Measurement of Radiographers’ Pandemic Experiences and Perceptions During COVID-19
Article Information
Muna AlMulla
Radiological Sciences Department, Faculty of Allied Health, Kuwait University, Jabreyah, Kuwait
*Corresponding author: Muna AlMulla. Radiological Sciences Department, Faculty of Allied Health, Kuwait University, Jabreyah, Kuwait. Tel: +009699195122.
Received: 08 March 2022; Accepted: 16 March 2022; Published: 22 March 2022
Citation: Muna AlMulla. Measurement of Radiographers’ Pandemic Experiences and Perceptions During COVID-19. Archives of Clinical and Biomedical Research 6 (2022): 322-334.
View / Download Pdf Share at FacebookAbstract
COVID-19 is a recent globally-manifested phenomenon that compels healthcare workers to face and rapidly adapt to forceful changes. While much of the research has a general focus on all healthcare professions,this work has the specific focus on radiographers because they play a critical role in monitoring the spread of COVID-19. A Pandemic Experiences and Perceptions Survey (PEPS) was used to report on radiographers’ experiences. A cross-sectional questionnaire survey was distributed to radiographers between May and June 2020. A number of 102 (29.4%) completed the survey (48 [47.1%] males and 54 [52.9%] females). With respect to the five PEPS tools, the means (± SD) of each tool were as follows: disruption, 2.487 (±0.94); resources, 2.576 (±0.914); risk perception, 2.946 (±1.57); impact on work-life areas, 3.81 (±0.711); and leadership, 3.795 (±0.807). Eighty percent of radiographers were in agreement that COVID-19 affected their work distribution and 74.5% did not consider their protective equipment, staff availability, and support staff competence to be adequate. Sixty-two percent of the participants reported fear of the virus. This study allows for front-line radiographers to quickly express concerns and provides insight into the issues that must be addressed during the current and future outbreaks.
Keywords
COVID-19; Computed tomography; Radiography; Ultrasound
COVID-19 articles; Computed tomography articles; Radiography articles; Ultrasound articles
Article Details
1. Introduction
Since COVID-19 surfaced in January, the pandemic has caused an increasing heavy load on healthcare systems. Hospitals, and medical clinics have had to readjust their working dynamics to address the changes associated with this outbreak. According to the Department of Occupational Safety and Health Administration (OSHA), healthcare workers are at high risk of infection because of their critical work controlling the outbreak [1]. They face mental stress, physical exhaustion, separation from families, stigma, and pain of losing their patients or colleagues. While much of the research on healthcare professionals during COVID has a general focus on all healthcare professions [2, 3] this study focuses specifically on radiographers. There is a lack of data on radiographers' wellbeing in Kuwait, especially during this pandemic. Radiography plays a critical role in monitoring the spread of COVID-19. In addition to laboratory testing, some of the essential diagnostic tools used to identify the prevalence of COVID-19 are general radiography (X-ray) and Computed Tomography (CT) imaging, which put radiographers in direct contact with COVID-19 patients [4-7]. Therefore, radiographers’ knowledge of COVID-19 is of great value in preventing the spread of infection [8]. An assessment of employees' experiences can provide leaders with crucial guidance to manage the current situation, lead organizational recovery afterward and anticipate future challenges [9,10]. For this study, a Pandemic Experiences and Perceptions Survey (PEPS) was used to report on radiographers’ experiences. The PEPS is a powerful tool to measure employees' experience during a pandemic and provides critical information on the extent of workflow disruption, the measure and availability of resources, risk perception, impact on working dynamics (e.g., workload, control, reward, community, fairness, values) and management [10]
2. Methods
2.1. Ethical approval
The study followed the Declaration of Helsinki checklist for reporting the results of Internet e-surveys (CHERRIES), which includes ethical clearance and approval from Kuwait's Ministry of Health Ethical Review Board.
2.2. Informed consent
The study maintained confidentiality by making all participants' information anonymous throughout the study. Eligible radiographers' participation in this survey was entirely voluntary. Before undertaking the survey, all participants signed electronic informed consent to activate the survey. Additionally, for every survey link sent by e-mail, consent was included. “Radiographers of all levels of experience (beginner to expert) are invited to participate in this study. Participants have the right to volunteer or withdraw from the study at any time. Radiographers who choose to participate in this study are requested to complete the following tools: (a) extent of impact, (b) resources, (c) risk perception, (d) work life, and (e) leadership. This study does not include any medical intervention. The researchers will keep all information confidential”.
2.3. Study population and participants
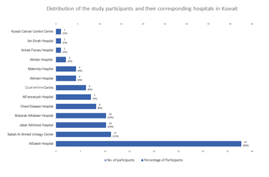
The study population consisted of radiographers who work in Kuwait government hospitals and newly authorized medical quarantine centers (Figure 1). The inclusion criteria covered all active radiographers of all ages, male or female, who had been and were still working in the locations mentioned from January (the start of the pandemic) to the present. The exclusion criteria were all other healthcare workers, radiography students, and radiographers who were not active during the pandemic period (Figure 1).
The survey was active online for participation from May 2020 until June 2020. The participants worked in different areas within departments, such as general and portable X-ray, Computed Tomography (CT), Magnetic Resonance Imaging (MRI), and Ultrasound (US). Participation was voluntary, and all personal information was anonymous. The survey distribution was conducted through different channels to encourage participation; examples include sending group e-mails, using radiography phone groups, using hospital social media channels, and contacting the head of radiography staff.
2.4. Pandemic experiences and perceptions survey (PEPS)
A license was purchased from Mind Garden Incorporated to administer the PEPS tool. The tool consists of 2 pages and 34 questions in total (Table 1), with an additional page that includes demographic variables such as age, gender, work experience, job title, and educational attainment (Table 2). Ten to 15 minutes are needed to complete the survey. The PEPS uses five main tools: disruption (i.e., the extent of workflow disruption), resources (i.e., adequacy of resources to meet demands), risk perception (i.e., contact, control, potential harm), impact on work-life areas (i.e., workload, control, reward, community, fairness), and perceptions of leadership (i.e., immediate and manager). The survey also includes two open-text items identifying what would help employees and what gives them hope.
|
Tool number |
PEPS tool name |
Number of items included |
Scale used |
|
1 |
Disruption |
3 |
0 = No Effect at All |
|
1 = Small Effect |
|||
|
2 = Moderate Effect |
|||
|
3 = Large Effect |
|||
|
4 = Completely Dominated the Work |
|||
|
2 |
Resources |
5 |
0 = Completely Inadequate |
|
1 = Barely Adequate |
|||
|
2 = Somewhat Adequate |
|||
|
3 = Mostly Adequate |
|||
|
4 = Completely Adequate |
|||
|
3 |
Risk Perception |
4 |
1 = No Risk at All |
|
2 = Minor Risk |
|||
|
3 = Serious Risk |
|||
|
4 = Life-Threatening Risk |
|||
|
4 |
Impact on Work-life Areas |
7 |
1 = Strongly Disagree |
|
2 = Disagree |
|||
|
3 = Hard to Decide |
|||
|
4 = Agree |
|||
|
5 = Strongly Agree |
|||
|
5 |
Leadership |
10 |
1 = Not at All |
|
2 = Once in Awhile |
|||
|
3 = Sometimes |
|||
|
4 = Fairly Often |
|||
|
5 = Frequently, if not Always |
Table 1: Categorization of the PEPS tool, items and scales.
Table 2: Characteristics of the respondents numbers, percentage, and the distribution of PEPS scores for five tools among healthcare workers (No. = 102); the statistic applied here was implemented according to a previous (Zhang et al., 2020) study and has been adapted to this work.
3. Data Analysis
Data were analyzed using Wizard (version 1.9. 42), Excel & Xlstat (version 16. 37), and Minitab Express (version 1.5.3) for Mac. Descriptive analysis was reported as a percentage, and the mean scores, average scoring, mean and Standard Deviation (SD) for all five PEPS tools were obtained. A t-test and ANOVA were conducted to analyze the relationship between the dependent variable (PEPS tools) and the independent variables (demographic characteristics of the participants). All the differences in the estimated variables were statistically significant if P <0.05.
4. Results
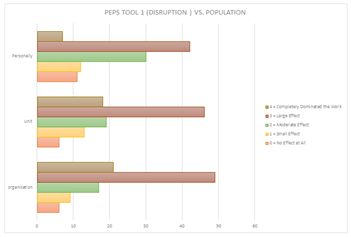
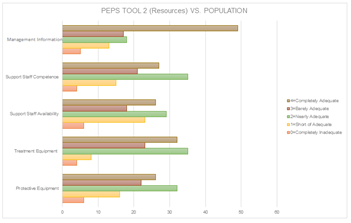
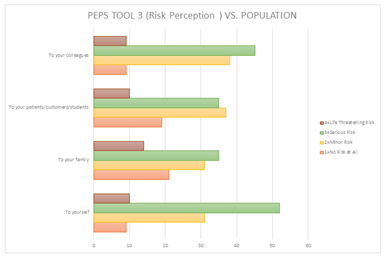
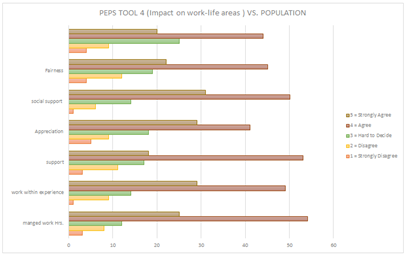
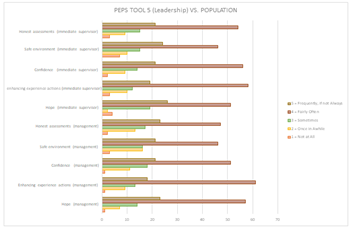
According to the latest statistics [11], there are 571 active diagnostic medical imaging radiographers in Kuwait. After applying the exclusion criteria, an estimated 400 radiographers are actively working with COVID-19 patients. A total of 347 participants (86%) attempted to complete the survey; however, 102 (29.4%) participants completed the survey, including 48 (47.1%) males and 54 (52.9%) females. The questionnaire participants had a mean (± SD) age of 35.7 ± 8.2 years. A total of 89% of participants indicated that they had been in direct contact with COVID-19. Of these participants, 57.8% stated that they had training, support, and equipment to provide them with some control over the virus. Furthermore, more than half of the participants (68.7%) expressed fear of the virus and believed that it presented a danger to them. The participants were also asked two open-text questions. The first question asked them to state what provided them with hope. For this question, 87% of the answers included one or a combination of the following items: management, family, friends, and religion, while 13% replied “nothing”. The second open-text question was on aspects of the working environment that the participants felt should be improved. For this question, 66% of the answers involved improving protective measures, equipment, management, and staff regulations, whereas 34% answered “nothing”. With regard to the five PEPS tools, the mean (± SD) score scales were as follows (Table 1): disruption 2.487 (±1.094), resources 2.580 (±1.196), risk perception 2.963 (±1.713), impact on work-life areas 3.810 (±0.992), and leadership 3.795 (±0.965). Radiographers who answered PEPS tool 1 thought that COVID-19 had a substantial effect on their work as an organization (48%), unit (45.1%), and personally (41.2%) (Figure 2). According to (Table 2), with regard to the association of demographic characteristics and PEPS for radiographers, nationality was significantly affected by the changes, P <0.001. In the second PEPS tool, radiographers provided mixed opinions with regard to the tool items. Almost half of the radiographers agreed that management provided entirely adequate information (48%); however, responses were mixed in rating staff support, availability, and equipment (Figure 3). PEPS tool 3 shows that radiographers agreed that COVID-19 presents serious risks (Figure 4). Almost half of the radiographers believed that the work-life impact was manageable and that their experience and knowledge were adequate (Figure 5). Half of the radiographers had a positive outlook on leadership, whether it be management or immediate supervisors, in dealing with pandemic-related issues (Figure 6).
5. Discussion
COVID-19 is a recent globally manifested phenomenon that compels healthcare workers to face and rapidly adapt to forceful changes. The impact of a pandemic is often intense, and reports that provide radiographers with feedback about their work experience can be an excellent source for necessary data on the pandemic. Moreover, Kuwait's radiographic population is diverse and consists of people with a wide range of ethnicities, genders, and physical abilities. Thus, the results generated from this report could be of great help to other healthcare workers in formulating recovery plans and future preparedness. To the best of our knowledge, this study is the first conducted in Kuwait that measures radiographers’ pandemic experiences and perceptions. This study started in the early to middle stages of the COVID-19 outbreak in areas that were pandemic and, non-pandemic but critically affected and during a full lockdown of the country. First, with regard to the extent of the workflow disruption for radiographers, 80% of radiographers agreed that COVID-19 affected their work as an organization, as a unit, and for themselves personally. When dealing with an epidemic, forced changes must be applied to overcome several factors (e.g., spread/infection). Recent publications suggest that some of the most effective ways to control the spread of the virus are by changing the dynamics of the working environment, such as segregating radiographers into teams, reducing the number of working staff (e.g., secretaries, administrators), continually disinfecting equipment, using additional isolation rooms, and increasing the use of mobile radiography units [4,12,13]. The daily requirement to wear heavy protective gear such as gloves, head cap, disposable gown, shoe covers, and protective goggles can be exhausting and time consuming [1,5,14] Consequently, radiographers rated these precautions in the second PEPS tool. In this section, the scores for management, resources, and control show that 4.9% of radiographers found that management's information was completely inadequate, 47.1% felt that they had some form of adequate information, and 48% agreed that completely adequate information was available from management in dealing with this crisis. Conversely, most radiographers (74.5%) agreed that their protective equipment, staff availability, and support staff competence were not adequate. Consequently, this affected their risk perception, which was the third item in the PEP survey. The participants scored their risk perception (e.g., contact, virulence, and control). Underestimating risk can prompt unnecessary incidents (e.g., carelessness, negligence) and lack of awareness often leads to an unconcerned attitude, which may adversely affect the preparedness to meet challenges, while overestimating risk can undermine organizational effectiveness (e.g., panic, chaos, fear). Sixty-two percent of the participants reported that they feared the virus and felt underprepared to deal with it, and they scored the risk perception of their colleagues at 54%. However, less than half of the participants believed that the virus would not be of great risk to the public (45%) or their families (49%). Significant demographics that affect this tool include the participants’ nationality (P 0.009 < 0.05), health condition (P 0.050 < 0.05) and radiographic working level (P 0.004 <0.005). More than half of the participating radiographers in this study had more than ten years of working experience (52%) and an education level of a bachelor’s degree (71.5%) or higher (23.5%) (Table 2). Surprisingly, however, these factors showed no significance in any PEPS tools.
Radiography is a skill-based practice that requires a high level of knowledge and continuous ongoing education and updates [15]. Like most healthcare workers, radiographers must undergo frequent job training, especially during a pandemic. Ongoing training provides new, critical information regardless of previous knowledge.5 Having training and knowledge enables workers to feel confident in doing their work, which provides some measure of stress reduction [9] All epidemics and pandemics have unique characteristics in terms of causality, progression, and control measures [16]. It is crucial to provide health education and awareness during such situations to effectively prevent the spread of disease [17]. A previous study showed that health professionals often have good awareness and positive attitudes toward epidemics/pandemics and often experience low anxiety [18]. Nevertheless, studies from Ethiopia reported poor knowledge and erroneous beliefs among healthcare professionals during two outbreaks in 2015 and 2020, and both studies encouraged intense training of healthcare professionals [19,20]. In a study conducted in Trinidad and Tobago following the H1N1 epidemic in 2016, it was found that a significant proportion of the general public was unaware of the seriousness and measures of prevention of the epidemic [17]. Research suggests that although all radiographers perform a similar technical occupation, the impact of the country’s culture on radiography manifests through the scope of practice and level of recognition within the healthcare spectrum [21]. This study examined radiographers who perform a similar technical occupation, but their departments were in a wide variety of cultural and socioeconomic environments, which significantly affected each radiographer. Finally, the work-life and leadership sections (PEPS 4 - 5) identify management areas that employees perceive as going well and those in which they would appreciate improvement. More than 70% felt that they had flexible working hours, their workload was within their capabilities, they felt supported, there was a good sense of community and fairness, and no conflict existed between priorities and values. Similarly, almost half of the participants agreed that leadership, whether management or immediate supervisors, provided hope, confidence, honest assessment, and a safe environment. It is the responsibility of managers and supervisors to provide training on the outbreak in a formal setting to ensure that all workers understand the details of disease transmission, screening, and the use of personal protective equipment. Radiographers’ working level showed significance in reports using the PEPS tool five. The working level indicates work responsibilities and supervision duties; as the level increases, radiographers’ obligations and responsibilities also increase. The majority of radiographers described fear of the risk of working with COVID-19; however, they had a positive attitude toward their leadership and management. Most radiographers stated that despite their faith in management, additional education interventions and campaigns were required to improve their sense of safety and confidence. People who work in an organizational environment that is insensitive to working with COVID-19 will likely experience some burnout depending on both the quality of the management system and how leaders react in real time. The PEPS tool can help to limit future burnout and conflicts.
6. Limitations
Despite the findings introduced here, it is important to stress that this survey shows some limitations. The number of radiographers and the amount of participation were low. Despite the rigorous methods of encouragement, it was challenging to encourage people to complete the survey; the short period of data collection may have contributed to this low number of responses. Nevertheless, the sample in this study is considered a moderate sample size. Moreover, this pandemic caused many to be busy watching the news and taking care of personal affairs. Thus, participation involved radiographers who were active on the Internet or social media during the short period of data collection, which might have led to selection bias and sampling error; this prevents the ability to generalize our results.
7. Conclusion
Medical practice differs widely among different countries, mainly due to the variability of access to resources (e.g., viral testing and imaging equipment, specialized staff, protective equipment). Medical imaging plays an essential auxiliary role in diagnosing COVID-19 patients. It has been well documented that chest radiographs should be the first-line imaging tool for diagnosing and monitoring COVID-19 patients. Radiology departments must reorganize their facilities and staff to enhance safety and minimize the risks of infection. Supporting radiographers' health and emotional well-being is key to maintaining essential services, now more than ever, as the daunting COVID-19 outbreak stresses workers.
Data accessibility statement
The authors confirm that the data supporting the findings of this study are available within the article. Raw data were generated at Mind Garden Inc [10]. Derived data supporting the findings of this study are available from the corresponding author on request.
Implications for practice
The PEPS allows front-line clinicians to quickly express their immediate concerns and provides leaders with insights into the issues that must be addressed to ensure long-term success as the pandemic evolves. This manuscript is not under consideration for publication elsewhere. The main author is responsible for the integrity of the work. There are no other authors. A copy has been submitted as a preprint to Research Square.
DOI: 10.21203/rs.3.rs-43360/v1
Conflict of interest statement
None
Acknowledgments
None
Funding
None
Role of the funding source
None
Clinical trial registration
None
What we already know
- The health and safety of radiographers, radiologists, allied professionals, patients and health care workers are of primary importance during the COVID-19 outbreak.
- To help radiology professionals make more informed decisions during the pandemic of COVID -19 information in the form of experiences have to be viewed and reported for others to benefit.
What this article adds
- The PEPS allows front-line clinicians to quickly express their immediate concerns.
- It provides leaders with insights into the issues that must be addressed to ensure long-term success as the pandemic evolves.
- It allows for preparedness in the case of future outbreaks.
References
- Occupational Safety and Health Administration (OSHA). Guidance on preparing workplaces for COVID-19. US Department of Labor (2020).
- Chersich MF, Gray G, Fairlie L, et al. COVID-19 in Africa: care and protection for frontline healthcare workers. Global Health 16 (2020): 46.
- Zhang M, Zhou M, Tang F, et al. Knowledge, attitude, and practice regarding COVID-19 among healthcare workers in Henan, China. J Hosp Infect 105 (2020): 183-187.
- Flor N, Dore R, Sardanelli F. On the role of chest radiography and CT in the coronavirus disease (COVID-19) pandemic. AJR Am J Roentgenol 215 (2020): 44.
- Kooraki S, Hosseiny M, Myers L, et al. Coronavirus (COVID-19) outbreak: what the department of radiology should know. J Am Coll Radiol 17 (2020): 447-451.
- Stevens BJ. Reporting radiographers' interpretation and use of the British Society of Thoracic Imaging's coding system when reporting COVID-19 chest x-rays. Radiography 27 (2021): 90-94.
- Yurdaisik I, Nurili F. Evaluation of chest CT findings in 50 coronavirus disease 2019 (COVID-19) patients treated in Turkey. Cureus 12 (2020): 8252.
- Sim WY, Chen RC, Aw LP, et al. How to safely and sustainably reorganise a large general radiography service facing the COVID-19 pandemic. Radiography 26 (2020): 303-311.
- Bhagavathula AS, Aldhaleei WA, Rahmani J, et al. Knowledge and perceptions of COVID-19 among health care workers: cross-sectional study. JMIR Public Health Surveill 6 (2020): 19160.
- Leiter M. The Pandemic Experiences and Perceptions Survey (PEPS). Group Report. Menlo Park, CA: Mind Garden Inc (2020).
- Kuwait Ministry of Health. Labor Force Statistics. Kuwait: State of Kuwait - Ministry of Health. (2020).
- Food and Drug Administration Staff. Enforcement policy for imaging systems during the coronavirus disease 2019 (COVID-19) public health emergency. Guidance for industry and food and drug administration staff. Rockville: U.S. Department of Health and Human Services Food and Drug Administration Center for Devices and Radiological Health (CDRH), Office of Product Evaluation and Quality (OPEQ) (2020).
- Stogiannos N, Fotopoulos D, Woznitza N, et al. COVID-19 in the radiology department: what radiographers need to know. Radiography 26 (2020): 254-263.
- Mohakud S, Ranjan A, Naik S, et al. COVID-19 preparedness for portable X-rays in an Indian hospital - safety of the radiographers, the frontline warriors. Radiography 26 (2020): 270-271.
- Elshami W, Elamrdi A, Alyafie S, et al. Continuing professional development in radiography: practice, attitude and barriers. Int J Med Res Health Sci 5 (2016): 68-73.
- Roy D, Tripathy S, Kar SK, et al. Study of knowledge, attitude, anxiety & perceived mental healthcare need in Indian population during COVID-19 pandemic. Asian J Psychiatr 51 (2020): 102083.
- Johnson EJ, Hariharan S. Public health awareness: knowledge, attitude and behaviour of the general public on health risks during the H1N1 influenza pandemic. J Public Health 25 (2017): 333-337.
- Mishra P, Bhadauria US, Dasar PL, et al. Knowledge,attitude and anxiety towards pandemic flu a potential bio weapon among health professionals in Indore city. Przegl Epidemiol 70 (2016): 41-45.
- Abebe TB, Bhagavathula AS, Tefera YG, et al. Healthcare professionals' awareness, knowledge, attitudes, perceptions and beliefs about Ebola at Gondar University Hospital, Northwest Ethiopia: a cross-sectional study. J Public Health Afr 7 (2016): 570.
- Jemal B, Ferede ZA, Mola S, et al. Knowledge, attitude and practice of healthcare workers towards COVID-19 and its prevention in Ethiopia: a multicenter study. Res Sq (2020).
- Cowling C, Lawson C. Assessing the impact of country culture on the socio-cultural practice of radiography. Radiography 26 (2020): 223-228.