Paradoxical TBC with Tuberculomas and Tubercular Meningoencephalitis in a Pregnant Woman with (SARS-CoV-2)
Article Information
Juna Musa1, Masum Rahman2, Abu Bakar Siddik3, Samar Ikram2, Ilir Ahmetgjekaj4, Valon Vokshi5, Ali Guy6, Anisa Cobo7, Alireza Shoushtarizadeh2, Blina Abdullahu7, Ibrahim Bajwa8, Essa Mohamed9, Keti Mamillo10, Fjolla Hyseni11
1Department of General Surgery, Mayo Clinic, Rochester, MN, USA
2Department of Neurological Surgery, Mayo Clinic, Rochester, MN, USA
3Department of Pain Medicine, Mayo Clinic, Jacksonville, Florida, USA
4Department of Radiology, UBT and UCC, Pristina, Kosovo
5Department of Anesthesiology, University Clinical Center of Kosovo
6Clinical Assistant Professor, Department of Rehabilitation Medicine, NYU Grossman School of Medicine, New York, USA
7Mother Teresa Hospital, Tirana, Albania
8FU Medical College, Foundation University Islamabad, Punjab, Pakistan
9Department of Cardiovascular Diseases, Mayo Clinic, Rochester, MN, USA
10Department of Anesthesiology, Mother Teresa Hospital, Tirana, Albania
11Medical Researcher, NYU Langone Health, New York, USA
*Corresponding Author: Fjolla Hyseni, Medical Researcher, NYU Langone Health, New York, USA
Received: 23 August 2021; Accepted: 07 September 2021; Published: 18 September 2021
Citation: Juna Musa, Masum Rahman, Abu Bakar Siddik, Samar Ikram, Ilir Ahmetgjekaj, Valon Vokshi, Ali Guy, Anisa Cobo, Alireza Shoushtarizadeh, Blina Abdullahu, Ibrahim Bajwa, Essa Mohamed, Keti Mamillo, Fjolla Hyseni. Paradoxical TBC with Tuberculomas and Tubercular Meningoencephalitis in a Pregnant Woman with (SARS-CoV-2). Archives of Clinical and Medical Case Reports 5 (2021): 640-648.
View / Download Pdf Share at FacebookAbstract
A paradoxical response is a clinical or radiological deterioration of existing or new lesions in tuberculosis patients following treatment. Female gender, HIV infection, length of illness are all known potential risk factors. However, the likelihood of developing a paradoxical response with a concurrent infection of COVID-19 is scarcely reported in the literature, as the circumstance with our patient. In this report, we discuss the case of a 21-year-old woman, at 39 weeks gestation, who presented to the OPD with complaints of headache, coughing, nausea, and abdominal pain. RT-PCR was positive for COVID-19, and radiological imaging was consistent with the diagnosis of Miliary Tuberculosis, further complicated by tuberculous meningitis. Our study aims to highlight the paradox of TB progression in an obstetric patient with prior history of treated TB, coupled with the risk factors associated with a paradoxical reaction.
Keywords
Paradoxical response; Tuberculosis; COVID-19; Meningitis
Paradoxical response article; Tuberculosis article; COVID-19 article; Meningitis article
Paradoxical response articles Paradoxical response Research articles Paradoxical response review articles Paradoxical response PubMed articles Paradoxical response PubMed Central articles Paradoxical response 2023 articles Paradoxical response 2024 articles Paradoxical response Scopus articles Paradoxical response impact factor journals Paradoxical response Scopus journals Paradoxical response PubMed journals Paradoxical response medical journals Paradoxical response free journals Paradoxical response best journals Paradoxical response top journals Paradoxical response free medical journals Paradoxical response famous journals Paradoxical response Google Scholar indexed journals Tuberculosis articles Tuberculosis Research articles Tuberculosis review articles Tuberculosis PubMed articles Tuberculosis PubMed Central articles Tuberculosis 2023 articles Tuberculosis 2024 articles Tuberculosis Scopus articles Tuberculosis impact factor journals Tuberculosis Scopus journals Tuberculosis PubMed journals Tuberculosis medical journals Tuberculosis free journals Tuberculosis best journals Tuberculosis top journals Tuberculosis free medical journals Tuberculosis famous journals Tuberculosis Google Scholar indexed journals COVID-19 articles COVID-19 Research articles COVID-19 review articles COVID-19 PubMed articles COVID-19 PubMed Central articles COVID-19 2023 articles COVID-19 2024 articles COVID-19 Scopus articles COVID-19 impact factor journals COVID-19 Scopus journals COVID-19 PubMed journals COVID-19 medical journals COVID-19 free journals COVID-19 best journals COVID-19 top journals COVID-19 free medical journals COVID-19 famous journals COVID-19 Google Scholar indexed journals Meningitis articles Meningitis Research articles Meningitis review articles Meningitis PubMed articles Meningitis PubMed Central articles Meningitis 2023 articles Meningitis 2024 articles Meningitis Scopus articles Meningitis impact factor journals Meningitis Scopus journals Meningitis PubMed journals Meningitis medical journals Meningitis free journals Meningitis best journals Meningitis top journals Meningitis free medical journals Meningitis famous journals Meningitis Google Scholar indexed journals Meningoencephalitis articles Meningoencephalitis Research articles Meningoencephalitis review articles Meningoencephalitis PubMed articles Meningoencephalitis PubMed Central articles Meningoencephalitis 2023 articles Meningoencephalitis 2024 articles Meningoencephalitis Scopus articles Meningoencephalitis impact factor journals Meningoencephalitis Scopus journals Meningoencephalitis PubMed journals Meningoencephalitis medical journals Meningoencephalitis free journals Meningoencephalitis best journals Meningoencephalitis top journals Meningoencephalitis free medical journals Meningoencephalitis famous journals Meningoencephalitis Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals CT articles CT Research articles CT review articles CT PubMed articles CT PubMed Central articles CT 2023 articles CT 2024 articles CT Scopus articles CT impact factor journals CT Scopus journals CT PubMed journals CT medical journals CT free journals CT best journals CT top journals CT free medical journals CT famous journals CT Google Scholar indexed journals Genotype articles Genotype Research articles Genotype review articles Genotype PubMed articles Genotype PubMed Central articles Genotype 2023 articles Genotype 2024 articles Genotype Scopus articles Genotype impact factor journals Genotype Scopus journals Genotype PubMed journals Genotype medical journals Genotype free journals Genotype best journals Genotype top journals Genotype free medical journals Genotype famous journals Genotype Google Scholar indexed journals Tuberculomas articles Tuberculomas Research articles Tuberculomas review articles Tuberculomas PubMed articles Tuberculomas PubMed Central articles Tuberculomas 2023 articles Tuberculomas 2024 articles Tuberculomas Scopus articles Tuberculomas impact factor journals Tuberculomas Scopus journals Tuberculomas PubMed journals Tuberculomas medical journals Tuberculomas free journals Tuberculomas best journals Tuberculomas top journals Tuberculomas free medical journals Tuberculomas famous journals Tuberculomas Google Scholar indexed journals Diabetes articles Diabetes Research articles Diabetes review articles Diabetes PubMed articles Diabetes PubMed Central articles Diabetes 2023 articles Diabetes 2024 articles Diabetes Scopus articles Diabetes impact factor journals Diabetes Scopus journals Diabetes PubMed journals Diabetes medical journals Diabetes free journals Diabetes best journals Diabetes top journals Diabetes free medical journals Diabetes famous journals Diabetes Google Scholar indexed journals
Article Details
1. Introduction
A paradoxical response is a clinical or radiological deterioration of existing or new lesions of tuberculosis (TB) patients following treatment. These phenomena are particularly prevalent in TB-affected lungs, central nervous system (CNS), and lymph nodes [1]. Choremis and his colleagues first identified a paradoxical response to imaging findings of a child treated for TB in 1955 [2]. Paradoxical reaction in a patient with CNS TB was first described by Thrush and Barwick in 1974 [3].
In patients with tuberculous meningitis, it is described as exacerbating pre-existing tuberculous lesions or the emergence of new tuberculous lesions despite initial improvement with anti-tuberculosis treatment. In about one-third of tuberculous meningitis patients, a paradoxical reaction occurs. Female sex, HIV infection, and length of illness are all important predictors. In patients with tuberculous meningitis, the duration of disease, alterations in consciousness, stage-III tuberculous meningitis, and presence of hydrocephalus all anticipate a poor outcome; paradoxical responses, in contrast, do not seem to have an adverse effect on the outcome [4]. However, it complicates the treatment of CNS tuberculosis and raises the possibility of emerging drug resistance.
The clinical or radiological worsening associated with such a reaction may lead to erroneous conclusions about drug resistance or treatment failure, prompting a search for a different diagnosis. Case reports and limited case series have mainly been used to explain paradoxical reaction manifestations, including clinical manifestations, imaging, and CSF findings. Lymphocytic pleocytosis, polymorphonuclear predominance, or a rise in protein levels are all possible changes in CSF. Corticosteroids have been shown to be effective; hence the paradoxical reaction does not necessarily indicate treatment failure [5-7].
2. Case Report
A 21-year-old woman, G1P0, at 39 weeks gestation, has presented with cough, headache, nausea, abdominal pain. She has been previously treated for tuberculosis 2 years ago. The patient was afebrile and had an arterial blood pressure of 135/80 mmHg, a heart rate of 111beats/min, respiratory rate of 32 breaths/min, and oxygen saturation SpO2=96% on room air. D-dimer was 1.3 μg/mL, other routine laboratory examinations were within normal limits.
Her neurological examination, including cranial nerves, motor, sensory and cerebellar examination, were within normal ranges. Chest auscultation revealed bilateral crepitation with bronchial breathing on the right side. Oropharyngeal throat swab sample yielded a positive result for COVID-19, detected by real-time reverse-transcriptase–polymerase-chain-reaction (RT-PCR) assay. Chest x-ray revealed cavitation at the upper lobe of the right lung with small nodules bilaterally in a random distribution with a suspect of military tuberculosis. Brain MRI was ordered which demostated FLAIR sequence hyperintensity in thalamus, T1 weighted image hypointense lesion without contrast enhancment while presenting water diffusion restriction in DWI/ADC hereby findings indicated late subacute ischemia. Axial T1 weighted images demostrated multiple small sub centimeter size nodular and ring enhancing lesions that were corresponding to tuberculomas in cerebellum. Also T1 weighted image demonstared contrast enhancment in the quadrigeminal cistern and the ambient cisten that correspond to tuberculomas. No presence of other supratentorial lesions were observed other than ischemia at this time.
The treatment was modified on lines of COVID-19 that included injectable azithromycin 500 mg once daily, injectable methylprednisolone 40mg twice daily, tablet hydroxychloroquine 400 mg twice daily, tablet vitamin C 500 mg twice daily, and tablet N-acetyl cysteine 600 mg twice daily. Anti-tuberculous regimen (Rifampicin-R, Isoniazid-Z, Ethambutol-E and Pyrazinamide-Z) was also started for TB component a 4-drug anti-tubercular therapy (rifampicin [R]=10 mg/kg/d, isoniazid [H]=8 mg/kg/d, ethambutol [E]=25 mg/kg/d, pyrazinamide [Z]=25 mg/kg/d), plus and intravenous steroids (dexamethasone 4 mg every 8 hours) was started. Acetylsalicylic acid and enoxaparin were added to the ongoing treatment.
Given the progression of disease, at 39w6d (hospital day 6), the fetal heart rate monitoring found acute fetal distress, and as result an urgent cesarean section was performed. Male baby was born with an Apgar scores of 3 and 5 after 1 and 5min, respectively, and birth weight was 1250g. Newborn presented with respiratory effort, which manifested by apnea (deep, intermittent, slow, spasmodic inspiratory efforts) and the successful resuscitation was established. However, despite resuscitative measures, the baby died of respiratory failure on Day-2 of hospitalization.
The patient’s status deteriorates post-partum (hospital day 8) which presented with somnolence, seizure, a temperature of 38.3, T/A 135/80, PP 111mmHg, SpO2=90%, with positive meningeal signs. The patient suffered 2 post-partum seizures over a period of 2 hours. Seizures were characterized by generalized muscle spasm, that terminated spontaneously, on examination immediately after the seizure she appeared post-ictal without focal neurological deficits. Treatment with intravenous magnesium sulphate infusion was added to prevent further convulsions. Lumbar puncture was performed, and the diagnosis of tubercular meningitis was suspected.
Second brain MRI was orderd after 7 weeks of treatment therapy which demostrated exarcibation of the tuberclulomas where FLAIR axial image and T1 weighted image post constrat presented the increased number and size of tuberculomas in cerebellum. It was also evident in T1 weighted images post contrast enhamcent that this time were more massive with increased inflamation in the quadrimenal cistern and the ambient cistern, many confluent and distinct lesions around suprasellar cistern left tentorium were demonstared. New sub centimer sized lesions were also present in supratentorium. Based on these findings we diagnosed these lesions as an onset of post treatment paradoxical reactions.
Accordingly, we prescribed the administration of corticosteroids (prednisolone, 30 mg/day, 0.6 mg/kg/day) which will be gradually tappering off. After 3 months of the corticosteroid treatment, the tuberculomas reduced and we tappered the dosage of prednisolone to 5 mg/day. The patient is in ongoing treatment.
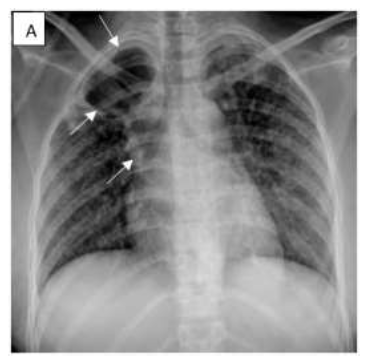
Figure 1: PA chest radiograph shows a right cavitary lesion (white arrows) accompanied by drainage on the corresponding side (white arrowhead). Small nodules are present bilaterally in a random distribution with a suspect of military tuberculosis.
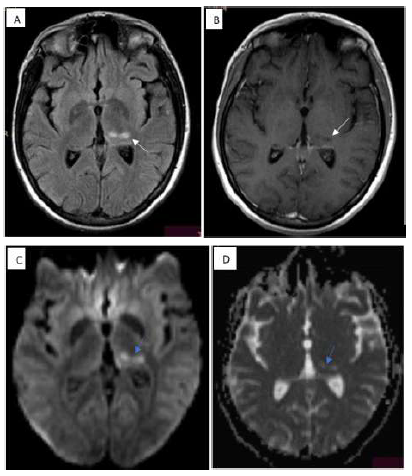
Figure 2: FLAIR sequence (A) demostrates hyperintensity in thalamus (white arrow), T1 weighted image shows hypointense lesion without contrast enhancment (B)( white arrohead), while presenting water diffusion restriction in DWI/ADC (C ,D)(blue arrows) hereby findings indicate late subacute ischemia.
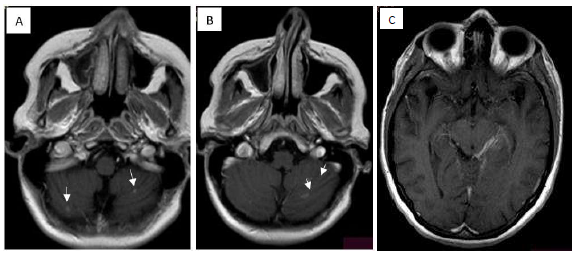
Figure 3: Axial T1 weighted images (A and B) presents multiple small sub centimeter size nodular and ring enhancing lesions with tuberculomas in cerebellum (White arrows).T1 weighted image (C) ( white arrowhead) demonstares contrast enhancment in the quadrigeminal cistern and the ambient cisten that correspond to tuberculomas. No presence other supratentorial lesions were observed other than ischemia.
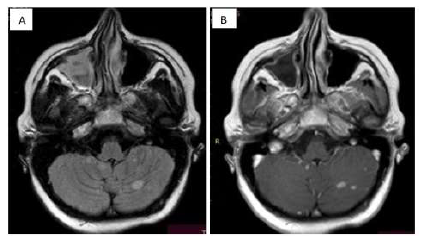
Figure 4: FLAIR axial image (A) and T1 weighted image post constrat (B) presenting the increased number and size of tuberculomas in cerebellum.
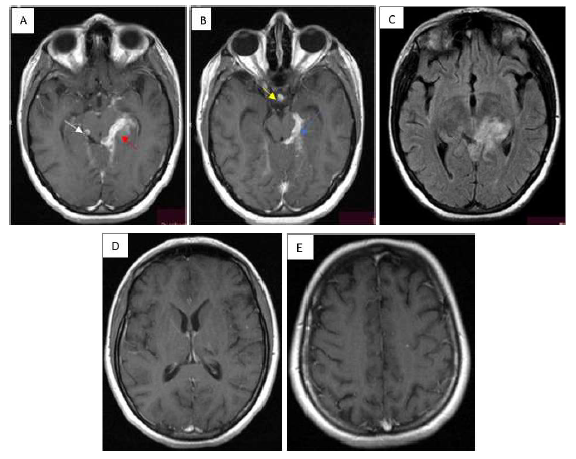
Figure 5: T1 weighted images presenting post contrast enhamcent that is much more massive inflamatory mass in the quadrimenal cistern and the ambient cister (A) ( red arrow), also many confluent and distinct lesions around suprasellar cistern (B) (yellow arrow), left tentorium (C)(blue arrow).New sub centimer sized lesions present in supratentorium(D,E)(black arrow).
3. Discussion
The present study is probably the first case report of paradoxical tuberculosis tuberculoma with meningoencephalitis and concurrent SARS-CoV2 in a pregnant woman. The paradoxical response occurs as a delayed hypersensitivity reaction due to the release of mycobacterial proteins into the subarachnoid space and the tuberculoma. This leads to an inflammatory cascade which further contributes to the expansion of the tuberculoma, edema, vasculitis, and infarction. A highly suggestive sign of meningoencephalitis is the increase in lymphocytic pleocytosis or polymorphonuclear cells which paradoxically occurs due to the administered therapeutics. This may occur due to the subarachnoid tubercles (Rich’s foci) in the meninges that expand readily and break down into the subarachnoid space. As with our case report above, the paradoxical response occurs many weeks after the treatment initiation and is often accompanied by clinical deterioration of patients. In the literature, paradoxical response has been reported to occur anywhere from 2 weeks to 18 months post initiation of anti-tuberculosis treatment.
The medical community has not reached an agreement on the appropriate management strategy for paradoxical tuberculomas. While some patients, like the one discussed in this report, respond to anti-tuberculosis therapies alongside systemic steroids, others may require second-line agents (due to resistance), or even neurosurgery. The justification for using steroids is to dampen the pro-inflammatory effects that follow the release of M. Tuberculosis bacilli. The improvements seen with the use of corticosteroids may be due to the reduction in cerebral edema and/or vasculitis. It is important to note that a paradoxical response does not warrant a change in the drug regimen or rather the assumption that the organism has developed drug resistance. If in resource poor setting where drug susceptibility testing is not a possibility, considering the addition of second-line agents (i.e levofloxacin and ethionamide) on top of the current regimen can be considered.
Surgical interventions are not used often, but when they are utilized, it is either for the treatment of acute complication (eg. Hydrocephalus), or confirmatory diagnosis of non-responsive lesions. The former may be treated with shunting procedures, and the latter via a stereotactic biopsy of the suspected tuberculoma. However, invasive diagnostic testing is not undertaken unless patient has not had any response to therapy for 8 weeks or longer. Some tuberculomas may cause mass effect and severe symptoms, in which case a neurosurgical decompression may be considered for relief of symptoms.
Physician must monitor and recognize early signs of paradoxical response. Early intervention with the appropriate therapeutics and neuroimaging may be life-saving and prevent further neurological damage. The same treatment regimen should continue when paradoxical response is recognized, and this should not be labeled as a new or resistant infection. Systemic corticosteroids may be added, or if already part of the treatment regimen, its dose may be increased to acquire the desired response. Lastly, if medical interventions fail to generate clinical improvements, neurosurgical interventions may be considered.
4. Conclusion
About one-third of tuberculous meningitis patients experience clinical or radiological worsening of pre-existing lesions, or the emergence of new lesions following treatment is known as the paradoxical reaction. Female gender, concurrent HIV infection, and a shorter illness span were all major predictors. The existence of COVID-19 can be a risk factor for this reaction. Paradoxical responses may not have a negative impact on treatment strategy and outcome.
References
- Silman JB, Peters JI, Levine SM, et al. Development of intracranial tuberculomas while receiving therapy for pulmonary fibrosis. American Journal of Respiratory and Critical Care Medicine 150 (1994): 1439-1440.
- Choremis CB, Padiatellis C, Zoumboulakis D, et al. Transitory exacerbation of fever and roentgenographic findings during treatment of tuberculosis in children. Am Rev Tuberc721955527536
- Thrush DC, Barwick DD. Three patients with intracranial tuberculomas with unusual features Journal of Neurology, Neurosurgery and Psychiatry 37 (1974): 566-569.
- Singh AK, Malhotra HS, Garg RK, et al. Paradoxical reaction in tuberculous meningitis: presentation, predictors and impact on prognosis. BMC Infect Dis 16 (2016): 306.
- Garcia-Monco JC, Ferreira E, Gomez-Beldarrain M. The therapeutic paradox in the diagnosis of tuberculous meningitis. Neurology 65 (2005):1991-1992.
- Teoh R, O'Mahony G, Yeung VT. Polymorphonuclear pleocytosis in the cerebrospinal fluid during chemotherapy for tuberculous meningitis. J Neurol 233 (1986): 237-241.
- Kim SH, Kim YS. Immunologic paradox in the diagnosis of tuberculous meningitis. Clin Vaccine Immunol 16 (2009):1847-1849.
