Oblique Compression Screw Fixation across the Physis for Tillaux Fractures in Adolescent
Article Information
Nicholas I Pilla*, Mikayla Borusiewicz, Emily Smith, William L Hennrikus
Penn State Hershey Medical Center, Pennsylvania, United States
*Corresponding Author: Dr. Nicholas I. Pilla, Penn State Hershey Bone and Joint Institute 30 Hope Drive, Hershey, PA 17033, United States
Received: 01 August 2020; Accepted: 10 August 2020; Published: 24 August 2020
Citation: Nicholas I Pilla, Mikayla Borusiewicz, Emily Smith, William L Hennrikus. Oblique Compression Screw Fixation across the Physis for Tillaux Fractures in Adolescent. Journal of Orthopaedics and Sports Medicine 2 (2020): 150-156.
View / Download Pdf Share at FacebookAbstract
Objective: Tillaux fractures are uncommon physeal injuries sustained by adolescents. Two different fixation techniques are described; the first involves placement of a screw obliquely into the tibial metaphysis, while the second involves placement of a screw parallel through the epiphysis without violating the physis. The purpose of this study was to report the outcomes, complications, and advantages of oblique screw fixation.
Methods: This study was approved by the College of Medicine institutional review board. Ten patients with displaced Tillaux fractures were reviewed. All patients underwent attempted closed reduction first. Open reduction and internal fixation was performed using a 4 mm solid partially threaded screw that crossed the physis. A short-leg non-weight bearing cast was placed for 3 weeks followed by a CAM boot.
Results: Outcomes measured included subjective pain and range of motion. No patient had pain, arthritis, stiffness, or limitations at final follow up. All returned to pre-injury sports as tolerated. Six patients had hardware removed. All patients had equal range of motion and no pain following oblique screw fixation.
Conclusion: Tillaux fractures are uncommon ankle injuries occurring in adolescents. Open reduction is recommended if there is more than 2 mm of fracture displacement. All patients in the current study reported equal outcomes of pain and range of motion. Use of an oblique screw resulted in excellent outcomes with no complications of growth arrest, arthritis, stiffness, or infection. This study demonstrates the advantages of the oblique screw placement including a technically simple, fast, and safe procedure.
Keywords
Tillaux; Tillaux fractures; Orthopaedics; Pediatric orthopaedics; Trauma; Lower extremity trauma
Tillaux fractures articles Tillaux fractures Research articles Tillaux fractures review articles Tillaux fractures PubMed articles Tillaux fractures PubMed Central articles Tillaux fractures 2023 articles Tillaux fractures 2024 articles Tillaux fractures Scopus articles Tillaux fractures impact factor journals Tillaux fractures Scopus journals Tillaux fractures PubMed journals Tillaux fractures medical journals Tillaux fractures free journals Tillaux fractures best journals Tillaux fractures top journals Tillaux fractures free medical journals Tillaux fractures famous journals Tillaux fractures Google Scholar indexed journals Distal tibial physis articles Distal tibial physis Research articles Distal tibial physis review articles Distal tibial physis PubMed articles Distal tibial physis PubMed Central articles Distal tibial physis 2023 articles Distal tibial physis 2024 articles Distal tibial physis Scopus articles Distal tibial physis impact factor journals Distal tibial physis Scopus journals Distal tibial physis PubMed journals Distal tibial physis medical journals Distal tibial physis free journals Distal tibial physis best journals Distal tibial physis top journals Distal tibial physis free medical journals Distal tibial physis famous journals Distal tibial physis Google Scholar indexed journals Anterior-inferior tibio-fibular ligament articles Anterior-inferior tibio-fibular ligament Research articles Anterior-inferior tibio-fibular ligament review articles Anterior-inferior tibio-fibular ligament PubMed articles Anterior-inferior tibio-fibular ligament PubMed Central articles Anterior-inferior tibio-fibular ligament 2023 articles Anterior-inferior tibio-fibular ligament 2024 articles Anterior-inferior tibio-fibular ligament Scopus articles Anterior-inferior tibio-fibular ligament impact factor journals Anterior-inferior tibio-fibular ligament Scopus journals Anterior-inferior tibio-fibular ligament PubMed journals Anterior-inferior tibio-fibular ligament medical journals Anterior-inferior tibio-fibular ligament free journals Anterior-inferior tibio-fibular ligament best journals Anterior-inferior tibio-fibular ligament top journals Anterior-inferior tibio-fibular ligament free medical journals Anterior-inferior tibio-fibular ligament famous journals Anterior-inferior tibio-fibular ligament Google Scholar indexed journals Salter-Harris fracture articles Salter-Harris fracture Research articles Salter-Harris fracture review articles Salter-Harris fracture PubMed articles Salter-Harris fracture PubMed Central articles Salter-Harris fracture 2023 articles Salter-Harris fracture 2024 articles Salter-Harris fracture Scopus articles Salter-Harris fracture impact factor journals Salter-Harris fracture Scopus journals Salter-Harris fracture PubMed journals Salter-Harris fracture medical journals Salter-Harris fracture free journals Salter-Harris fracture best journals Salter-Harris fracture top journals Salter-Harris fracture free medical journals Salter-Harris fracture famous journals Salter-Harris fracture Google Scholar indexed journals Arthritis articles Arthritis Research articles Arthritis review articles Arthritis PubMed articles Arthritis PubMed Central articles Arthritis 2023 articles Arthritis 2024 articles Arthritis Scopus articles Arthritis impact factor journals Arthritis Scopus journals Arthritis PubMed journals Arthritis medical journals Arthritis free journals Arthritis best journals Arthritis top journals Arthritis free medical journals Arthritis famous journals Arthritis Google Scholar indexed journals Oblique screw articles Oblique screw Research articles Oblique screw review articles Oblique screw PubMed articles Oblique screw PubMed Central articles Oblique screw 2023 articles Oblique screw 2024 articles Oblique screw Scopus articles Oblique screw impact factor journals Oblique screw Scopus journals Oblique screw PubMed journals Oblique screw medical journals Oblique screw free journals Oblique screw best journals Oblique screw top journals Oblique screw free medical journals Oblique screw famous journals Oblique screw Google Scholar indexed journals Arthrotomy articles Arthrotomy Research articles Arthrotomy review articles Arthrotomy PubMed articles Arthrotomy PubMed Central articles Arthrotomy 2023 articles Arthrotomy 2024 articles Arthrotomy Scopus articles Arthrotomy impact factor journals Arthrotomy Scopus journals Arthrotomy PubMed journals Arthrotomy medical journals Arthrotomy free journals Arthrotomy best journals Arthrotomy top journals Arthrotomy free medical journals Arthrotomy famous journals Arthrotomy Google Scholar indexed journals Nerve injuries articles Nerve injuries Research articles Nerve injuries review articles Nerve injuries PubMed articles Nerve injuries PubMed Central articles Nerve injuries 2023 articles Nerve injuries 2024 articles Nerve injuries Scopus articles Nerve injuries impact factor journals Nerve injuries Scopus journals Nerve injuries PubMed journals Nerve injuries medical journals Nerve injuries free journals Nerve injuries best journals Nerve injuries top journals Nerve injuries free medical journals Nerve injuries famous journals Nerve injuries Google Scholar indexed journals Joint stiffness articles Joint stiffness Research articles Joint stiffness review articles Joint stiffness PubMed articles Joint stiffness PubMed Central articles Joint stiffness 2023 articles Joint stiffness 2024 articles Joint stiffness Scopus articles Joint stiffness impact factor journals Joint stiffness Scopus journals Joint stiffness PubMed journals Joint stiffness medical journals Joint stiffness free journals Joint stiffness best journals Joint stiffness top journals Joint stiffness free medical journals Joint stiffness famous journals Joint stiffness Google Scholar indexed journals Skeletal maturity articles Skeletal maturity Research articles Skeletal maturity review articles Skeletal maturity PubMed articles Skeletal maturity PubMed Central articles Skeletal maturity 2023 articles Skeletal maturity 2024 articles Skeletal maturity Scopus articles Skeletal maturity impact factor journals Skeletal maturity Scopus journals Skeletal maturity PubMed journals Skeletal maturity medical journals Skeletal maturity free journals Skeletal maturity best journals Skeletal maturity top journals Skeletal maturity free medical journals Skeletal maturity famous journals Skeletal maturity Google Scholar indexed journals Angular deformity articles Angular deformity Research articles Angular deformity review articles Angular deformity PubMed articles Angular deformity PubMed Central articles Angular deformity 2023 articles Angular deformity 2024 articles Angular deformity Scopus articles Angular deformity impact factor journals Angular deformity Scopus journals Angular deformity PubMed journals Angular deformity medical journals Angular deformity free journals Angular deformity best journals Angular deformity top journals Angular deformity free medical journals Angular deformity famous journals Angular deformity Google Scholar indexed journals Pre-injury articles Pre-injury Research articles Pre-injury review articles Pre-injury PubMed articles Pre-injury PubMed Central articles Pre-injury 2023 articles Pre-injury 2024 articles Pre-injury Scopus articles Pre-injury impact factor journals Pre-injury Scopus journals Pre-injury PubMed journals Pre-injury medical journals Pre-injury free journals Pre-injury best journals Pre-injury top journals Pre-injury free medical journals Pre-injury famous journals Pre-injury Google Scholar indexed journals Sports articles Sports Research articles Sports review articles Sports PubMed articles Sports PubMed Central articles Sports 2023 articles Sports 2024 articles Sports Scopus articles Sports impact factor journals Sports Scopus journals Sports PubMed journals Sports medical journals Sports free journals Sports best journals Sports top journals Sports free medical journals Sports famous journals Sports Google Scholar indexed journals Bone articles Bone Research articles Bone review articles Bone PubMed articles Bone PubMed Central articles Bone 2023 articles Bone 2024 articles Bone Scopus articles Bone impact factor journals Bone Scopus journals Bone PubMed journals Bone medical journals Bone free journals Bone best journals Bone top journals Bone free medical journals Bone famous journals Bone Google Scholar indexed journals Pain articles Pain Research articles Pain review articles Pain PubMed articles Pain PubMed Central articles Pain 2023 articles Pain 2024 articles Pain Scopus articles Pain impact factor journals Pain Scopus journals Pain PubMed journals Pain medical journals Pain free journals Pain best journals Pain top journals Pain free medical journals Pain famous journals Pain Google Scholar indexed journals
Article Details
1. Introduction
Recognized by Paul Tillaux, and later described by Kleiger and Mankin, the Tillaux fracture occurs in adolescents whom a portion of the distal tibial physis has started to close [1-7]. Closure happens in early adolescence; first centrally, then medially, and finally laterally [1]. The Tillaux fracture pattern results from an external rotation injury to the foot causing the anterior-inferior tibio-fibular ligament (AITFL) to avulse a portion of the open distal tibia physis, resulting in a Salter-Harris III Fracture An attempt at closed reduction and casting may be performed in adolescents with a displaced fracture [1, 8, 9]. Fractures displaced more than 2 mm have been treated with open reduction internal fixation (ORIF) due to a report demonstrating degenerative changes and increased risk of arthritis if the fracture and joint surface remains displaced [10] A recent article by Lurie et al demonstrated that fractures with a gap greater than 2.5 mm after closed reduction is an indication for surgical management [11] ORIF results in alignment of the joint surface, and prevention of articular incongruity and arthritis [12-20].
The literature describes two different fixation techniques. The first involves placement of one or two pins or screws obliquely from the epiphyseal fragment into the distal tibial metaphysis [15-17, 21-24] This technique violates the physis with the screw. The second technique involves placement of one or two screws parallel through the epiphysis and the Tillaux fragment [19]. The second technique does not violate the physis but requires very precise screw placement. A 2019 article from Gordon et al demonstrated that both direct and indirect fixation of juvenile Tillaux fractures were effective in maintaining an anatomic reduction of the fracture [23]. The purpose of this study was to report the outcomes, complications, and advantages of fixation of Tillaux fractures treated with an oblique compression screw that crosses the physis into the metaphysis.
2. Materials and Methods
This study was reviewed and approved by the college of medicine institutional review board. Ten patients with Tillaux fractures displaced greater than 2 mm were reviewed over a 3-year period. Three males and seven females were treated. The average age was 14 years. Inclusion criteria included individuals with a Tillaux fracture that remained displaced more than 2 mm following closed reduction. Patients were excluded if they did not undergo operative fixation for a Tillaux fracture. Measurements were made by the attending orthopedic surgeon on X-ray film. All patients failed closed reduction. Open reduction was performed via an anterolateral vertical 3 cm incision. General anesthesia, a tourniquet and fluoroscopy were utilized. A small arthrotomy was used to evaluate the articular surface. Fixation was performed with an obliquely placed 4 mm solid partially threaded screw (Synthes Paoli PA) that crossed the growth plate. A short leg non-weight bearing cast was placed for 3 weeks followed by a CAM boot for an additional 3 weeks with weight bearing as tolerated. Physical therapy was not utilized for any patient.
3. Results
10 patients with Tillaux fractures were reviewed. The mechanism of injury in two patients were the result of playing soccer, one from wrestling, one from roller skating, one from cross country, one playing baseball, one making a tackle, and three from a fall from height. The pre-operative fracture displacement averaged 4 mm (range 3 to 6). All fractures failed closed reduction. All fractures were anatomically reduced by open reduction and fixation with the use of an oblique screw placement (Figures 1 and 2). The average tourniquet time was 28 min (range 16 to 38). No infections, nerve injuries, or loss of reduction occurred. The average final follow-up period was 15 months with a range of 12 to 33 months. At final follow up, all had equal leg lengths and no angulation. Final leg-length discrepancy was measured using standardized blocks in clinic. No patient had pain, arthritis, joint stiffness, or limitation of activities at final follow up. All returned to pre-injury sports as tolerated. Six patients had hardware removed at an average of 18 weeks after surgery (range 8 to 30).
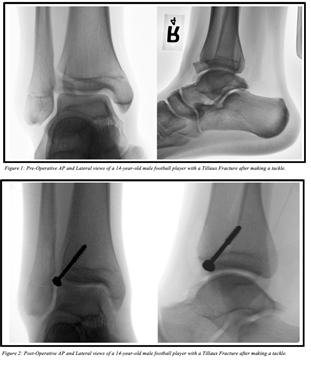
Figure 1:
4. Discussion
The distal tibia growth plate is the third most commonly injured growth plate [25-27]. Tillaux fractures are a transitional fracture of the growth plate. Most reports on Tillaux fractures are case series [28-31]. The most accepted mechanism of injury involves external rotation of the foot or internal rotation of the leg on a fixed foot [1, 5, 6]. This fracture pattern can be explained by an analysis of growth plate closure in adolescents. The distal tibial physis begins closing eighteen months before cessation of tibial growth. During this eighteen-month period, the physis begins to close. This occurs centrally first, then medially, and laterally last. A period of time exists where the lateral physis solely remains open. External rotation during this period of time results in a Tillaux fracture as the bony central and medial tibia are stronger than the lateral physis. Complete closure of the growth plate on average occurs at age 16-17 in boys and around 14-15 in girls. This makes the most susceptible age group for Tillaux fractures ages 12-16, before the growth plates have completely closed [1, 21, 28, 32].
Physeal injury is of less concern since most patients are close to skeletal maturity, and therefore complications like leg length discrepancy and angular deformity are rare due to decreased growth remaining at the physis [28]. However, these fracture types demand increased clinical awareness because it involves a major weight bearing articular surface. This case series demonstrated that anatomic reduction of the joint surface is the most important aspect of treating these fractures to minimize the risk of arthritis. Lurie et al reported that fractures with a gap greater than 2.5 mm after attempt at closed reduction was a negative predictor of functional outcome at a mean follow-up of 4.5 years [11] The current case series had no infections, nerve injuries, or loss of reduction with oblique screw placement; at final follow up, all had equal leg lengths and no angulation. No patient had pain, arthritis, joint stiffness or limitation of activities, and all returned to pre-injury sports as tolerated.
Use of an oblique screw which crosses the growth plate rather than parallel to the growth plate does not increase risk of complications. After successful bone healing and return to pre-injury activities, we recommended hardware removal to all patients. Four patients chose not to proceed with hardware removal. One study by Charlton et al. showed that total force, peak contact pressure and contact area were increased in cadavers after screw placement and decreased after screw removal [33].
The advantages to oblique screw placement through the physis include a technically simple, fast, and safe procedure. First, the angle can vary with oblique screw placement as noted in Figures 3 and 4, which allows for placement of a screw from any direction that the fracture morphology allows. Second, the procedure is theoretically faster due to the fact that perfection is not necessary with regards to screw angulation. Finally, the Tillaux fracture fragment can be so small that screws found in the fracture-sets often contain threads too numerous to obtain compression when used parallel to the physis. This can cause potential distraction of the fracture fragment as demonstrated in Figure 5. The limitations of this study include a small homogenous cohort of patients, lack of a control group, use of historical control groups from the literature, and lack of ten-year outcomes to evaluate for arthritis development. No patient in our cohort developed arthritis at the short term follow up. To our knowledge, there are no long-term studies evaluating the relationship of sustaining a Tillaux fracture to the future development of arthritis.
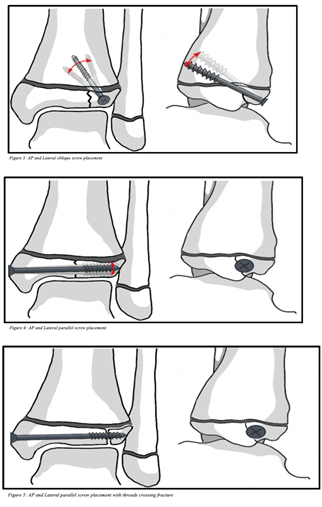
Figure 1:
5. Conclusion
The Tillaux fracture occurs in adolescents because of the unique pattern of closure of the distal tibial epiphysis. All patients in the current study that underwent ORIF reported similar outcomes of pain and range of motion. Use of an oblique screw crossing the growth plate did not lead to complications such as growth arrest, arthritis, loss of reduction, stiffness, or infection.
References
- Kleiger B, Mankin HJ. Fracture of the lateral portion of the distal tibial epiphysis. J Bone Joint Surg [Am] 46 (1964): 25-32.
- Letts RM. The hidden adolescent ankle fracture. J Pediatr Orthop 2 (1982): 161-164.
- Love SM, Ganey T, Ogden JA. (1990) Postnatal epiphyseal development: the distal tibia and fibula. J Pediatr Orthop 10 (1990): 298-305.
- Ogden JA, McCarthy SM. (1983) Radiology of postnatal skeletal development. VIII. Distal tibia and fibula. Skeletal Radiol 10 (1983): 209-220.
- Protas JM, Kornblatt BA. Fractures of the lateral margin of the distal tibia. The Tillaux fracture. Radiology 138 (1981): 55-57.
- Rang M. Children’s Fractures. (2nd edn). Philadelphia and Toronto: J.B. Lippincott Company (1983).
- Spinella AJ, Turco VJ. Avulsion fracture of the distal tibial epiphysis in skeletally immature athletes (juvenile Tillaux fracture). Orthop Rev 17 (1988): 1245-1249.
- Kleiger B. The mechanism of ankle injuries. J Bone Joint Surg [Am] 38 (1956): 59-70
- Spiegel PG, Cooperman DR, Laros GS. Epiphyseal fractures of the distal ends of the tibia and fibula. J Bone Joint Surg [Am] 60 (1978): 1046-1050.
- Ertl JP, Barrack RL, Alexander AH, et al. Triplane fracture of the distal tibial epiphysis. J Bone Joint Surg [Am] 70 (1988): 967-976.
- Lurie B, Van Rysselberghe N, Pennock AT, et al. Functional Outcomes of Tillaux and Triplane Fractures with 2 to 5 Millimeters of Intra-Articular Gap. J Bone Joint Surg Am 102 (2020): 679-686.
- Britton PD. Adolescent-type Tillaux fracture of the ankle: two case reports. Arch Emerg Med 5 (1988): 180-183.
- Dailiana ZH, Malizos KN, Zacharis K, et al. Distal tibial epiphyseal fractures in adolescents. Am J Orthop 28 (1999): 309-312.
- de Sanctis N, Della Corte S, Pempinello C. Distal tibial and fibular epiphyseal fractures in children: prognostic criteria and long-term results in 158 patients. JvPediatr Orthop B 9 (2000): 40-44.
- Dias LS, Giegerich CR. Fractures of the distal tibial epiphysis in adolescence J Bone Joint Surg [Am] 65 (1983): 438-44.
- Kling TF Jr. Operative treatment of ankle fractures in children. Orthop Clin North Am 21(1990): 381-392.
- Kling TF Jr, Bright RW, Hensinger RN. Distal tibial physeal fractures in children that may require open reduction. J Bone Joint Surg [Am] 66 (1984): 647-657.
- Koury SI, Stone CK, Harrell G, et al. Recognition and management of Tillaux fractures in adolescents. Pediatr Emerg Care 15 (1999): 37-39.
- Lintecum N, Blasier RD. Direct reduction with indirect fixation of distal tibial physeal fractures: a report of a technique. J Pediatr Orthop 16 (1996): 107-112.
- von Laer L. Classification, diagnosis, and treatment of transitional fractures of the distal part of the tibia. J Bone Joint Surg [Am] 67 (1985): 687-698.
- Dias LS, Tachdjian MO. Physeal injuries of the ankle in children. Clin Orthop 136 (1978): 230-233.
- Dingeman RD, Shaver GB. Operative treatment of displaced Salter-Harris III distal tibial fractures. Clin Orthop 135 (1978): 101-103.
- Gordon JE, Schoenecker PL, Klein SE. Juvenile Tillaux Fractures: A Comparison of Direct and Indirect Fixation. Integr J Orthop Traumatol 2 (2019): 1-6.
- Salter RB. Injuries of the ankle in children. Orthop Clin North Am 5 (1974): 147-152.
- Mann DC, Rajmaira S. Distribution of physeal and nonphyseal fractures in 2,650 long-bone fractures in children aged 0-16 years. J Pediatr Orthop 10 (1990): 713-716.
- Mizuta T, Benson WM, Foster BK, et al. Statistical analysis of the incidence of physeal injuries. J Pediatr Orthop 7 (1987): 518-523.
- Peterson CA, Peterson HA. Analysis of the incidence of injuries to the epiphyseal growth plate. The Journal of Trauma: Injury, Infection, and Critical Care 12 (1972): 275-281.
- Choudhry I, Wall E, Eismann E, et al. Functional outcome analysis of Triplane and Tillaux fractures after closed reduction and Percutaneous fixation. J Pediatr Orthop (2013).
- Gross RH. Ankle Fractures in Children. Bull N Y Acad Med 63 (1987): 739-761.
- Kaya A, Altay T, Ozturk H, et al. Open reduction and internal fixation in displaced juvenile Tillaux fractures. Injury 38 (2007): 201-205.
- Tiefenboeck TM, Binder H, Joestl J, et al. Displaced juvenile Tillaux fractures: Surgical treatment and outcome. Wien Klin Wochenschr 129 (2017): 169-175.
- Schlesinger I, Wedge JH. Percutaneous reduction and fixation of displaced juvenile Tillaux fractures: a new surgical technique. JPediatrOrthop 13 (1993): 389-391.
- Charlton M, Costello R, Mooney JF, et al. Ankle Joint Biomechanics Following Transepiphyseal Screw Fixation of the Distal Tibia. Journal of Pediatric Orthopaedics 25 (2005): 635-640.
