Manual Therapy Followed by Dynamic Strengthening Exercise Along With Conventional Physiotherapy Versus Manual Therapy Along With Conventional Physiotherapy on The Improvement of Pain and Functional Disability In Patients With Chronic Non-Specific Low Back Pain: A Randomized-Controlled Pilot Study
Article Information
Md Nazmul Hassan1*, Parvin Akter1, Mohammad Anwar Hossain2, Koushik Ahmed3, Farjana Sharmin4, Md Shahoriar Ahmed1, Kumar Amitav5, Md Ashif Ikbal khan5, Shazal Kumar Das6, Lori M. Walton7, Mohammad Habibur Rahman8
1Senior Clinical Physiotherapist, CRP, Savar, Dhaka, Bangladesh
2Senior Consultant Physiotherapist, CRP, Savar, Dhaka, Bangladesh
3Junior Consultant Physiotherapist, CRP, Savar, Dhaka, Bangladesh
4Consultant Physiotherapist, CRP, Savar, Dhaka, Bangladesh
5Clinical Physiotherapist, CRP, Savar, Dhaka, Bangladesh
6Lecturer, Department of Physiotherapy, BHPI, Savar, Dhaka
7Professor, Department of Physiotherapy, University of Scranton, PA, USA
8Assistant Professor, Open University, Dhaka, Bangladesh
Corresponding Author: Md Nazmul Hassan, Department of Physiotherapy, CRP, Savar, Dhaka-1343, Bangladesh.
Received: 05 September 2022; Accepted: 12 September 2022; Published: 22 September 2022
Citation: Md Nazmul Hassan, Parvin Akter, Mohammad Anwar Hossain, Koushik Ahmed, Farjana Sharmin, Md Shahoriar Ahmed, Kumar Amitav, Md Ashif Ikbal khan, Shazal Kumar Das, Lori M. Walton, Mohammad Habibur Rahman. Manual therapy followed by dynamic strengthening exercise along with conventional physiotherapy versus manual therapy along with conventional physiotherapy on the improvement of pain and functional disability in patients with chronic non-specific low back pain: a randomized-controlled pilot study. Journal of Surgery and Research 4(3) (2022): 104-110
View / Download Pdf Share at FacebookAbstract
Chronic low back pain (LBP), defined as back pain persisting for more than 12 weeks, affects over 50% of the general population.[1] It is the second most common factor for patients in search of primary care services.[2]According to the US National Center for Health Statistics, 14% of new patients admitted to a hospital for treatment had low back pain, representing 13 million people.[3] Also, it is estimated that over 70% of adults have had at least one episode of LBP in their lifetime.[4]In 2007, another study revealed that lower back region pain is caused by disc degeneration, spondylolisthesis, lumbar stenosis, epidural hematoma, and other causes, and 3% of all patients discharged from hospitals have symptomatic low back pain.[5] Because the causes of LBP are variable, different exercise regimens have been used to treat patients, including lumbar flexion, extension, isometric flexion, passive extension, and intensive dynamic back exercise regimens, and many of these exercise regimens have not yielded satisfactory results.[6]Recently, some studies have focused on exercises that aim to maintain or improve lumbar spine stability, such as lumbar stabilization exercises, which are aimed at improving the neuromuscular control, strength, and endurance of the muscles that are fundamental to maintaining spinal and trunk stability through several groups of muscles, particularly transverse abdominis and lumbar multifidi, but also other paraspinal, abdominal, diaphragmatic, and pelvic muscles.[7] Unsubstantiated suggestions that stabilization training may be useful in reducing pain and disability for all patients with nonspecific LBP, have appeared in the literature,[8] but these assertions have not been definitively demonstrated. Weakness of the abdominal muscles among the trunk muscles of low back pain patients is generally prevalent, and the strengthening of the abdominal muscles is essential in the recovery of the spinal neutral position.[9] When imbalance between the
Keywords
CLBP; Gradual Back Strengthening Exercise; Dynamic Back strengthening exercise
CLBP articles CLBP Research articles CLBP review articles CLBP PubMed articles CLBP PubMed Central articles CLBP 2023 articles CLBP 2024 articles CLBP Scopus articles CLBP impact factor journals CLBP Scopus journals CLBP PubMed journals CLBP medical journals CLBP free journals CLBP best journals CLBP top journals CLBP free medical journals CLBP famous journals CLBP Google Scholar indexed journals Gradual Back Strengthening Exercise articles Gradual Back Strengthening Exercise Research articles Gradual Back Strengthening Exercise review articles Gradual Back Strengthening Exercise PubMed articles Gradual Back Strengthening Exercise PubMed Central articles Gradual Back Strengthening Exercise 2023 articles Gradual Back Strengthening Exercise 2024 articles Gradual Back Strengthening Exercise Scopus articles Gradual Back Strengthening Exercise impact factor journals Gradual Back Strengthening Exercise Scopus journals Gradual Back Strengthening Exercise PubMed journals Gradual Back Strengthening Exercise medical journals Gradual Back Strengthening Exercise free journals Gradual Back Strengthening Exercise best journals Gradual Back Strengthening Exercise top journals Gradual Back Strengthening Exercise free medical journals Gradual Back Strengthening Exercise famous journals Gradual Back Strengthening Exercise Google Scholar indexed journals Dynamic Back strengthening exercise articles Dynamic Back strengthening exercise Research articles Dynamic Back strengthening exercise review articles Dynamic Back strengthening exercise PubMed articles Dynamic Back strengthening exercise PubMed Central articles Dynamic Back strengthening exercise 2023 articles Dynamic Back strengthening exercise 2024 articles Dynamic Back strengthening exercise Scopus articles Dynamic Back strengthening exercise impact factor journals Dynamic Back strengthening exercise Scopus journals Dynamic Back strengthening exercise PubMed journals Dynamic Back strengthening exercise medical journals Dynamic Back strengthening exercise free journals Dynamic Back strengthening exercise best journals Dynamic Back strengthening exercise top journals Dynamic Back strengthening exercise free medical journals Dynamic Back strengthening exercise famous journals Dynamic Back strengthening exercise Google Scholar indexed journals low back pain articles low back pain Research articles low back pain review articles low back pain PubMed articles low back pain PubMed Central articles low back pain 2023 articles low back pain 2024 articles low back pain Scopus articles low back pain impact factor journals low back pain Scopus journals low back pain PubMed journals low back pain medical journals low back pain free journals low back pain best journals low back pain top journals low back pain free medical journals low back pain famous journals low back pain Google Scholar indexed journals disc degeneration articles disc degeneration Research articles disc degeneration review articles disc degeneration PubMed articles disc degeneration PubMed Central articles disc degeneration 2023 articles disc degeneration 2024 articles disc degeneration Scopus articles disc degeneration impact factor journals disc degeneration Scopus journals disc degeneration PubMed journals disc degeneration medical journals disc degeneration free journals disc degeneration best journals disc degeneration top journals disc degeneration free medical journals disc degeneration famous journals disc degeneration Google Scholar indexed journals spondylolisthesis articles spondylolisthesis Research articles spondylolisthesis review articles spondylolisthesis PubMed articles spondylolisthesis PubMed Central articles spondylolisthesis 2023 articles spondylolisthesis 2024 articles spondylolisthesis Scopus articles spondylolisthesis impact factor journals spondylolisthesis Scopus journals spondylolisthesis PubMed journals spondylolisthesis medical journals spondylolisthesis free journals spondylolisthesis best journals spondylolisthesis top journals spondylolisthesis free medical journals spondylolisthesis famous journals spondylolisthesis Google Scholar indexed journals lumbar stenosis articles lumbar stenosis Research articles lumbar stenosis review articles lumbar stenosis PubMed articles lumbar stenosis PubMed Central articles lumbar stenosis 2023 articles lumbar stenosis 2024 articles lumbar stenosis Scopus articles lumbar stenosis impact factor journals lumbar stenosis Scopus journals lumbar stenosis PubMed journals lumbar stenosis medical journals lumbar stenosis free journals lumbar stenosis best journals lumbar stenosis top journals lumbar stenosis free medical journals lumbar stenosis famous journals lumbar stenosis Google Scholar indexed journals epidural hematoma articles epidural hematoma Research articles epidural hematoma review articles epidural hematoma PubMed articles epidural hematoma PubMed Central articles epidural hematoma 2023 articles epidural hematoma 2024 articles epidural hematoma Scopus articles epidural hematoma impact factor journals epidural hematoma Scopus journals epidural hematoma PubMed journals epidural hematoma medical journals epidural hematoma free journals epidural hematoma best journals epidural hematoma top journals epidural hematoma free medical journals epidural hematoma famous journals epidural hematoma Google Scholar indexed journals paraspinal articles paraspinal Research articles paraspinal review articles paraspinal PubMed articles paraspinal PubMed Central articles paraspinal 2023 articles paraspinal 2024 articles paraspinal Scopus articles paraspinal impact factor journals paraspinal Scopus journals paraspinal PubMed journals paraspinal medical journals paraspinal free journals paraspinal best journals paraspinal top journals paraspinal free medical journals paraspinal famous journals paraspinal Google Scholar indexed journals pelvic muscles articles pelvic muscles Research articles pelvic muscles review articles pelvic muscles PubMed articles pelvic muscles PubMed Central articles pelvic muscles 2023 articles pelvic muscles 2024 articles pelvic muscles Scopus articles pelvic muscles impact factor journals pelvic muscles Scopus journals pelvic muscles PubMed journals pelvic muscles medical journals pelvic muscles free journals pelvic muscles best journals pelvic muscles top journals pelvic muscles free medical journals pelvic muscles famous journals pelvic muscles Google Scholar indexed journals
Article Details
Background
Chronic low back pain (LBP), defined as back pain persisting for more than 12 weeks, affects over 50% of the general population.[1] It is the second most common factor for patients in search of primary care services.[2]According to the US National Center for Health Statistics, 14% of new patients admitted to a hospital for treatment had low back pain, representing 13 million people.[3] Also, it is estimated that over 70% of adults have had at least one episode of LBP in their lifetime.[4]In 2007, another study revealed that lower back region pain is caused by disc degeneration, spondylolisthesis, lumbar stenosis, epidural hematoma, and other causes, and 3% of all patients discharged from hospitals have symptomatic low back pain.[5] Because the causes of LBP are variable, different exercise regimens have been used to treat patients, including lumbar flexion, extension, isometric flexion, passive extension, and intensive dynamic back exercise regimens, and many of these exercise regimens have not yielded satisfactory results.[6]Recently, some studies have focused on exercises that aim to maintain or improve lumbar spine stability, such as lumbar stabilization exercises, which are aimed at improving the neuromuscular control, strength, and endurance of the muscles that are fundamental to maintaining spinal and trunk stability through several groups of muscles, particularly transverse abdominis and lumbar multifidi, but also other paraspinal, abdominal, diaphragmatic, and pelvic muscles.[7] Unsubstantiated suggestions that stabilization training may be useful in reducing pain and disability for all patients with nonspecific LBP, have appeared in the literature,[8] but these assertions have not been definitively demonstrated. Weakness of the abdominal muscles among the trunk muscles of low back pain patients is generally prevalent, and the strengthening of the abdominal muscles is essential in the recovery of the spinal neutral position.[9] When imbalance between the abdominal muscles of the trunk and extensor muscles occurs, it triggers slow back pain and reduces stabilization of the lumbar.[10]The ability to actively control the muscles of the hip plays an important part in lumbar segmental stability. If the sacroiliac joint moves excessively, it results in pressure on the joints and disks between the L5–S1 vertebral body, sacroiliac joint, and pubic symphysis, which leads to functional failure of the sacroiliac joint and low back pain. This causes the gluteus maximus muscle to contract, creating a self-locking mechanism, thereby providing stability to the sacroiliac joint.[11]There are various forms of exercise that can be prescribed based on different schools of thought, which include intensive dynamic back extensor exercises (motor control exercises), yoga and aerobic exercises.[12]Graded strengthening exercises are aimed at improving the neuromuscular control, strength, and endurance of the muscles that are central to maintaining dynamic spinal and trunk stability. The effect of graded lumbar stabilization exercises has been studied in subjects with recurrent LBP (8). Dynamic strengthening exercises can strengthen the spinal column and supporting structures.[13] An electromyography study to compare recruitment of the rectus abdominis and erector spinae muscles during dynamic strengthening exercise revealed higher muscle activity in these muscles.[14]Therefore, the aim of this study is to compare the effects of graded lumbar strengthening exercises and lumbar dynamic strengthening exercises on the maximal isometric contraction strength of the lumbar extensors, pain severity, and functional disability in patients with nonspecific chronic LBP. According to many studies, the first step of the physiotherapy treatment pyramid is education of the patient.[15] In another study, researchers explored several research studies that included evidence on conservative treatments,[16] which included manual therapy or conservative physiotherapy, which included exercises, mobilization, McKenzie approach treatment, manipulation, strengthening programs, advice, and other manual therapy techniques, which have strong evidence of effectiveness for chronic low back pain patients.[17] According to a study,[18] rest and exercise are effective for low back pain patients.
Patients and Methods
Study design and study population
This study was an experimental design of quantitative research, which was a randomized clinical trial (RCT), chosen because the experimental study is the best way to find out the effectiveness of any study. The researcher wished to conduct the study with an experimental group and a control group with the aim of comparing the experimental group and the control group. It was a double-blind study where the assessor and participants were blinded. Data was collected randomly from the outpatient, Musculoskeletal Physiotherapy unit of the Centre for the Rehabilitation of the Paralyzed (CRP), Savar. The duration of the study was from October 2021 to December 2021.
The researcher has taken eight participants as a sample. Obviously, this is a small sample as part of a pilot study. The researcher has to choose eight participants to conduct this study.
Intervention
The experimental group participants were received dynamic strengthening exercise with conventional physiotherapy treatment. The treatment was given according to patient’s condition and dynamic back strengthening also given as the home advice. In control group participants were given conventional physiotherapy treatment. Both group received physiotherapy treatment three days in a week. Treatment has given by five professional physiotherapists who were registered in Bangladesh.
Experimental group comprises of Conventional physiotherapy interventions & Dynamic strengthening exercise. The exercise program consisted of twelve sessions, each lasting half an hour, spread out over four weeks. The program was similar to the core strengthening exercises aimed at all the back muscle groups. The overall aim was to accelerate and enrich rehabilitation protocol of the spine. No special equipment was needed. Although, conventional physiotherapy approach continued along with the program.
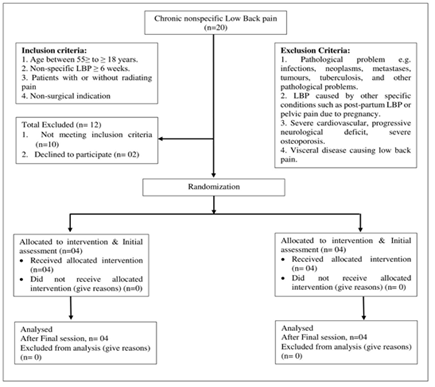
Figure 1: Strobe diagram
Data collection procedure
Result
The result found that, among the participants, ages ranged between 25 and 55, with a mean age of 41.12 years (32 years in the experimental group and 50.25 years in the control group). Males made up 62.5 percent (n=5) of all participants (37.5% in the experimental group and 25% in the control group), while females made up 37.5 percent (n=3) of all participants (12.5% in the experimental group and 25% in the control group).Among the participants, 37.5% (n=3) were housewives (12.5% in the experimental group and 25% in the control group), 25% (n=2) were businessmen (12.5% in the experimental group and 12.5% in the control group), and 37.5% (n=3) were the others. In this study, among the 08 participants, 62.5% (n=5) have completed secondary studies (25% in the experimental group and 37.5% in the control group), 25% (n=2) have completed graduation and further studies (they are in the experimental group), and 12.5% (n=1) have completed primary (in the control group).
|
Experimental Group |
Control Group |
|||
|
Mean with SD |
Min.-Max. |
Mean with SD |
Min.-Max. |
|
|
Age (yrs.) |
32 (±5.715) |
25-38 |
50.25 (±5.5) |
45-55 |
|
Height of the patient (inches) |
65 (±6) |
56-68 |
62.75 (±4.031) |
57-66 |
|
Weight of the Patient (kg) |
63.25 (±4.272) |
58-68 |
64 (±4.83) |
60-71 |
|
Initial |
Final |
Initial |
Final |
|
|
ODI |
43.50 (±17.464) |
42.50 (±18.574) |
61.50 (±26.096) |
61.00 (±25.534) |
Table 1: Baseline Data
|
Mann-Whitney U |
Asymp. Sig. (2-tailed) |
|
|
Pain-post |
5 |
0.386 |
|
Pain at night- post |
5.5 |
0.468 |
|
Interfere with lifestyle- post |
5 |
0.386 |
|
Pain severity at forward bending activity- post |
7 |
0.773 |
|
Back Stiffness- post |
8 |
1 |
|
Interfere with Walking- post |
6 |
0.564 |
|
Hurt when Walking- post |
4 |
0.248 |
|
Pain keep from standing still- post |
5 |
0.386 |
|
Pain keep from twisting- post |
7.5 |
0.885 |
|
Sit in upright hard chair- post |
7.5 |
0.885 |
|
Sit in soft arm chair- post |
6 |
0.564 |
|
Pain in lying- post |
3 |
0.149 |
|
Pain limit normal lifestyle- post |
6 |
0.564 |
|
Interfere with work- post |
7.5 |
0.885 |
|
Change of workplace- post |
8 |
1 |
|
Oswestry Disability Index- post |
4 |
0.248 |
Table 2: Between group test statistics
In case of between group statistics, as the data are not normally distributed and the sample size is very small, researcher has applied Mann-Whitney ‘U’ test statistics. From the above mentioned chart, the calculated value of ‘U’ at 5% level of significance are less than critical value of ‘U’ and ‘p’ value of the test statistics is larger than the 0.05 which indicate that the null hypotheses may be accepted. We may come to conclusion that there is no significance difference in between group analysis for all traits of Dallas pain questionnaire and Oswestry disability questionnaire.
|
Conventional Group |
Interventional Group |
||||
|
Z |
Asymp. Sig. (2-tailed) |
Z |
Asymp. Sig. (2-tailed) |
||
|
Pain-Day post - Pain-Day pre |
-1.461a |
0.144 |
-1.826a |
0.068 |
|
|
Pain at night-Day post - Pain at night-Day 1 |
-1.069a |
0.285 |
-1.342a |
0.18 |
|
|
Interfere with lifestyle-Day post - Interfere with lifestyle-Day pre |
.000b |
1 |
-1.604a |
0.109 |
|
|
Pain severity at forward bending activity-Day post - Pain severity at forward bending activity-Day pre |
-.730a |
0.465 |
-1.289a |
0.197 |
|
|
Interfere with Walking-Day post - Interfere with Walking-Day pre |
-1.826a |
0.068 |
-1.095a |
0.273 |
|
|
Hurt when Walking-Day post - Hurt when Walking-Day pre |
-1.841a |
0.066 |
-1.105a |
0.269 |
|
|
Pain keep from standing still-Day post - Pain keep from standing still-Day pre |
-1.826a |
0.068 |
-1.841a |
0.066 |
|
|
Pain keep from twisting-Day post - Pain keep from twisting-Initial-Day pre |
-1.069a |
0.285 |
-.184a |
0.854 |
|
|
Sit in upright hard chair-Day post - Sit in upright hard chair--Day pre |
-.730a |
0.465 |
-.447a |
0.655 |
|
|
Sit in soft arm chair-Day post - Sit in soft arm chair-Day pre |
-.535a |
0.593 |
-.736b |
0.461 |
|
|
Pain in lying-Day post - Pain in lying-Day pre |
-1.890a |
0.059 |
-.743b |
0.458 |
|
|
Pain limit normal lifestyle-Day post - Pain limit normal lifestyle-Day pre |
-1.826a |
0.068 |
-1.826a |
0.068 |
|
|
Interfere with work-Day post - Interfere with work-Day pre |
-1.289a |
0.197 |
-1.826a |
0.068 |
|
|
Change of workplace-Day post - Change of workplace-Day pre |
.000b |
1 |
.000c |
1 |
|
|
a. Based on positive ranks. |
a. Based on positive ranks. |
||||
|
b. The sum of negative ranks equals the sum of positive ranks. |
b. Based on negative ranks. |
||||
|
c. Wilcoxon Signed Ranks Test. |
c. The sum of negative ranks equals the sum of positive ranks. |
||||
|
d. Wilcoxon Signed Ranks Test |
|||||
Table 3: Within group test statistics
From the above mentioned chart, it has been revealed that there is no significance difference comparing the pre-post data within the groups at the 5% level of significance. That means, there is no significance improvement at within groups.
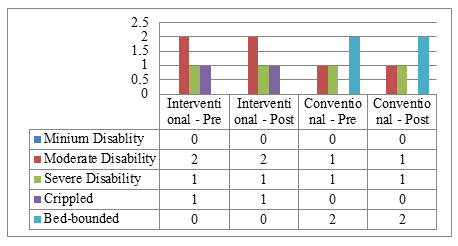
Figure 2: Disability among the participants
Discussion
The researcher tried to explore the effectiveness of the dynamic strengthening treatment approach for CLBP patients compared with conventional physiotherapy treatment. The different measurement tools were used to examine the hypothesis. A self-oriented structural questionnaire was used to find out the socio-demographical indicators. Different measures were recorded before and after treatment.
When it comes to between-group statistics, Mann-Whitney 'U' is the method of choice because the data is not normally distributed and the sample size is very small with a degree of freedom. From the data analysis, the observed value of "U" was less than the critical value of "U" and the level of significance was greater than p = > 0.05, which revealed that there was no significant difference in between-group analysis for all traits of the Dallas Pain Questionnaire and the Oswestry Disability Questionnaire.
In this study, 50% (n = 2) of the participants in the control group (n = 4) were bed-bound. On the other hand, in the experimental group (n = 4), 50% of the participants (n = 2) had moderate disability.
The Dallas pain scale was used to assess pain and discomfort in various working positions, such as general pain intensity, night pain intensity, pain interference with lifestyles, pain at forward-bending activity, back stiffness, interference with walking, pain with standing still, twisting activity, upright hard chair sitting, soft arm chair sitting, lying in bed, pain limiting normal life, pain interfering in work, and workplace change. Among these indicators, any one was not found statistically significant at a p value of 0.05% for the "Man Whitney "U" test. All of the domains did not show any significance statistically (p >.05).
In this study, the Oswestry disability index was used to evaluate the level of disability impacted by the CLBP subjects. According to the classification criteria determined by ODI, among the participants of the control group (n=4), 50% of the participants (n=2) had bed-bound disability. On the other hand, in the experimental group (n = 4), 50% of the participants (n = 2) had moderate disability. On the other hand, there were no participants with a bed-bound disability within the experimental group. Besides this, 50% of participants had severe disability in the initial assessment as well as in the final assessment. In this study, among the participants, the rate of mean disability was slightly higher within the control group. In the Oswestry low back pain disability questionnaire, both groups remained the same at p = 0.248%. From Wilcoxon Z statistics, it has been revealed that there is no significant difference when comparing the pre-post data within the groups at the 5% level of significance. That means there is no significant improvement within the groups.
The 10 sections of the ODI domains are: pain intensity, personal care, lifting, walking, sitting, standing, sleeping, sex life, social life, and traveling, which give an outline of disability (in percentage; %).[19] It was found that the mean disability for the control group was at a moderate level (38%) on the initial day and was also at a moderate level (22.4%) on the final day. On the other hand, the mean disability for the experimental group was at a severe level (45%) at the initial day and a moderate level (27.20%) after 8 sessions of treatment, where they found two patients with bed-bound disability (82% and 90%) and one patient with a crippled level of disability (72%) at the very first session within the experimental group, whilst only one patient was found with crippled disability (78%) within the control group.
Limitation
As a pilot study, Data was collected from only one clinical setting i.e. CRP at Savar; it can be influencing to the result. Besides, the time was very limited for conducting, so less number of participants were taken by following criteria. Also, Mean age of the conventional group along with level of disability were comparatively higher than the interventional group.
Conclusion
The results of this study have shown that the effectiveness of Dynamic Strengthening Exercise along with conventional physiotherapy was the same in comparison to the conventional physiotherapy treatment for patients with CLBP. In these limited sessions, it has been found that the strengthening program could be started earlier but not for all kinds of patients. As the disability level has been improved by both groups, so it can be introduced earlier with the patients. A complete study should be done with a larger sample size to find out the effectiveness of the dynamic strengthening exercise along with the conventional physiotherapy treatment approach for CLBP patients.
Conflict of interest:
- The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
- The authors whose names are listed as authors certify that they have NO affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
- I hereby disclose all of my conflicts of interest and other potentially conflicting interests, including specific financial interests and relationships and affiliations relevant to Journal of Spine and Surgery (eg, employment/affiliation, grants or funding, consultancies, honoraria, stock ownership or stock options, expert testimony, royalties, or patents filed, received, or pending). This applies to the past 5 years and the foreseeable future. I agree that I will disqualify myself from reviewing, editing, or participating in editorial decisions about Journal of Spine and Surgery submission that deals with a matter in which either I or a member of my immediate family (ie, my spouse, domestic partner, or minor children) have direct financial interest or a competing financial interest (eg, employment or affiliation, grants or funding, consultancies, honoraria, stock ownership or stock options, expert testimony, royalties, or patents filed, received, or pending).
References
- França F R, Burke T N, Caffaro R R, et al. Effects of muscular stretching and segmental stabilization on functional disability and pain in patients with chronic low back pain: a randomized, controlled trial. Journal of manipulative and physiological therapeutics 35 (2012): 279-285.
- Werneke M W, Hart D, Oliver D, et al. Prevalence of classification methods for patients with lumbar impairments using the McKenzie syndromes, pain pattern, manipulation, and stabilization clinical prediction rules. Journal of Manual & Manipulative Therapy 18 (2010): 197-204.
- Njomo D W. Factors Influencing Compliance with Mass Treatment in the National Programme for the Elimination of Lymphatic Filariasis in Kenya (Doctoral dissertation).
- Vasudevan J M, Smuck M, Fredericson M. Evaluation of the athlete with buttock pain. Current Sports Medicine Reports 11 (2012): 35-42.
- Bartynski W S, Petropoulou K A. The MR imaging features and clinical correlates in low back pain–related syndromes. Magnetic resonance imaging clinics of North America 15(2007):137-154.
- Arokoski J P, Valta T, Kankaanpää M, Airaksinen O. Activation of lumbar paraspinal and abdominal muscles during therapeutic exercises in chronic low back pain patients. Archives of physical medicine and rehabilitation 85 (2004): 823-832.
- Moon H J, Choi K H, Kim D H, et al. Effect of lumbar stabilization and dynamic lumbar strengthening exercises in patients with chronic low back pain. Annals of rehabilitation medicin 37 (2013): 110-117.
- Koumantakis G A, Watson P J, Oldham J A. Trunk muscle stabilization training plus general exercise versus general exercise only: randomized controlled trial of patients with recurrent low back pain. Physical therapy. 85 (2005): 209-225.
- Lee W, Lee Y, Gong W. The effect of lumbar strengthening exercise on pain and the cross-sectional area change of lumbar muscles. Journal of physical therapy science 23 (2011): 209-212.
- Silfies S P, Squillante D, Maurer P, et al. Trunk muscle recruitment patterns in specific chronic low back pain populations. Clinical biomechanics 20 (2005): 465-473.
- Jeong U C, Sim J H, Kim C Y, et al. The effects of gluteus muscle strengthening exercise and lumbar stabilization exercise on lumbar muscle strength and balance in chronic low back pain patients. Journal of physical therapy science 27 (2015): 3813-3816.
- Macedo L G, Maher C G, Latimer J, McAuley J H. Motor control exercise for persistent, nonspecific low back pain: a systematic review. Physical therapy 89 (2009): 9-25.
- Carpes F P, Reinehr F B, Mota C B. Effects of a program for trunk strength and stability on pain, low back and pelvis kinematics, and body balance: a pilot study. Journal of bodywork and movement therapies 12 (2008): 22-30.
- Comfort P, Pearson S J, Mather D. An electromyographical comparison of trunk muscle activity during isometric trunk and dynamic strengthening exercises. The Journal of Strength & Conditioning Research 25 (2011): 149-154.
- Menon A, Korner-Bitensky N, Kastner M, et al. Strategies for rehabilitation professionals to move evidence-based knowledge into practice: a systematic review. Database of Abstracts of Reviews of Effects (DARE): Quality-assessed Reviews [Internet]. 2009.
- Weinstein J N, Lurie J D, Tosteson T D, et al. Surgical versus non-operative treatment for lumbar disc herniation: four-year results for the Spine Patient Outcomes Research Trial (SPORT). Spine 33 (2008): 2789.
- Frode A O, Hoel N J. Manual therapy and exercise therapy in patients with chronic low back pain: a randomized, controlled trial with 1-year follow-up. Spine 28 (2003): 525-531.
- Koes BW, Van Tulder M, Lin CW, Macedo LG, McAuley J, Maher C. An updated overview of clinical guidelines for the management of non-specific low back pain in primary care. European Spine Journal 19 (2010): 2075-2094.
- Longo U G, Loppini M, Denaro L, Maffulli N, Denaro V. Rating scales for low back pain. British medical bulletin 94 (2010): 81-144.
