Left Subclavian Artery Aneurysm in a Child with Turner Syndrome: A Case Report
Article Information
María Alejandra Rodríguez Brilla1, Johnathon Trapp2, Monesha Gupta Malhotra3, Victor Bautista-Hernandez1*
1Division of Cardio-thoracic Surgery, William E. DeBakey. Department of Surgery. Baylor College of Medicine at Christus Children’s Hospital of San Antonio, Texas, USA
2University of the Incarnate Word School of Osteopathic Medicine, San Antonio, USA
3Department of Pediatric Cardiology. Baylor College of Medicine at Christus Children's Hospital of San Antonio, Texas, USA
*Corresponding Author: Victor Bautista-Hernandez, M.D., PhD, FEBCTS. Division of Cardio-thoracic Surgery, Michael E. DeBakey. Department of surgery. Baylor College of Medicine at Christus Children’s San Antonio, Texas, USA. 333 N Santa Rosa, San Antonio, Tx 78207, USA.
Received: 07 March 2024; Accepted: 14 March 2024; Published: 29 March 2024
Citation:
Maria Alejandra Rodriguez Brilla, Johnathon Trapp, Monesha Gupta Malhotra, Victor Bautista-Hernandez. Left Subclavian Artery Aneurysm in a Child with Turner Syndrome: A Case Report. Archives of Clinical and Medical Case Reports. 8 (2024): 66-68.
View / Download Pdf Share at FacebookAbstract
Turner syndrome is associated with congenital cardiac defects and vasculopathies in children, however association with a left subclavian artery aneurysm is extremely rare. We report a case of an 11-year-old girl with Turner syndrome and a left subclavian artery aneurysm. Aneurysmal repair was performed by exclusion and placement of a vascular Dacron graft from the distal left subclavian artery to the descending thoracic aorta. During the 10-month follow-up after surgery there is no evidence of aneurysmal recurrence, and the graft remains patent with no complications.
Keywords
<p>Left subclavian artery aneurysm; Turner syndrome; Vasculopathies</p>
Left subclavian artery aneurysm articles; Turner syndrome articles; Vasculopathies articles.
Breast Cancer articles Breast Cancer Research articles Breast Cancer review articles Breast Cancer PubMed articles Breast Cancer PubMed Central articles Breast Cancer 2023 articles Breast Cancer 2024 articles Breast Cancer Scopus articles Breast Cancer impact factor journals Breast Cancer Scopus journals Breast Cancer PubMed journals Breast Cancer medical journals Breast Cancer free journals Breast Cancer best journals Breast Cancer top journals Breast Cancer free medical journals Breast Cancer famous journals Breast Cancer Google Scholar indexed journals Left subclavian artery aneurysm articles Left subclavian artery aneurysm Research articles Left subclavian artery aneurysm review articles Left subclavian artery aneurysm PubMed articles Left subclavian artery aneurysm PubMed Central articles Left subclavian artery aneurysm 2023 articles Left subclavian artery aneurysm 2024 articles Left subclavian artery aneurysm Scopus articles Left subclavian artery aneurysm impact factor journals Left subclavian artery aneurysm Scopus journals Left subclavian artery aneurysm PubMed journals Left subclavian artery aneurysm medical journals Left subclavian artery aneurysm free journals Left subclavian artery aneurysm best journals Left subclavian artery aneurysm top journals Left subclavian artery aneurysm free medical journals Left subclavian artery aneurysm famous journals Left subclavian artery aneurysm Google Scholar indexed journals ultrasound articles ultrasound Research articles ultrasound review articles ultrasound PubMed articles ultrasound PubMed Central articles ultrasound 2023 articles ultrasound 2024 articles ultrasound Scopus articles ultrasound impact factor journals ultrasound Scopus journals ultrasound PubMed journals ultrasound medical journals ultrasound free journals ultrasound best journals ultrasound top journals ultrasound free medical journals ultrasound famous journals ultrasound Google Scholar indexed journals artery aneurysm articles artery aneurysm Research articles artery aneurysm review articles artery aneurysm PubMed articles artery aneurysm PubMed Central articles artery aneurysm 2023 articles artery aneurysm 2024 articles artery aneurysm Scopus articles artery aneurysm impact factor journals artery aneurysm Scopus journals artery aneurysm PubMed journals artery aneurysm medical journals artery aneurysm free journals artery aneurysm best journals artery aneurysm top journals artery aneurysm free medical journals artery aneurysm famous journals artery aneurysm Google Scholar indexed journals Turner syndrome articles Turner syndrome Research articles Turner syndrome review articles Turner syndrome PubMed articles Turner syndrome PubMed Central articles Turner syndrome 2023 articles Turner syndrome 2024 articles Turner syndrome Scopus articles Turner syndrome impact factor journals Turner syndrome Scopus journals Turner syndrome PubMed journals Turner syndrome medical journals Turner syndrome free journals Turner syndrome best journals Turner syndrome top journals Turner syndrome free medical journals Turner syndrome famous journals Turner syndrome Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals CT articles CT Research articles CT review articles CT PubMed articles CT PubMed Central articles CT 2023 articles CT 2024 articles CT Scopus articles CT impact factor journals CT Scopus journals CT PubMed journals CT medical journals CT free journals CT best journals CT top journals CT free medical journals CT famous journals CT Google Scholar indexed journals surgery articles surgery Research articles surgery review articles surgery PubMed articles surgery PubMed Central articles surgery 2023 articles surgery 2024 articles surgery Scopus articles surgery impact factor journals surgery Scopus journals surgery PubMed journals surgery medical journals surgery free journals surgery best journals surgery top journals surgery free medical journals surgery famous journals surgery Google Scholar indexed journals syndrome articles syndrome Research articles syndrome review articles syndrome PubMed articles syndrome PubMed Central articles syndrome 2023 articles syndrome 2024 articles syndrome Scopus articles syndrome impact factor journals syndrome Scopus journals syndrome PubMed journals syndrome medical journals syndrome free journals syndrome best journals syndrome top journals syndrome free medical journals syndrome famous journals syndrome Google Scholar indexed journals Vasculopathies articles Vasculopathies Research articles Vasculopathies review articles Vasculopathies PubMed articles Vasculopathies PubMed Central articles Vasculopathies 2023 articles Vasculopathies 2024 articles Vasculopathies Scopus articles Vasculopathies impact factor journals Vasculopathies Scopus journals Vasculopathies PubMed journals Vasculopathies medical journals Vasculopathies free journals Vasculopathies best journals Vasculopathies top journals Vasculopathies free medical journals Vasculopathies famous journals Vasculopathies Google Scholar indexed journals
Article Details
1. Introduction
Turner syndrome (TS), occurring approximately in 1 in 2500 live births, results from X chromosome deletion or non-functioning in females, presented as monosomy X (45,X0) or mosaicism (45,X) [1]. Cardiovascular abnormalities occur in 23 to 50% of patients with TS, representing the most frequent cause of early mortality, and include bicuspid aortic valve, aortic coarctation, and thoracic aortic aneurysms [2]. Medium caliber artery aneurysms in patients with TS are very rare, and have been described to affect the subclavian, celiac, and coronary arteries [2,3].
Subclavian artery aneurysms are usually asymptomatic, but can present as compressive symptoms, being the associated complications rupture, thrombosis, and upper extremity emboli [1,4]. Aneurysmal repair is indicated according to the size, progression of the aneurysm, history of connective tissue disorder, strong family history, and symptoms [5]. Treatment options encompass conservative management, open surgical repair, endovascular exclusion, and various hybrid techniques [4]. Location of the aneurysm in the aortic arch makes surgical approach more challenging. We describe the case of an elective thoracotomy for surgical repair of a left subclavian artery (LSA) aneurysm in a child with TS.
2. Case Summary
An 11-year-old girl with past medical history of TS (45X0) on growth hormone therapy, presented with palpitations and exercise intolerance, and on further evaluation was diagnosed with persistent left superior vena cava, absent right superior vena cava, and pseudocoarctation and tortuosity of the aorta with elongation of the transverse arch. A routine transthoracic echocardiogram demonstrated dilation of the LSA and was confirmed by Cardiac Computed Tomography Angiography (CCTA) as a LSA aneurysm at its origin from the aortic arch (Figure 1). The patient was started on oral betablocker therapy. A 5-month follow-up cardiac MRI was performed that revealed an enlarging LSA aneurysm, located at the take-off from the aortic arch, approximately 29 mm in length, maximum dimensions measured 24 mm x 24 mm (Figure 2).
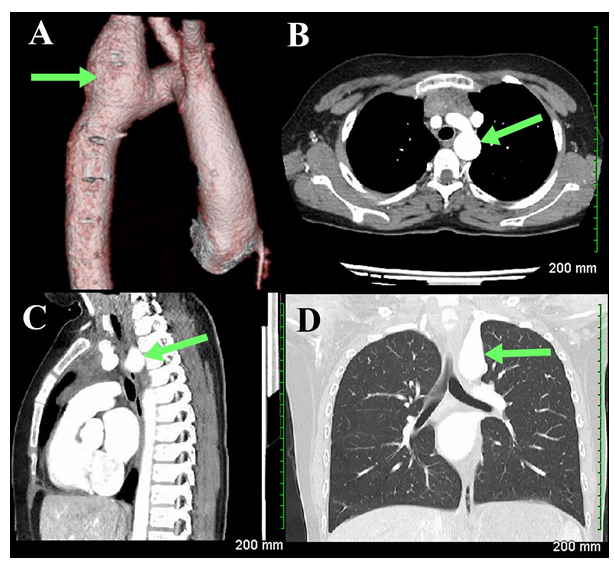
Figure 1: Cardiac Computed Tomography Angiography. Posterior view, 3D reconstruction of the aortic arch demonstrating (A) left subclavian artery aneurysm. Axial view showing (B) aneurysmal dilation at the base of left subclavian artery. Sagittal (C) and coronal (D) view showing left subclavian artery aneurysm at its origin from the aortic arch.
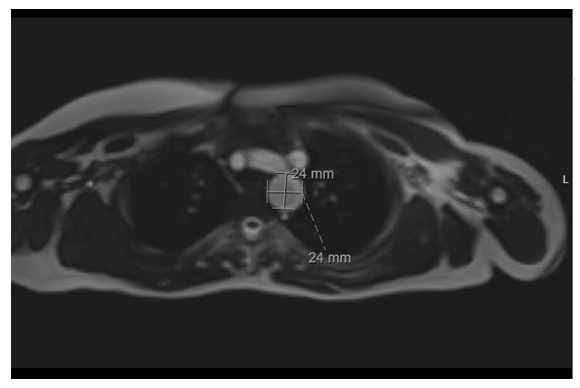
Figure 2: Magnetic Resonance Imaging. Axial view revealing an aneurysmal dilation of the left subclavian artery at its origin from the aortic arch measuring 24 x 24 mm.
The patient was evaluated from an endovascular standpoint and stent grafting was ruled out, considering the need to include the origin of the LSA in the landing zone, the specific vascular tissue abnormalities seen in TS patients, and the risk of restenting due to the child’s growth potential. Avoidance of cardio-pulmonary by-pass surgery with deep hypothermia was planned and thus, the patient underwent a left posterior thoracotomy for aneurysmal exclusion and repair. Vascular clamps were applied distally on the LSA, and partially on the descending thoracic aorta. The LSA was transected distal to the aneurysm and aneurysmal exclusion was achieved through 2 pledgeted purse-string sutures. Of note, a significant amount of abnormal lymphatic tissue was surrounding the aorta that was carefully cauterized. The LSA was reconstructed with an interposition Dacron graft (caliber 10 mm) from the distal LSA to the descending thoracic aorta. The patient’s recovery was uneventful, and she was discharged on post-operative day 5. During her 10-month follow-up she was asymptomatic, with a successful aneurysmal exclusion and a patent interposition graft observed on CCTA (Figure 3).
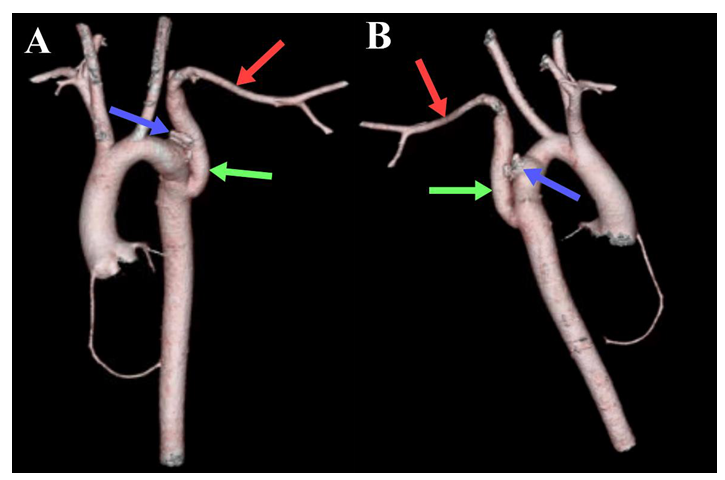
Figure 3: CCTA 3D reconstruction of the post-operative ascending aorta, aortic arch, descending aorta, and aortic branches. Anterior (A) and posterior view (B) demonstrating patent Dacron graft (green arrow) in the descending aorta anastomosing with the left subclavian artery (red arrow), and the resected aneurysm stump (blue arrow).
3. Discussion
LSA aneurysms in TS patients are extremely rare, only 4 cases have been reported in the literature being the youngest report from a 15-year-old patient [1,2,5,6]. The reported pathological findings of the aneurysmal tissue revealed elastic fibers dissociation by a mucopolysaccharide substance in the intima and media [2,6].
Proximal and mid-clavicular aneurysms have a higher incidence of rupture with associated mortality of 19% [4]. In TS there is more than 100-fold risk of acute aortic dissection in young and middle-aged patients, involving both the ascending and descending aorta, and being attributed to untreated aortic coarctations [2,7]. Aneurysmal repair is aimed to reduce the risk of compressive symptoms, distal embolization, and rupture [4].
In this case, surgical treatment was indicated considering aneurysmal dilation located in a major branch of the aorta involving the aortic arch, TS, and an increasing aneurysmal size overtime. Percutaneous Transfemoral Endovascular Aneurysmal Repair (TEVAR) was not recommended by reason of the anatomic location, the underlying syndrome leading to abnormal aortic tissue, and the expected growth of the child. Thus, resection and interposition vascular graft placement for enlarging LSA aneurysm repair was indicated.
Minimally invasive approach via left posterior thoracotomy was preferred over an anterior median sternotomy, which might have required because of the aortic arch location of the aneurysm, more invasive procedures including cardiopulmonary bypass, cross clamping of the aorta, selective cerebral perfusion vs circulatory arrest, and significant hypothermia. Aortic wall in patients with TS is thin, fragile, and easily torn [2]. Careful surgical dissection of the aorta and resection of the aneurysm was carried out, having especial precaution with the friable vascular tissue to prevent the risk of aortic laceration or massive hemorrhaging. Also, abnormal lymphatic tissue has been described in these patients with some of them developing chylothorax after surgical repair [8]. Therefore, careful cauterization of the surrounding abnormal lymphatic tissue should be performed.
We describe the case of an 11-year-old female with TS and a LSA aneurysm who underwent successful surgical treatment. Surgical exclusion for LSA aneurysm provided our patient with TS a durable repair, minimizing the potential life-threatening complications of this disease, and could be the treatment of choice for this challenging population.
Conflicts of interest
None
Funding
None
Declaration of interests
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
References
- Columbo J, Simons JP, Baril DT, Schanzer A. Management of a Patient with Turner Syndrome Presenting With an Isolated Left Subclavian Artery Aneurysm. Vasc Endovasc Surg 47 (2013): 397-399.
- Akasaka T, Mitsuishi T, Nakajima H, Suzuki R, Shimizu S. Aneurysm of the left subclavian artery associated with Turner's syndrome. Successful surgical treatment. J Cardiovasc Surg (Torino) 30 (1989): 945-947.
- Polkampally PR, Matta JR, McAreavey D, et al. Aneurysmal dilatation of medium caliber arteries in Turner syndrome. Congenit Heart Dis 6 (2011): 382-383.
- Vierhout BP, Zeebregts CJ, Van den Dungen JJAM, Reijnen MMPJ. Changing Profiles of Diagnostic and Treatment Options in Subclavian Artery Aneurysms. Eur J Vascu Endovasc Surg 40 (2010): 27-34.
- Hudson, Christopher CC, Jeremie S, Carole D, Tarek M, et al. Severe tracheobronchial compression in a patient with Turner′s syndrome undergoing repair of a complex aorto-subclavian aneurysm: Anesthesia perspectives. Annals of Cardiac Anaesthesia 17 (2014): 302-305.
- Lacombe M, Esteva B, Tillous-Borde I, Lesèche G. Anévrisme sous-clavier associé à un syndrome de Turner [Aneurism of the subclavian artery associated with Turner's syndrome]. Arch Pediatr 11 (2004): 344-346.
- Bondy C. Aortic Dissection in Turner Syndrome. Curr Opin Cardiol 23 (2008): 519–526.
- Chew JD, Hill KD, Jacobs ML, Jacobs JP, et al. Congenital Heart Surgery Outcomes in Turner Syndrome: The Society of Thoracic Surgeons Database Analysis. Thorac Surg 108 (2019): 1430-1438.
