Oral Hematomas following Oral Sex in Individuals with Disrupted Coagulation
Article Information
G Tobias1,2*, T Chackartchi2,3, L Abramov4, J Mann1,2, M Findler2,5
1Department of Community Dentistry, Hadassah Medical Center, Faculty of Dental Medicine, Hebrew University of Jerusalem, Israel
2Dental Research Unit – Maccabi-Dent, Maccabi Healthcare Fund, Israel
3Department of Periodontology, Hadassah Medical Center, Faculty of Dental Medicine, Hebrew University of Jerusalem, Israel
4Former Head of The Sex Therapy Clinic, Lis Maternity Hospital, Tel Aviv Sourasky Medical Center, Sackler Faculty of Medicine, Tel-Aviv University. Tel Aviv, Israel
5Former Senior lecturer, Head of the Medically Complex Patient Clinic, Department of Oral Medicine, the Hebrew University-Hadassah School of Dental Medicine, Jerusalem, Israel
*Corresponding Author: Guy Tobias, Department of Community Dentistry, Hadassah Medical, Center, Faculty of Dental Medicine, Hebrew University of Jerusalem, Israel.
Received: 14 May 2022; Accepted: 09 June 2022; Published: 29 June 2022
Citation: G Tobias, T Chackartchi, L Abramov, J Mann, M Findler. Oral Hematomas following Oral Sex in Individuals with Disrupted Coagulation. Archives of Clinical and Medical Case Reports 6 (2022): 486-490.
View / Download Pdf Share at FacebookAbstract
Protected oral sex is relatively safe and harmless. There are hardly any reports in the literature regarding palatal bruises and hematomas following oral sexual activity in those with a bleeding tendency. Here we report oral sub-mucosal hemorrhage in three women with a disrupted coagulation system. The traumatic hemorrhage was attributed to violent activity during oral sexual practices. This short report presents a seemingly unnoticed and unreported phenomenon following oral sexual behavior.
Keywords
<p>Sub-mucosal hemorrhage; Oral sexual activity; Bleeding tendency; Fellatio</p>
Sub-mucosal hemorrhage articles; Oral sexual activity articles; Bleeding tendency articles; Fellatio articles
Sub-mucosal hemorrhage articles Sub-mucosal hemorrhage Research articles Sub-mucosal hemorrhage review articles Sub-mucosal hemorrhage PubMed articles Sub-mucosal hemorrhage PubMed Central articles Sub-mucosal hemorrhage 2023 articles Sub-mucosal hemorrhage 2024 articles Sub-mucosal hemorrhage Scopus articles Sub-mucosal hemorrhage impact factor journals Sub-mucosal hemorrhage Scopus journals Sub-mucosal hemorrhage PubMed journals Sub-mucosal hemorrhage medical journals Sub-mucosal hemorrhage free journals Sub-mucosal hemorrhage best journals Sub-mucosal hemorrhage top journals Sub-mucosal hemorrhage free medical journals Sub-mucosal hemorrhage famous journals Sub-mucosal hemorrhage Google Scholar indexed journals COVID-19 articles COVID-19 Research articles COVID-19 review articles COVID-19 PubMed articles COVID-19 PubMed Central articles COVID-19 2023 articles COVID-19 2024 articles COVID-19 Scopus articles COVID-19 impact factor journals COVID-19 Scopus journals COVID-19 PubMed journals COVID-19 medical journals COVID-19 free journals COVID-19 best journals COVID-19 top journals COVID-19 free medical journals COVID-19 famous journals COVID-19 Google Scholar indexed journals Bleeding tendency articles Bleeding tendency Research articles Bleeding tendency review articles Bleeding tendency PubMed articles Bleeding tendency PubMed Central articles Bleeding tendency 2023 articles Bleeding tendency 2024 articles Bleeding tendency Scopus articles Bleeding tendency impact factor journals Bleeding tendency Scopus journals Bleeding tendency PubMed journals Bleeding tendency medical journals Bleeding tendency free journals Bleeding tendency best journals Bleeding tendency top journals Bleeding tendency free medical journals Bleeding tendency famous journals Bleeding tendency Google Scholar indexed journals Coronary articles Coronary Research articles Coronary review articles Coronary PubMed articles Coronary PubMed Central articles Coronary 2023 articles Coronary 2024 articles Coronary Scopus articles Coronary impact factor journals Coronary Scopus journals Coronary PubMed journals Coronary medical journals Coronary free journals Coronary best journals Coronary top journals Coronary free medical journals Coronary famous journals Coronary Google Scholar indexed journals Fellatio articles Fellatio Research articles Fellatio review articles Fellatio PubMed articles Fellatio PubMed Central articles Fellatio 2023 articles Fellatio 2024 articles Fellatio Scopus articles Fellatio impact factor journals Fellatio Scopus journals Fellatio PubMed journals Fellatio medical journals Fellatio free journals Fellatio best journals Fellatio top journals Fellatio free medical journals Fellatio famous journals Fellatio Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals CT articles CT Research articles CT review articles CT PubMed articles CT PubMed Central articles CT 2023 articles CT 2024 articles CT Scopus articles CT impact factor journals CT Scopus journals CT PubMed journals CT medical journals CT free journals CT best journals CT top journals CT free medical journals CT famous journals CT Google Scholar indexed journals atherosclerosis articles atherosclerosis Research articles atherosclerosis review articles atherosclerosis PubMed articles atherosclerosis PubMed Central articles atherosclerosis 2023 articles atherosclerosis 2024 articles atherosclerosis Scopus articles atherosclerosis impact factor journals atherosclerosis Scopus journals atherosclerosis PubMed journals atherosclerosis medical journals atherosclerosis free journals atherosclerosis best journals atherosclerosis top journals atherosclerosis free medical journals atherosclerosis famous journals atherosclerosis Google Scholar indexed journals Skin grafts articles Skin grafts Research articles Skin grafts review articles Skin grafts PubMed articles Skin grafts PubMed Central articles Skin grafts 2023 articles Skin grafts 2024 articles Skin grafts Scopus articles Skin grafts impact factor journals Skin grafts Scopus journals Skin grafts PubMed journals Skin grafts medical journals Skin grafts free journals Skin grafts best journals Skin grafts top journals Skin grafts free medical journals Skin grafts famous journals Skin grafts Google Scholar indexed journals SARS-CoV2 articles SARS-CoV2 Research articles SARS-CoV2 review articles SARS-CoV2 PubMed articles SARS-CoV2 PubMed Central articles SARS-CoV2 2023 articles SARS-CoV2 2024 articles SARS-CoV2 Scopus articles SARS-CoV2 impact factor journals SARS-CoV2 Scopus journals SARS-CoV2 PubMed journals SARS-CoV2 medical journals SARS-CoV2 free journals SARS-CoV2 best journals SARS-CoV2 top journals SARS-CoV2 free medical journals SARS-CoV2 famous journals SARS-CoV2 Google Scholar indexed journals
Article Details
1. Introduction
Protected oral sexual practice is considered relatively safe [1]. Tears, lacerations, and bruises have been reported following aggressive (consensual or non-consensual) oral sexual behavior [2]. Intra-oral traumatic injury can be caused by an overenthusiastic thrust or by strong sucking, and will eventually cause sub mucosal hemorrhage [3, 4]. In healthy individuals this interaction causes a minute extravasation of blood, and petechial lesions on the hard and/or soft palate and may be the sole clinical presentation, termed “intra oral lesion of fellatio” [5]. Petechiae are defined as a cluster of small red to purple points less than 3mm, purpura are similar lesions up to. 10mm, whereas an ecchymosis is larger than 1cm in diameter [6]. Ecchymosis and extended sub mucosal bleeding are rarely seen in routine clinical practice. In this report we present intra oral sub mucosal hemorrhage following traumatic oral sexual activity. The patients described here have disrupted coagulation systems due to Immune Thrombocytopenic Purpura (ITP), anti-thrombotic medication and anticoagulant therapy.
2. Case Reports
2.1. Case 1
A 55-year-old Caucasian woman was referred to the Oral Medicine clinic due to a disturbing purple mass on the palate that appeared 24 hours before presentation (Figure 1). The patient is known to suffer from ITP with a platelet count of 20,000-40,000 per microliter. No history of trauma other than oral sexual activity was mentioned. No treatment was advised, and the patient recovered within a week.
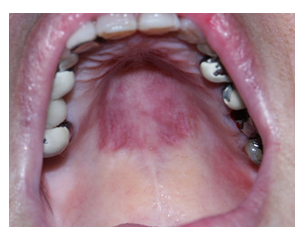
Figure 1: Extended hematoma in patient no.1 with ITP.
2.2. Case 2
A 50-year-old Caucasian woman presented at the oral medicine clinic with a chief complaint of an itching sensation beneath her maxillary partial denture (Figure 2). The patient was medicated with sodium warfarin following an aortic valve replacement 15 years earlier. Examination revealed a palatal abrasion with extensive ecchymosis extending beyond the borders of the denture. She performed a blood coagulation test, and her International normalized Ratio – INR was 3.1. The patient confirmed oral sex the evening before. With no treatment the lesion subsided within a week.
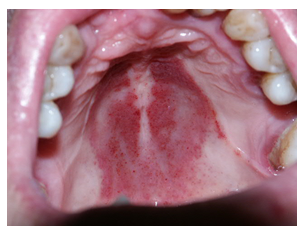
Figure 2: Hematoma in Patient No.2, using an anticoagulant. The white lines on either side of the red hematoma lesion deliniate the border of the denture.
2.3. Case 3
A 57-year-old Caucasian female presented at the oral medicine clinic with an unusual feeling on the palate for the last 24 hours (Figure 3). The patient has a long history of ischemic heart disease and underwent percutaneous coronary intervention following which she was given double anti platelet aggregate therapy: aspirin 100 mg and clopidogrel 75 mg per day. Oral intercourse was only confirmed on her second visit. An antiseptic oral rinse was prescribed, and all symptoms subsided within one week.
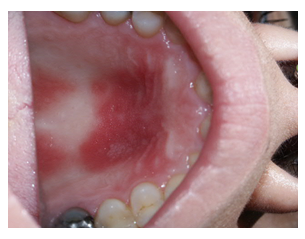
Figure 3: Palatal hematoma in patient No.3.
3. Discussion
Oral Soft tissue extravascular collections of blood may appear as red – purple to blue lesions on the tongue, cheek, base of oral cavity and palate. These lesions can be caused by infectious diseases and trauma or as a consequence of disrupted coagulation including blood disease, platelet dysfunction, anti-thrombotic treatment, vascular fragility, increased capillary pressure (caused by vomiting or choking) [5]. Current evidence based clinical guidelines for prescribing anti-thrombotic therapy recommend this medication for: primary and secondary prevention of ischemic heart disease, following percutaneous coronary intervention, chronic atrial fibrillation, thrombophilia's and other diseases [6]. All users of antithrombotic treatments should be informed of the possibility of traumatic blood extravasation from oral sexual activity. Even though palatal sub mucosal bleeding is harmless, it needs to be differentiated from other conditions that may present as sub mucosal accumulations of blood. Doughnut lesions, an erythematous papule with a pale center, located on the soft or hard palates is a presenting sign of Group A Streptococcal (GAS) pharyngitis [7, 8]. Their raised appearance allows differentiation from the flat oral lesion of fellatio [9]. Other infectious causes of palatal petechiae include rubella virus (Cheimer sign), cytomegalovirus, herpes simplex virus, human herpes virus 6 (roseola), Epstein-Barr virus, HIV, Treponema pallidum, and Toxoplasma [10]. A thorough review of these clinical conditions is beyond the scope of this article.
4. Conclusions
Protected oral sex is safe. Nevertheless, considering the increasing number of individuals prescribed anti-thrombotic medications, clinicians should be aware of the possibility of oral sub mucosal hematomas following fellatio. Patients should also be informed about this seemingly completely reversible phenomenon.
Disclosure and Conflict of Interests
None of the authors have any disclosures to make with no conflict of interest
References
- Halpern-Felsher BL, Cornell JL, Kropp RY, et Oral versus vaginal sex among adolescents: perceptions, attitudes, and behavior. Pediatrics 115 (2005): 845-851.
- Neville BW, Damm DD, AllenCM, et al. Oral and maxillofacial pathology. 2009, 3rd Saundr Elsevier Pennsylvania 780.
- Cohen PR, Miller VM. Fellatio-associated petechiae of the palate: report of purpuric palatal lesions developing after oral sex. Dermatol Online J 19 (2013): 18963.
- Mendez LA, Martinez R, Rubio M. Fellatio-associated erythema of the soft palate: an incidental finding during a routine dental evaluation. BMJ Case Rep 11 (2018): 2017-221901.
- Neville BW, Damm DD, Allen CM, et al. Oral and maxillofacial pathology. 2009, 3rd Saundr Elsevier Pennsylvania 307-308.
- Mitchell RS, Kumar V, Robbins SL, et al. Robbins basic pathology 8th ed). Saunders/Elsevier Pennsylvania (2007): 10-11.
- Darmstadt GL, Purpura In, Long SS, et al. Principles and practice of pediatric infectious diseases. 2001, 2nd ed. Philadelphia: Churchill Livingston (2001): 437.
- Guyatt GH, Akel EA, Crowther M, et al. Introduction to the 9th edition: Antithrombotic therapy and prevention of thrombosis, 9th ed. American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest 141(2012): 48S-52S.
- Amren DP. Unusual forms of streptococcal disease. In: Wannamaker LW, Matsen JM, eds. Streptococci and streptococcal diseases: recognition, understanding and management.1972, New York: Academic Press (1972): 552-554.
- Wannamaker LW. Diagnosis of pharyngitis: clinical and epidemiologic features. In: Shulman ST, ed. Pharyngitis. Management in an era of declining rheumatic fever (1984). New York: Praeger Scientific (1984): 35-36.
- Schwartz RH, Gerber MA. Pharyngeal findings of group A streptococcal pharyngitis. Arch Pediatr Adolesc Med 152 (1998T): 927-928.
- Darmstadt GL, Purpura In, Long SS, et al. Principles and practice of pediatric infectious diseases. 2001, 2nd ed. Philadelphia: Churchill Livingstone 437.
