Peak Exercise Cardiac Output but Not Oxygen Uptake Increases in All Heart Failure Patients After Successful Resynchronization Therapy
Article Information
Gaia Cattadori1#, Carlo Vignati2,5#, Alice Bonomi2, Massimo Mapelli3,5, Susanna Sciomer3, Mauro Pepi2, Claudio Tondo2, Giuseppe Ambrosio4, Silvia Di Marco1, Massimo Baravelli1, Piergiuseppe Agostoni2,5*
1IRCCS Multimedica, Milan, Italy
2Centro Cardiologico Monzino IRCCS, Milan, Italy
3Department of Cardiovascular, Respiratory, Nephrological, Anesthesiological and Geriatric Sciences, University of Rome 'Sapienza', Rome, Italy
4Division of Cardiology, Department of Medicine, University of Perugia, Perugia, Italy
5Department of Clinical Sciences and Community Health, University of Milan, Milan, Italy
*Corresponding Authors: Piergiuseppe Agostoni, Centro Cardiologico Monzino, IRRCS, Department of Clinical Sciences and Community Health, University of Milan, Via Parea 4, 20138 Milan, Italy
#Both authors share the first author privileges and responsibilities
Received: 06 April 2020; Accepted: 13 April 2020; Published: 03 August 2020
Citation: Gaia Cattadori, Carlo Vignati, Alice Bonomi, Massimo Mapelli, Susanna Sciomer, Mauro Pepi, Claudio Tondo, Giuseppe Ambrosio, Silvia Di Marco, Massimo Baravelli, Piergiuseppe Agostoni. Peak Exercise Cardiac Output but Not Oxygen Uptake Increases in All Heart Failure Patients After Successful Resynchronization Therapy. Cardiology and Cardiovascular Medicine 4 (2020): 386-395.
View / Download Pdf Share at FacebookAbstract
Objectives and Background: Hemodynamic changes at rest and during exercise in heart failure (HF) after cardiac resynchronization therapy (CRT) are still undefined.
Methods: In 93 HF patients, before and 8 ± 3 months after CRT, we assessed clinical conditions, ECG and standard echocardiography and we performed a maximal cardiopulmonary exercise test with non-invasive measurement of cardiac output (CO) by inert gas rebreathing method.
Results: At rest, CRT shortened QRS and improved NYHA class and left ventricular ejection fraction (LVEF), but not CO and stroke volume (SV). On average, at peak exercise, a significant improvement of oxygen uptake (VO2) (from 13.8 ± 3.8 ml/min/kg to 14.9 ± 4.6, p<0.0025), CO (from 6.19 ± 1.82 L/min to 6.97 ± 2.21, p<0.0001), and SV (from 62 ± 18 mL to 71 ± 19, p<0.0001) were detected. Regardless of HF severity, after CRT, patients showed a significant peak SV and CO increase, but a significant peak VO2 increase was observed only in patients with the lowest pre-CRT peak VO2 (5.9-11.3 ml/kg/min).
Conclusions: Our data showed that: a) SV at rest was not affected by CRT, regardless of LVEF improvement; b) post-CRT peak VO2 improvement was limited to HF patients with low pre-CRT peak VO2; c) post-CRT, a similar peak CO increase was observed regardless of pre-CRT peak VO2. Consequently, the assessment of peak CO is preferable to analyze CRT effects on exercise.
Keywords
Cardiac Resynchronization Therapy; Heart Failure; Cardiac Output
Article Details
1. Introduction
Cardiac resynchronization therapy (CRT) is nowadays an established treatment for heart failure (HF) [1-6]. CRT was conceived by the observation that an enlargement of QRS is frequent in HF patients, it is often the expression of mechanical dissynchrony of cardiac contraction and it is associated with poor prognosis [7]. The effects of CRT are evident in the acute setting as a reduction of QRS and left ventricular (LV) volumes and as an improvement of LV function. In the chronic setting, CRT is associated with NYHA class reduction [7], LV inverse remodeling, LV ejection fraction increase (EF) [8], and peak oxygen uptake (VO2) increase [9-11], leading to mortality and morbidity improvement [12]. However, the precise hemodynamic mechanism by which CRT improves HF patients’ condition, both at rest and during exercise, is still undefined. This study was conceived to assess whether and how CRT improves HF patients’ hemodynamic patterns at rest and during exercise.
2. Methods
2.1 Study Population
We studied subjects belonging to a cohort of HF patients regularly followed at our HF Units. All patients had been previously familiarized with cardiopulmonary exercise test (CPET). Study inclusion criterion was the presence of the main recognized criteria for CRT selection at the time of inclusion, specifically QRS width>120 msec with a left bundle branch block (LBBB) morphology, HF with reduced ejection fraction (HFrEF) due to ischemic or dilated cardiomyopathy with a LVEF <35%, presence of sinus rhythm and NYHA class II or III (1-6). Patients also had to be capable of performing CPET and the respiratory maneuvers needed for cardiac output (CO) determination by inert gas rebreathing (IGR). Study exclusion criteria were comorbidities or other limitations that interfere with performing measurements during effort, major cardiovascular events or cardiovascular procedures within the previous 6 weeks, cardiovascular procedures planned within the next 6 months, significant pulmonary dysfunction. The study complies with the Declaration of Helsinki, the locally appointed Ethics Committee approved the research protocol (CCM-473), and informed consent was obtained from all patients.
2.2 Study design
2.2.1 Pre-CRT evaluation: Before CRT, all patients received careful clinical evaluation associated with collection of history and recent instrumental data to confirm CRT selection. All subjects underwent an ECG, a standard echocardiogram, a CPET for familiarization purposes, and at least one teaching section to understand and familiarize with the IGR methodology. Finally, a CPET based on a personalized ramp protocol aimed at achieving maximal effort was performed, along with a measurement of CO by IGR at rest and at peak exercise. Arteriovenous O2 content difference (ΔC(a-v)O2) was calculated following the Fick principle: peak VO2 = CO × ΔC(a-v)O2. Resting stroke volume (SV) was calculated both by IGR following the formula: CO/heart rate (HR), and by echocardiographic method following the formula: end-diastolic volume (EDV) - end-systolic volume (ESV).
2.2.2 Post-CRT evaluation: After at least 6 months of follow-up (range 6-16), all patients underwent clinical and instrumental re-evaluation, performing a CPET with CO measurement at rest and at peak exercise and using the same ramp workload protocol of the pre-CRT test. Data analysis was performed considering the entire population and assessing patients with different exercise performance. To do so, patients were grouped considering pre-CRT tertiles of peak VO2.
2.3 Echocardiography
Standard two-dimensional, color, and spectral Doppler measurements were performed. No specific data on ventricular dissynchrony were collected. LVEF was determined using the Simpson’s rule algorithm by tracing the left ventricular 2D-area in standard apical two- and four-chamber view at end-systole and end-diastole [13].
2.4 Ramp Protocol CPET
CPET was performed on a cycle ergometer with progressive work-rate increase in a ramp pattern, after 3 minutes of rest and 3 minutes of unloaded cycling. Expiratory O2, carbon dioxide (CO2), and ventilation were measured breath by breath (Innocor® rebreathing system, Innovision A/S, Odense, Denmark). A 12-lead ECG was recorded continuously during the test (Marquette, Case800, Milwaukee, WI). Patients were strongly encouraged to perform a maximal test, allowing the final 30 seconds for the rebreathing maneuver. The work-rate increase during the test was set to achieve peak exercise in 8 to 10 minutes during the increasing work-rate period [14, 15]. Peak VO2 is reported as a mean over the last 20 seconds [15].
2.5 CO measurement
Non-invasive CO measurements were performed during CPET at baseline and at peak exercise using the Innocor rebreathing system (Innovision A/S, Odense, Denmark) [16-21]. The IGR technique uses an oxygen-enriched mixture of an inert soluble gas (0.5% nitrous oxide-N2O) and an inert insoluble gas (0.1% Sulphur Hexafluoride-SF6) from a pre-filled bag. Patients breathe into a respiratory valve via a mouthpiece and a bacterial filter with a nose clip. At the end of the expiration, the valve is activated, so that the patient re-breaths from the pre-filled bag for a period of 10-20 seconds. After this period, the patient is switched back to ambient air, and CO measurement is terminated. Photo-acoustic analyzers measure gas concentration over a 5-breath interval. SF6 is insoluble in blood, and it is used to determine lung volume. N2O is soluble in blood, and its concentration decreases during rebreathing with a rate proportional to pulmonary blood flow (PBF), that is the blood flow that perfuses the active part of the alveoli. CO is equal to PBF when the arterial oxygen saturation measure (SpO2) is high (>98% using the pulse oximeter), showing the absence of pulmonary shunt flow or the presence of only a negligible one. Two experts independently read each test, and the results were averaged.
2.6 Statistical analysis
Continuous variables were presented as mean ± standard deviation (SD). Differences between before and after CRT were evaluated by paired t-test. The differences between patients in tertiles of pre-CRT peak VO2 were measured by ANOVA. Tests were two sided. P-values <0.05 were considered statistically significant. Analyses were performed by SAS version 9.4 (SAS Institute Inc., Cary, NC).
3. Results
Of the 100 patients enrolled, 7 were unable to complete the follow-up for different reasons: 1 subject died (cardiovascular death), 2 had cerebral strokes, 1 had atrial fibrillation, 1 had aortic aneurism, 1 became unable to perform exercise due to claudicatio intermittens, and 1 subject was lost to follow-up. The data of the remaining 93 patients (age 67 ± 10; M/F 77/16) were analyzed (Table 1 and Table 2). CRT was successfully implanted in all 93 subjects without major complications. CPET with CO measurement at rest and at peak exercise was performed in all patients, before and after CRT (average time between tests 8 ± 3 months).
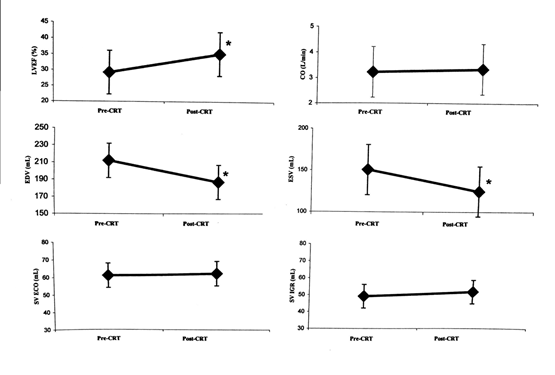
NYHA class, QRS, echocardiographic data, and measures of resting VO2, CO, SV, HR, and ΔC(a-v)O2 of the entire population before and after CRT are reported in Table 1. On average, CRT significantly shortened QRS (from 166 ± 25 msec to 138 ± 27, p<0.0001) and improved NYHA class (from 2.5 ± 0.5 to 2.0 ± 0.4, p<0.0001), LVEF (from 28.2 ± 6.3% to 35.1 ± 9.1, p<0.0001), and ESV (from 150 ± 60 ml to 125 ± 58, p<0.0001), confirming a positive response to CRT according to the usually applied parameters for CRT efficacy evaluation. Differently, no CO or SV difference was observed at rest after CRT. Figure 1 shows that, regardless of the LVEF improvement, resting CO and SV-the latter measured both by IGR and by echocardiography-remained unchanged after CRT.
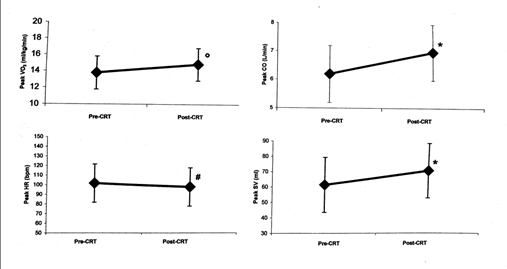
At peak exercise, significant improvements of peak VO2 (from 13.8 ± 3.8 ml/min/kg to 14.9 ± 4.6, p<0.0025), CO (from 6.19 ± 1.82 L/min to 6.97 ± 2.21, p<0.0001), and SV (from 62 ± 18 mL to 71 ± 19, p<0.0001) were detected (Table 2 and Figure 2).
Functional capacity changes after CRT were also evaluated grouping patients into tertiles of pre-CRT peak VO2. Patients with the lowest pre-CRT peak VO2 (Group 1: 5.9 - 11.3 ml/kg/min, mean 9.7 ± 1.2) showed a significant peak VO2 increase after CRT (from 9.6 ± 1.2 ml/min/kg to 11.7 ± 2.3, ΔVO2 2.1 ± 1.4). Patients with pre-CRT peak VO2 between 11.4 and 15.4 ml/kg/min (Group 2; mean peak VO2 13.2 ± 1.3) and those with peak VO2 between 15.5 and 23.1 ml/kg/min (Group 3; mean 18.1 ± 2.4,) had no significant peak VO2 improvement after CRT from 13.2 ± 1.3 ml/min/kg to 13.7 ± 3.7, ΔVO2 0.3 ± 2.4 ml/min/kg and from 18.1 ± 2.4 to 18.9 ± 2.4, ΔVO2 0.8 ± 1.7 (Figure 3).
After CRT, regardless of pre-CRT peak VO2 all patients showed a significant peak exercise SV increase from 58 ± 17 mL to 63 ± 17 (ΔSV 6 ± 17), from 59 ± 17 to 72 ± 21 (ΔSV12 ± 14) and from 69 ± 18 to 80 ± 17 (ΔSV 11 ± 16) in Group 1, 2 and 3 respectively and a significant peak CO increase from 4.8 ± 1.1 L/min to 5.5 ± 1.4 (ΔCO 0.7 ± 0.3), from 6.2 ± 1.8 to 7.0 ± 2.2, (ΔCO 0.8 ± 0.6) and from 7.5 ± 1.4 to 8.3 ± 2.0, (ΔCO 0.8 ± 0.6 L/min) in Group 1, 2 and , respectively, showing that, unlike peak VO2, peak SV and CO increase are independent of pre-CRT functional performance. Differently, ΔC(a-v)O2 at peak exercise showed a non-significant increase in Group 1 (Δ0.7 ± 0.1, p=0.25), a reduction in Group 2 (Δ-1.1 ± 0.2, p=0.027) and a non-significant reduction in Group 3 (Δ-0.6 ± 0.2, p=0.24) (Figure 3).
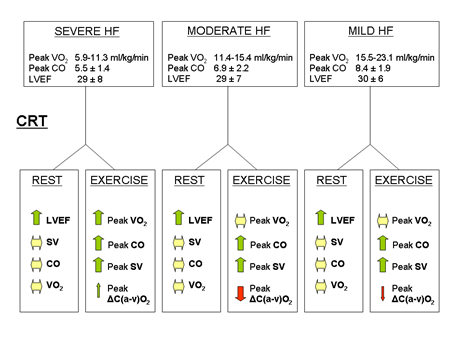
In brief, at rest, CRT improves LVEF but not CO or SV in all categories of HF. At peak exercise, CRT improves SV and CO in all patients, but it increases peak VO2 only in severe HF patients (Figure 3).
|
NYHA class |
Pre-CRT |
Post-CRT |
p |
|
2.5 ± 0.5 |
2.0 ± 0.4 |
<.0001 |
|
|
QRS (ms) |
166 ± 25 |
138 ± 27 |
<.0001 |
|
LVEF (%) |
28.2 ± 6.3 |
35.1 ± 9.1 |
<.0001 |
|
EDV (mL) |
212 ± 69 |
187 ± 69 |
<.0001 |
|
ESV (mL) |
150 ± 60 |
125 ± 58 |
<.0001 |
|
MI (grade) |
1.28 ± 0.81 |
1.05 ± 0.67 |
0.0004 |
|
VO2 (mL/min) |
300 ± 82 |
312 ± 70 |
0.1852 |
|
CO (L/min) |
3.23 ± 1.03 |
3.36 ± 0.94 |
0.3559 |
|
HR (bpm) |
67 ± 12 |
66 ± 10 |
0.1091 |
|
SV (ml) |
49 ± 18 |
52 ± 15 |
0.1262 |
|
ΔC(a-v)O2 (mL/100mL) |
9.9 ± 3.5 |
9.8 ± 3.0 |
0.7562 |
CRT: cardiac resynchronization therapy; NYHA: New York Heart Association; LVEF: left ventricular ejection fraction; EDV: end-diastolic volume; ESV: end-systolic volume; MI: mitral insufficiency; VO2: oxygen consumption; CO: cardiac output; HR: heart rate; SV: stroke volume; ΔC(a-v)O2: arterial-venous O2 content difference
Table 1: Pre- and post-CRT measurements at rest.
|
Peak RER |
Pre-CRT |
Post-CRT |
p |
|
1.1 ± 0.1 |
1.05 ± 0.11 |
0.5018 |
|
|
Peak WR (watt) |
67 ± 30 |
70 ± 30 |
0.0573 |
|
Peak VO2 (mL/min) |
1067 ± 357 |
1156 ± 377 |
0.0006 |
|
Peak VO2/kg (mL/min/kg) |
13.8 ± 3.8 |
14.9 ± 4.6 |
0.0025 |
|
Peak VO2 (%pred) |
58 ± 15 |
62 ± 14 |
0.0003 |
|
Peak CO (L/min) |
6.19 ± 1.82 |
6.97 ± 2.21 |
<.0001 |
|
Peak ΔC(a-v)O2 (mL/100mL) |
17.1 ± 3.0 |
16.74 ± 2.87 |
0.2551 |
|
Peak HR (bpm) |
102 ± 20 |
98 ± 18 |
0.0166 |
|
Peak SV (ml) |
62 ± 18 |
71 ± 19 |
<.0001 |
|
VE/VCO2 slope |
37 ± 8 |
35 ± 10 |
0.0333 |
|
VO2 AT/kg (mL/min/kg) |
9.1 ± 4.3 |
11.1 ± 2.9 |
<.0001 |
CRT: cardiac resynchronization therapy; RER: respiratory equivalent ratio; WR: work rate; VO2: oxygen consumption; CO: cardiac output; ΔC(a-v)O2: arterial-venous O2 content difference; HR: heart rate; SV: stroke volume; VE: ventilation; VCO2: carbon dioxide production; AT: anaerobic threshold
Table 2: Pre- and post-CRT measurements at Peak exercise
Figure 1: Changes in left ventricular ejection fraction (LVEF), cardiac output (CO), end-diastolic volume (EDV), end-systolic volume (ESV), stroke volume by echocardiogram (SV ECO), and stroke volume by inert gas rebreathing method (SV IGR) at rest before cardiac resynchronization therapy (CRT) (pre-CRT) and after CRT (post-CRT). *: p<0.0001.
Figure 3: Changes in left ventricular ejection fraction (LVEF), cardiac output (CO), stroke volume (SV), oxygen consumption (VO2) and arteriovenous O2 content difference (ΔC(a-v)O2) after cardiac resynchronization therapy (CRT) at rest and at peak exercise in heart failure (HF) patients grouped into tertiles of pre-CRT peak VO2.
4. Discussion
Our study evaluated a typical population of HF patients who underwent CRT implant. As expected, CRT improved NYHA class and LVEF, and it shortened QRS. The findings unique to the present study are: a) CO and SV at rest were not affected by CRT regardless of the LVEF improvement, b) post-CRT exercise performance improvement was observed only in patients with low pre-CRT peak VO2, c) post-CRT peak CO increase was similar in all patients regardless of pre-CRT exercise performance, suggesting a pivotal role of blood flow distribution during exercise in post-CRT exercise performance change.
We non-invasively measured CO at rest and at peak exercise using IGR method. Since 2005, IGR has been shown to be a reliable technique to measure CO at rest and during exercise in HF patients, having been compared to CO measurement by thermodilution and Fick [17, 20]. Several authors have successfully used IGR in HF to measure CO at rest, during sub-maximal exercise, or at peak exercise [16-21]. Most importantly, IGR allows evaluating exercise with patients sitting on the bike, avoiding positions unnatural for exercise, such as laying on a side or supine as during stress echo or during exercise with invasive measurements. Schlosshan et al. [22] tested 15 HF patients before and after CRT, and they suggested a possible role of CO change as the cause of VO2 improvement. At rest, our data showed that, although LVEF increased due to LV volume reduction, CO and SV remained unchanged, underlining the real meaning of LVEF as an LV reverse remodeling parameter with almost no value as a hemodynamic marker. Differently, at peak exercise, our study confirmed in a large scale the pioneering report of Schlosshan et al., showing that CRT improves peak VO2 through an increase of CO and SV at peak exercise, but only in patients with severe HF.
CRT indication is based on parameters measured at rest-specifically LBBB morphology and low LVEF on top of a NYHA class ≥II – and recognized indicators of successful CRT are clinical changes, LVEF improvement, and QRS shortening [1-6]. However, there is no clear definition of post-CRT functional changes. Indeed, apart from NYHA class evaluation, exercise performance is hardly considered, both in patient selection and in the assessment of CRT efficacy. As regards the response to exercise, improvement following CRT has been shown in HF patients in NYHA class II to IV, and also in a few class I patients, i.e. across virtually all patients with symptomatic HF, without significant differences between NYHA classes [23, 24]. Differently, peak VO2, which is the gold standard of exercise performance evaluation, has been reported to increase after CRT only in patients with severely reduced exercise performance(10), and specifically in subjects with a peak VO2<12 ml/kg/min [9, 11], suggesting inconsistency between NYHA class improvement and peak VO2 changes. Our data confirm these findings, suggesting a low threshold of peak VO2 in CRT responders (peak VO2<11.3 ml/min/kg).
The simultaneous measurement of VO2 and CO during exercise is an advance in the post-CRT evaluation of HF patients. Indeed, knowing both CO and VO2 allows calculating the ΔC(a-v)O2 and, in practice, to discriminate between post-CRT change due to LV pump function improvement and improvement due to peripheral causes such as blood flow distribution, O2 extraction, and muscle function [25]. Our data showed that peak CO increase after CRT is similar in all patients and unaffected by pre-CRT peak VO2, while peak VO2 showed no significant increase after CRT in patients with peak VO2>11.3 ml/min/kg. The difference is by necessity associated with the behavior of ΔC(a-v)O2, which reflects muscle O2 extraction, muscle function, and blood flow distribution during exercise. Notably, very similar data were observed in the post-HF rehabilitation setting [26]. Specifically, knowing the hemodynamic response to CRT during exercise opens a new scenario for patients with improved CO but similar VO2. We believe that post-CRT patients who increase their peak CO but not their peak VO2 are likely a suitable target of an intensive rehabilitation program, which was not performed in the studied patients.
In conclusion, CRT improves exercise performance in HF patients by changing peak exercise CO and SV in all classes of HF patients. However, post CRT peak CO improvement translates into peak VO2 improvement only in patients with severe HF.
References
- Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JGF, Coats AJS, et al. Esc guidelines for the diagnosis and treatment of acute and chronic heart failure: The task force for the diagnosis and treatment of acute and chronic heart failure of the european society of cardiology (esc) developed with the special contribution of the heart failure association (hfa) of the esc. European heart journal 37 (2016): 2129-2200.
- Brignole M, Auricchio A, Baron-Esquivias G, Bordachar P, Boriani G, Breithardt OA, et al. Esc guidelines on cardiac pacing and cardiac resynchronization therapy: The task force on cardiac pacing and resynchronization therapy of the european society of cardiology (esc). Developed in collaboration with the european heart rhythm association (ehra). European heart journal 34 (2013): 2281-2329.
- Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE, Jr., Drazner MH, et al. Accf/aha guideline for the management of heart failure: Executive summary: A report of the american college of cardiology foundation/american heart association task force on practice guidelines. Circulation 128 (2013): 1810-1852.
- Ezekowitz JA, O'Meara E, McDonald MA, Abrams H, Chan M, Ducharme A, et al. Comprehensive update of the canadian cardiovascular society guidelines for the management of heart failure. The Canadian journal of cardiology 33 (2017): 1342-1433.
- Krum H, Jelinek MV, Stewart S, Sindone A, Atherton JJ. Update to national heart foundation of australia and cardiac society of australia and new zealand guidelines for the prevention, detection and management of chronic heart failure in australia, 2006. The Medical journal of Australia 194 (2011): 405-409.
- National institute for health and care excellence. Implantable cardioverter defibrillators and cardiac resynchronisation therapy for arrhythmias and heart failure. Nice guideline (ta314) (2014).
- Boehmer JP. Device therapy for heart failure. The American journal of cardiology 91 (2003): 53D-59D.
- Kalra PR, Sharma R, Shamim W, Doehner W, Wensel R, Bolger AP, et al. Clinical characteristics and survival of patients with chronic heart failure and prolonged qrs duration. International journal of cardiology 86 (2002): 225-231.
- Wasserman K, Sun XG, Hansen JE. Effect of biventricular pacing on the exercise pathophysiology of heart failure. Chest 132 (2007): 250-261.
- Auricchio A, Kloss M, Trautmann SI, Rodner S, Klein H. Exercise performance following cardiac resynchronization therapy in patients with heart failure and ventricular conduction delay. The American journal of cardiology 89 (2002): 198-203.
- Cattadori G, Schmid JP, Agostoni P. Noninvasive measurement of cardiac output during exercise by inert gas rebreathing technique. Heart failure clinics 5 (2009): 209-215.
- Cleland JG, Daubert JC, Erdmann E, Freemantle N, Gras D, Kappenberger L, et al. The effect of cardiac resynchronization on morbidity and mortality in heart failure. The New England journal of medicine 352 (2005): 1539-1549.
- Lang RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, Pellikka PA, et al. Recommendations for chamber quantification. European journal of echocardiography: the journal of the Working Group on Echocardiography of the European Society of Cardiology 7 (2006): 79-108.
- Agostoni P, Bianchi M, Moraschi A, Palermo P, Cattadori G, La Gioia R, et al. Work-rate affects cardiopulmonary exercise test results in heart failure. European journal of heart failure 7 (2005): 498-504.
- Wasserman K, Hansen JE, Sue DY, Stringer WW, Whipp BJ. Clinical exercise testing. Principles of exercise testing and interpretation including pathophysiology and clinical applications. Lippincott Williams and Wilkins (2005): 138-139.
- Kallay MC, Hyde RW, Smith RJ, Rothbard RL, Schreiner BF. Cardiac output by rebreathing in patients with cardiopulmonary diseases. J Appl Physiol 63 (1987): 201-210.
- Agostoni P, Cattadori G. Noninvasive cardiac output measurement: A new tool in heart failure. Cardiology 114 (2009): 244-246.
- Agostoni P, Cattadori G, Apostolo A, Contini M, Palermo P, et al. Noninvasive measurement of cardiac output during exercise by inert gas rebreathing technique: A new tool for heart failure evaluation. Journal of the American College of Cardiology 46 (2005): 1779-1781.
- Goda A, Lang CC, Williams P, Jones M, Farr MJ, et al. Usefulness of non-invasive measurement of cardiac output during sub-maximal exercise to predict outcome in patients with chronic heart failure. The American journal of cardiology 104 (2009): 1556-1560.
- Lang CC, Karlin P, Haythe J, Lim TK, Mancini DM. Peak cardiac power output, measured noninvasively, is a powerful predictor of outcome in chronic heart failure. Circulation. Heart failure 2 (2009): 33-38.
- Shelton RJ, Ingle L, Rigby AS, Witte KK, Cleland JG, Clark AL. Cardiac output does not limit submaximal exercise capacity in patients with chronic heart failure. European journal of heart failure 12 (2010): 983-989.
- Schlosshan D, Barker D, Pepper C, Williams G, Morley C, Tan LB. Crt improves the exercise capacity and functional reserve of the failing heart through enhancing the cardiac flow- and pressure-generating capacity. European journal of heart failure 8 (2006): 515-521.
- Goldenberg I, Kutyifa V, Klein HU, Cannom DS, Brown MW, Dan A, et al. Survival with cardiac-resynchronization therapy in mild heart failure. The New England journal of medicine 370 (2014): 1694-1701.
- Reynolds CR, Gold MR. Cardiac resynchronization therapy for mild heart failure: The time has come. Circulation 123 (2011): 195-202.
- Vignati C, Cattadori G. Measuring cardiac output during cardiopulmonary exercise testing. Annals of the American Thoracic Society 14 (2017): S48-S52.
- Cattadori G, Schmid JP, Brugger N, Gondoni E, Palermo P, Agostoni P. Hemodynamic effects of exercise training in heart failure. Journal of cardiac failure 17 (2011): 916-922.