Schistosomiasis Co-morbid with Posterior Reversible Encephalopathy Syndrome and HIV/AIDS
Article Information
Willem van Aswegen, Dali Magazi*
Department of Neurology, Sefako Makgatho Health Sciences University, South Africa
*Corresponding Author: Dali Magazi, MBBCh, MMed (Neuro), FCP (Neuro)SA, Department of Neurology, Sefako Makgatho Health Sciences University, PO Box 108, Medunsa, 0204, South Africa
Received: 06 January 2021; Accepted: 25 January 2021; Published: 05 February 2021
Citation: Willem van Aswegen, Dali Magazi. Schistosomiasis Co-morbid with Posterior Reversible Encephalopathy Syndrome and HIV/AIDS. Archives of Clinical and Medical Case Reports 5 (2021): 210-215.
View / Download Pdf Share at FacebookAbstract
We describe a young female patient with schistosomiasis, HIV and posterior reversible encephalopathy syndrome (PRES) from a South African township. There are overlapping pathophysiological molecular mechanisms between schistosomiasis and PRES and yet no previous descriptions linking the two conditions. This presentation highlights the need for further investigation of this possible link. It also serves to emphasize the need for an updated geographical distribution map of schistosomiasis in South Africa. The interplay between HIV and schistosomiasis continues to be an important study subject in endemic areas.
Keywords
Schistosomiasis; HIV; PRES; South Africa
Article Details
Abbreviations:
NTD- Neglected Tropical Diseases; CRP- C-Reactive Protein; HIV- Human immunodeficiency virus; CD4- Cluster of differentiation 4; ICAM 1- Intercellular adhesion molecule 1
1. Introduction
A German physician, Theodor Bilharz described a condition that was to bear his name from autopsy findings of an Egyptian patient in 1851. There are however,earlier descriptions from ancient Egyptian papyri of what is reminiscent of bilharzia, including literature from times of ancient Mesopotamia [1]. In the early 2000’s, the world health organisation (WHO) recognised a group of communicable conditions affecting rural poor communities which were not prioritized on the global agenda, aptly referred to as neglected tropical diseases (NTDs). Schistosomiasis or Bilharzia being amongst the NTDs, affects approximately 230 million people, worldwide, an estimated 85% being in sub-Saharan Africa where the principal species are schistosoma hematobium and mansoni excreted in urine and faeces, respectively. Ambitious goals by the WHO were to have schistosomiasis controlled by 2020 and to have a “world free of schistosomiasis” by 2025 [2].
The parasites causing schistosomiasis are waterborne, found in rivers, ponds and dams with a well described lifecycle from the time the fluke penetrates human skin to the excretion of the eggs in urine or faeces. An estimated 20 – 55% of the eggs are successfully excreted, the rest lodge in various organs including the liver, kidney, brain and even the eyes, resulting in granulomas with fibrotic damage [3]. A cascade of immunological events are triggered by the schistosome in the host cell, including activation of type 2 cytokines like interleukins 4 & 5 and a host of others [4]. Mortality from schistosomiasis continues to be significant, the global estimates being 200 000 per annum [5].
South Africa has approximately 4.5 million people infected with schistosomiasis, the north eastern parts covering a quarter of the country being traditionally endemic [6]. The geographic spread of schistosomiasis in South Africa however, has been shown to be in flux, influenced by various factors, including rural-urban migration and cross border movements from endemic regions [7]. Weather patterns are another identified determinant of schistosomal geographical distribution, meaning that global climate change could possibly have an impact on present day patterns of schistosomiasis [8].
2. Index Case Presentation
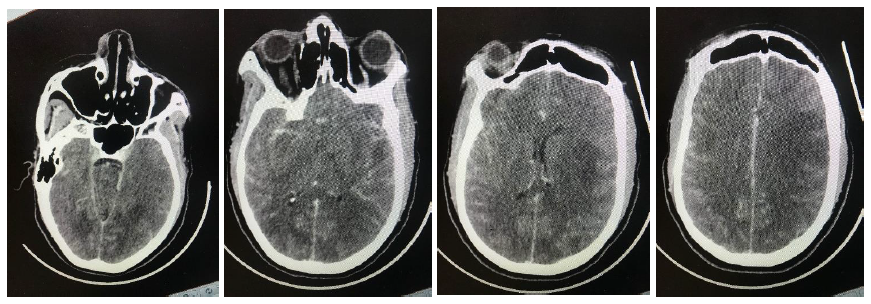
A 31-year old female from Soshanguve, one of the north western townships of Pretoria, South Africa was found unresponsive. She had previously complained of a headache followed by erratic behavior over a period of two weeks. The Glasgow coma scale on hospital arrival was 7/15. She also had bilateral papilloedema with globally absent deep tendon reflexes. A brain CT scan showed extensive hypodense areas in both cerebral hemispheres, a picture suggestive of posterior reversible encephalopathy syndrome (PRES) shown in the figure below. She also had an iron deficiency anemia (hemoglobin of 9.5g/l) with a high C-reactive protein (CRP) of 54 mg/l. She was further diagnosed positive for the human immunodeficiency virus (HIV) with a CD4 count of 13 cells/ µl and a viral load of 284 772 copies/ml. A lumbar puncture was deferred due to clinical and radiological evidence of raised intracranial pressure and was treated empirically for bacterial and cryptococcal meningitis, the latter owing to the profoundly low immunity status. Urine microscopy showed Schistosoma haematobium ova and hematuria for which an antihelminth was commenced.
3. Discussion
At a molecular level, there exists an overlap in the host response to schistosomal infection and the underlying pathophysiology of PRES. Schistosomiasis results in a demonstrable upregulation of intercellular adhesion molecule1 (ICAM 1), a transmembrane protein found on the surface of leukocytes and endothelium with a resultant increase in vessel permeability [9]. Cytokine activation and an overexpression of ICAM 1 have also been demonstrated and hypothesized to be an important causative contributor for PRES [10]. The latter is a radiologically diagnosed acute condition characterized by bilateral cerebral edema, usually maximal in the occipital lobes with no identifiable solid brain lesions (eg: abscess, granulomas or tumors). Neuroschistosomiasis is a rare manifestation of the helminth infection with a spectrum of clinical manifestations including headaches, confusion and coma [11]. Present day definitions of neuroschistosomiasis are not necessarily hinged on isolation of the helminth in the central nervous system (peripheral isolation and neurological clinical features sufficing), leading to some authors pointing out a gap in diagnostic standards [12]. A literature search on schistosomiasis and PRES did not yield results. HIV has however, been described with PRES and postulated to be largely from endothelial damage in the brain [13]. The index patient could have had endothelial dysfunction as a result of contributory mechanisms from an interplay between HIV and schistosomiasis.
Sub-Saharan Africa, endemic for both HIV and schistosomiasis prompted studies to investigate a potential interaction between that retrovirus and bilharzia. Urogenital ulceration from schistosomiasis has been described to make females particularly vulnerable to contracting HIV during intercourse [14]. The hematuria and iron deficiency anemia seen in our patient was explained by the schistosoma hematobium infection. Upregulation of CD4 receptors which are docking stations for HIV has been demonstrated with schistosomiasis suggesting further interplay between the two conditions at a molecular level. People living with HIV and Schistosomal infection as a co-morbidity have also been associated with higher viral load than those without schistosomiasis [15]. This however, is not universal with some studies finding no such association [16]. The sub-Saharan African region stands to benefit from an in-depth understanding of the interplay between schistosoma and HIV, in the interest of having informed preventative programs.
The index patient serves to highlight that city areas like Pretoria, the capital city of South Africa could be having a silently growing problem of schistosomiasis. Our patient was a rural-urban migrant from an area endemic for schistosomiasis. Informal settlements along the banks of rivers, in townships on the outskirts of cities (eg: Jukskei & Moretele rivers in Alexandra and Mamelodi townships, Johannesburg and Pretoria, respectively) are a possible risk for a surge of schistosomiasis in previously quiescent areas.
4. Conclusion
The authors realize that a single case report is not enough to prove an association between schistosomiasis and PRES. This is however, a call for further robust studies to interrogate a possible link between the two conditions. An updated national disease burden registry for schistosomiasis would be important for South Africa in order to inform government preventative programs way ahead of possible future epidemics. A better understanding of a possible link between schistosomiasis and HIV is of paramount importance in endemic areas. A complete global elimination of Bilharzia, worldwide as per the WHO goals can only come about from well grounded preventative programs which in turn would be from an informed standpoint.
Acknowledgments
Not applicable
Funding
No special funding was received
Disclosure and Conflict of Interests
None of the authors have any disclosures to make with no conflict of interest
Ethical Approval
Permission was sought and granted by the patient’s family to publish the presentation anonymously.
Ethical Publication Statement
We confirm that we have read the Journal’s position on issues involved in ethical publication and affirm that this report is consistent with those guidelines.
References
- Di Bella S, Riccardi N, Giacobbe DR, et al. History of schistosomiasis (bilharziasis) in humans: from Egyptian medical papyri to molecular biology on mummies. Pathogens and Global Health 112 (2018): 268-273.
- Deol AK, Fleming FM, Calvo-Urbano B, et al. Schistosomiasis—assessing progress toward the 2020 and 2025 global goals. New England Journal of Medicine 381 (2019): 2519-2528.
- Costain AH, MacDonald AS, Smits HH. Schistosome egg migration: mechanisms, pathogenesis and host immune responses. Frontiers in Immunology 9 (2018): 3042.
- de Oliveira Fraga LA, Torrero MN, Tocheva AS, et al. Induction of type 2 responses by schistosome worms during prepatent infection. The Journal of Infectious Diseases 201 (2010): 464-472.
- Verjee MA. Schistosomiasis: Still a cause of significant morbidity and mortality. Research and reports in Tropical Medicine 10 (2019): 153.
- Magaisa K, Taylor M, Kjetland EF, Naidoo PJ. A review of the control of schistosomiasis in South Africa. South African Journal of Science 111 (2015): 1-6.
- Appleton CC, Ngxongo SM, Braack LE, et al. Schistosoma mansoni in migrants entering South Africa from Moçambique--a threat to public health in north-eastern KwaZulu-Natal?. South African Medical Journal 86 (1996): 350-353.
- Moodley I, Kleinschmidt I, Sharp B, et al. Temperature-suitability maps for schistosomiasis in South Africa. Annals of Tropical Medicine & Parasitology 97 (2003): 617-627.
- Ritter DM, McKerrow JH. Intercellular adhesion molecule 1 is the major adhesion molecule expressed during schistosome granuloma formation. Infection and Immunity 64 (1996): 4706-4713.
- Marra A, Vargas M, Striano P, et al. Posterior reversible encephalopathy syndrome: the endothelial hypotheses. Medical Hypotheses 82 (2014): 619-622.
- Ferrari TC, Moreira PR. Neuroschistosomiasis: clinical symptoms and pathogenesis. The Lancet Neurology 10 (2011): 853-864.
- Härter G, Frickmann H, Zenk S, et al. Diagnosis of neuroschistosomiasis by antibody specificity index and semi-quantitative real-time PCR from cerebrospinal fluid and serum. Journal of Medical Microbiology 63 (2014): 309-312.
- Nightingale S, Wood C, Ainsworth J. The posterior reversible encephalopathy syndrome in HIV infection. Case Reports 2012 (2012): bcr0120125647.
- Wall KM, Kilembe W, Vwalika B, et al. Schistosomiasis is associated with incident HIV transmission and death in Zambia. PLoS Neglected Tropical Diseases 12 (2018): e0006902.
- Walson JL, Herrin BR, John-Stewart G. Deworming helminth co-infected individuals for delaying HIV disease progression. The Cochrane Database of Systematic Reviews 8 (2009): CD006419.
- Bochner AF, Secor WE, Baeten JM, et al. Schistosomiasis was not associated with higher HIV-1 plasma or genital set point viral loads among HIV seroconverters from four cohort studies. PLoS Neglected Tropical Diseases 13 (2019): e0007886.