Nursing Care of Skin Damage of Elbow Gottron’s Disease in a Case of Amyopathic Dermatomyositis Based on Multidisciplinary Cooperation
Article Information
Sha Yaping, Xu Hongbo*, Qian Liping*, Wang Haiting
Department of Rheumatology, RenJi Hospital South Campus, School of Medicine, Shanghai Jiaotong University, Shanghai, China
*Corresponding Author: Xu Hongbo, Department of Rheumatology, RenJi Hospital South Campus, School of Medicine, Shanghai Jiaotong University, Shanghai, China
Qian Liping, Department of Rheumatology, RenJi Hospital South Campus, School of Medicine, Shanghai Jiaotong University, Shanghai, China
Received: 15 October 2019; Accepted: 03 December 2019; Published: 11 December 2019
Citation:
Sha Yaping, Xu Hongbo, Qian Liping, Wang Haiting. Nursing Care of Skin Damage of Elbow Gottron’s Disease in a Case of Amyopathic Dermatomyositis Based on Multidisciplinary Cooperation. Fortune Journal of Rheumatology 1 (2019): 034-039.
View / Download Pdf Share at FacebookAbstract
Objectives: To analyze the effect of multidisciplinary collaboration in the treatment of skin lesion wounds caused by Gottron's disease of elbow in a patient with amyopathic dermatomyositis.
Methods: A multi-disciplinary team of rheumatologists, orthopaedicians, nutritionists and wound therapists are formed to cooperate in patient disease control, wound debridement, wound bed preparation and surgically sutured the wound of joints.
Results: The right elbow wound of the patient healed in 47 days and the left elbow wound healed in 74 days.
Conclusions: Multidisciplinary cooperation can take care of patients in an all-round way, reduce wound pain and wound healing.
Keywords
<p>Amyopathic dermatomyositis, Elbow lesions, Multidisciplinary collaboration</p>
Amyopathic dermatomyositis articles, Elbow lesions articles, Multidisciplinary collaboration articles
Amyopathic dermatomyositis articles Amyopathic dermatomyositis Research articles Amyopathic dermatomyositis review articles Amyopathic dermatomyositis PubMed articles Amyopathic dermatomyositis PubMed Central articles Amyopathic dermatomyositis 2023 articles Amyopathic dermatomyositis 2024 articles Amyopathic dermatomyositis Scopus articles Amyopathic dermatomyositis impact factor journals Amyopathic dermatomyositis Scopus journals Amyopathic dermatomyositis PubMed journals Amyopathic dermatomyositis medical journals Amyopathic dermatomyositis free journals Amyopathic dermatomyositis best journals Amyopathic dermatomyositis top journals Amyopathic dermatomyositis free medical journals Amyopathic dermatomyositis famous journals Amyopathic dermatomyositis Google Scholar indexed journals Elbow lesions articles Elbow lesions Research articles Elbow lesions review articles Elbow lesions PubMed articles Elbow lesions PubMed Central articles Elbow lesions 2023 articles Elbow lesions 2024 articles Elbow lesions Scopus articles Elbow lesions impact factor journals Elbow lesions Scopus journals Elbow lesions PubMed journals Elbow lesions medical journals Elbow lesions free journals Elbow lesions best journals Elbow lesions top journals Elbow lesions free medical journals Elbow lesions famous journals Elbow lesions Google Scholar indexed journals Multidisciplinary collaboration articles Multidisciplinary collaboration Research articles Multidisciplinary collaboration review articles Multidisciplinary collaboration PubMed articles Multidisciplinary collaboration PubMed Central articles Multidisciplinary collaboration 2023 articles Multidisciplinary collaboration 2024 articles Multidisciplinary collaboration Scopus articles Multidisciplinary collaboration impact factor journals Multidisciplinary collaboration Scopus journals Multidisciplinary collaboration PubMed journals Multidisciplinary collaboration medical journals Multidisciplinary collaboration free journals Multidisciplinary collaboration best journals Multidisciplinary collaboration top journals Multidisciplinary collaboration free medical journals Multidisciplinary collaboration famous journals Multidisciplinary collaboration Google Scholar indexed journals rheumatologists articles rheumatologists Research articles rheumatologists review articles rheumatologists PubMed articles rheumatologists PubMed Central articles rheumatologists 2023 articles rheumatologists 2024 articles rheumatologists Scopus articles rheumatologists impact factor journals rheumatologists Scopus journals rheumatologists PubMed journals rheumatologists medical journals rheumatologists free journals rheumatologists best journals rheumatologists top journals rheumatologists free medical journals rheumatologists famous journals rheumatologists Google Scholar indexed journals orthopaedicians articles orthopaedicians Research articles orthopaedicians review articles orthopaedicians PubMed articles orthopaedicians PubMed Central articles orthopaedicians 2023 articles orthopaedicians 2024 articles orthopaedicians Scopus articles orthopaedicians impact factor journals orthopaedicians Scopus journals orthopaedicians PubMed journals orthopaedicians medical journals orthopaedicians free journals orthopaedicians best journals orthopaedicians top journals orthopaedicians free medical journals orthopaedicians famous journals orthopaedicians Google Scholar indexed journals wound therapists articles wound therapists Research articles wound therapists review articles wound therapists PubMed articles wound therapists PubMed Central articles wound therapists 2023 articles wound therapists 2024 articles wound therapists Scopus articles wound therapists impact factor journals wound therapists Scopus journals wound therapists PubMed journals wound therapists medical journals wound therapists free journals wound therapists best journals wound therapists top journals wound therapists free medical journals wound therapists famous journals wound therapists Google Scholar indexed journals joints articles joints Research articles joints review articles joints PubMed articles joints PubMed Central articles joints 2023 articles joints 2024 articles joints Scopus articles joints impact factor journals joints Scopus journals joints PubMed journals joints medical journals joints free journals joints best journals joints top journals joints free medical journals joints famous journals joints Google Scholar indexed journals electromyography articles electromyography Research articles electromyography review articles electromyography PubMed articles electromyography PubMed Central articles electromyography 2023 articles electromyography 2024 articles electromyography Scopus articles electromyography impact factor journals electromyography Scopus journals electromyography PubMed journals electromyography medical journals electromyography free journals electromyography best journals electromyography top journals electromyography free medical journals electromyography famous journals electromyography Google Scholar indexed journals myositis articles myositis Research articles myositis review articles myositis PubMed articles myositis PubMed Central articles myositis 2023 articles myositis 2024 articles myositis Scopus articles myositis impact factor journals myositis Scopus journals myositis PubMed journals myositis medical journals myositis free journals myositis best journals myositis top journals myositis free medical journals myositis famous journals myositis Google Scholar indexed journals dermatomyositis articles dermatomyositis Research articles dermatomyositis review articles dermatomyositis PubMed articles dermatomyositis PubMed Central articles dermatomyositis 2023 articles dermatomyositis 2024 articles dermatomyositis Scopus articles dermatomyositis impact factor journals dermatomyositis Scopus journals dermatomyositis PubMed journals dermatomyositis medical journals dermatomyositis free journals dermatomyositis best journals dermatomyositis top journals dermatomyositis free medical journals dermatomyositis famous journals dermatomyositis Google Scholar indexed journals
Article Details
1. Introduction
Dermatomyositis (DM) is an autoimmune disease affecting skin and muscle. At present, patients with typical DM lesions as the main clinical manifestation, no myositis for at least 6 months or longer, or laboratory examinations such as muscle magnetic resonance or electromyography with mild myositis are collectively referred to as clinical amyopathic dermatomyositis. DM lesions are not only closely related to disease activity, but also seriously affect the quality of life and long-term prognosis of patients. Gottron maculopapular rash is a typical skin lesion in amyopathic dermatomyositis, which is accompanied by pain [1] and found on rubbed joints, such as metacarpophalangeal joints, interphalangeal joints, elbows and knees. Besides, amyopathic dermatomyositis is also characterized by symmetrical weakness of upper limb muscles, neck muscles and swallowing muscles. Malnutrition results from the dysphagia and the use of glucocorticoid or immunosuppressive drugs associate with the delayed wound healing. The core idea of multidisciplinary collaboration is to develop a standardized, individualized and continuous comprehensive treatment plan for patients with specific rheumatic diseases. From October 25, 2018 to February 26, 2019, a 56-year-old male DM patient was treated in our multi-disciplinary team of rheumatologists, orthopaedicians, nutritionists and wound therapists. The rheumatologist adjusted the medication precisely and the nutritionist regulated the diet and nutrition. The wound team prepared the wound bed using the theory of wet healing and the orthopedic surgeon sutured the wound. Finally, the patient's bilateral elbow wound healed. The process, method and follow-up of wound treatment are reported as follows.
2. Results
The patient, a 56-year-old male, had a history of long-term exposure to NaOH in an electroplating factory. In August 2018, he developed multiple skin blisters on both upper extremities, accompanied by ulceration, pus and scab. He also experienced fever, Tmax >39°C, accompanied by chills and fatigue. Pulmonary CT showed effusion in the lower lobes of both lungs. In September, the symptoms progressed, he felt chest tightness and shortness of breath. In October, capillary dilated erythema was found on the lateral cheek, posterior ear and anterior V-shaped area of the neck. There were ulcers on both sides of the elbows (4 cm × 3 cm and 3 cm × 3 cm). On October 25, 2018, he was admitted to our rheumatology department and the myositis antibody test showed positive anti-MDA5 and anti-Ro52 antibodies. So the diagnosis of myopathic dermatomyositis was established [3] and he immediately received methylprednisolone intravenously and tofacitinib orally. Rituximab and cyclophosphamide were also given to the patient due to the rapid development of the pulmonary fibrosis. At the same time, the painful skin lesion of elbow were taken care by the nurses and wound therapist.
2.1 Combined debridement method
2.1.1 Mechanical debridement: The wound was wiped with saline cotton ball to clear away superficial necrotic tissue. Then, necrotic tissue at the bottom of the wound was removed using tweezers and scissors without injuring the joint cavity. Autolysis debridement can degrade necrotic tissue by using effective ingredients such as inflammatory cells and growth factors secreted by the wound itself to promote granulation growth [4]. Oil gauze was used to keep the moist of the wound and promote the growth of the fresh tissue. After 18 days, 75% of the yellow necrotic tissue in the wound decreased to 25%. After 30 days, 100% of the yellow necrotic tissue in the base was clear, turned to 100% red fresh tissue.
2.1.2 Reduce friction: Elastic bandage was used to reduce friction between wound and dressing. After the wound bed is fully prepared, seamless tape was used to pull the wound in the right elbow [5] and the patient was told to cooperate with the upper limb immobilization.
2.1.3 Surgical suture: Since the use of immunosuppressive agents and glucocorticoid increases the risk of wound infection and delayed healing, the wound was sutured by the orthopaedic surgeon longitudinally after assessing that the microbial culture was negative. After two weeks, the suture was removed, and the wound healed well.
2.2 Nutritional support
Nutritional Risk Screening 2002 (NRS2002) score was 4 when he was admitted to hospital, which means nutritional risk and nutritional therapy was needed. The patient was given oral administration of nutrient powder which was convenient and full of protein. Albumin was given weekly to correct hypoproteinemia. The patient's blood sugar was also monitored, and caloric controlled diet was given.
2.3 Psychological nursing
To relieve the pain, lidocaine diluent gauze was used while changing dressings. Besides, visual pain score was used to evaluate the pain and communication was performed with family members before dressing change to inform wound outcome and obtain informed consent.
2.4 Follow up
After multi-disciplinary collaboration, all the wounds healed, and the patient was followed up after discharge. The condition was stable, the wounds were painless and uncomfortable, and the elbow movement function was good.
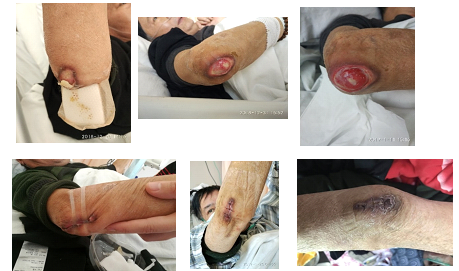
Figure 1: Right elbow wound of Gottron disease healing process.
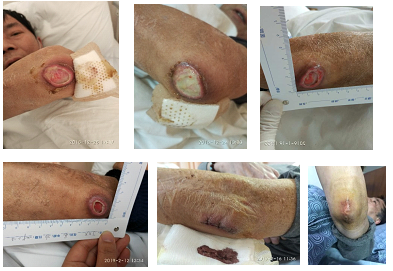
Figure 2: Left elbow wound of Gottron disease healing process.
3. Discussion
3.1 Evidence-based individualized wound treatment
3.1.1 Preparation of wound bed: The erythema scab on the elbow of the patient worsened further during the active period of the disease. The scab fell off and the wound was covered with yellow necrotic tissue. The wound was delayed and became a chronic wound due to the disease. Wound bed preparation includes not only debridement, anti-infection, wet treatment, but also comprehensive conditioning of patients general conditions such as nutritional balance, pain relief, alleviating psychological anxiety, etc. [7]. Studies have shown that pain and anxiety can affect wound healing time [8]. Therefore, before preparing the wound bed for the patient, the pain degree of the patient was assessed and wet dressing with gauze diluted with lidocaine was given to relieve the pain of cleaning the wound. Fixed dressings and immobilized affected limbs to reduce pain and discomfort caused by wound friction. Calcium alginate was used to remove yellow necrotic tissue and promote the growth of wound granulation tissue. Finally, the wound was turned into red granulation tissue, and then foam dressing was used for wet healing to promote granulation growth and epithelial crawling.
3.1.2 Combined debridement: Research showed that combined debridement plays a good role in the treatment and nursing of pressure ulcer and the application of diabetic foot ulcer [9, 10]. Combined debridement overcomes the shortcomings of vascular or tissue injury and pain caused by sharp debridement, and overcomes the shortcomings of long autolysis debridement cycle. It could shorten the debridement cycle, reduce the operational risk and reduce pain.
3.1.3 Joint wound healing: The elbow extension wound is affected by joint movement, which easily forms friction force to separate the epidermis from the subcutaneous tissue and hinder the healing of the wound. Studies have shown that the use of seamless tap to pull wounds after bandage compression treatment of abdominal infection wounds has obvious effect [11]. We tried to promote the healing of elbow wounds in a non-invasive way when the wound bed is well prepared. Because of poor pulmonary function, hypoxia and hypoxia, the patient's agitation was not effective. Ultimately, surgical suture healed the wound and achieved the final wound healing.
3.2 Multidisciplinary diagnosis and treatment improves the treatment level of chronic wounds in joint sites
Rheumatic diseases can damage many organs in the whole body. Dermatomyositis affects many organs such as muscle, skin, lung and so on. It requires comprehensive diagnosis and treatment of multi-disciplinary knowledge. At present, the multi-disciplinary cooperation model is also widely used in wound treatment [13, 14]. In this case, the rheumatologist carried out comprehensive control of patients, including the control of the disease, improvement of lung function, rational use of antibiotics, according to the results of drug sensitivity and systemic inflammation indicators; nutritionists strengthened enteral nutrition support to improve body tolerance; wound specialist nurses assessed patients' general and local conditions, according to the results of drug sensitivity and systemic inflammation indicators. Principle of wound treatment and preparation of wound bed. The orthopaedic surgeon sutures the wound at the joint. Eventually, both elbow wounds healed and the quality of life improved.
4. Conclusion
Multidisciplinary collaboration should be widely used in patients with rheumatism. Amyopathic dermatomyositis has typical skin lesions, and most of them appeared at rubbed joints. During the active stage of disease, skin damage is difficult to heal due to poor nutrition, joint friction, immunosuppressive drugs and so on. At present, wound specialist nurses have little research on wounds caused by rheumatic immune diseases, which calls for more exploration and research.
References
- Hu Bingyan, Wang Jinfeng, Gao Zhenhui. Study on the status quo of polymyositis/dermatomyositis. Chinese and foreign medical treatment (2017).
- Huang Xiaowei, Wang Kai, Ding Liren. Retrospective comparative analysis of amniotic dermatomyositis and typical dermatomyositis. Chinese Journal of Emergency Medicine 27 (2018): 562.
- Wang Yi, Li Ying, Li Shengjin. Meta-analysis of the diagnostic efficacy of anti-MDA5 antibody in adult and juvenile dermatomyositis complicated with interstitial lung disease. Journal of Clinical Laboratory (2018).
- Zhang Wei. Application of combined debridement technique in patients with lower extremity venous ulcer. Integrated Chinese and Western Medicine Nursing (Chinese and English) 3 (2017): 111-113.
- Huang Manrong, Xiaoping, Wu Shaoyun, et al. Analysis of the effect of delayed wound healing after seamless tape bonding. Chinese Journal of Practical Nursing 27 (2011): 2-3.
- Effects of nutritional support on nutritional status and prognosis of stroke patients with dysphagia under the guidance of NRS 2002 nutritional risk screening. Medical clinical study 34 (2017): 2010-2012.
- Gaoqiong, Xue Xiaodong. Research progress of wound bed preparation. Clinical medicine research and practice 28 (2017): 200-202.
- Liu Jia, Yu Ruiying, Chen Jin, et al. The effect of pain during dressing replacement on wound healing rate. PLA Journal of Nursing 28 (2011): 22-24.
- Chen Meihong, Wang Yongmei. Treatment and nursing of pressure sore by combined debridement. Journal of Nurse Education 25 (2010): 478-479.
- Wu Weiying, Chen Yingjie, Huang Jianshi, et al. Application of combined debridement in diabetic foot ulcer. Chinese Journal of Modern Nursing 17 (2011).
- Huang Liming, Li Shuimei, Li Dongli, et al. Observation of the effect of tension and compression combined with abdominal band fixation in the treatment of infectious wounds after abdominal surgery. Journal of Nurse Education 20 (2017): 80-81.
- Lin Xiaohui, Chen Pan. Progress in diagnosis and treatment of dermatomyositis and polymyositis. Chinese Medicine (2018).
- Chen Yan, Xia Dongyun, Wu Ling. Application of multidisciplinary diagnosis and treatment model for chronic wounds in wound care clinic. China Nursing Management 18 (2018): 1013-1017.
- Ningning, Chen Jiali, Chen Zhonglan, et al. Exploring team building in the multidisciplinary cooperation model of chronic wound treatment. Journal of Nurses' Further Education 25 (2010): 1373-1377.
