]). For Italy and other European countries, convincing their anti-vax populations is an urgent matter, just like another issue: helping African countries vaccinate their population. The urgency of convincing those who are hesitant/reluctant to vaccinate in Italy can be easily seen from the data provided by the Italian Superior Institute of Public Health, summarized in the following table.
Table 1: Relative risk for anti-vax people compared to that of pro - vaccine people with two doses taken within five months - (Source: https://www.epicentro.iss.it/coronavirus/sars-cov-2-sorveglianza-dati)
|
Italy - Relative Risk |
|
|
(for the ANTI - VAX people compared to VAX people with two doses taken within five months) |
|
|
Hospitalization |
10.40% |
|
ICU admission |
16.30% |
|
Death |
9.40% |
Based on Table 1, it is possible to observe that for the ANTI-VAX people, the relative risk of
- hospitalization (h) is 10.4% higher
- ICU admission (icu) is 16.3% higher
- death (d) is 9.4% higher
than the relative risks (h), (icu) and (d) of the VAX people with two doses carried out within five months. This is also true for vaccine-hesitant and anti-vaccine people. The question is why, despite evidence, a fraction of the population, particularly those who are hesitant, decides not to get vaccinated. Moreover, is there anything governments can do to get them to change their minds, at least for the hesitant/reluctant subgroup of the anti-vax people?
2. The ‘link a fear’ bias and the war against the ‘fakedemic’ on the COVID – 19 vaccine
Answering the previous questions is not easy, and it is closely linked to the ability to ensure an effective public health communication strategy [12]. In a recent report OECD [17] experts noticed that
“…an outbreak of disinformation (i.e., false or misleading information, deliberately circulated to cause harm) about COVID-19 has spread quickly, widely and inexpensively across the internet, endangering lives and hampering the recovery”.
Clearly, scientific communication [16] and related information campaigns on COVID-19 vaccines carried out in various countries do not seem to affect the beliefs of the anti-vax people, while colliding with the large amounts of fake news circulating on the internet and in particular on social media, such as Facebook, Instagram and Twitter [13]. The Italian SISC (Social Investment Studies Center – known in Italy as Censis [28]) has drawn up a list (table 2) of the most common fake news that circulate among the anti-vax population through social media [14, 15] as summarized in the following table with the percentage of diffusion within the population.
Table 2: List of most common fake news on COVID-19 vaccines within the anti-vax population and percentage of diffusion. Source: CENSIS - 55th Report on the social situation of the country (Dec. 2021)
|
The vaccine is an experimental drug and Italians are acting as guinea pigs |
31.40% |
|
Science creates more harm than good |
12.70% |
|
Vaccines are useless and ineffective |
10.90% |
|
Covid-19 does not exist |
5.90% |
The problem is that, in the comparison between scientific communication and fake news, part of the population, whose beliefs are represented by the anti-vax movements in Italy and in other countries such as the UK and Ireland [19], tends to give greater credibility to the latter rather than to the former [18]. There are different reasons for this belief. On the one hand, many people, and particularly those that associate with the anti-vax movements, question the reliability of science. Because these people “fueled mainly by conspiracy theories, false beliefs, lack of confidence in the approval process of the vaccines and others” [17] think as follows:
- “Science creates more harm than good”; as indicated in the survey by the Italian SISC on the most common fake news.
- Science is conditioned by power; this vision seems to be the result of an erroneous simplification of the complex mosaic that relates scientific research to politics [19].
On the other hand, there are a myriad of personal beliefs sometimes linked to superstitions. Faced with the irrationality of the choice of not getting vaccinated, it is difficult to draw rational conclusions on the reasons for the aforementioned choice. However, in this article, I argue that one of the reasons for the decision to not receive the vaccine can be the ‘fear of the unknown’. In this case, the unknown being a new vaccine to treat a lethal virus that caused the pandemic. As a result, people with extreme fear may have a distorted view of the world and consequently can make equally distorted decisions (i.e., not to get vaccinated). This has to do with many different aspects, such as concerns about the Covid-19 vaccine, cultural preparation, trust in institutions, family education, personal beliefs, the possibility of accessing correct scientific information, misreading correct scientific information, or exposure to incorrect scientific information. There is a long tradition in the literature of assessing the existence of a link between perceptual biases, related biased decisions, and extreme fear. As Teachman, Stefanucci, Clerkin, Cody & Proffitt 2008 [29] noticed in their 2008 study, there is:
“…initial evidence that perceptual biases are associated with extreme fear. This suggests fearful persons are not just interpreting the world in a threatening way, but may actually see it differently.”
Additional evidence of such a strong relationship between extreme fear, inaccurate and false information [20], and irrational behavior, which might have had a bad epidemiological impact on the population during health emergencies, can be found in the recent West African Ebola Epidemic [23] between 2014 – 2016. As Ornell et al. (2016) noted:
“ease of access to communication technologies and the transmission of sensational, inaccurate or false information can increase harmful social reactions.”
In this way, 'fake news' and its diffusion on the internet can cause a chain reaction in some people and determine their decision not to get vaccinated (Special issue on the role of internet use in the decision to get vaccinated, Journal Vaccine, 2012). When the amount of 'fake news' becomes exorbitant, in other words, when there is a real pandemic of 'fake news', that is a 'fakedemic', it becomes difficult to govern. How can we fight against this other pandemic, the 'fakedemic', and the harmful effects it has on the decision to get vaccinated? If we accept the idea that one of the reasons for choosing not to vaccinate is the fear of an unknown vaccine, a possible strategy could be to use a greater fear to convince the anti-vax population to vaccinate. In other words, we could try to reduce a bias with a counter bias. Fearful people try to convince themselves that not to get vaccinated was the right choice, based on a psychological mechanism, as follows.
- First, they try to rationalize their choice by associating their decision with information they consider reliable. Unfortunately, most of the time, such information consists of false beliefs, incorrect scientific communication or an incorrect interpretation.
- Second, they try to find consensus in groups of people who share their opinion.
In this setting, “fake news”, such as those enlisted in Table 2, fuel fears and the decision not to get vaccinated.
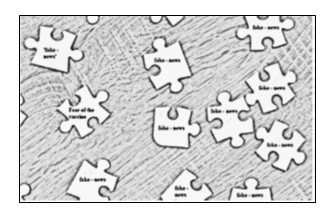
The mechanism that I define and introduce in this article is illustrated in Figures 1.a and 1.b. The 'link a fear' bias is in fact a counter-bias that might be used to counter the biased decision of not getting vaccinated. The ‘link a fear bias’ can be seen as the result of the encounter between two elements: on the one side the fear of the vaccine (i.e. the fear of the unknown) and on the other side the 'fake news on the vaccine' (i.e. ‘fake news’ about the unknown). The result of this encounter is the decision not to get vaccinated and the construction of a 'comfort zone' within which the anti-vax people meet. In Figure 1.a, where the ‘fear of the vaccine’ and 'fake news' are represented by the pieces of a puzzle, the fear of the unknown (i.e., fear of the new anti-Covid vaccine) finds fertile soil in the 'fake news' setting.
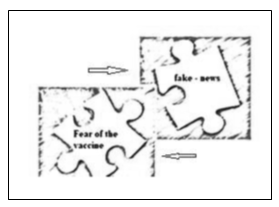
In Figure 1.b, the 'link a fear bias' is represented by the interlocking pieces of the puzzle, ‘fear of the vaccine’ and 'fake news’. For example, an individual's irrational fear of the vaccine finds solace in the 'fake news' about the capability of the vaccine to change an individual's genetic profile. Those who are afraid of the vaccine can, even unconsciously, conclude that their fears and therefore their decision not to get vaccinated are supported by evidence, without examining whether the evidence is factual or not.
Other people may confuse the notions of correlation and causality and think that some accidents (i.e. deaths of individuals after vaccinations) were caused by the vaccine and therefore decide not to get vaccinated. As the phrase goes, "correlation is not causation." That is, just because two events happened close in time to each other (e.g., death after getting vaccinated), it does not necessarily mean that one event (vaccination) causes the other event (death). Correlations between two things can be caused by a third factor (for example, an allergy to the vaccine) that affects both factors. In statistics, such a factor is called a confounder (a variable that affects both the independent and the dependent variables, but in reality, the association is spurious). The fact that there are several reasons for not getting vaccinated makes it difficult to find a single solution to the problem.
3. Can the ‘link a fear biases be pacified?
Professor Richard Thaler [30], was awarded the Nobel price in Economics in 2017. He has explained to us some of the biases that get in the way of good decision-making and why individuals sometimes act against their own interests. [31] Have shown to the world that governments can use ‘nudges’ [31] to subtly change “how choices are offered” [25] and to design new policy lines aimed at modifying the behavior of individuals for a good purpose (for example, following a healthy diet). The grave global health crisis triggered by the COVID-19 pandemic necessitated a large-scale change in behavior. In this setting, behavioral sciences can be utilized to align individual behaviors with recommendations from health experts. An example of the effective use of ‘nudging’ to motivate a healthier behavior was placing hand sanitizer dispensers in accessible places and indicating their presence with visual signals.
Sunstein (2020) [1] underlines the importance of investing resources in ‘nudging’, noticing that the Behavioral Insights Team in the UK has studied what worked more effectively to convince people to wear the mask (during the time when masks were not mandatory) and to remind people of the importance of social distancing.
During the worst periods of the second and third waves of the pandemic in the U.S.A., Mullainathan and Thaler (2020) [33] suggested that to ramp up hospitals’ patient capacity, policy-makers should relax “some regulations that may be limiting the supply of health-care personnel and equipment”. We all know that, however, the gravity of the situation due to the pandemic has prompted various governments to issue regulations and laws aimed at imposing behavioral mandates on the population that suited the pandemic emergency. For instance, introduction of the so-called lockdown and curfews were among the most striking behavioral restrictions.
Now that the pandemic curve has flattened in many countries due to widespread vaccination, the next major step is to convince the fraction of the population who do not want to get vaccinated. The fourth wave of the pandemic is proving that the countries with the lowest percentage of vaccination suffer the most. Thaler (2021) [27] observes that governments have “a broad range of responses” at their disposal. For example, an extreme government mandate is for people to get vaccinated or “face severe punishment”. At the other extreme, governments may use ‘nudges,’ such as “informing people about the benefits of vaccinations and making it as easy as possible to get a shot”, or “gently guide people without requirements or economic incentives”. At this stage, it is clear that “information campaigns” can be a valid tool to “stress the safety and efficacy of the vaccines” and “it is important to target the messages at the most hesitant groups.” However, it seems also clear that ‘nudging’ may not be enough to convince unvaccinated individuals. The delicate and urgent matter is to balance the health urgency with the economic urgency, considering the uncertainty that still characterizes the world situation as well as the possible and unpredictable emergence of new variants of the virus or of the possible aggravation or attrition of the pandemic.
3. The Italian experiment
A solution to the fear of getting vaccinated that seems to have an impact on the anti-vax people in Italy so far is the mixed strategy consisting of:
- Nudging, or a toolkit given by “choice architecture” to gently convince people to behave virtuously (for example, visual cues in restaurants and public places that people can enter only if they’re vaccinated).
- Introduction of a more restrictive regulation through the so-called Green Pass [34] (i.e., a sort of digital passport on COVID-19 vaccination with a QR code that can be easily scanned) that is now mandatory in the job market for people working in both the private and public sectors.
The Italian government introduced an even stronger version of the Green Pass for the winter holidays, namely, the Super Green Pass. To be able to go to work and have a social, cultural and sports life, Italians now have two options:
- The Basic Green Pass, issued upon a negative COVID-19 test result.
- The Super Green Pass, which cannot be obtained via a negative COVID-19 test result but only with vaccination, which has significant repercussions for people who are unvaccinated.
The following table lists the range of activities (from work to social) that can be carried out according to the type of green pass.
Table 3: Activities allowed in Italy with the green pass in the different zones [35] - Source: Ministry of Health
It is evident from Table 3 that people who are not vaccinated can perform only a very limited number of activities both in the workplace and in the social, cultural and sport settings of their workplaces.
In Italy, legislation, without formally providing for the mandatory nature of the vaccine, implicitly obliges those who are not vaccinated to be vaccinated to carry out their work and social activities.
The combination of
- this composite strategy (nudging and stricter regulation),
- together with the recent announcement made by the World Health Organization about the new Omicron variant
had a strong impact on the population, causing a considerable increase in overall vaccinations and in first doses in Italy, as illustrated in Table 4:
Table 4: Daily number of total inoculations and first doses of the COVID-19 vaccination. November – December 2021 - Source: Ministry of Health (Italian Government) - https://www.governo.it/it/cscovid19/report-vaccini/ - https://github.com/italia/covid19-opendata-vaccini
|
The Italian Government introduces the so called Super green pass (from Dec. 6th to Jan. 15) |
(total inoculation) 315495 Wed. Nov. 24 th, 2021 (the day of the announcement) |
(first dose) 22355 Wed. Nov 24 th, 2021 |
(total inoculation) 519322 Mon. Dec. 9 th, 2021 (after 16 days) |
(first dose) 36757 Mon. Dec. 9 th, 2021 (after 16 days) |
|
The World Health Organization announces the new variant Omicron |
(total inoculation) 310975 Sat. Nov. 27 th, 2021 (the day after the announcement) |
(first dose) 29880 Sat. Nov. 27 th, 2021 |
(total inoculation) 519322 Mon. Dec. 9 th, 2021 (after 14 days) |
(first dose) 36757 Mon. Dec. 9 th, 2021 (after 14 days) |
On December 9th, 2021, i.e., sixteen days after the announcement (Nov. 24th, 2021) by the Italian Government regarding the stricter regulation of Basic Green Pass and Super Green Pass, and fourteen days (Nov. 27th, 2021) after the announcement of the new variant Omicron by the World Health Organization, the total inoculation and the first doses increased by more than 6%.
Even though it is not possible to make a comparison with the same period of the previous year, (the start of the vaccination campaign was Dec. 27th, 2020, the so-called “vaccine day”) and the two events described are too recent to have enough empirical evidence to work with, we can easily notice from Table 5 (spanning from Aug. 16th, 2021 to Sept. 30th, 2021) that during and after Summer 2021:
- The number of total inoculations decreased consistently. The total inoculations on August 16th, 2021, were 235,103; while on September 30th, 2021, total inoculations diminished to 203,997 (i.e., more than a 13% decrease in 45 days).
- Similarly, the number of first doses of the vaccine also The number of first doses on August 16th, 2021 was 130,114, while on September 30th, 2021, it diminished to 87,582 (i.e., more than a 33% decrease in the same time span of 45 days).
Table 5: Daily number of total inoculations and first doses of the COVID-19 vaccine. August – September 2021 Source: Ministry of Health (Italian Government) - https://www.governo.it/it/cscovid19/report-vaccini/- https://github.com/italia/covid19-opendata-vaccini
|
From the third week of August 2021 |
(total inoculation) 235103 Mon. Aug. 16th, 2021 |
(first dose) 130114 Mon. Aug. 16 th, 2021 |
|
To the fourth week of September 2021 |
(total inoculation) 203997 Thu. Sept. 30th 2021 |
(first dose) 87582 Thu. Sept. 16th, 2021 |
However, in Table 6 (spanning from Oct. 1st, 2021 to Nov. 22nd, 2021), it is notable that during Autumn 2021:
- The number of total inoculations slightly increased. Total inoculations on Oct. 1st, 2021 were 176,590; while on Nov. 22nd, 2021 total inoculations increased to 203,997 (i.e. approximately a 15% increase in 53 days).
- Similar to Table 4, the number of first doses of the vaccine consistently decreased. The first doses on Oct. 1st, 2021 were 68,847; while on Nov. 22nd, 2021 the first doses diminished to 22,579 (i.e., more than a 66% decrease in the same time span of 53 days).
Table 6: Daily number of total inoculations and first doses of the COVID-19 vaccine. October – November 2021 - Source: Ministry of Health (Italian Government) - https://www.governo.it/it/cscovid19/report-vaccini/ - https://github.com/italia/covid19-opendata-vaccini
|
From the first week of October 2021 |
(total inoculation) |
(first dose) |
|
To |
(total inoculation) |
(first dose) |
Important evidence emerges from the count of the number of third doses (the so-called boosters), which are particularly relevant to fight against the new variant Omicron. Some experts are already asserting that a new variant of the COVID-19 vaccine is needed for this purpose
Table 7: Number of third doses (boosters) of the COVID-19 vaccine. November – December 2021 - Source: Ministry of Health (Italian Government) - https://www.governo.it/it/cscovid19/report-vaccini/ - https://github.com/italia/covid19-opendata-vaccini
|
(third dose) |
(third dose) |
|
(third dose) |
(third dose) |
From Table 7, it can be noticed that the number of inoculation of third doses has increased by 3.314.000 units in 23 days, from Nov. 4th, 2021 to Nov. 27th, 2021. That means an increase of boosters in approximately 5.75% of the overall population (i.e. from 2.086.000 to 5.400.000, or from 3.5% to 9.24% of the overall population). After the Italian Government and the World Health Organization announcements, in sixteen days, from Nov. 27th, 2021 to Dec. 13th, 2021, the number of third doses has increased by 10.05% (i.e. from 5.400.000 to 11.605.340, or from 9.25% to 19.3% of the overall population).
In other words, the percentage increase of the number of inoculations of the third doses in approximately two weeks after the two announcements doubled with respect to the number of inoculations of the third doses in the four-week period of time previously considered. Clearly, to draw stronger conclusions more data is needed about the ongoing vaccinations. Still, leaving aside considerations such that:
- people during the summer might be on vacation;
- at the beginning of the cold season (coinciding in Italy with the end of October and the beginning of November), people are more worried about viruses, and therefore vaccinations slightly increase;
- the number of first doses has naturally decreased since an increasing fraction of the population has already been vaccinated;
- the third-dose vaccination campaign has only recently started;
It is clear from the data of Table 4 that there was a positive ‘announcement effect’ on the number of total inoculations and of first doses within 14-16 days; since both the total and first dose vaccine administrations increased by more than 6%. As a result, at first glance, the fear of getting vaccinated (‘link a fear bias’) seems to have been overcome for a growing number of the anti-vax people, at least for the hesitant ones, due to the grater fear of losing their job, the restrictions on their social, cultural, sport life and the announcement about the new variant.
4. Concluding remarks
Fear of vaccination can distort the choices of a fraction of the population, and it has found a fertile soil ('link a fear' bias) in the 'fake - news' pandemic. A possible method to solve the problem may be to counter the biased decision of not getting vaccinated with a combination of 'nudging' and stricter regulation. The regulations could grant access to people in the labor market or in social, cultural and sporting activities only if they are vaccinated, and the regulations could enforce showing digital certificates of vaccination.
Disclosures
The author has no conflicts of interest to declare.
Funding
The author has not received any funding
Acknowledgements
None
Data Availability Statement (DAS)
|
Availability of data |
Data Availability Statement |
Policy |
|
Data openly available in a public repository that does not issue DOIs |
The data that support the findings of this study are openly available at |
All |
|
Italian Ministry of Health |
||
|
https://opendatadpc.maps.arcgis.com/apps/dashboards/b0c68bce2cce478eaac82fe38d4138b1 |
||
|
https://www.salute.gov.it/portale/nuovocoronavirus/dettaglioContenutiNuovoCoronavirus.jsp?lingua=italiano&id=5452&area=nuovoCoronavirus&menu=vuoto |
||
|
https://www.salute.gov.it/portale/nuovocoronavirus/homeNuovoCoronavirus.jsp |
||
|
https://www.salute.gov.it/portale/nuovocoronavirus/dettaglioContenutiNuovoCoronavirus.jsp?lingua=italiano&id=5452&area=nuovoCoronavirus&menu=vuoto |
||
|
https://www.salute.gov.it/portale/nuovocoronavirus/dettaglioContenutiNuovoCoronavirus.jsp?lingua=italiano&id=5351&area=nuovoCoronavirus&menu=vuoto |
||
|
https://www.salute.gov.it/portale/nuovocoronavirus/dettaglioContenutiNuovoCoronavirus.jsp?lingua=italiano&id=5452&area=nuovoCoronavirus&menu=vuoto |
||
|
https://github.com/italia/covid19-opendata-vaccini |
||
|
https://github.com/italia/covid19-opendata vaccini/blame/a78dc2fcafee4792ad5d054a8b1985037fffd4e7/dati/somministrazioni-vaccini-summary-latest.csv |
||
|
Italian Government |
||
|
https://www.governo.it/it/cscovid19/report-vaccini/ |
||
|
Istituto Superiore della Sanità (Italian Ministry of Health) |
||
|
I vaccini anti COVID-19 (iss.it) |
||
|
Piano nazionale di vaccinazione COVID-19 (iss.it) |
||
|
Gimbe Foundation – Evidence for Health |
||
|
https://coronavirus.gimbe.org/ |
||
References
- Collins K, Shiffman D, Rock J. How Are Scientists Using Social Media in the Workplace? PLoS ONE 11 (2016): e0162680.
- Ahlqvist T, Bäck A, Halonen M, Heinonen S. Social media roadmaps: exploring the futures triggered by social media. VTT Tiedotteita Valtion Teknillinen Tutkimuskeskus, (2008).
- Danah m. boyd, Nicole B. Ellison, Social Network Sites: Definition, History, and Scholarship, Journal of Computer-Mediated Communication 13 (2007): 210–230.
- Haythornthwaite C. Social networks and Internet connectivity effects, Information, Communication & Society 8 (2005): 125-147.
- Kaplan AM, Haenlein M. Users of the world, unite! The challenges and opportunities of Social Media, Business Horizons 53 (2010): 59-68.
- Darling ES, Shiffman D, Côté IM, Drew JA. The role of Twitter in the life cycle of a scientific publication. Ideas Ecol Evol 6 (2013): 32–43.
- Thaler AD, Zelnio KA, Freitag A, MacPherson R, Shiffman D, Bik H, et al. Digital environmentalism: tools and strategies for the evolving online ecosystem. SAGE Reference–Environmental Leadership: A Reference Handbook. London: SAGE Publications, (2011).
- Merchant R & Asch D. Protecting the Value of Medical Science in the Age of Social Media and “Fake News”, JAMA 320 (2018): 2415-2416.
- Wang Y, McKee M, Torbica A, Stuckler D. Systematic literature review on the spread of health-related misinformation on social media. Soc Sci Med, 240 (2019): 112552.
- Johnson SB, Park HS, Gross CP, Yu JB. Complementary medicine, refusal of conventional cancer therapy, and survival among patients with curable cancers. JAMA Oncol, 4 (2018): 1375-1381.
- Larson HJ, Jarrett C, Eckersberger E, Smith D, Paterson P. Understanding vaccine hesitancy around vaccines and vaccination from a global perspective: A systematic review of published literature, 2007–2012, 32 (2014): 2150-2159.
- European Centre for Disease Prevention and Control. Let’s talk about hesitancy. Stockholm: ECDC; (2016).
- Edwards DJ Ensuring Effective Public Health Communication: Insights and Modeling Efforts From Theories of Behavioral Economics, Heuristics, and Behavioral Analysis for Decision Making Under Risk. Front. Psychol 12 (2021): 715159.
- Firdaus SN, Ding C, Sadeghian A. Retweet Prediction based on Topic, Emotion and Personality, Online Social Networks and Media 25 (2021): 100165.
- Andreadis S, Antzoulatos G, Mavropoulos T, Giannakeris P, et al. A social media analytics platform visualising the spread of COVID-19 in Italy via exploitation of automatically geotagged tweets, Online Social Networks and Media 23 (2021): 100134.
- Rimal RN, Lapinski MK. Why health communication is important in public health. Bull World Health Organ Apr 87 (2009): 247-247a.
- OECD (2020). Combatting COVID-19 disinformation on online platforms, OECD Paris.
- Guarino S, Pierri F, Di Giovanni M, Celestini A. Information disorders during the COVID-19 infodemic: The case of Italian Facebook, Online Social Networks and Media 22 (2021): 100124.
- Murphy J, Vallières F, Bentall RP et al. Psychological characteristics associated with COVID-19 vaccine hesitancy and resistance in Ireland and the United Kingdom. Nat Commun 12 (2021): 29.
- Ransing R, Dashi E, Rehman S, Chepure A, Mehta V, et al. COVID-19 anti-vaccine movement and mental health: Challenges and the way forward, Asian Journal of Psychiatry 58 (2021): 102614.
- Fähnrich B and Ruser A. ‘Operator, please’—Connecting truth and power at the science-policy interface. JCOM – Journal of Science Communication 18 (2019).
- Sell TK, Hosangadi D & Trotochaud M. Misinformation and the US Ebola communication crisis: analyzing the veracity and content of social media messages related to a fear-inducing infectious disease outbreak. BMC Public Health 20 (2020): 550.
- Bell BP, Damon IK, Jernigan DB et al. Overview, Control Strategies, and Lessons Learned in the CDC Response to the 2014–2016 Ebola Epidemic. Morbidity and Mortality Weekly Report 65 (2016): 4–11.
- Benartzi S, Beshears J, Katherine L, Milkman, Sunstein CR, Thaler RH, et al. Should Governments Invest More in Nudging? Psychological Science 28 (2017): 1041–1055.
- Patel M. Test behavioural nudges to boost COVID immunization. Nature 590 (2021): 185.
- Thaler RH, Sunstein CR. Nudge: Improving Decision about Health, Wealth and Happiness. London: Penguin (2008).
- Thaler RH. More Than Nudges Are Needed to End the Pandemic. New York: New York Times Company (2021).
- Censis, Center for Social Investments Studies, is a socioeconomic research institute founded in 1964 and that in 1973 became a Foundation recognized by the Decree of the President of the Italian Republic n, 712 of 11 October (1973).
- Teachman BA, Stefanucci JK, Clerkin EM, Cody MW, & Proffitt DR. A new mode of fear expression: Perceptual bias in height fear. Emotion 8 (2020): 296–301.
- Thaler RH. From Cashews to Nudges: The Evolution of Behavioral Economics. Nobel Prize Lecture, December, (2017).
- Thaler RH, Sunstein CR. Nudge. New Haven & London: Yale University Press; (2008).
- Wofford B. Questions for Cass Sunstein: Can We “Nudge” to a Better Pandemic Policy? Washingtonian, July 13 (2020).
- Cockrell J. How Can Relaxing Regulations Improve the US’ Pandemic Response? Chicago Booth. The University of Chicago Booth School of Business (2020).
- The so called Covid-19 Green Pass, following the definition of the Italian Health Ministry “attests to one of the following criteria: vaccination against Covid-19, a negative antigenic or molecular swab taken within the last 48 hours, or recovery from the infection.
- Regions and Autonomous Provinces are classified in Italy into four areas - white (safest), yellow (safer), orange (medium risk) and red (high risk) - corresponding to the Covid-19 different risk scenarios.
- Calabresi, Guido and Bobbitt, Philip Chase Tragic Choices. Books. 83. W.W. Norton and Company New York (1978).
- Thaler RH. Misbehaving: The Making of Behavioral Economics. New York: W. W. Norton & Company (2015).
- Thaler RH, Mental Accounting and Consumer Choice. Marketing Science 4 (1985): 199–214.
- Thaler RH, Mental Accounting Matters. Journal of Behavioral Decision Making 12 (1999): 183–206.
- Thaler RH, and Shefrin HR. An Economic Theory of Self-Control. Journal of Political Economy 89 (1981): 392–410.
- Thaler RH, and Sunstein CR. Libertarian Paternalism. American Economic Review 93 (2003): 175–179.
- Tversky A, and Kahneman D. Judgment Under Uncertainty: Heuristics and Biases.” Science: (1974): 1124–1131.
- Sunstein CR. People Prefer System 2 Nudges (Kind of) Duke LJ 66 (2016): 121–168.
- Sunstein CR, Reisch LA, Rauber J. A worldwide consensus on nudging? Not quite, but almost. Regulation & Governance 12 (2018): 3–22.
- Sunstein CR. The Ethics of Influence: Government in the Age of Behavioral Science. Cambridge University Press (2016).
- Sunstein CR. Nudges vs. Shoves. Harvard Law Review Forum 127 (2013): 210.
- Szaszi B, Palinkas A, Palfi B, Szollosi A, Aczel B. A Systematic Scoping Review of the Choice Architecture Movement: Toward Understanding When and Why Nudges Work. Journal of Behavioral Decision Making 31 (2018): 355–366.
- Duda´s L, Szànto´ R. Nudging in the time of coronavirus? Comparing public support for soft and hard preventive measures, highlighting the role of risk perception and experience. PLoS ONE 16 (2021).
- Bavel JJV, Baicker K, Boggio PS, Capraro V, Cichocka A, et al. Using social and behavioural science to support COVID-19 pandemic response. Nature Human Behaviour 4 (2020): 460–471.
- Burki T. The online anti-vaccine movement in the age of COVID-19. Lancet Digital Health 2 (2020): e504 – e505.
- Chilvers J & Kearnes M. (Eds.) Remaking Participation: Science, Environment and Emergent Publics. Routledge (2015).
- Bucchi M, & Trench B. (Eds.) Routledge Handbook of Public Communication of Science and Technology: Second edition Routledge (2014).
- Davies SR, Hara N. Public Science in a Wired World: How Online Media Are Shaping Science Communication. Science Communication 39 (2017): 563-568.
- Adam DI, Kramer, Guillory JE, Hancock JT Experimental evidence of massive-scale emotional contagion through social networks of the National Academy of Sciences Jun 111 (2014): 8788-8790.
- Bond R, Fariss C, Jones J et al. A 61-million-person experiment in social influence and political mobilization. Nature 489 (2012): 295–298.
- Lunn P et al. Using behavioural science to help fight the coronavirus. ESRI Working Paper No 2020 (656).
- Kim DA et al. Social network targeting to maximise population behaviour change: a cluster randomised controlled trial. Lancet 386 (2015): 145–153.
- Christakis NA & Fowler JH Social contagion theory: examining dynamic social networks and human behavior. Stat. Med 32 (2013): 556–577.
- Halpern D. Inside the Nudge Unit: How Small Changes Can Make a Big Difference (Random House) (2015).
- Gelfand MJ, Harrington JR & Jackson JC. Perspect. Psychol Sci, 12 (2017): 800–809.
- Ellis EG. The coronavirus outbreak is a petridish for conspiracy theories. Wired (2020).
- Leman P & Cinnirella M. A major event has a major cause: evidence for the role of heuristics in reasoning about conspiracy theories. Soc. Psychol. Rev 9 (2007): 18–28.
- Graeupner D & Coman A. The dark side of meaning-making: how social exclusion leads to superstitious thinking. J. Exp. Soc. Psychol 69 (2017): 218–222.
- Frenkel S, Alba D & Zhong R. Surge of virus misinformation stumps Facebook and Twitter. The New York Times (2020).
- Guess A, Nagler J & Tucker J Less than you think: prevalence and predictors of fake news dissemination on Facebook. Sci. Adv 5 (2019): u4586.
- Swire B & Ecker UKH. Misinformation and its correction: Cognitive mechanisms and recommendations for mass communication in Misinformation and Mass Audiences (eds. Southwell, B. G., Thorson, E. A. & Sheble, L.) (2018): 195–2011. (University of Texas Press).
- Pennycook G, McPhetres J, Zhang Y, Lu JG, Rand DG. Fighting COVID-19 Misinformation on Social Media: Experimental Evidence for a Scalable Accuracy-Nudge Intervention. Psychological Science 31 (2020): 770-780
- Bronstein MV, Pennycook G, Bear A, Rand DG. & Cannon TD. Belief in fake news is associated with delusionality, dogmatism, religious fundamentalism, and reduced analytic thinking. J. Appl. Res. Mem. Cogn 8 (2019): 108–117.
- Dias N, Pennycook G & Rand DG. Emphasizing publishers does not effectively reduce susceptibility to misinformation on social media. The Harvard Kennedy School Misinformation Review1 January 1 (2020).
- Ferreira CM et al. Communication in health: a new time Food Sci. Technol 37 (2017).
- Paschalides D, Christodoulou C, Orphanou K, Andreou R, Kornilakis A, et al. Check-It: A plugin for detecting fake news on the web, Online Social Networks and Media 25 (2021): 100156.
- Khan T, Michalas A, Akhunzada A. Fake news outbreak 2021: Can we stop the viral spread?, Journal of Network and Computer Applications 190 (2021): 103112.
- Khan T, Michalas A. Trust and believe - should we? evaluating the trustworthiness of twitter users. In: 2020 IEEE 19th International Conference on Trust, Security and Privacy in Computing and Communications (TrustCom). IEEE Computer Society, Los Alamitos, CA, USA (2020): 1791–1800.
- Ornell F, Schuch JB, Sordi AO, Kessler FHP. ‘‘Pandemic fear’’ and COVID-19: mental health burden and strategies. Brazilian Journal of Psychiatry 42 (2020): 232-235.
- Reardon S. Ebola's mental-health wounds linger in Africa. Nature 5 (2015): 13-4.
- Shultz JM, Cooper JL, Baingana F, Oquendo MA, Espinel Z, Althouse BM, et al. The role of fear-related behaviors in the 2013-2016 West Africa ebola virus disease outbreak. Curr Psychiatry Rep 18 (2016): 104.
- Wang Y, McKee M, Torbica A, Stuckler D. Systematic literature review on the spread of health-related misinformation on social media. Soc Sci Med 240 (2019): 112552.
- Shigemura J, Ursano RJ, Morganstein JC, Kurosawa M, Benedek DM. Public responses to the novel 2019 coronavirus (2019-nCoV) in Japan: mental health consequences and target populations Psychiatry Clin Neurosci 74 (2020): 281-2.
- Special Issue: The Role of Internet Use in Vaccination Decisions Edited by Cornelia Betsch, Katharina Sachse 30 (2012): 3723-3818.
- Hengen Kristina M, Alpers Georg W. What’s the Risk? Fearful Individuals Generally Overestimate Negative Outcomes and They Dread Outcomes of Specific Events, Frontiers in Psychology 10 (2019): 1676.
- Zaman J, Struyf D, Ceulemans E et al. Probing the role of perception in fear generalization. Sci Rep 9 (2019): 10026.
- Terraneo M, Lombi L, & Bradby H. Depressive symptoms and perception of risk during the first wave of the COVID-19 pandemic: A web-based cross-country comparative survey. Sociology of Health & Illness 43 (2021): 1660–1681.
- Eder SJ, Steyrl D, Stefanczyk MM, Pieniak M, Marti´nez Molina J, Pesout O, et al. Predicting fear and perceived health during the COVID-19 pandemic using machine learning: A cross-national longitudinal study. PLoS ONE 16 (2021): e0247997.
- Schudy A, Zurek K, Wisniewska M, Piejka A, Gaweda L, and Okruszek L. Mental Well-Being During Pandemic: The Role of Cognitive Biases and Emotion Regulation Strategies in Risk Perception and Affective Response to COVID-19. Front. Psychiatry 11 (2020): 589973.
- Maganga GD, Kapetshi J., Berthet N, et al. Ebola virus disease in the Democratic Republic of Congo. N Engl J Med 371 (2014): 2083-2091.
- Daniel A. Erku, Sewunet A. Belachew, Solomon Abrha, Mahipal Sinnollareddy, Jackson Thomas, Kathryn J. Steadman, Wubshet H. Tesfaye When fear and misinformation go viral: Pharmacists' role in deterring medication misinformation during the 'infodemic' surrounding COVID-19, Research in Social and Administrative Pharmacy 17 (2021): 1954-1963.
- Betsch C, Sachse K.: Dr. Jekyll or Mr. Hyde? (How) the Internet influences vaccination decisions: Recent evidence and tentative guidelines for online vaccine communication, Vaccine, Special Issue (2012): 3723-3726.
- Betsch C, Brewer NT, Brocard P, Davies P. et al Opportunities and challenges of Web 2.0 for vaccination decisions, Vaccine, Special Issue (2012): 3727-3733.
- Witteman HO, Zikmund-Fisher BJ. The defining characteristics of Web 2.0 and their potential influence in the online vaccination debate, Vaccine, Special Issue (2012): 3734-3740.
- Kata A. Anti-vaccine activists, Web 2.0, and the postmodern paradigm – An overview of tactics and tropes used online by the anti-vaccination movement. Vaccine, Special Issue (2012): 3778-3789.
- Reyna VF. Risk perception and communication in vaccination decisions: A fuzzy-trace theory approach, Vaccine, Special Issue (2012): 3790-3797.
- Connolly T. and Reb J. Toward interactive, Internet-based decision aid for vaccination decisions: Better information alone is not enough, Vaccine, Special Issue (2012): 3778 – 3789.
- Appel G, Grewal L, Hadi, R. et al. The future of social media in marketing. J. of the Acad. Mark Sci, 48 (2020): 79–95.
- Cinelli M, Quattrociocchi W, Galeazzi A. et al. The COVID-19 social media infodemic. Sci Rep 10 (2020): 16598.