Retrospective Assessment of Smart Watch Haptic Feedback to Treat Nightmares in the U.S. Military
Article Information
Robertson BD1,2, Werner JK2,3, Pearce TR1, Rayl KR1, Wargo EF1, Karlin DR1,4,5,Collen JF2,3, Assefa SZ6, Dan AC7, and Kuperan S3
1Nightware, Inc.
2Uniformed Services University of the Health Sciences, Bethesda, MD
3Walter Reed National Military Medical Center, Bethesda, MD
4MindMed, Inc.
5Tufts University School of Medicine, Medford, MA
6Alexander T. Augusta Military Medical Center, Ft. Belvoir, VA
7Marriotts Ridge High School, Marriottsville, MD
*Corresponding Author: Robertson, NightWare, Inc, USA
Received: 27 October 2023; Accepted: 06 November 2023; Published: 14 November 2023
Citation: Robertson BD., Werner JK,, Pearce TR, Rayl KR, Wargo EF, Karlin DR,Collen JF, Assefa SZ, Dan AC, and Kuperan S. Retrospective Assessment of Smart Watch Haptic Feedback to Treat Nightmares in The U.S. Military.Journal of Psychiatry and Psychiatric Disorders 7 (2023): 186-191.
View / Download Pdf Share at FacebookAbstract
Objective: Nightmares are a common co-morbid condition among patients with mental health disorders and sleep disturbances. Patients with Nightmare Disorder (ND) or Post-Traumatic Stress Disorder (PTSD)-related nightmares experience sleep fragmentation, reduced sleep quality, and insufficient sleep quantity. NightWare is an FDA-cleared digital medical device that monitors patients’ heart rate and movement during sleep to predict the patient may be entering into or experiencing a nightmare. It delivers vibrotactile feedback to the patient which is believed to interrupt the nightmares and thus improve sleep quality in patients with PTSD-related nightmares or ND.
Methods: Active-duty United States military patients who were prescribed NightWare during their regular clinical care provided feedback to their durable medical equipment (DME) provider regarding improvement in sleep quality and reduction of nightmares. We evaluated their response to treatment with NightWare in this real-world treatment paradigm.
Results: In this retrospective study, we found that 68.4% of patients reported a good or excellent response to treatment, and 92.9% of patients reported at least some improvement in sleep quality and/or a reduction in nightmares with the use of NightWare. Only 7.1% of patients reported that the device was disrupting their sleep or was ineffective for them.
Conclusions: This qualitative study of real-world patients demonstrated improved sleep quality and a clinically significant reduction or elimination of nightmares with the use of NightWare therapy for both PTSD-related nightmares and ND.
Keywords
Nightmare Disorder; Post-Traumatic Stress Disorder
Nightmare Disorder articles; Post-Traumatic Stress Disorder articles
Nightmare Disorder articles Nightmare Disorder Research articles Nightmare Disorder review articles Nightmare Disorder PubMed articles Nightmare Disorder PubMed Central articles Nightmare Disorder 2023 articles Nightmare Disorder 2024 articles Nightmare Disorder Scopus articles Nightmare Disorder impact factor journals Nightmare Disorder Scopus journals Nightmare Disorder PubMed journals Nightmare Disorder medical journals Nightmare Disorder free journals Nightmare Disorder best journals Nightmare Disorder top journals Nightmare Disorder free medical journals Nightmare Disorder famous journals Nightmare Disorder Google Scholar indexed journals Post-Traumatic Stress Disorder articles Post-Traumatic Stress Disorder Research articles Post-Traumatic Stress Disorder review articles Post-Traumatic Stress Disorder PubMed articles Post-Traumatic Stress Disorder PubMed Central articles Post-Traumatic Stress Disorder 2023 articles Post-Traumatic Stress Disorder 2024 articles Post-Traumatic Stress Disorder Scopus articles Post-Traumatic Stress Disorder impact factor journals Post-Traumatic Stress Disorder Scopus journals Post-Traumatic Stress Disorder PubMed journals Post-Traumatic Stress Disorder medical journals Post-Traumatic Stress Disorder free journals Post-Traumatic Stress Disorder best journals Post-Traumatic Stress Disorder top journals Post-Traumatic Stress Disorder free medical journals Post-Traumatic Stress Disorder famous journals Post-Traumatic Stress Disorder Google Scholar indexed journals Minneapolis articles Minneapolis Research articles Minneapolis review articles Minneapolis PubMed articles Minneapolis PubMed Central articles Minneapolis 2023 articles Minneapolis 2024 articles Minneapolis Scopus articles Minneapolis impact factor journals Minneapolis Scopus journals Minneapolis PubMed journals Minneapolis medical journals Minneapolis free journals Minneapolis best journals Minneapolis top journals Minneapolis free medical journals Minneapolis famous journals Minneapolis Google Scholar indexed journals pharmacotherapy articles pharmacotherapy Research articles pharmacotherapy review articles pharmacotherapy PubMed articles pharmacotherapy PubMed Central articles pharmacotherapy 2023 articles pharmacotherapy 2024 articles pharmacotherapy Scopus articles pharmacotherapy impact factor journals pharmacotherapy Scopus journals pharmacotherapy PubMed journals pharmacotherapy medical journals pharmacotherapy free journals pharmacotherapy best journals pharmacotherapy top journals pharmacotherapy free medical journals pharmacotherapy famous journals pharmacotherapy Google Scholar indexed journals sleep articles sleep Research articles sleep review articles sleep PubMed articles sleep PubMed Central articles sleep 2023 articles sleep 2024 articles sleep Scopus articles sleep impact factor journals sleep Scopus journals sleep PubMed journals sleep medical journals sleep free journals sleep best journals sleep top journals sleep free medical journals sleep famous journals sleep Google Scholar indexed journals Durable Medical Equipment articles Durable Medical Equipment Research articles Durable Medical Equipment review articles Durable Medical Equipment PubMed articles Durable Medical Equipment PubMed Central articles Durable Medical Equipment 2023 articles Durable Medical Equipment 2024 articles Durable Medical Equipment Scopus articles Durable Medical Equipment impact factor journals Durable Medical Equipment Scopus journals Durable Medical Equipment PubMed journals Durable Medical Equipment medical journals Durable Medical Equipment free journals Durable Medical Equipment best journals Durable Medical Equipment top journals Durable Medical Equipment free medical journals Durable Medical Equipment famous journals Durable Medical Equipment Google Scholar indexed journals imagery rehearsal therapy articles imagery rehearsal therapy Research articles imagery rehearsal therapy review articles imagery rehearsal therapy PubMed articles imagery rehearsal therapy PubMed Central articles imagery rehearsal therapy 2023 articles imagery rehearsal therapy 2024 articles imagery rehearsal therapy Scopus articles imagery rehearsal therapy impact factor journals imagery rehearsal therapy Scopus journals imagery rehearsal therapy PubMed journals imagery rehearsal therapy medical journals imagery rehearsal therapy free journals imagery rehearsal therapy best journals imagery rehearsal therapy top journals imagery rehearsal therapy free medical journals imagery rehearsal therapy famous journals imagery rehearsal therapy Google Scholar indexed journals Smart Watch articles Smart Watch Research articles Smart Watch review articles Smart Watch PubMed articles Smart Watch PubMed Central articles Smart Watch 2023 articles Smart Watch 2024 articles Smart Watch Scopus articles Smart Watch impact factor journals Smart Watch Scopus journals Smart Watch PubMed journals Smart Watch medical journals Smart Watch free journals Smart Watch best journals Smart Watch top journals Smart Watch free medical journals Smart Watch famous journals Smart Watch Google Scholar indexed journals FDA articles FDA Research articles FDA review articles FDA PubMed articles FDA PubMed Central articles FDA 2023 articles FDA 2024 articles FDA Scopus articles FDA impact factor journals FDA Scopus journals FDA PubMed journals FDA medical journals FDA free journals FDA best journals FDA top journals FDA free medical journals FDA famous journals FDA Google Scholar indexed journals NightWare therapy articles NightWare therapy Research articles NightWare therapy review articles NightWare therapy PubMed articles NightWare therapy PubMed Central articles NightWare therapy 2023 articles NightWare therapy 2024 articles NightWare therapy Scopus articles NightWare therapy impact factor journals NightWare therapy Scopus journals NightWare therapy PubMed journals NightWare therapy medical journals NightWare therapy free journals NightWare therapy best journals NightWare therapy top journals NightWare therapy free medical journals NightWare therapy famous journals NightWare therapy Google Scholar indexed journals
Article Details
1. Introduction
Nightmare Disorder (ND) is a prevalent parasomnia and is defined by extremely dysphoric well-remembered dreams that tend to consist of threats to survival, security, or physical integrity. [1] ND is often comorbid with other mental health conditions such as Post-Traumatic Stress Disorder (PTSD), anxiety, and depression. Clinically significant nightmares, typically defined as nightmares occurring one or more times per week, affect from 0.9% to 6.8% of the adult population. [1–5] The majority of individuals afflicted with PTSD experience more frequent trauma-related nightmares, occurring in approximately 50-90% of the PTSD population. [6–8] Frequent nightmares occur in 52.4% of combat veterans with PTSD, while only occurring in 4.8% of combat veterans without PTSD and 3.4% of civilians. [7] Frequent, severe nightmares in the setting of PTSD, especially with co-morbid insomnia and sleep apnea, are associated with worse outcomes for global PTSD symptoms. [9] While several treatments are available for ND, including medication and psychotherapy, some patients may not respond to or are unable to tolerate side effects from these traditional treatments. Patients face a number of barriers accessing mental health care in healthcare systems throughout the United States. There is a shortage of behavioral sleep medicine providers across the US. [10] In the Department of Defense (DoD), there is a high demand for and often inadequate numbers of mental health care providers. [11] Therefore, although treatments such as imagery rehearsal therapy and lucid dreaming can be effective for nightmare disorder, access to providers willing and able to provide such interventions competently is severely limited, in most cases, to a small number of tertiary care institutions. In the case of imagery rehearsal therapy, although it is recommended by a position paper about nightmare disorder treatment,[12] many patients cannot or will not participate in this therapy. [13] Many patients with nightmares are treated with prazosin, an alpha-adrenergic antagonist, which is an American Academy of Sleep Medicine (AASM) recommended therapy for nightmare disorder. [14] However, many patients with PTSD-related nightmare disorder prove refractory to prazosin or are unable to tolerate prazosin-related side effects, which can include orthostasis. [15,16] Many of these patients are already on multiple medications for the treatment of mood disorders and sleep related symptoms, and additional medications can compound adverse effects on sleep architecture and daytime function. NightWare (Minneapolis, MN) is a treatment for PTSD-associated nightmares and ND. NightWare is an FDA-cleared class II medical device based on the Apple Watch platform. It monitors patients’ sympathetic activation during sleep to calculate a real-time stress index, predicts when the patient may be having a nightmare, and delivers vibrotactile feedback in response. The vibrations from the watch are believed to interrupt the nightmares and, thus, improve sleep quality. [17] The intervention threshold is usually determined automatically and adapted over time for each participant by a proprietary algorithm. In a recent randomized, sham-controlled clinical trial of NightWare in 65 military veterans, Davenport and Werner found that there was a significant improvement in sleep quality and nightmares with both sham and active treatment, while intention-to-treat analysis revealed a trend suggesting treatment may have been superior to sham. Furthermore, in a post-hoc analysis that evaluated only those who used the watch at least 50% (comparable in each arm) of the time, there was a clear, significant improvement in active treatment compared to sham in multiple outcomes, including sleep quality, nightmare severity, and frequency. [17]
NightWare has been prescribed to active-duty military members since 2021. The prescribers of this device work primarily in mental health and sleep medicine, although other specialties have also been prescribing this device. Psychologists, Licensed Clinical Social Workers, psychiatrists, sleep medicine physicians, family practice physicians, PM&R clinicians, and neurologists have all prescribed NightWare. This paper reports their patients’ response to this treatment.
2. Methods
From June 2021 to July 2023, 1,131 patients have been prescribed NightWare in the DoD. Of these, 983 patients received devices supplied by one Durable Medical Equipment (DME) provider and were contacted for feedback. The DME provider contacted the patients on the following schedule: An initial call was placed once the patient received the device; follow-up calls were then made weekly for the first 4 weeks of treatment, and every 30 days for 5 months thereafter. The patients in this study were asked if they 1) had improved sleep quality and 2) had resolution or reduction of their nightmares to a frequency of <1 time per week after starting NightWare. All patients who provided feedback regarding their response to treatment were included in this analysis. The patients' responses were used to assign each patient a category, using the criteria shown in Table 1 below. A positive response was recorded if the patient indicated that the treatment device prevented or noticeably decreased their nightmares and improved sleep quality. A negative response was recorded if the patient indicated that the vibrations disturbed their sleep, if the device did not prevent nightmares, or if they/their provider opted to discontinue use. Some patients reported technical problems or user interface issues related to using the device. This information was collected and placed into 3 categories: training and education issues (e.g., not understanding how to set the time on the device), hardware/software problems, and problems with the vibrations being too disruptive to sleep or not stopping nightmares. All authors reviewed the patient categorizations and approved of them to ensure accuracy of the scoring. Three hundred fifty-three patients either were unable to be contacted for feedback or only reported technical issues- (without reporting any qualitative feedback) and were therefore omitted from the analysis. (See Figure 1, CONSORT Diagram) The remaining 630 patients were included in the study results. The percentage of each category of patients was calculated as part of the 630 patients who provided adequate feedback for inclusion in the analysis.
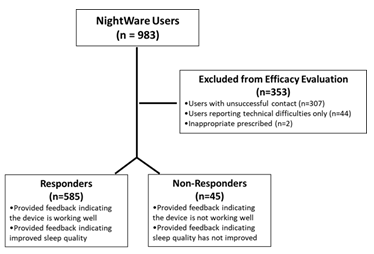
Figure 1: CONSORT Diagram of patient responses.
3. Results
Patients largely reported a positive response to this treatment. Overall, of the 630 patients who provided feedback, 468 (68.4%) reported excellent or good response to treatment, and 585 of the 630 (92.9%) patients reported at least some improvement in sleep and nightmares. (See Figure 2, Pie chart) The average age of these 630 patients was 37.7 (SD 8.2) years and 79% were male. The 585 patients that reported a positive response were divided into three groups based on the feedback provided. Their results are as follows: 139 (22.1%) reported an excellent response, 292 (46.3%) reported a good response, and 154 (24.4%) reported a modestly improved response to treatment with NightWare. (Table 1)
Table 1: Scoring Criteria and Scoring Results
|
Scoring Criteria |
Scoring Results |
|||
|
Category |
Criteria Description |
Qualitative Feedback Response |
n |
Portion of Population |
|
Excellent Response (Group 1) |
• ≥1 Reference of improved sleep and/or reduction/improvement with nightmares |
Positive treatment response excellent response |
139 |
22.1% |
|
• ≥2 Patient response that the device is working “perfectly", "really well", "very well", "great" or "still going well" |
||||
|
• ≥2 references of the device "working", "receiving benefit", or "doing what is supposed to" |
||||
|
• 1 reference of “perfectly", "really well", "very well", "great" or "still going well" AND 1 reference of the device "working", "receiving benefit", or "doing what is supposed to" |
||||
|
Good Response (Group 2) |
• ≥2 references of the device working "good" or well" |
Positive treatment response, good response |
292 |
46.3% |
|
• 1 reference of their sleep going "perfectly", "really well", "very well", "great" or "still going well" |
||||
|
• 1 reference of the device "working", "receiving benefit", or "doing what is supposed to" |
||||
|
• 1 reference of things going "good" or "well" and 1 reference of the device working "ok", "fine" |
||||
|
• 1 reference of things going "good" or "well" and data in the portal/wearing every night/wearing as much as possible |
||||
|
Modest Response (Group 3) |
• 1 reference of the device working "good" or well" |
Positive treatment response, modest improvement |
154 |
24.4% |
|
• ≥1 reference(s) of the device working "ok" |
||||
|
Poor Response (Group 4) |
The device wakes the patient and/or the vibrations are too disruptive |
Negative treatment response, vibrations bothersome |
22 |
3.5% |
|
Poor Response (Group 5) |
The device is not working to stop nightmares |
Negative treatment response, did not stop nightmares |
16 |
2.5% |
|
Poor Response (Group 6) |
Patient does not want to wear the watch/advised by a clinician to not use it |
Negative treatment response, does not want to use device or was advised not use it |
7 |
1.1% |
Forty-five of the 630 patients (7.1%) who provided feedback were treatment non-responders. (See Table and Figure 2) Only 22/630 (3.5%) reported that the vibrations were too bothersome for the device to be effective, 16/630 (2.5%) reported that the device did not stop their nightmares, and 7/630 (1.1%) did not want to use the device or were advised to stop using it by their provider.
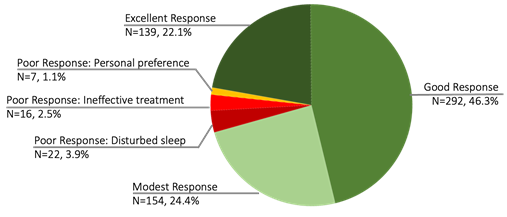
Figure 2: Detailed Patient Feedback Scoring Results. Of the 630 patients who provided feedback about the device and their treatment, 22.1% reported having an Excellent Response and more than 90% reported at least some benefit from the treatment. The most common cause of a poor response was haptic feedback that was disruptive to their sleep
In this group of 630 patients providing treatment response feedback, the majority, 476 (75.6%), did not have technical issues related to the device. (See Figure 3, bar graph technical problems). Complaints related to training and education (e.g., lack of understanding of how to use the device) were the most common, accounting for 40% of all issues. Another 38% of complaints involved hardware or software problems. Only 22% of the complaints involved problems with the interventions, such as tattoos impeding heart rate detection and intervention delivery, or the haptic feedback was uncomfortable or disruptive.
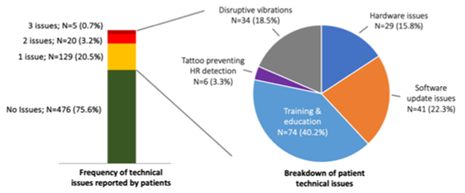
Figure 3: Summary of issues experienced by NightWare users. Of the 630 patients who provided feedback about their treatment, 75.6% did not report any issues with the device. Of the 154 patients who did report issues there were 184 unique issues reported, of which Training & Education (40.2%) and Software update issues (22.3%) were the most common.
Responders to treatment reported fewer issues than non-responders. The most common questions/concerns of the non-responder group were related to the frequency and intensity of the haptic feedback interventions being disruptive, reported by 21 of 45 (47%) of all treatment non-responders. In contrast, only 13 of the 585 (2%) treatment responders reported concerns about the disruptiveness of the haptic feedback interventions. Overall, only 34 of 630 (5%) of the patients could not tolerate the haptic feedback interventions.
4. Discussion
This study captures real-world effectiveness data of a novel intervention in over 600 patients with nightmare disorders who self-reported the impact of the device on their nightmares and sleep quality. Patient selection is essential to successful treatment with this therapy, as with other therapies. Specifically, because this treatment relies on heart rate changes to detect when nightmares are most likely to be occurring, we believe that the presence of pronounced sympathetic nervous system activation symptoms (i.e., palpitations, sweating, awakening with panic attack-like symptoms) is an important symptom set to consider for patient selection. The percentage of patients that reported improved sleep and decreased nightmares is very high (92.9%), which we believe reflects good patient selection by the clinicians. Most of the patients that reported poor response to treatment fell into two categories—the vibrations from the device were too bothersome or the vibrations did not stop their nightmares. Further improvements to adjust the intensity of the vibrations or to lower the threshold for intervention may result in increased effectiveness of this device. For the 24% of patients that reported a problem, very few were related to the haptic feedback interventions, and 95% of the problems were resolvable issues (i.e., setting the time on the device, resolving software conflicts). In addition to randomized trials, it is important to consider evidence from other types of research. One strength of this study is that the results are generalizable to other patients with nightmare disorder or PTSD-associated nightmares. [18] This study also avoids the “healthy-volunteer” effect that can be a source of bias in randomized clinical trials, and it shares some features of pragmatic trials. [19] The device manufacturer gave all clinicians who prescribed the device in this study some instructions on patient selection. This patient selection instruction is easy to disseminate widely in various forms, and implementation of this treatment modality can and should be accompanied by this information.
There are some limitations to this study. By their nature, retrospective analyses of this type may not be able to access data on a representative control group. Further, the patients in this study may have been receiving other treatments for mental health conditions. However, the close temporal relationship between the start of treatment with NightWare and the improvement suggests that the device is responsible for improving nightmares, rather than attributing such improvement to other interventions. Race and ethnicity data were not collected from the patients in this analysis, so the effect of race and ethnicity on treatment outcomes could not be evaluated.
Treatments for nightmares can be limited by patient and health system factors. This wearable non-invasive device can help address these gaps in available therapy. Prazosin, for example, while effective for some patients, is limited by side effects in others. Treatments such as Imagery Rehearsal Therapy and Eye Movement Desensitization and Rescripting Therapy are limited by the availability of qualified therapists and the willingness of patients to engage fully in these therapies. In some populations, such as pilots and firefighters, the use of medications to treat nightmares is limited by work requirements. In contrast, NightWare is a low-risk alternative that is simple to use, provides relief from nightmares quickly, and can be quickly scaled for widespread use with little demand for clinician time. Treatment with NightWare to address nightmares allows the clinicians to use appointment time to provide the needed PTSD-specific therapy that patients require. By treating nightmares, this device can improve sleep quality and quantity,[17] which are both critical to good mental and physical health. Resolving insufficient sleep can help make patients better able to participate in other types of therapy for comorbid psychiatric disorders because the patients are better able to think clearly and have better emotional regulation. [20] This wearable treatment satisfies the gaps that exist with current therapies: it is readily accessible, is not impacted by provider shortages or limits of expertise, and does not have the significant side effects that exist with pharmacotherapy. For patients who feel that there is a stigma towards seeking care with a behavioral healthcare provider, a wearable treatment device may provide the privacy that they seek. Future research on this device could include evaluating how it performs when used in conjunction with medications like prazosin, evaluating how it performs in the setting of both treated and untreated obstructive sleep apnea, and evaluating the impact of decreasing nightmares and improving sleep quality on the success of psychotherapy for other symptoms of PTSD.
5. Conclusion
In conclusion, this large retrospective study evaluated the real-world effectiveness of the NightWare device in DoD patients. This experience has shown that the device works well in decreasing or eliminating nightmares and improving sleep quality in appropriately selected patients. Although additional well-controlled clinical trials are needed to further evaluate this device, similar results can be expected in the future.
Acknowledgements
Acknowledgements: The authors would like to thank Blair Landry and Markie Edler for their assistance with data collection and input on this work.
Disclosure
All authors have seen and approved the manuscript. The research reported here was provided by NightWare, Inc. and Sleep Management LLC. This company participated in the analysis and reporting of results. Any opinions, findings, conclusions, or recommendations expressed in this publication are those of the author(s) and do not necessarily reflect the views of the Uniformed Services University, US Government, or the Department of Defense, and no official endorsement should be inferred. Authors BD Robertson, TR Pearce, KR Rayl, EF Wargo, and DR Karlin are employees of NightWare, Inc.
References:
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fifth Edition. American Psychiatric Association; 2013.
- Tanskanen A, Tuomilehto J, Viinamäki H, et al. Nightmares as predictors of suicide. Sleep. 24 (2001): 844-847.
- Bjorvatn B, Grønli J, Pallesen S. Prevalence of different parasomnias in the general population. Sleep Med. 11 (2010): 1031-1034.
- Janson C, Gislason T, De Backer W, et al. Prevalence of sleep disturbances among young adults in three European countries. Sleep. 18 (1995): 589-597.
- Schredl M. Dream recall frequency and sleep quality of patients with restless legs syndrome. Eur J Neurol. 8 (2001):185-189.
- Creamer JL, Brock MS, Matsangas P, Motamedi V, Mysliwiec V. Nightmares in United States Military Personnel With Sleep Disturbances. J Clin Sleep Med JCSM Off Publ Am Acad Sleep Med. 14 (2018): 419-426.
- Neylan TC, Marmar CR, Metzler TJ, et al. Sleep Disturbances in the Vietnam Generation: Findings From a Nationally Representative Sample of Male Vietnam Veterans. Am J Psychiatry. 155 (1998): 929-933.
- Leskin GA, Woodward SH, Young HE, et al. Effects of comorbid diagnoses on sleep disturbance in PTSD. J Psychiatr Res. 36 (2002): 449-452.
- Pruiksma KE, Taylor DJ, Wachen JS, et al. Residual sleep disturbances following PTSD treatment in active duty military personnel. Psychol Trauma Theory Res Pract Policy. 8 (2016): 697-701.
- Thoits PA. Clinical Need, Perceived Need, and Treatment Use: Estimating Unmet Need for Mental Health Services in the Adult Population. J Health Soc Behav. 63 (2022): 491-507.
- Office of the Inspector General. Evaluation of Access to Mental Health Care in the Department of Defense. Department of Defense; 2020:74.
- Morgenthaler TI, Auerbach S, Casey KR, et al. Position Paper for the Treatment of Nightmare Disorder in Adults: An American Academy of Sleep Medicine Position Paper. J Clin Sleep Med JCSM Off Publ Am Acad Sleep Med. 14 (2018):1041-1055.
- Cook JM, Harb GC, Gehrman PR, et al. Imagery rehearsal for posttraumatic nightmares: A randomized controlled trial. J Trauma Stress. 2010;23 (2010): 553-563.
- Management of Posttraumatic Stress Disorder and Acute Stress Disorder Work Group. VA/DoD CLINICAL PRACTICE GUIDELINE FOR MANAGEMENT OF POSTTRAUMATIC STRESS DISORDER AND ACUTE STRESS DISORDER. Government Printing Office; 2023.
- Raskind MA, Peskind ER, Chow B, et al. Trial of Prazosin for Post-Traumatic Stress Disorder in Military Veterans. N Engl J Med. 378 (2018): 507-517.
- Pfizer Labs. Minipress capsules: prescribing information. Published online 2009.
- Davenport ND, Werner JK. A randomized sham-controlled clinical trial of a novel wearable intervention for trauma-related nightmares in military veterans. J Clin Sleep Med. Published online 2022.
- Kostis JB, Dobrzynski JM. Limitations of Randomized Clinical Trials. Am J Cardiol. 2020;129 (2020):109-115.
- Ford I, Norrie J. Pragmatic Trials. N Engl J Med. 2016;375 (2016): 454-463.
- Barber L, Grawitch MJ, Munz DC. Are better sleepers more engaged workers? A self-regulatory approach to sleep hygiene and work engagement. Stress Health J Int Soc Investig Stress. 29 (2013): 307-316.
