Postoperative Residual Curarization in Difficult Environment for the Practice of General Anesthesia: Inventory of the Yaounde/Essos Hospital Center
Article Information
Jemea B1,4, Nga Nomo S2,5*, Iroume C1,4, Djomo Tamchom D3,6, Chewa G5, Mouafo B5, Nkoumou S5, Ze Minkande J1, Binam F1
1Departement of surgery and specialities, Faculty of medicine and biomedical sciences, University of Yaounde 1, Cameroon
2Departement of surgery and specialities, Higher institute of medical technology, University of Douala
3Departement of surgery and specialities, Faculty of health science, University of Buea
4Anesthesia and intensive care departement, Yaounde Teaching Hospital, Cameroon
5Anesthesia and intensive care departement, Yaounde-Essos hospital center, Cameroon
6Anesthesia and intensive care departement, Gyneco-obstetrics and pediatric hospital of Douala, Cameroon
*Corresponding Author: Nga Nomo Serge Vivier, Departement of surgery and specialities, Higher institute of medical technology (ISTM), University of Douala, Cameroon.
Received: 18 January 2022; Accepted: 25 January 2022; Published: 31 March 2022
Citation: Jemea B, Nga Nomo S, Iroume C, Djomo Tamchom D, Chewa G, Mouafo B, Nkoumou S, Ze Minkande J, Binam F. Postoperative Residual Curarization in Difficult Environment for the Practice of General Anesthesia: Inventory of the Yaounde/Essos Hospital Center. Anesthesia and Critical Care 4 (2022): 64-72.
View / Download Pdf Share at FacebookAbstract
Background
Residual curarization is dangerous, it promotes postoperative pneumonia. The objective of this study was to assess the relevance of clinical extubation criteria in the prevention of residual curarization.
Patients and methods
This was a prospective and descriptive study carried out over a period of 3 months in the anesthesia department of the Yaounde-Essos hospital center. It included all adult patients operated on under general anesthesia for elective surgery, and who received vecuronium bromide administration during the anesthetic procedure.
Results
A total of 80 patients were collected from 150 acts of anesthesia performed during the study period. The average age was 44 years old, the sex ratio of 1.10 in favor of men. The patient's extubation was based in the majority of cases (82.6%) on the combination of the following clinical criteria: the presence of spontaneous ventilation and swallowing reflex, the positive head lift test and the level of correct consciousness. The incidence of postoperative residual curarization was 50%. The main complications were hypoventilation associated with hypoxia (40%), diplopia (35%) and apnea (25%).
Conclusion
The incidence of residual curarization remains high at the essos hospital centre. Reliable detection of curarization can only be done with a measuring instrument.
Keywords
<p>Residual curarization, General anesthesia</p>
Residual curarization articles; General anesthesia articles
Residual curarization articles Residual curarization Research articles Residual curarization review articles Residual curarization PubMed articles Residual curarization PubMed Central articles Residual curarization 2023 articles Residual curarization 2024 articles Residual curarization Scopus articles Residual curarization impact factor journals Residual curarization Scopus journals Residual curarization PubMed journals Residual curarization medical journals Residual curarization free journals Residual curarization best journals Residual curarization top journals Residual curarization free medical journals Residual curarization famous journals Residual curarization Google Scholar indexed journals General anesthesia articles General anesthesia Research articles General anesthesia review articles General anesthesia PubMed articles General anesthesia PubMed Central articles General anesthesia 2023 articles General anesthesia 2024 articles General anesthesia Scopus articles General anesthesia impact factor journals General anesthesia Scopus journals General anesthesia PubMed journals General anesthesia medical journals General anesthesia free journals General anesthesia best journals General anesthesia top journals General anesthesia free medical journals General anesthesia famous journals General anesthesia Google Scholar indexed journals hypoventilation articles hypoventilation Research articles hypoventilation review articles hypoventilation PubMed articles hypoventilation PubMed Central articles hypoventilation 2023 articles hypoventilation 2024 articles hypoventilation Scopus articles hypoventilation impact factor journals hypoventilation Scopus journals hypoventilation PubMed journals hypoventilation medical journals hypoventilation free journals hypoventilation best journals hypoventilation top journals hypoventilation free medical journals hypoventilation famous journals hypoventilation Google Scholar indexed journals postoperative residual curarization articles postoperative residual curarization Research articles postoperative residual curarization review articles postoperative residual curarization PubMed articles postoperative residual curarization PubMed Central articles postoperative residual curarization 2023 articles postoperative residual curarization 2024 articles postoperative residual curarization Scopus articles postoperative residual curarization impact factor journals postoperative residual curarization Scopus journals postoperative residual curarization PubMed journals postoperative residual curarization medical journals postoperative residual curarization free journals postoperative residual curarization best journals postoperative residual curarization top journals postoperative residual curarization free medical journals postoperative residual curarization famous journals postoperative residual curarization Google Scholar indexed journals surgery articles surgery Research articles surgery review articles surgery PubMed articles surgery PubMed Central articles surgery 2023 articles surgery 2024 articles surgery Scopus articles surgery impact factor journals surgery Scopus journals surgery PubMed journals surgery medical journals surgery free journals surgery best journals surgery top journals surgery free medical journals surgery famous journals surgery Google Scholar indexed journals T4/T1 ratio articles T4/T1 ratio Research articles T4/T1 ratio review articles T4/T1 ratio PubMed articles T4/T1 ratio PubMed Central articles T4/T1 ratio 2023 articles T4/T1 ratio 2024 articles T4/T1 ratio Scopus articles T4/T1 ratio impact factor journals T4/T1 ratio Scopus journals T4/T1 ratio PubMed journals T4/T1 ratio medical journals T4/T1 ratio free journals T4/T1 ratio best journals T4/T1 ratio top journals T4/T1 ratio free medical journals T4/T1 ratio famous journals T4/T1 ratio Google Scholar indexed journals
Article Details
1. Introduction
Curarization is caused by the administration of curarizing substances which cause muscle paralysis. Residual postoperative curarization is the persistence of curative clinical effects or the absence of complete restoration of muscle strength after administration of curare [1,2,3]. It is defined by a T4/T1 ratio of less than 90% at the train of four on the abductor of the thumb in the postoperative period [1,3]. It is potentially responsible for postoperative respiratory complications [3]. Monitoring of curarization is an essential part of the practice of general anesthesia [1,3]. It makes it possible to use non-depolarizing curares with precision, to obtain good intubation conditions, muscle relaxation adapted to the type of surgery, as well as a rigorous assessment of the decurarization process. In sub-Saharan Africa, the lack of adequate infrastructure for the correct practice of general anesthesia makes extubation of the patient difficult at the end of the surgical procedure. The decision to extubate the patient at the end of the surgery is usually based on finding the clinical criteria for decurarization. This work was initiated with the aim of evaluating the relevance of clinical extubation criteria in the prevention of postoperative residual curarization in regulated surgery in adults, in an environment unfavorable to the practice of general anesthesia.
2. Patients and Methods
This was a prospective descriptive study over a 3-month period, from November 28, 2019 to February 28, 2020. It took place in the anesthesia department of the Yaounde-Essos hospital center. After ethics committee approval, patients over 18 years of age seen in an anesthesia consultation for scheduled surgery under general anesthesia were included in the study. Myasthenic patients and pregnant women were excluded, as were those who refused to participate in the study. A detailed explanation of the protocol was provided to patients in order to obtain free and informed consent. All participants were seen in a pre-anesthetic consultation to assess the anesthetic and operative risk. To avoid misinterpretation, the premedication was non-drug only. The method of calculating the preoperative fasting compensation was that of Holliday and Segar (4-2-1 rule). The surgery was said to be "short" when it was less than 90 minutes, "medium" if it was between 90 and 180 minutes, and "long" if it was longer than 180 minutes. All patients received the same anesthetic induction protocol: fentanyl 5μg/kg IV, propofol 3mg/kg IV, vecuronium bromide 0.10mg/kg IV. The patient's extubation on the operating table was decided on the basis of clinical decurarization criteria:
- The positive “head lift test” or the possibility of keeping the head elevated above the plane of the bed for 5 seconds,
- The resumption of spontaneous ventilation with a respiratory rate between 10 and 30 cycles per minute,
- The presence of the swallowing reflex,
- The absence of diplopia
- And the positive “tongue depressor test” which designates a clinical test which assesses the muscle strength of the masseters by asking the patient to squeeze a tongue depressor between the incisors.
Curarization monitoring was performed systematically after extubation using a train of four scan (TOFscan®), by an independent anesthesiologist who was not involved in the patient's anesthetic management. It is a curare monitor using the technique of three-dimensional accelerometry and, allowing objective and precise measurement of the functioning of the neuromuscular junction. The dependent variable studied was postoperative residual curarization. The independent variables were those related to anthropometric and clinical data (age, sex, ASA class, history) and those related to postoperative residual curarization (non-depolarizing curare, method of stimulation, site of stimulation, antagonization to prostigmine, duration of surgery, reinjections of vecuronium, value of the T4/T1 ratio, complications of postoperative residual curarization, clinical criteria for decurarization). The data collected was compiled and analyzed using statistical analysis software CSPro 7.1. and SPSS. The tables and figures were developed using Microsoft Excel 2016 software. The link between the clinical criteria for decurarization and postoperative residual curarization was noted. The Chi-square test was used for the comparison of proportions. The probability p less than 0.05 was retained as significant.
3. Results
During the study period, 80 patients met the inclusion criteria for a total of 150 acts of anesthesia performed during the same period, or 53.3%. The characteristics of the study population are shown in table 1. The average age of the patients was 44 years with extremes ranging from 18 to 75 years. The sex ratio was 1.10 in favor of men. According the physical status classification system of American Society of Anesthesiologist (ASA), the patients mainly belonged to the ASA I (53%) and ASA II (46%) classes. Almost half of the workforce (47%) received reinjection of curare during the anesthetic procedure. Antagonization of vecuronium by neostigmine at the end of the surgical procedure was performed in 28 patients (17.5%), of whom 18 (11.25%) had persistent neuromuscular block (T4/T1 <90%). The criteria which authorized antagonization by neostigmine in our sample were: either the resumption of spontaneous ventilation in 57.2% (with the absence of other clinical signs of decurarization), or the total absence of clinical criteria for decurarization (42.8%). The decision to extubate the patient at the end of the surgery was based on the combination of the following criteria: the presence of spontaneous ventilation with a respiratory rate greater than 10 cycles per minute (cpm), the presence of the reflex of swallowing, the positive head lift test and the correct level of consciousness (82.6%). The association "presence of the swallowing reflex and spontaneous ventilation with FR >10 cpm" guided the decision to remove the tracheal tube in 15% of cases. Half of the study population had a T4/T1 ratio <90% by the first minute after tracheal extubation (Figure 1). The surgery was of average duration in more than half of the cases (59%), of short duration in 21% of cases and of long duration in 20% of cases. The frequency of complications from postoperative residual curarization was 40%. The main complications were bradypnea (40%), transient apnea (35%), diplopia (25%). The management of these complications was straightforward in all cases: supplementation with oxygen with a face mask, and ventilation with a self-inflating balloon with a one-way valve for the patients who presented with apnea. There was a significant correlation between age group and depth of postoperative residual curarization (Table 2). The level of postoperative residual curarization was deeper in the subject over 65 years of age. There was also a significant link between the duration of surgery and postoperative residual curarization (Table 3). Residual curarization was found mainly in the group of patients who had undergone short-term surgery in 88.2% of cases. Furthermore, there was no causal link between the residual curarization, the history and the ASA class of the patient.
|
Number (n) |
Percentage (%) |
|
|
Gender |
||
|
Male |
42 |
52,5 |
|
Female |
38 |
47,5 |
|
Total |
80 |
100 |
|
Age group (year) |
||
|
18-25 |
9 |
11,3 |
|
26-35 |
16 |
20 |
|
36-45 |
20 |
25 |
|
46-55 |
13 |
16,3 |
|
56-65 |
15 |
18,8 |
|
66-75 |
7 |
8,8 |
|
Total |
80 |
100 |
Table 1: Characteristics of the study population
|
Age group |
Value of the T4/T1 ratio at the first minute after extubation n (%) |
Total |
P=0,049 |
|||
|
< 70% |
[70-80%] |
[80-90%] |
>90% |
|||
|
[18-25] |
- |
- |
2 (22,2%) |
7 (77,8%) |
9 (100 %) |
|
|
[25 35] |
2 (12,5%) |
5 (31,3%) |
4 (25%) |
5 (31,3%) |
16 (100%) |
|
|
[35-45] |
6 (30%) |
2 (10%) |
3 (15%) |
9 (45%) |
20 (100%) |
|
|
[45-55] |
- |
1 (7,7%) |
4 (30,8%) |
8 (61,5%) |
13 (100%) |
|
|
[55-65] |
1 (6,7%) |
5 (33,3%) |
1 (6,7%) |
8 (53,3%) |
15 (100%) |
|
|
[65-75] |
3 (42,9%) |
- |
1 (14,3%) |
3 (42,9%) |
7 (100%) |
|
|
Total |
12 (15%) |
13 (16,3%) |
15 (18,8%) |
40 (50%) |
80 (100%) |
|
Table 2: Distribution of patients with postoperative residual curarization according to age group
|
Duration of surgery |
Value of the T4/T1 ratio after extubation n (%) |
Total |
P=0,002 |
|||
|
< 70% |
[70-80%] |
[80-90%] |
>90% |
|||
|
[30-90 min] |
1(11,8%) |
4(23,5%) |
9 (52,9%) |
2 (11,8%) |
16 (100 %) |
|
|
[90-180 min] |
7 (14,9%) |
7 (14,9%) |
4 (8,5%) |
29 (61,7%) |
47 (100%) |
|
|
>180 min |
3 (18,8%) |
2 (12,5%) |
2 (12,5%) |
9 (56,3%) |
16 (100%) |
|
|
Total |
12 (18,8%) |
13 (16,3%) |
15 (18,8%) |
40 (50%) |
80 (100%) |
|
Table 3: Distribution of patients with postoperative residual curarization according to the duration of surgery
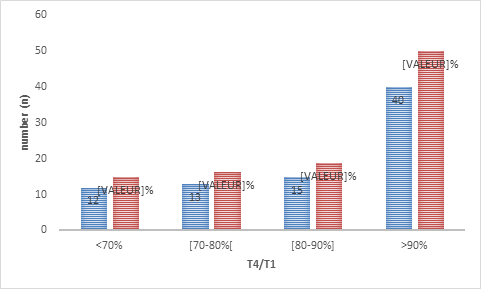
Figure 1: Distribution of patients according to the depth of curarization at the first minute after extubation.
4. Discussion
The study of postoperative residual curarization was carried out as part of an evaluation process of professional practices in order to assess the relevance of clinical extubation criteria in the prevention of postoperative residual curarization, and to improve patient safety in the operating room. Our study took place in a referral hospital center in Central Africa. This is the first study to assess postoperative residual curarization in Central Africa. The main limitations of the study are represented by the sample size and the monocentric nature of the study.
In the Canadian study carried out by Charlotte Dei Svaldi in 2014 [4] on residual curarization and the prediction of the time required for complete recovery from neuromuscular block, the mean age of the study population was 64 years with extremes ranging from from 36 to 91 years old. Our results are different from those obtained by these authors, and are probably explained by the demographic evolution in Cameroon. According to the results of the last population census in 2005, Cameroon still has slightly more women (50.6%) than men (49.4%). Half of the population is under 17.7 years old and the demographic weight of those under 15 is 43.6%. People over the age of 60 represent only 5.5% of the total population. The incidence of residual curarization at Essos hospital center is 50. Since 1979, Viby-Mogensen et al. [2] showed that 42% of patients considered clinically decurarized actually had a T4/T1 ratio <90%. Despite advances in pharmacology with the introduction of short-acting anesthesia drugs on the market, the incidence of residual curarization remains high. Residual curarization is still present in nearly one in two patients in the postoperative period [3]. The doubt about the postoperative curarization has been dispelled in France, two observational studies involving more than a thousand patients have confirmed the existence of postoperative residual curarization [5,6]. Leif Saager et all [7] found in their study a prevalence of residual curarization of 67.7%. In the series by Ismail Aytac et all [8], a survey on postoperative residual curarization, the incidence of residual curarization was 43% (n = 179) for the TOF <0.9 and 15% (n = 61) for the TOF <0.7. Majekodunmi and all in Nigeria found in their work that the incidence of residual curarization was 75.6% (n = 31), with severe postoperative residual curarization (T4/T1 <70%) observed in 41.5% ( n = 17) of the patients [9]. Residual curarization, defined by a T4/T1 ratio <90% at the adductor of the thumb at the train of four, remains an undeniable fact at the Essos hospital in 2020. The high prevalence testifies that the clinical criteria of extubation do not represent sufficient arguments to predict and/or detected residual postoperative curarization. Despite pharmacological progress, the incidence of residual curarization remains underestimated by anesthesiologists in view of the abundant literature on the subject [5-9]. Residual postoperative curarization is potentially the cause of complications, particularly on the respiratory level [8]. The prevention of these accidents is ensured by the choice of a curare of duration of action adapted to the type of surgery, the monitoring of the depth of the neuromuscular block during the operative period, and the systematic recourse to a pharmacological decurarization at the end of the surgery [8-10]. The frequency of complications induced by postoperative residual curarization was 40% in our study. Majekodunmi et al. [9] found no complications related to postoperative residual curarization in their work, but they suggest quantitative monitoring of residual paralysis as part of routine monitoring with the use of a curare monitor to improve the anesthetic safety of patients. In our study, antagonization of vecuronium bromide by neostigmine was achieved in 17.5% of cases. In the population of patients who benefited from antagonization of the action of vecuronium by neostigmine, 11.25% had persistent neuromuscular block, a T4 / T1 ratio <90% at the time of extubation. Antagonization of curarization should be done under the control of quantitative monitoring of neuromuscular block. The dose to be administered is a dose between 40 and 50 μg / kg adapted to the ideal mass of the patient. These concepts must be integrated into the algorithms for patient management in the operating room at Essos hospital center. Regarding the extubation of the patient at the end of the surgical intervention, the results of a survey carried out among residents of the anesthesia-resuscitation specialty of Île-de-France in 2008 [11] on the practices of Neuromuscular monitoring observed in the reception services revealed that the presence of a curarization monitor per operating room was reported in 56% (95% CI: 46–65%) of cases. They were 70% (95% CI: 60–78%) to use the curarization monitor for waking [11]. The decurarization threshold defined by a train-of-four (T4/T1) greater than or equal to 90% was respected in 55% (95% CI: 46–64%) of cases [11]. When indicated, 49% (95% CI: 40–58%) of residents reported that antagonization before extubation was performed systematically [11]. Significant residual curarization may occur if the T4/T1 ratio <90% [12,13]. In principle, it takes 30 to 60 min to go from surgical curarization (1-2 visible responses) when using an intermediate-acting curare such as vecuronium bromide, but some subjects are found outside these margins [12,13]. In the absence of monitoring, the time since the last dose does not guarantee complete decurarization. Indeed, even after 4 hours after administration of an intermediate-acting curare, some individuals show residual curarization [11-13]. The decision to use pharmacological decurarization should be based on a quantitative measurement of the T4/T1 ratio. It is strongly recommended to use quantitative monitoring of adductor curarization of the thumb for the diagnosis of residual curarization and to obtain a ratio between the fourth and the first response to the train of four (ratio T4/T1) higher or equal to 90% to the adductor of the thumb to formally rule out the diagnosis of residual curarization [12-14]. The level of postoperative residual curarization was deeper in the subject over 65 years of age and there was a significant correlation between the age range and the depth of postoperative residual curarization (p = 0.049). Aging is accompanied by physiological changes [14]. The decrease in lean mass, total body water and the increase in fat mass modify the distribution, but also the elimination of anesthetic agents in the elderly [15-17]. The physiological deterioration associated with age could explain the link between the depth of curarization and old age in our series. The initial curarizing doses of vecuronium are little affected by age, but the times to curarization and recovery may be slower, thus justifying the higher incidence of the depth of curarization in the elderly. Residual curarization was found mainly in the group of patients who had undergone short-term surgery in 88.2% of cases. This clinical situation could be explained by the high percentage of short-term surgery of less than 60 minutes in our sample. After an initial vecuronium dose of 0.1 mg / kg intravenously, the first maintenance dose is usually required within 25 to 40 minutes; subsequent maintenance doses, if required, can be given at approximately 12 to 15 minute intervals [17,18].
Conclusion
The prevalence of postoperative residual curarization remains high in our practice despite the use of clinical tests to aid in diagnosis. The practice of pharmacological decurarization remains empirical in sub-Saharan Africa, and particularly in Cameroon. The absence of residual postoperative curarization can only be confirmed by monitoring the curarization at the end of the operation. A T4/T1 ratio measured at the train-of-four at the adductor of the thumb of more than 90% is sufficient proof of this. Currently, no clinical test is sensitive enough to detect residual postoperative curarization. With a view to improving patient safety in anesthesia, the systematization of quantitative monitoring in the train of four would reliably avoid the presence of postoperative residual curarization and its complications.
Conflict of interest for each author
The authors declare no conflicts of interest.
Author Contribution
All authors contributed to the development and conduction of this manuscript. All authors have read and approved the final version of the manuscript.
Acknowledgments
The authors wish to thank the anesthesiologists, surgeons and the nursing staff of the operating theatre of the Yaounde/Essos Hospital Center for their support of this study.
References
- Arselen Ghribi, David Hajage, Marylin Smeyers et al. Comparison of performance of TOF Watch and TOF Scan for evaluation of residual curarization in morbidly obese patients. Anesthesia & Resuscitation 1 (2015): A361-A362.
- Viby-Mogensen J, Jorgensen BC, Ording H. Residual curarization in the recovery room. Anesthesiology 50 (1979): 539-41.
- Baillard C, Beaussier M. Residual curarization. Update Conferences 5 (2006): 113-120.
- Charlotte Dei Svaldi. Prediction of the time required for complete recovery from neuromuscular block after visual recovery from double burst stimulation. Life Sciences (2014).
- Debaene B, Plaud B, Dilly MP et al. Residual paralysis in the PACU after a single intubating dose of nondepolarizing muscle relaxant with an intermediate duration of action. Anesthesiology 98 (2003): 1042-1048.
- Baillard C, Gehan G, Reboul-Marty J, et al. Residual curarization in the recovery room after vecuronium. Br J Anaesth (2000): 394-395.
- Leif Saager, Eric M Maiese, Lori D Bash et al. Incidence, Risk Factors, and Consequences of Residual Neuromuscular Blockade in the United States: A Prospective, Observational, Multicenter RECITE-US Study. J Clin Anesth 55 (2019): 33-41.
- Aytac, Ismail, Aysun Postaci et al. Investigation of postoperative residual curarization, acute respiratory events and the approach of anesthesiologists. Rev Bras de Anestesiol 66 (2016): 55-62.
- AA Majekodunmi, OA Ikotun, OD Oladokun. Incidence of postoperative residual paralysis in a nigerian teaching hospital. Nigerian Journal of clinical practice 20 (2017): 1561-1565.
- Butterly A, Bittner EA, George E et al. Postoperative residual curarization by intermediate-acting neuromuscular blocking agents delays exit from the recovery room. BJA 105 (2010): 304-309.
- Solis A, Cherradi N, Beloucif S, et al. Evaluation of neuromuscular monitoring practices in the operating room by residents of Île-de-France. French Annals of Anesthesia-Resuscitation 27 (2008): 896-899.
- Benoît P, Christophe B, Jean-LB et al. Guidelines on muscle relaxants and reversal in anaesthesia. Anaesth Crit Care Pain Med 39 (2020): 125-142.
- Naguib M, Kopman AF, Lien CA et al. A survey of current management of neuromuscular block in the United States and Europe. Anesth Analg 111 (2010): 110-119.
- Debaene B. How do I use curarization monitoring in practice? MAPAR (2016): 433-443.
- de Jaeger. Physiology of aging. EMC - Physiotherapy-Physical Medicine-Rehabilitation 14 (2018): 1-11.
- Passot, M. Stehlin. Pharmacology applied to the anesthesia of the great old man S. 52nd national congress of anesthesia and resuscitation. The French Society of Anaesthesia, Critical Care and perioperative Medecine - SFAR (2010).
- Thomas Fuchs-Buder, Denis Schmartz. How to master the use of muscle relaxants? The Practitioner in Anesthesia Resuscitation 21(2017): 212-215.
- Duvaldestin P, Cunin P, Plaud B et al. Practice survey on the use of muscle relaxants in adults in anesthesia in France. French Annals of Anesthesia and Resuscitation (27) 2008: 483-489.
