Rare Localisation of Glomus Tumor under greater Toenail Bed, presenting with Pain for a Decade-A Case Report
Article Information
Kursad Aytekin1*, Cem Zeki Esenyel1, Zafer Unsal Coskun2
1University of Giresun, School of Medicine, Department of Orthopaedics and Traumatology, Giresun, Turkey
2University of Health Sciences, Istanbul Sultan Abdulhamid Training hospital, Istanbul, Turkey
*Corresponding Author: Kursad Aytekin MD PhD, University of Giresun, School of Medicine, Departments of Orthopaedics and Traumatology & Anatomy, Giresun, Turkey
Received: 18 June 2019; Accepted: 01 July 2019; Published: 05 July 2019
Citation: Kursad Aytekin, Cem Zeki Esenyel, Zafer Unsal Coskun. Rare Localisation of Glomus Tumor under greater Toenail Bed, presenting with Pain for a Decade-A Case Report. Journal of Orthopaedics and Sports Medicine 1 (2019): 060-065.
View / Download Pdf Share at FacebookAbstract
Glomus tumors are usually presented with late diagnosis and treatment. This slow process may be caused due to the pain that only occur with provocative contact. In this case report, follow up of a patient is presented who has prolonged symptoms at a rare localisation of glomus tumor. After the glomus tumor of greater toe excised totally, the complaints of the patient were cut dramatically.
Keywords
<p>Glomus tumor, Greater toe, Doppler ultrasound</p>
Toenail bed articles Toenail bed Research articles Toenail bed review articles Toenail bed PubMed articles Toenail bed PubMed Central articles Toenail bed 2023 articles Toenail bed 2024 articles Toenail bed Scopus articles Toenail bed impact factor journals Toenail bed Scopus journals Toenail bed PubMed journals Toenail bed medical journals Toenail bed free journals Toenail bed best journals Toenail bed top journals Toenail bed free medical journals Toenail bed famous journals Toenail bed Google Scholar indexed journals Glomus articles Glomus Research articles Glomus review articles Glomus PubMed articles Glomus PubMed Central articles Glomus 2023 articles Glomus 2024 articles Glomus Scopus articles Glomus impact factor journals Glomus Scopus journals Glomus PubMed journals Glomus medical journals Glomus free journals Glomus best journals Glomus top journals Glomus free medical journals Glomus famous journals Glomus Google Scholar indexed journals Neoplastic articles Neoplastic Research articles Neoplastic review articles Neoplastic PubMed articles Neoplastic PubMed Central articles Neoplastic 2023 articles Neoplastic 2024 articles Neoplastic Scopus articles Neoplastic impact factor journals Neoplastic Scopus journals Neoplastic PubMed journals Neoplastic medical journals Neoplastic free journals Neoplastic best journals Neoplastic top journals Neoplastic free medical journals Neoplastic famous journals Neoplastic Google Scholar indexed journals Connective tissue articles Connective tissue Research articles Connective tissue review articles Connective tissue PubMed articles Connective tissue PubMed Central articles Connective tissue 2023 articles Connective tissue 2024 articles Connective tissue Scopus articles Connective tissue impact factor journals Connective tissue Scopus journals Connective tissue PubMed journals Connective tissue medical journals Connective tissue free journals Connective tissue best journals Connective tissue top journals Connective tissue free medical journals Connective tissue famous journals Connective tissue Google Scholar indexed journals Neuromyoarterial articles Neuromyoarterial Research articles Neuromyoarterial review articles Neuromyoarterial PubMed articles Neuromyoarterial PubMed Central articles Neuromyoarterial 2023 articles Neuromyoarterial 2024 articles Neuromyoarterial Scopus articles Neuromyoarterial impact factor journals Neuromyoarterial Scopus journals Neuromyoarterial PubMed journals Neuromyoarterial medical journals Neuromyoarterial free journals Neuromyoarterial best journals Neuromyoarterial top journals Neuromyoarterial free medical journals Neuromyoarterial famous journals Neuromyoarterial Google Scholar indexed journals Soft tissue tumor articles Soft tissue tumor Research articles Soft tissue tumor review articles Soft tissue tumor PubMed articles Soft tissue tumor PubMed Central articles Soft tissue tumor 2023 articles Soft tissue tumor 2024 articles Soft tissue tumor Scopus articles Soft tissue tumor impact factor journals Soft tissue tumor Scopus journals Soft tissue tumor PubMed journals Soft tissue tumor medical journals Soft tissue tumor free journals Soft tissue tumor best journals Soft tissue tumor top journals Soft tissue tumor free medical journals Soft tissue tumor famous journals Soft tissue tumor Google Scholar indexed journals Fingernails articles Fingernails Research articles Fingernails review articles Fingernails PubMed articles Fingernails PubMed Central articles Fingernails 2023 articles Fingernails 2024 articles Fingernails Scopus articles Fingernails impact factor journals Fingernails Scopus journals Fingernails PubMed journals Fingernails medical journals Fingernails free journals Fingernails best journals Fingernails top journals Fingernails free medical journals Fingernails famous journals Fingernails Google Scholar indexed journals Physical examination articles Physical examination Research articles Physical examination review articles Physical examination PubMed articles Physical examination PubMed Central articles Physical examination 2023 articles Physical examination 2024 articles Physical examination Scopus articles Physical examination impact factor journals Physical examination Scopus journals Physical examination PubMed journals Physical examination medical journals Physical examination free journals Physical examination best journals Physical examination top journals Physical examination free medical journals Physical examination famous journals Physical examination Google Scholar indexed journals Hypoechoic lesion articles Hypoechoic lesion Research articles Hypoechoic lesion review articles Hypoechoic lesion PubMed articles Hypoechoic lesion PubMed Central articles Hypoechoic lesion 2023 articles Hypoechoic lesion 2024 articles Hypoechoic lesion Scopus articles Hypoechoic lesion impact factor journals Hypoechoic lesion Scopus journals Hypoechoic lesion PubMed journals Hypoechoic lesion medical journals Hypoechoic lesion free journals Hypoechoic lesion best journals Hypoechoic lesion top journals Hypoechoic lesion free medical journals Hypoechoic lesion famous journals Hypoechoic lesion Google Scholar indexed journals Antiinflammatory articles Antiinflammatory Research articles Antiinflammatory review articles Antiinflammatory PubMed articles Antiinflammatory PubMed Central articles Antiinflammatory 2023 articles Antiinflammatory 2024 articles Antiinflammatory Scopus articles Antiinflammatory impact factor journals Antiinflammatory Scopus journals Antiinflammatory PubMed journals Antiinflammatory medical journals Antiinflammatory free journals Antiinflammatory best journals Antiinflammatory top journals Antiinflammatory free medical journals Antiinflammatory famous journals Antiinflammatory Google Scholar indexed journals Hemangioma articles Hemangioma Research articles Hemangioma review articles Hemangioma PubMed articles Hemangioma PubMed Central articles Hemangioma 2023 articles Hemangioma 2024 articles Hemangioma Scopus articles Hemangioma impact factor journals Hemangioma Scopus journals Hemangioma PubMed journals Hemangioma medical journals Hemangioma free journals Hemangioma best journals Hemangioma top journals Hemangioma free medical journals Hemangioma famous journals Hemangioma Google Scholar indexed journals Ultrasonographic articles Ultrasonographic Research articles Ultrasonographic review articles Ultrasonographic PubMed articles Ultrasonographic PubMed Central articles Ultrasonographic 2023 articles Ultrasonographic 2024 articles Ultrasonographic Scopus articles Ultrasonographic impact factor journals Ultrasonographic Scopus journals Ultrasonographic PubMed journals Ultrasonographic medical journals Ultrasonographic free journals Ultrasonographic best journals Ultrasonographic top journals Ultrasonographic free medical journals Ultrasonographic famous journals Ultrasonographic Google Scholar indexed journals
Article Details
1. Introduction
Glomus bodies are arteriovenous anastomoses responsible for thermoregulation by regulating skin blood flow [1]. These bodies are found in the retinacular layer of the dermis throughout the body, also in the palms and feet [2]. They have an arteriovenous complex with neurovascular retinaculum, afferent arteriole, and efferent arteriole. They are specialized structures for arteriolar current and temperature control. Neoplastic growth of the glomus bodies creates the glomus tumor. Glomus tumors consist of vascular channels and glomus cell piles separated histopathologically by a connective tissue stroma [3]. Glomus tumors are benign tumors composed of cells that resemble the modified perivascular smooth muscle cells of the normal glomus body and they are neuromyoarterial malformations [4-7]. Glomus tumors are usually subuncal localized and patients experience pain for a long time until they are diagnosed and treated. In the diagnosis, a defect in the bone may be seen on the X-ray. Since it is a soft tissue tumor, US, Doppler US and MRI are useful in the diagnosis. Differential diagnosis of glomus tumor includes vascular pathologies [8]. The definitive diagnosis is made histopathologically after excision of the tumor. Surgical excision is very successful for treatment. In this case report, we present a two-year follow-up of a female patient with right greater toe subuncal glomus tumor treated with transuncal excision.
2. Case Report
Forty one year-old female patient was admitted to the orthopedics and the traumatology outpatient clinic with complaints of pain in her right greater toe. Her complaints were caused by exposure to cold or any contact with her fingernails. The patient’s complaints started 10 years ago. The patient did not benefit from shoe modification and NSAID treatment. Physical examination revealed purple discoloration on the fibular side of the greater toenail (Figure 1). Love and cold sensitivity tests were positive.
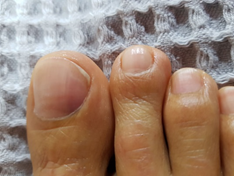
Figure 1: Purplish color change under the fibular side of toe nail.
For diagnosis, Doppler USG (Figure 2A, 2B) (Hitachi, Japan) examination were performed with 10 Mhz linear transducer. Contrast MRI (Figure 3) (MAGNETOM Aera(®); Siemens Healthcare, Erlangen, Germany) was performed in addition to conventional sequences using superficial coil. 3.0 × 2.0 mm tumor was observed radiologically.
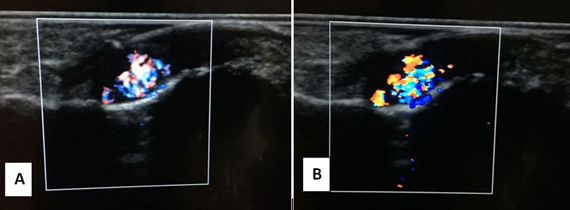
Figure 2: A) There is a well defined hypoechoic lesion (3.0 × 2.0 mm) under nailbed; B) showing hypervascularity on color Doppler USG.
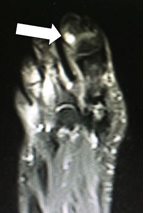
Figure 3: Contrast-enhanced coronal MRI, T1 weighted sequence. Small nodule on the dorsal aspect of distal phalanx of the greater toe with homogenous contrast uptake. White arrow shows the glomus tumor.
The patient was thought to have a subuncal glomus tumor of the right greater toenail and surgical excision decision was made. Tumor excision was performed with transuncal technique [8] under local anesthesia (Figure 4). Pathological diagnosis was consistent with glomus tumor. She was dressed every other day until the suture was removed 3 weeks later. During the 2-year follow-up, she did not have any complaints.
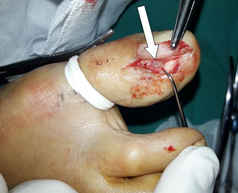
Figure 4: Intraoperative clinical appearance of subuncal localized glomus tumor. White arrow shows the glomus tumor.
3. Discussion
Glomus bodies are located in the stratum reticularis of the dermis and mostly located in the fingers. Patients often complain of long-standing pain. Glomus tumors in the extremities are frequently observed in women in the 4th to 5th decades of life. Glomus tumor can appear in any part of the body, although it mostly appears in the extremities, accounting for just 1.5-2% of all the neoplasms in the extremities at the subungual level [7, 9, 10]. Greater toe is one of the rare localisation of glomus tumor [11]. Pain, discoloration and cold hypersensitivity are reported as classic triads in the literature [7]. Since developing from glomus bodies, which are dense at the fingertips and contribute to thermoregulation, glomus tumors are hypersensitive to cold. Physical examination may reveal a purplish discoloration and deformity under the nail [9]. In the Love test, which is used for diagnosis in the examination, the complaints are aggravated when a point-like compression is applied to the suspicious area with a pen tip or needle [8]. Another diagnostic test is the cold sensitivity test [8]. Pain increases with cold and decreases when warm. Antiinflammatory treatment is ineffective [12]. When suspected with anamnesis and examination, MRI and USG can be used to confirm the diagnosis. Defect can be observed in the area where the tumor is located on the bone [13]. Imaging methods allow the detection of such lesions and give precise location for surgical removal [14]. Surgical excision allows histopathological diagnosis and quick recovery of symptoms [15]. If bony erosions are present and indicate bony involvement, dissection of the tumor down to the surface of the bone will decrease the chance of recurrence [16].
Differential diagnosis includes inflammatory/infectious diseases (psoriasis, abscess), benign lesions (cysts, arteriovenous malformations, subungual exostosis) and malignancies (squamous cell carcinoma, malignant melanoma) [15]. Hemangiomas, which can be considered in the differential diagnosis of glomus tumor, occur at an early age (present at birth or in the first 2 weeks). In hemangiomas, diffuse or exfoliated erythema with local swelling is accompanied by subcutaneous tumor. hemangioma usually shows rapid development in 1 year. Sonographically, it is difficult to define glomus tumor and true hemangioma. There is pain associated with pressure in the glomus tumor. Hemangioma is more common in infants and young children. In vascular malformations, the ultrasound image is more irregular, painless with pressure, and there is no specific surface distribution. Ultrasonographic findings of glomus tumor are regular and pain is the most important finding. Melanoma has a high rate of malignancy and metastasis is rapid. Glomus tumors progress slowly and patients have long-standing complaints [17].
There are high rates of misdiagnosis in the diagnosis of glomus tumor [18]. The correct diagnosis rate by USG is 88% [12]. With improved resolution, high-frequency ultrasound can clearly show the characteristics of the tumor only in real time and accurately determine the localization before surgery [12]. Considering that the treatment of glomus tumors consists of complete surgical resection of the lesion [2, 19] imaging methods, especially US and MRI, play an important role in the diagnostic confirmation of this entity. Given the fact that glomus tumor is a neuromyoaterial malformation, the benefit of Doppler US in the diagnosis can be particularly helpful in the differential diagnosis. In addition, these methods allow accurate detection of the tumor, facilitating surgical planning, and exclusion of other differential diagnoses. However, it is important to emphasize the non-specific nature of the imaging findings of these lesions, and therefore the diagnosis should be based on correlation with clinical findings [20].
Our patient was a 41-year-old woman, consistent with the literature [10]. We performed surgery with the most commonly used transuncal method in the literature [21]. Possible complications in glomus tumor surgeries include recurrence, nail dystrophy, nail surface irregularity, wound opening, suture border necrosis or infection [8, 22]. Any complication was not observed during the 2 year follow-up. Since glomus tumor was a neuromyoarterial tumor, we used USG and MRI together with doppler USG to rule out vascular differential diagnoses. Subungal glomus tumor of the toe, which is a rare condition, should be kept in mind in patients presenting with pain in the toe. Complete resection of the tumor is a useful method to completely improve the patient’s complaints.
References
- Montandon C, Costa JC, Dias LA, et al. Subunkal glomus tumors: imaging findings. Radiol Bras 42 (2009): 371-374.
- Theumann NH, Goettmann S, Le Viet D, et al. Recurrent glomus tumors of fingertips: MR imaging evaluation. Radiology 223 (2002): 143-151.
- Tsuneyoshi M, Enjogi M. Glomus Tumor. A clinicopathologic and electromicroscobic study. Journal of cancer 50 (1982): 1601-1607.
- Shin DK, Kim MS, Kim SW, et al. A painful glomus tumor on the pulp of the distal phalanx. J Korean Neurosurg Soc 48 (2010): 185-187.
- Sapuan J, Paul AG, Abdullah S. Glomus tumor in the second toe: a clinical insight. J Foot Ankle Surg 47 (2008): 483-486.
- Polo C, Borda D, Poggio D, et al. Glomus tumor of the hallux: review of the literature and report of two cases. Foot Ankle Surg 18 (2012): 89-93.
- Lui TH, Mak SM. Glomus Tumor of the Great Toe. J Foot Ankle Surg 53 (2014): 360-363.
- Samaniego E, Crespo A, Sanz A. Key diagnostic features and treatment of subungual glomus tumor. Actas Dermo-Sifiliográficas (English Edition) 100 (2009): 875-882.
- Song M, Ko HC, Kwon KS, et al. Surgical treatment of subungual glomus tumor: a unique and simple method. Dermatol Surg 35 (2009): 786-791.
- Tsuchie H, Okada K, Nagasawa H, et al. Glomus tumor of the toe with symptoms similar to those of Morton’s disease. J Orthop Sci 14 (2009): 826-829.
- Mohindra M, Sambandam B, Gautam VK, et al. A Rare Case of Glomus Tumor of the Great Toe: An Analysis of Behavior at This Rare Site. Foot and ankle specialist 9 (2016): 83-87.
- Fan Z, Wu G, Ji B, et al. Color Doppler ultrasound morphology of glomus tumors of the extremities. Springerplus 5 (2016): 1319.
- Chou T, Pan SC, Shieh SJ, et al. Glomus Tumor Twenty-Year Experience and Literature Review. Ann Plast Surg 76 (2016): 35-40.
- Baek HJ, Lee SJ, Cho KH, et al. Subungual tumors: clinicopathologic correlation with US and MR imaging findings. Radiographics 30 (2010): 1621-1636.
- Vieira FG, Nakamura R, Costa FM, et al. Subungual Glomus Tumor. J Clin Rheumatol 22 (2016): 331.
- Lin YC, Hsiao PF,Wu YH, et al. Recurrent digital glomus tumor: analysis of 75 cases. Dermatol Surg 36 (2010): 1396-1400.
- Carlson ML, Sweeney AD, Wanna GB, et al. Natural history of glomus jugulare: a review of 16 tumors managed with primary observation. Otolaryngol Head Neck Surg 152 (2015): 98-105.
- Sun BG, Yun-tao W, Jia-zhen L. Glomus tumours of the hand and foot. Int Orthop 20 (1996): 339-341.
- Drapé JL, Idy-Peretti I, Goettmann S, et al. Subungual glomus tumors: evaluation with MR imaging. Radiology 195 (1995): 507-515.
- Fornage BD. Glomus tumors in the fingers: diagnosis with US. Radiology 167 (1988): 183-185.
- Kale S, Rao V, Bentz M. Glomus tumor of the index finger. J Craniofac Surg 17 (2006): 801-804.
- Garg B, Machhindra MV, Tiwari V, et al. Nail-preserving modified lateral subperiosteal approach for subungual glomus tumour: a novel surgical approach. Musculoskelet Surg 100 (2016): 43-48.
