Post-Operative Astigmatism Using Clear Corneal Tunnel Incision in Children with Developmental Cataract
Article Information
Urmi Atika Islam1, *, Jannatun Noor2, Nasimul Gani Chy3, Jewel Das Gupta4
1Teaching Assistant, Institute of Community Ophthalmology (ICO), Chittagong Eye Infirmary & Training Complex Campus, Chittagong.
2Teaching Assistant, Institute of Community Ophthalmology (ICO), Chittagong Eye Infirmary & Training Complex Campus, Chittagong.
3Senior Consultant, Pediatric Department, Chittagong Eye Infirmary & Training Complex (CEITC), Chittagong.
4Lecturer and Course co-ordinator, Institute of Community Ophthalmology (ICO), Chittagong Eye Infirmary & Training Complex Campus, Chittagong.
*Corresponding author: Urmi Atika Islam, Teaching Assistant, Institute of Community Ophthalmology (ICO), Chittagong Eye Infirmary & Training Complex Campus, Chittagong, Bangladesh.
Received: 11 October 2021; Accepted: 27 October 2021; Published: 07 March 2022
Citation: Urmi Atika Islam, Jannatun Noor, Nasimul Gani Chy, Jewel Das Gupta. Post-Operative Astigmatism Using Clear Corneal Tunnel Incision in Children with Developmental Cataract. Journal of Ophthalmology and Research 5 (2022): 35-42.
View / Download Pdf Share at FacebookAbstract
Purpose: To evaluate the post-operative changes in astigmatism in Pseudophakic eyes of children using sutured clear corneal incisions.
Methods: The charts of children who underwent surgery for developmental Cataract using clear corneal tunnel incision at 10’O clock and 2’O clock position were retrospectively reviewed. All the sutures from cornea were removed after 1 month of surgery. Refraction was done at 1 month, 3months 6 months and 1 year interval. Statistical analysis was done by SPSS version 16.
Result: With the rule astigmatism was highest in the study cases. By postoperative 1 month, 3 months, 6 months and 1 year, there was a shift to With the Rule Astigmatism with 73.7%, 76.3%, 78.9% and 86.8% of eyes respectively. Astigmatism became stable after 6 months of surgery. There were no significant changes in astigmatism after 6 months or 1 year of surgery.
Conclusion: Clear corneal incision at 10’O clock and 2’O clock did not significantly influence preoperative existing astigmatism. There was no significant change in astigmatism after 6 months & 1 year of surgery.
Keywords
<p>Astigmatism, Corneal Tunnel, With the Rule Astigmatism</p>
Article Details
1. Intruduction
Though several surgical approaches have been suggested, the introduction of clear corneal incisions revolutionized Cataract surgery in children. Nowadays, this is perhaps the most popular and widely accepted approach to perform Pediatric Cataract surgery. Because of low corneo-scleral rigidity in children, clear corneal wound are usually sutured.
The refractive condition of the eye regards as refractive components (corneal power, lens power, anterior chamber depth, and axial length) which are interdependent rather than independent variables. During the early years in life the eye grows in such a way that the refractive state tends towards emmetropia [1, 2].The human eye refractive status is reliant on the balance of change in overall eye size and refractive components, that is to say, the cornea and crystalline lens [3].
Humans are typically born with a wide variation of defocus. During the first year of postnatal development, as normal emmetropization proceeds, axial length increases significantly whereas both the cornea and the crystalline lens lose its powers by flattening. The majority of axial length elongation takes place in the first three to 6 months of life and a gradual declining rate of growth over the next two years [4] and by three years the adult eye size is obtained [5]. After the age of three, there are still increases in axial length and the anterior chamber depth, with a significant reduction in the crystalline lens power, but there is limited change in the corneal power [6, 7].
Astigmatism happens more commonly in infancy in compared to the general adult population. Photometric measurements suggest corneal curvature as the major component of infantile astigmatism. Longitudinal studies have demonstrated a decreased in the incidence of astigmatism with age, with the most notable changes occurring between the first & second year of life [8].There is also a change in the axis of astigmatism; thus, by age 6, with the rule astigmatism predominates [9]. Abrahamson et al [10]. Suggested that there is no actual change in cylinder axis in individual cases; however, an increased number of cases of with the rule astigmatism and a decreased number of cases of against the rule astigmatism occurred at age 3 to 4 years. In infants, with a high degree of infantile astigmatism particularly with oblique axis, the astigmatism may not revert to normal.
In adults, corneal astigmatism is a well reported finding after cataract surgery. The amounts of astigmatism controlled by various factors, such as the type and location of the surgical incision, the amount of scleral cauterization performed, the suturing material and suture placement, use of steroid postoperatively [11-14]. The preoperative existing astigmatism also influences the postoperative refractive error of the child.
These study approaches to find out the astigmatic changes after Developmental Cataract Surgery with Intraocular Lens Implantation using corneal tunnel incision in children.
2. Patients and Methods
This retrospective review was conducted in 20 children who were previously diagnosed as developmental cataract and surgeries were performed in Chittagong Eye infirmary & training complex (CEITC), Chattogram between June 2019 to June 2020. Data were included on age, gender, time interval of surgeries between two eyes, preoperative Keratometry reading and post-operative astigmatism. Exclusion criteria were associated ocular anomalies, systemic and mental disorders, children below 3years and follow up less than 1 year. All surgeries were performed by a single pediatric ophthalmologist and children were followed up according to a defined protocol.
The preoperative examination included Visual acuity, slit lamp bio microscopy, direct and indirect ophthalmoscopy after full dilatation and B-scan ultrasonography. Intraocular lens (IOL) power calculations were made by using the SRK-II formula on the basis of axial length (A scan) and keratometric readings. IOL power was adjusted according to Dahans formula.
All the patients underwent cataract surgeries under General Anesthesia (GA) with spontaneous ventilation. Corneal tunnels were done at 10’O clock and 2’O clock by MVR blade. Adrenaline was injected into anterior chamber to dilate the pupil. Trypan blue was used to stain the anterior capsule of lens. An irrigating cystitome was inserted into the anterior chamber to create continuous curvilinear capsulorrhexis (CCC).Aspiration of lens was accomplished by using an automated I/A hand piece with Optikon 2000 S.P.A system (Model-PULSAR-2). After in bag implantation of soft foldable hydrophobic acrylic lenses (Alcon, MBI), primary posterior Capsulectomy (Vitrectorrhexis) and anterior vitrectomy were done in all cases by automated vitrectomy machine. Corneal tunnel were closed by 10-0 nylon. All patients received a sub-conjunctival injection of Gentamicine (5mg) and dexamethasone (2mg).The eye remain padded until the 1st post-operative examination.
Children were discharged from the hospital after one day of surgery and were reviewed after one week, one month, three months and at six months of interval. Atropine and antibiotics eye drops were continued up to one month. Steroid eye drop was reduced slowly over the following 8 weeks. All the sutures from cornea were removed after 1 month of surgery.
VA was measured by CSM method, crowding Kay Picture test (KPT), Lea symbol and Snellen charts. Streak retinoscopy was done in every case. The best corrected visual acuity was recorded according to subjective refraction. Refraction and spectacles prescription were given at 4 weeks after removal of corneal sutures. Part time occlusion (4 to 6 hours) and active vision therapy were given for amblyopic eyes.
SPSS version 16 was used for analysis. Descriptive analysis and central tendency were used for analysis. The Friedman (k dependent) test and Wilcoxon signed test were used to compare the outcome variables at the different postoperative periods. A value of P <0.05 was defined as statistically significant.
3. Results
A total 38 eyes of 20 patients with developmental cataract (14 Boys and 6 Girls) were included in this study. The mean patient age at surgery was 6.62±3.04 years (range 3 year to 12 years).Time interval of surgeries between 2 eyes was 2.16±1.29 months. Post-operative VA of the respondents at 1 month, 3 months, 6 months & 1 year are depicted in table 01.
Mean preoperative refractive astigmatism was 1.41±.90 (D). Mean postoperative refractive astigmatism at 1 month after surgery was 1.16±.84 (D). The mean astigmatism was 1.20±.81 (D) at postoperative 3 moths. At postoperative month 6, the mean refractive astigmatism was 1.22±.79 (D) and 1.23±.68 at 1 year. The decrease in refractive astigmatism from preoperative to postoperative 1 year was statistically significant (p=0.006), but the difference from postoperative month 1 to postoperative 1 year was not significant (p=0.199). (Table 2)
The type of astigmatism was classified into 3 subgroups. Preoperatively, 92.1% of eyes had WTR astigmatism, 2.6% had ATR astigmatism, and 5.3% had oblique astigmatism. At post-operative month 1, 73.7% had WTR astigmatism, 5.2% had ATR astigmatism, and 7.9% had oblique astigmatism. About 13.1% percent were astigmatically neutral. By postoperative 3 months, 6 months and 1 year, there was a shift to WTR astigmatism with 76.3%,78.9% and 86.8% of eyes respectively in this category which was statistically significant (p=0.045) showed in table 3.
|
Post-operative BCVA |
Post-operative VA at 1 month Eyes (%) |
Post-operative VA at 3 months Eyes (%) |
Post-operative VA at 6 months Eyes (%) |
Post-operative VA at 1 year Eyes (%) |
|
6/6 |
13.2 |
15.8 |
15.8 |
23.7 |
|
6/9-6/18 |
44.7 |
39.5 |
55.4 |
50 |
|
<6/18-3/60 |
13.1 |
15.7 |
13.1 |
10.5 |
|
<3/60 |
- |
- |
2.6 |
10.6 |
|
CSM +ve |
28.9 |
28.9 |
13.2 |
5.3 |
|
CSM -ve |
- |
- |
- |
- |
|
Total |
100.0 |
100.0 |
100.0 |
100.0 |
Table 1: Post-operative Visual Acuity of the Bespondents
|
Time |
Refractive astigmatism Mean±SD |
|
Pre-op (keratometric) |
1.41±.90 |
|
Post-op at 1 month |
1.26±.84 |
|
Post-op at 3 months |
1.20±.81 |
|
Post-op at 6 months |
1.22±.79 |
|
Post-op at 1 year |
1.23±.68 |
Table 2: Mean Postoperative Refractive Astigmatism
|
Time |
Astigmatism type Eyes (%) |
No astigmatism Eyes (%) |
||
|
With the rule |
Against the rule |
Oblique |
||
|
Pre-op (keratometric) |
92.1 |
2.6 |
5.3 |
- |
|
Post-op at 1 month |
73.7 |
5.2 |
7.9 |
13.2 |
|
Post-op at 3 months |
76.3 |
2.6 |
7.9 |
13.2 |
|
Post-op at 6 months |
78.9 |
- |
7.9 |
13.2 |
|
Post-op at 1 year |
86.8 |
- |
7.9 |
5.3 |
Table 3: Types of postoperative Astigmatism at different periods
4. Discussion
In this study, we evaluated the change in postoperative refractive astigmatism in pediatric patients after cataract extraction with IOL implantation using temporal and nasal clear corneal incision closed with 10-0 nylon suture.
The findings of postoperative astigmatism are important, especially in children, because of its adverse effect on vision development and the risk of amblyopia. In adults, a few months of delay in correcting the refractive error does not affect the final visual acuity, whereas in children, the optical refraction must be precisely corrected as soon as possible.
In this study, Preoperative refractive astigmatism mean was 1.41±0.90 diopters (D) whereas the postoperative refractive astigmatism one year after surgery was 1.23±0.68(D).The decrease in refractive astigmatism from preoperative to postoperative 1 year was statistically significant (p=0.006), according to Wilcoxon signed rank test. Our patients also had a shift toward WTR astigmatism over time. Previous studies have demonstrated that flattening of the cornea occurs along the incisional meridian [15].This results in with the rule astigmatic changes when a temporal incision is used [15, 16], consistent with the result of our study.
Our results are comparable to the study by Spierer and Bar-Sela which showed that in clear-corneal cataract incisions, postoperative astigmatism declines significantly by 3 months postoperatively, and stabilizes by 3 to 5 months postoperatively [17, 18].
Our data is comparable to the clear corneal incision data from the study by Bradfield et al., which showed a postoperative astigmatism range of 0-4.50D the first month after surgery [19] however in that study a superior clear corneal incision was used. Some studies have demonstrated that temporal incisions induce less astigmatism than superior wounds [15, 20] but others have shown comparable results [15].
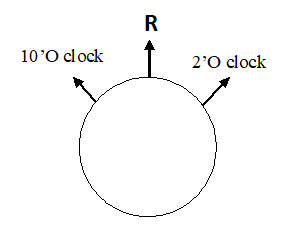
Preoperatively, 92.1% of eyes had WTR astigmatism, 2.6% had ATR astigmatism, and 5.3% had oblique astigmatism. At post-operative month 1, 73.7% had WTR astigmatism, 5.2% had ATR astigmatism, and 7.9% had oblique astigmatism. About 13.1% were astigmatically neutral. By postoperative 3 months, 6 months and 1 year, there was a shift to WTR astigmatism with 76.3%,78.9% and 86.8% of eyes respectively in this category which was statistically significant (p=0.045).In this study, majority of the cases of preexisting with the rule astigmatism remains as it is after 1 year of surgery. The probable explanation is that traction in the 10’O clock and 2’O clock position creates vector resulting in 12’ O clock position (900) which causes with the rule astigmatism. (figure-01)
A small portion of the children (13.2%) gains 6/6 visual acuity range after one month’s post-operative follow up which percentage was gradually increased as near as one quarter(23.7%) at the range of 6/6 visual acuity group after one year post-operative follow up. Maximum visual acuity percentage (44.7%) was in the range of visual acuity 6/9 to 6/18 at first one month follow up which was noticeably increased (55.4%) at 6 months follow up after surgery. However, Amblyopia was found in 33.3% of eyes.
Limitations include smaller sample size and difficulty in actual quantification of visual acuity in children.
5. Conclusion
Postoperative refractive astigmatism in pediatric patients can be expected to occur after sutured temporal and nasal clear corneal tunnel cataract surgery with IOL placement. This refractive astigmatism decreases early after surgery and seems to stabilize by the first 3 to 6 months after surgery. There was no significant change in astigmatism after 6 months & 1 year of surgery. Because the amount of astigmatism may be higher in the early postoperative period, it requires close follow-up after surgery. Consideration should be given to reassess refraction in the first few months after surgery to ensure optimal correction of refractive error in patients in the amblyopic age range.
Acknowledgements
We would like to express our gratitude to all the staffs of Pediatric and Low vision departments of Chittagong Eye infirmary & training complex (CEITC) for their support during data collection. We also thankful to those guardians of children who maintain regular postoperative follow up and support us to make this study successful.
Conflicts of Interest
The authors declare that there are no conflicts of interest regarding the publication of this study.
References
- Stenstrom, “Investigation of the variation and correlation of the optical elements of human eyes,” American Journal of Optometry & Archives of American Academy of Optometry 25 (1949): 496–504.
- J. Hirsch and F. W. Weymouth, “Notes on ametropia: a further analysis of Stenstrom's data,” American Journal of Optometry & Archives of American Academy of Optometry 24 (1947): 601–608.
- Troilo, “Neonatal eye growth and emmetriopisation-a literature review,” Eye 6(1992): 154–160.
- Duke elder WS. System of ophthalmology. Ophthalmic optics and refraction 5 (1970): 238.
- Grosvenor and R. Scott, “Role of the axial length/corneal radius ratio in determining the refractive state of the eye,” Optometry and Vision Science 71 (1994): 573–579.
- Investigation of the variation and the correlation of the optical elements of human eyes. Am J Optom 25 (1948): 218–232.
- Sorsby A, Leary GA. A Longitudinal Study of Refraction and Its Components during Growth. 1970;Her Majesty’s Stationery Office London.publication 309 (1970): 1-41.
- Atkinson J, Braddick O, French J. Infant astigmatism: its disappearance with age. Vision research 20 (1980): 891-3.
- Gwiazda J, Scheiman M, Mohindra I, Held R. Astigmatism in children: changes in axis and amount from birth to six years. Investigative ophthalmology & visual science 25 (1984): 88-92.
- Abrahamsson M, Fabian G, Sjöstrand J. Changes in astigmatism between the ages of 1 and 4 years: a longitudinal study. British journal of ophthalmology 72 (1988): 145-9.
- Spierer, A., Nahum, A. Changes in astigmatism after congenital cataract surgery and intraocular lens implantation using scleral tunnel incision Eye16 (2002): 466–468.
- Jaffe NS. Cataract Surgery and its Complications, 3rd ednCV Mosby: St Louis (1981): 92–110.
- Seeto R, Ng S, McClellan K, Billson FA. Non absorbable suture material in cataract surgery: a comparison of Novafil and nylon. Ophthalmic Surg33 (1992): 538–544.
- Lim TS, Gunning FP, Greve EL . Astigmatism following cataract surgery: comparison of a scleral and a corneal incision in a mixed group of patients with and without glaucoma. Int Ophthalmol16 (1992): 177–183.
- Oshika T, Sugita G, Tanabe T, Tomidokoro A, Amano S. Regular and irregular astigmatism after superior versus temporal scleral incision cataract surgery. Ophthalmology 107 (2000): 2049–53.
- Barequet IS, Yu E, Vitale S, Cassard S, Azar DT, Stark WJ. Astigmatism outcomes of horizontal temporal versus nasal clear corneal incision cataract surgery. J Cataract Refract Surg30 (2004): 1418–23.
- Speirer A, Bar-Sela SM. Changes in astigmatism after congenital cataract surgery and intraocular lens implantation. Arch Ophthalmol 122 (2004): 695–7.
- Speirer A, Bar-Sela SM. Changes in astigmatism after congenital cataract surgery and foldable intraocular lens implantation J AAPOS 41 (2004): 35–8.
- Bradfield YS, Plager DA, Neely DE, Sprunger DT, Sondhi N. Astigmatism after small-incision clear corneal cataract extraction and intraocular lens implantation in children. J Cataract Refract Surg. 30 (2004): 1948–52.
- Roman SJ, Auclin FX, Chong-Sit DA, Ullern MM. Surgically induced astigmatism with superior and temporal incisions in cases of with-the-rule preoperative astigmatism. J Cataract Refract Surg 24 (1998): 1636–41.