Interdisciplinary Approach in Periodontology - A Mini-Review and A Report of Two Complex Cases
Article Information
Christina Doulkeridou1*, Ioannis Vouros1, Anastasios Petridis1, Zarkadi Athanasia-Eirini2, Charis Theodoridis1, 3
1Department of Preventive Dentistry, Periodontology and Implant Biology, Faculty of Dentistry, Aristotle University of Thessaloniki, Thessaloniki, Greece
2Post-Graduate Student of Public Health, European University Cyprus, Nicosia, Cyprus
3Cretan District Health Directorate, Agia Foteini Health Center, Rethymnon, Greece
*Corresponding Author: Christina Doulkeridou, Department of Preventive Dentistry, Periodontology and Implant Biology, Faculty of Dentistry, Aristotle University of Thessaloniki, Thessaloniki, Greece
Received: 05 July 2020; Accepted: 16 July 2020; Published: 20 July 2020
Citation: Christina Doulkeridou, Ioannis Vouros, Anastasios Petridis, Zarkadi Athanasia-Eirini, Charis Theodoridis. Interdisciplinary Approach in Periodontology - A Mini-Review and A Report of Two Complex Cases. Dental Research and Oral Health 3 (2020): 107-120.
View / Download Pdf Share at FacebookAbstract
Increasing life expectancy, higher quality of biomaterials used in dentistry and the rapid evolution of clinical procedures, has led to more demanding patient requests and more complicated treatment choices. Such complex cases require holistic management, which frequently mandates clinicians to cooperate in a multidisciplinary approach, in order to fulfil therapeutical objectives and to provide successful treatment concerning functional rehabilitation and aesthetical enhancement. Periodontology cannot be practised in isolation but has to be combined with other fields of dentistry, since periodontal diseases are quite prevalent and affect oral health in various ways. It is evident that these interactions and interrelationships between periodontology practice and other dental fields, such as endodontics, prosthodontics and orthodontics are quite crucial so as the utmost care to be delivered. Combined endodontic-periodontal lesions, adult orthodontics, especially in patients having been treated for periodontitis, prosthetic restoration and dental implant placement in patients with history of periodontitis are some challenging treatment modalities that may require interdisciplinary approach. In the first case reported, non-surgical as well as surgical periodontal treatment and periodontal health stabilization created the proper background for successful orthodontic treatment to be applied in a patient with severe chronic periodontitis. In the second case, periodontal therapy and surgical lengthening of the clinical crowns, with respect to biological width fundamentals, provided more favourable conditions in order a patient with alternative passive eruption and gummy smile to be restored prosthetically.
Keywords
<p>Interdisciplinary Approach, Multidisciplinary Periodontology, Periodontal Therapy, Alternative Passive Eruption, Periodontal Surgery</p>
Interdisciplinary Approach articles, Multidisciplinary Periodontology articles, Periodontal Therapy articles, Alternative Passive Eruption articles, Periodontal Surgery articles
Interdisciplinary Approach articles Interdisciplinary Approach Research articles Interdisciplinary Approach review articles Interdisciplinary Approach PubMed articles Interdisciplinary Approach PubMed Central articles Interdisciplinary Approach 2023 articles Interdisciplinary Approach 2024 articles Interdisciplinary Approach Scopus articles Interdisciplinary Approach impact factor journals Interdisciplinary Approach Scopus journals Interdisciplinary Approach PubMed journals Interdisciplinary Approach medical journals Interdisciplinary Approach free journals Interdisciplinary Approach best journals Interdisciplinary Approach top journals Interdisciplinary Approach free medical journals Interdisciplinary Approach famous journals Interdisciplinary Approach Google Scholar indexed journals Multidisciplinary Periodontology articles Multidisciplinary Periodontology Research articles Multidisciplinary Periodontology review articles Multidisciplinary Periodontology PubMed articles Multidisciplinary Periodontology PubMed Central articles Multidisciplinary Periodontology 2023 articles Multidisciplinary Periodontology 2024 articles Multidisciplinary Periodontology Scopus articles Multidisciplinary Periodontology impact factor journals Multidisciplinary Periodontology Scopus journals Multidisciplinary Periodontology PubMed journals Multidisciplinary Periodontology medical journals Multidisciplinary Periodontology free journals Multidisciplinary Periodontology best journals Multidisciplinary Periodontology top journals Multidisciplinary Periodontology free medical journals Multidisciplinary Periodontology famous journals Multidisciplinary Periodontology Google Scholar indexed journals Periodontal Therapy articles Periodontal Therapy Research articles Periodontal Therapy review articles Periodontal Therapy PubMed articles Periodontal Therapy PubMed Central articles Periodontal Therapy 2023 articles Periodontal Therapy 2024 articles Periodontal Therapy Scopus articles Periodontal Therapy impact factor journals Periodontal Therapy Scopus journals Periodontal Therapy PubMed journals Periodontal Therapy medical journals Periodontal Therapy free journals Periodontal Therapy best journals Periodontal Therapy top journals Periodontal Therapy free medical journals Periodontal Therapy famous journals Periodontal Therapy Google Scholar indexed journals Alternative Passive Eruption articles Alternative Passive Eruption Research articles Alternative Passive Eruption review articles Alternative Passive Eruption PubMed articles Alternative Passive Eruption PubMed Central articles Alternative Passive Eruption 2023 articles Alternative Passive Eruption 2024 articles Alternative Passive Eruption Scopus articles Alternative Passive Eruption impact factor journals Alternative Passive Eruption Scopus journals Alternative Passive Eruption PubMed journals Alternative Passive Eruption medical journals Alternative Passive Eruption free journals Alternative Passive Eruption best journals Alternative Passive Eruption top journals Alternative Passive Eruption free medical journals Alternative Passive Eruption famous journals Alternative Passive Eruption Google Scholar indexed journals Periodontal Surgery articles Periodontal Surgery Research articles Periodontal Surgery review articles Periodontal Surgery PubMed articles Periodontal Surgery PubMed Central articles Periodontal Surgery 2023 articles Periodontal Surgery 2024 articles Periodontal Surgery Scopus articles Periodontal Surgery impact factor journals Periodontal Surgery Scopus journals Periodontal Surgery PubMed journals Periodontal Surgery medical journals Periodontal Surgery free journals Periodontal Surgery best journals Periodontal Surgery top journals Periodontal Surgery free medical journals Periodontal Surgery famous journals Periodontal Surgery Google Scholar indexed journals periodontology articles periodontology Research articles periodontology review articles periodontology PubMed articles periodontology PubMed Central articles periodontology 2023 articles periodontology 2024 articles periodontology Scopus articles periodontology impact factor journals periodontology Scopus journals periodontology PubMed journals periodontology medical journals periodontology free journals periodontology best journals periodontology top journals periodontology free medical journals periodontology famous journals periodontology Google Scholar indexed journals orthodontics articles orthodontics Research articles orthodontics review articles orthodontics PubMed articles orthodontics PubMed Central articles orthodontics 2023 articles orthodontics 2024 articles orthodontics Scopus articles orthodontics impact factor journals orthodontics Scopus journals orthodontics PubMed journals orthodontics medical journals orthodontics free journals orthodontics best journals orthodontics top journals orthodontics free medical journals orthodontics famous journals orthodontics Google Scholar indexed journals
Article Details
1. Introduction
Increased life expectancy, as well as the rapidly progressing innovations in clinical procedures and biomaterials, have resulted in more complicated treatment modalities, which may incorporate various interventions that ought to combine functional needs with higher aesthetic requirements. Additionally, as population ageing advances, more and more medically compromised patients, such as cardiovascular patients [1], seek dental and periodontal care to reestablish their dentition and their holistic management may mandate clinicians to cooperate in order to encounter composite and complex challenges in a multidisciplinary approach including the combination of many medical and dental disciplines such as periodontics, orthodontics, endodontics and prosthodontics [2, 3]. A significant proportion of patients develop periodontitis, which undoubtedly affects both oral health and patients’ quality of life [4]. Nevertheless, periodontal approach is not practiced in isolation, since periodontal patients often face a plethora of other dental needs, which have to be considered with the trend for teeth to be retained or restored, functionally and aesthetically, with satisfactory longevity. Hence, interdisciplinary approach in Periodontology declares the interactions and interrelationship between periodontal tissues or periodontal diseases and other fields of dentistry such as endodontics, esthetic dentistry, fixed prosthodontics, orthodontics and implant dentistry [3]. Understanding these interrelationships can improve the clinicians’ ability to establish the correct diagnosis, to evaluate prognosis of the affected tooth or teeth and to design and carry out an appropriate treatment according to biological and clinical evidence [5].
1.1 Interdisciplinary approach in periodontology
Interaction between periodontology and endodontics is reported primarily because of the combined endodontic-periodontal lesions, which may be challenging concerning diagnosis and management. Communication between dental pulp and periodontium can be achieved by three avenues: exposed dentinal tubules, small portals of exit and the apical foramen. From apical foramen and/or the openings of the small portals of exit, the infected pulp elicits an inflammatory response in the periodontal structures [6]. On the other hand, it has been suggested that periodontal disease has no severe effect on the pulp, except the case that periodontal disease leads to advanced attachment loss, where lateral or accessory canals might be connected with the oral environment. When the apical foramen is affected, dental pulp may cause a chronic inflammatory reaction followed by pulp necrosis [7, 8]. Common pathogen profiles, from a microbiological perspective, have been detected in endodontic samples and also in teeth with chronic periodontitis. These pathogens have been considered to lead to pulp necrosis and inflammatory periapical lesion formation [9, 10]. Additional contributing factors, such as poor endodontic treatment or poor restoration, trauma, root resorption and dental malformations, which decrease treatment success rate, have been reported to influence the ecological balance between endodontium and surrounding periodontal tissues [11, 12, 13]. A classification for diagnosis and treatment of combined endo-perio lesions is suggested, and is divided into three categories: i) primary endodontic disease with secondary periodontal involvement, ii) primary periodontal disease with secondary endodontic involvement and iii) true combined diseases [5, 14]. Treatment prognosis depends primarily on the diagnosis of the specific category and two main factors are considered for appropriate decision-making: pulp vitality and type and extent of the periodontal defect [5, 15].
Given that orthodontic therapy in adults has been evolved into a frequent and predictable treatment opinion, many orthodontic patients present with a degree of periodontal disease or with a reduced periodontium on account of periodontitis history [16, 17]. It has also been suggested that adjunct orthodontic treatment may play an important role in developing of the optimal base needed for re-establishing an esthetic and functional dentition, especially in some cases with pathological migration or in cases where unfavorable tooth position cause remaining periodontal infection [16, 18]. Further indications of orthodontic interventions with regard to specific periodontal disease manifestations may be space closure and/or correction of excessively tipped molars, intrusion of elongated teeth and orthodontic extrusion for managing infra-osseous defects or augmenting soft and hard tissue around hopeless teeth before implant placement [19-23]. Interdisciplinary approach between periodontology and orthodontics needs to take special consideration on further bone loss prevention, which can lead to tooth loss or on malocclusion worsening. For these reasons, treatment modifications concerning mechanics and retention have to be considered for orthodontic patients with reduced periodontium [24]. Prior to treatment plan establishment, periodontal screening, appropriate medical history intake and clinical examination are mandatory so as primary diagnosis and initial treatment approach to be decided [25]. Periodontal therapy precedes orthodontics to ensure a healthy periodontal background with reduced pocket depths and absence of inflammatory signs and symptoms. In cases that residual deep pockets remain after initial non-surgical therapy, periodontal surgery, depending on the case requirements as well as on the anatomy of periodontal tissues (periodontal biotype, biological width), may be considered [4]. Regenerative periodontal surgery is suggested, when indicated, combined with patient’s compliance in oral health instructions [16, 26]. Orthodontic treatment can be considered after periodontal tissue healing [27] and orthodontic appliances must be placed carefully, in distance from subgingival environment, so as plaque development and periodontal inflammation relapse to be prevented [28, 29]. Orthodontic forces exerted on teeth with reduced periodontium require caution and in general an appropriate force system should be followed without heavy forces that may result in harmful periodontal response [17, 18].
Prosthetic restoration of missing or damaged dentition enhances patients’comfort, function, health and aesthetics and mandates periodontal health in order desired prosthetic rehabilitation longevity to be achieved [30]. Perio-Prostho interdisciplinary approach includes successive periodontal treatment and inflammation control as well as prosthetic restoration maintenance with regard to periodontal health in the long term. Prosthesis cleansability and biologic width (BW) are two crucial parameters that have to be considered when prosthodontic treatment planning and conduction is arranged. Prosthesis cleansability is influenced by prosthesis design, pontic morphology and patient’s compliance. BW is the physiologic dimension of the junctional epithelium and the connective tissue attachment and histologically, it is the combination of the averages of 1 mm of connective tissue attachment and 1 mm of epithelial attachment. Coronal to the biologic width is the gingival sulcus that is, on average, 0.69 mm [31, 32]. BW may vary in height and orientation around different teeth, based on gingival biotype and even around the same tooth, but it has been used as a guide for clinicians for decades. Fixed prostheses margin placement is suggested to follow gingival contour and not be extended more than 0,5mm into the sulcus. Otherwise gingival inflammation, attachment loss and gingival recession may be observed [33-37]. It is generally accepted among clinicians that a 3mm distance between alveolar crest and the restoration margin might significantly reduce the risk of periodontal attachment loss [35]. In the scope of the above, teeth with insufficient clinical crown height may be considered for surgical crown lengthening, aiming at creating a new gingival attachment complex and crown margins without violating BW. Apart from “functional” crown lengthening surgery, the same concept may be followed for aesthetic reasons, especially in the anterior sextants [38]. More specifically, a relatively common phenomenon that occurs in the population and affects smile aesthetics is the excess of gingival display, caused by altered passive eruption (APE) [39]. This condition is characterized by gingival overlapping over the enamel limits, resulting in a short clinical crown appearance that gives the sensation of hidden teeth and gummy smile, especially in the presence of a medium or a high lip line [38]. APE has been classified into two types, depending on the range of gingival margin, and into two subcategories according to the distance of alveolar crest from the cemento-enamel junction [40]. Based on this classification, the necessity of osteoplasty or osseous contour modification, with cementoenamel junction being used as a landmark, may be evaluated, when apically positioned flap is applied [41]. On the contrary, other cases may require additive methods, such as free gingival grafts, to correct gingival level and contour by augmenting the gingival tissues and reducing the height of the clinical crown [42]. In such cases the width of attached gingivae can be increased and dental hypersensitivity symptoms may be controlled [30]. Additional noteworthy factors that have to be considered in Perio-Prostho interdisciplinary approach are the preparation margin, with minimal marginal opening being more favorable, since it reduces the exposed cement line and subsequent leakage [43-45], the number and quality of abutment teeth, prosthesis material and patient factors such as compliance and expectations.
When dental implants are considered for partial edentulism management, history of periodontitis has to be assessed. Dental implants are frequently used in such cases [46, 47], nevertheless, peri-implant tissues are susceptible to similar host-modulated, plaque-induced factors that cause periodontal inflammation [51, 52]. It has been stated that residual pockets may act as niches of infection for dental implants and that putative periodontal pathogens are present even after infected teeth extractions [53, 54]. With regard to clinical studies, findings coming from well-designed and recent systematic reviews advocate a probable worsening in clinical outcomes, such as survival rates and marginal bone loss, of dental implants placed in patients with history of chronic or aggressive periodontitis [52, 53]. For all the plethora of existing clinical studies, there is no protocol homogeneity, especially in case definitions [54] and in methodological aspects, such as confounding factor control and follow up period comparability [53]. Although, history of periodontitis, even regarding the aggressive types, may not be considered an absolute contraindication for implant therapy, since dental implants can be recommended in patients successfully treated for both chronic and aggressive periodontitis [53], a supportive, preventative program for all patients, based on a risk assessment, is mandatory. During long term and individualized supportive therapy, patients should be encouraged to embrace strict compliance concerning plaque control and to regulate risk factors, such as smoking habits, which are common for both periodontal inflammation and peri-implantitis [54].
2. Case Reports
2.1 Case 1
A 45-year old female private tutor, with no reported medical conditions, presented with chronic generalized severe periodontitis and advanced bone loss, as diagnosed by clinical examination and periapical radiographs (Figure 1a). According to the latest “Classification of Periodontal and Peri-Implant Diseases and Conditions” in 2017, the patient’s periodontitis was evaluated as Stage III, Grade II [55]. Furthermore, the patient complained of occlusal disharmony, due to pathological migration and teeth spacing. Initial (stage I) treatment plan included: a) initial, non-surgical periodontal therapy, which comprised oral hygiene instructions, supra-gingival scaling and subgingival scaling and root planing, b) endodontic treatment in relation to teeth 16, 17, 46, c) extractions of teeth 14 and 45, with poor prognosis on account of excessive mobility, overdone bone loss and combined endo-perio lesions. After initial treatment plan completion and healing period of 12 weeks, stage II treatment included: a) periodontal surgery (access flap with osteoplasty, if needed) in sites, which after re-evaluation, presented with residual probing pocket depth ≥ 6 mm and simultaneous bleeding on probing, in order to gain access for further removal of the subgingival deposits (teeth 15-17, 23 and 37) b) buco-distal root extraction in tooth 17, c) clinical re-evaluation after 1, 3 and 6 months. One year after completion of stage II treatment and since periodontal health was achieved and maintained, the patient was considered for orthodontic treatment initiation (Figure 1b). The latter was completed after 2 years (Figure 1c) and a clinical and radiographical assessment was performed (figure 1d, 1e). The same clinical status, compatible with periodontal health, good functionality and satisfying aesthetics, is still maintained, with the last re-evaluation having been lately, 4 years after overall treatment completion (Figure 1f).
2.2 Case 2
A 65-year old female, medically healthy pensioner attended our private clinic, complaining for unattractive smile and decreased function concerning her anterior teeth. Clinical examination (Figure 2a) revealed intermediate wear of the incisal plane in both mandible and maxilla, resulting in insufficient teeth height, accompanied by an excessive gingival display since the gingival margin occupied a more incisal position. Additionally, the patient presented with slight to moderate localized periodontal lesions in posterior maxilla, according the AAP Classification in regards to severity [56, 57], and with advanced carious lesions in mandibular second molars, which were evaluated clinically and radiographically (Figure 2b). Eight weeks after mandibular second molar extractions and initial, non-surgical periodontal therapy, which included oral hygiene instructions, supra-gingival scaling and subgingival scaling and root planing, the patient presented with no periodontal pockets deeper than 3mm and with an adequate oral hygiene levels (full-mouth bleeding and plaque scores ≤ 10%). Anterior maxillary and mandibular manifestations were considered to be consistent with altered passive eruption and a gummy smile and hence, surgical lengthening of the clinical crowns prior to prosthetic restoration was suggested in order enhanced aesthetics to be fulfilled. According to Garber & Salama classification [40], the range of gingival margin was evaluated as sufficient and the distance of alveolar crest from the cemento-enamel junction was considered normal. Consequently, a conservative form of the apically positioned flap, without osteoplasty, was chosen and conducted in both maxillary (Figure 2c) and mandibular anterior region (Figure 2d). Post-operative conditions were monitored and assessed and crown preparation of the anterior teeth took place after 2 months of healing period (Figure 2e). Given the fact that final prosthetic treatment should initiate at least three months after surgery [38], provisional crowns were placed (Figure 2f), for an additional month, and afterwards final impression was considered. Figure 2g depicts the final prostheses just immediately after cementation. The patient chose not to have the posterior mandibular edentulism restored with implant supported restorations, due to financial considerations. Thus, the existing partial lower denture was suggested to be repaired and relined. This particular treatment choice was a compromised treatment plan based primarily on patient’s individualized desires so as not to proceed to dental implant therapy.
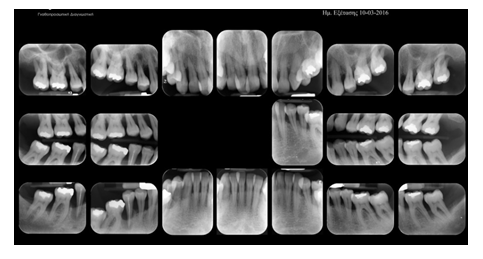
Figure 1a: Initial radiological screening with periapical radiographs.
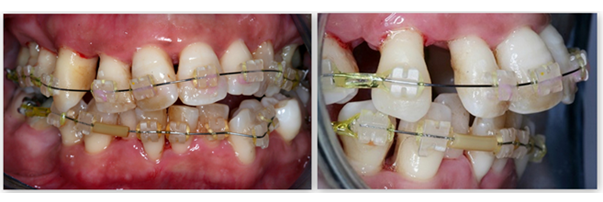
Figure 1b: Initiation of orthodontic treatment.
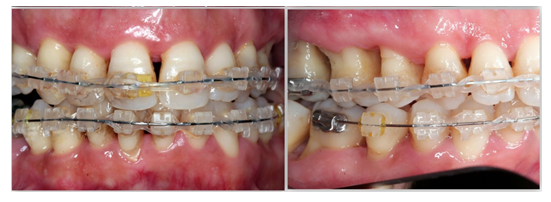
Figure 1c: Completion of orthodontic treatment.
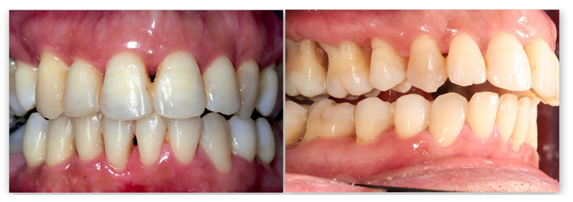
Figure 1d: Post-treatment clinical evaluation.
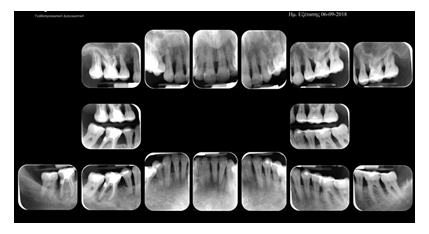
Figure 1e: Post-treatment radiological assessment with periapical radiographs.
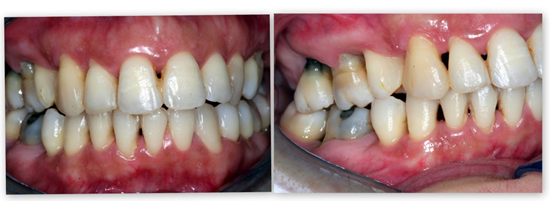
Figure 1f: Clinical evaluation, 4 years after overall treatment completion.
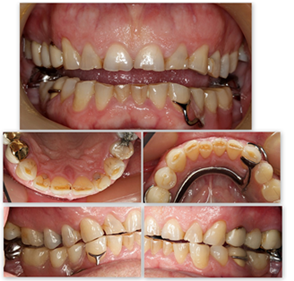
Figure 2a: Initial clinical assessment.
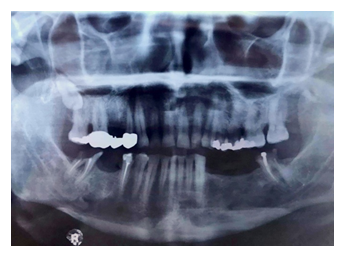
Figure 2b: Initial radiological screening with panoramic radiograph.
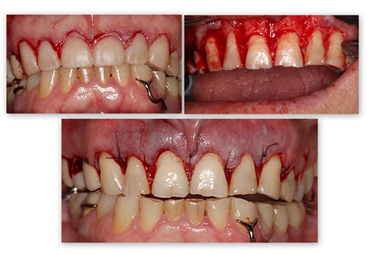
Figure 2c: Clinical crown surgical lengthening of the 6 anterior maxillary teeth.
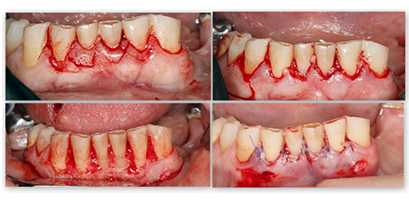
Figure 2d: Clinical crown surgical lengthening of the 4 anterior mandibular teeth.
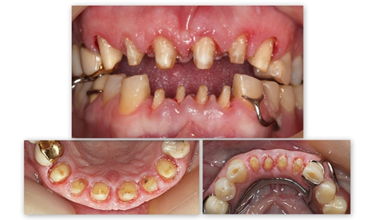
Figure 2e: Crown preparation for metal-ceramic prostheses.
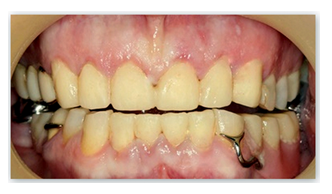
Figure 2f: Provisional crowns.
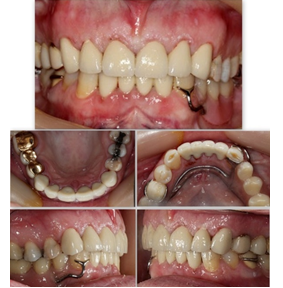
Figure 2g: Final prosthetic restorations after cementation.
3. Discussion
In order clinicians to fulfill the challenging and increased functional and aesthetic requirements that have arisen nowadays and to deliver satisfying therapeutical outcomes, they should consider embracing the interdisciplinary approach, especially when complex cases are being treated. This approach may be a challenging but rewarding way concerning dentistry practice and aims at offering the patient the utmost care [58]. From a periodontal point of view, contemporary treatment may incorporate various interventions, such as surgical periodontal therapy, soft tissue management/regeneration and bone augmentation procedures [59], which eventually are capable of preventing disease progression and enhance dentition longevity. Nevertheless, initial non-surgical periodontal treatment remains the “cornerstone” of therapy as it not only improves clinical parameters in the long term [60, 61] but it also inflicts a positive influence towards patient’s perception of treatment outcomes [4]. Surgical lengthening of the clinical crown is still considered a valuable treatment modality, often carried out, prior to fixed prosthodontics treatment and may enhance functional or aesthetic conditions in a variety of complex cases, such as caries, subgingival fractures or APE [37]. These techniques include gingivectomy, gingivoplasty and apically positioned flaps with or without osteoplasty. If the remaining, post-operative gingival width is less than 3 mm, apically positioned flap may be considered a more proper choice than merely gingivactomy [62, 63]. At any case, the clinical borderline of 3 mm supracrestal soft tissue has to be taken into consideration either in the prediction of post-operative gingival vertical position or when designing crown preparation margins in such cases. Severe bone loss and reduced periodontium may lead to additional manifestations, such as pathological migration, unfavorable tooth position or infrabony defects, which apparently cause occlusion disharmony and aesthetic concerns. These treatments may be complicated and time-consuming and therefore a “Perio-Ortho” multidisciplinary approach is often necessary [64] Adjunct orthodontic therapy may need some modifications when patients with history of periodontitis are being treated, which were previously presented more extensively. Periodontal health and absence of inflammatory signs and symptoms, prior to and during orthodontic treatment, may be considered the key-factor for predictable and successful clinical outcomes.
Disclosure Statement
The authors report no conflict of interest and that they did not receive any financial support for this study.
References
- Lillis T, Didagelos M, Lillis L, et al. Impact of Post-Exodontia Bleeding in Cardiovascular Patients: A New Classification Proposal. Open Cardiovasc Med J 11 (2017): 102-110.
- Deepa D, Mehta DS, Viren K Puri, et al. Combined periodontic-orthodonticendodontic interdisciplinary approach in the treatment of periodontally compromised tooth. J Indian Soc Periodontol 14 (2010): 139-143.
- Lyons M K, Darby I. Interdisciplinary periodontics: the multidisciplinary approach to the planning and treatment of complex cases. Periodontology 2000 74 (2017): 7-10.
- Theodoridis C, Violesti A, Nikiforidou M, et al. Short-Term Impact of Non-Surgical and Surgical Periodontal Therapy on Oral Health-Related Quality of Life in a Greek Population-A Prospective Cohort Study. Dent. J. 2020;8(2):54.
- Rotstein I. Interaction between endodontics and periodontics. Periodontology 2000 74 (2017): 11-39.
- Seltzer S, Bender IB, Nazimov H, et al. Pulpitis-induced interradicular periodontal changes in experimental animals. J Periodontol 38 (1967): 124-129.
- Czarnecki RT, Schilder H. A histological evaluation of the human pulp in teeth with varying degrees of periodontal disease. J Endod 5 (1979): 242-253.
- Langeland K, Rodrigues H, Dowden W. Periodontal disease, bacteria, and pulpal histopathology. Oral Surg Oral Med Oral Pathol 37 (1974): 257-270.
- Kakehashi S, Stanley HR, Fitzgerald RJ. The effects of surgical exposures of dental pulps in germ-free and conventional laboratory rats. Oral Surg Oral Med Oral Pathol 20 (1965): 340-349.
- Rupf S, Kannengiesser S, Merte K, et al. Comparison of profiles of key periodontal pathogens in periodontium and endodontium. Endod Dent Traumatol 16 (2000): 269-275.
- Saunders WP, Saunders EM. Coronal leakage as a cause of failure in root-canal therapy: a review. Endod Dent Traumatol 10 (1994): 105-108.
- Peters LB, Wesselink PR, Moorer WR. The fate and the role of bacteria left in root dentinal tubules. Int Endod J 28 (1995): 95-99.
- Simon JHS. Root extrusion-rationale and techniques. Dent Clin North Am 28 (1984): 909-921.
- Rotstein I, Simon JHS. The endo-perio lesion: a critical appraisal of the disease condition. Endod Topics 13 (2006): 34-56.
- Jansson L, Ehnevid H, Blomlof L, et al. Endodontic pathogens in periodontal disease augmentation. J Clin Periodontol 22 (1995): 598-602.
- Reichert C, Hagner M, Jepsen S, et al. Interfaces between orthodontic and periodontal treatment. J Orofac Orthop 72 (2011): 165-186.
- Antoun S J, Li Me I, Gibbs K, et al. Effect of orthodontic treatment on the periodontal tissues. Periodontology 2000 74 (2017): 140-157.
- Melsen B, Agerbaek N. Orthodontics as an adjunct to rehabilitation. Periodontol 2000 4 (1994): 148-159.
- Nasry HA, Barclay SC. Periodontal lesions associated with deep traumatic overbite. Br Dent J 200 (2006): 557-561.
- Reitan K. Tissue behavior during orthodontic tooth movement. Am J Orthod 46 (1960): 881-900.
- Ingber JS. Forced eruption. I. A method of treating isolated one and two wall infrabony osseous defects-rationale and case report. J Perio-dontol 45 (1974): 199-206.
- Brindis MA, Block MS. Orthodontic tooth extrusion to enhance soft tissue implant esthetics. J Oral Maxillofac Surg 67 (2009): 49-59.
- Zuccati G, Bocchieri A. Implant site development by orthodontic extrusion of teeth with poor prognosis. J Clin Orthod 37 (2003): 307-311.
- Handelman CS. Orthodontic care of the periodontally compromised patient followed long-term: Part I. Maximising favorable outcomes. World J Orthod 2 (2001): 127-141.
- Meyle J, Jepsen S. Der parodontale Screening-Index (PSI). Parodontologie 11 (2000): 17-21.
- Ramseier AC, Lang NP. Die Parodontalbet-reuungein Lernprogramm zur Qualitätssicherung in der Parodontologie (2007).
- Machtei EE. Outcome variables for the study of periodontal regeneration. Ann Periodontol 2 (1997): 229-239.
- Zachrisson BU. Gingival condition associated with orthodontic treatment. II. Histologic findings. Angle Orthod 42 (1972): 353-357.
- Zachrisson S, Zachrisson BU. Gingival condition associated with orthodontic treatment. Angle Orthod 42 (1972): 26-34.
- Abduo J, Lyons M. K. Interdisciplinary interface between fixed prosthodontics and periodontics. Periodontology 2000 74 (2017): 40-62.
- Gargiulo AW, Wentz FM, Orban B. Dimensions and relations of the dentogingival junction in humans. J Periodontol 32 (1961): 261-267.
- Vacek JS, Gher ME, Assad DA, Richardson AC, Giambarresi LI. The dimensions of the human dentogingival junction. Int J Periodontics Restorative Dent 14 (1994): 154-165.
- Kois JC. The restorative-periodontal interface: biological parameters. Periodontol 2000 11 (1996): 29-38.
- Carnevale G, Sterrantino SF, Di Febo G. Soft and hard tissue wound healing following tooth preparation to the alveolar crest. Int J Periodontics Restorative Dent 3 (1983): 36-53.
- Nevins M, Skurow HM. The intracrevicular restorative margin, the biologic width, and the maintenance of the gingival margin. Int J Periodontics Restorative Dent 4 (1984): 30-49.
- Flores-de-Jacoby L, Zafiropoulos GG, Ciancio S. Effect of crown margin location on plaque and periodontal health. Int J Periodontics Restorative Dent 9 (1989): 197-205.
- Silness J. Fixed prosthodontics and periodontal health. Dent Clin North Am 24 (1980): 317-329.
- Hempton TJ, Dominici JT. Contemporary crown-lengthening therapy: a review. J Am Dent Assoc 141 (2010): 647-655.
- Tjan AH, Miller GD, The JG. Some esthetic factors in a smile. J Prosth Dentistry 51 (1984): 24-28.
- Garber DA, Salama MA. The aesthetic smile: diagnosis and treatment. Periodontology 2000 11 (1996): 81-88.
- Camargo PM, Melnick PR, Pirih FQ, et al. Treatment of drug-induced gingival enlargement: aesthetic and functional considerations. Periodontol 2000 27 (2001): 131-138.
- Camargo PM, Melnick PR, Kenney EB. The use of free gingival grafts for aesthetic purposes. Periodontol 2000 27 (2001): 72-96.
- Byrne G. Influence of finish-line form on crown cementation. Int J Prosthodont 5 (1992): 137-144.
- Jacobs MS, Windeler AS. An investigation of dental luting cement solubility as a function of the marginal gap. J Prosthet Dent 65 (1991): 436-442.
- Padilla MT, Bailey JH. Margin configuration, die spacers, fitting of retainers/crowns, and soldering. Dent Clin North Am 36 (1992): 743-764.
- Ferreira S, Silva G, Cortelli J, et al. Prevalence and risk variables for peri-implant disease in Brazilian subjects. J Clin Periodontol 33 (2006): 929-993.
- Fransson C, Lekholm U, Jemt T, et al. Prevalence of subjects with progressive bone loss at implants. Clin OralImplants Res 16 (2005): 440-446.
- Leonhardt Å, Berglundh T, Ericsson I, et al. Putative periodontal and teeth in pathogens on titanium implants and teeth in experimental gingivitis and periodontitis in beagle dogs. Clin Oral Implants Res 3 (1992): 112-119.
- Zhuang LF, Watt RM, Mattheos N, et al. Periodontal and peri-implant microbiota in patients with healthy and inflamed periodontal and peri-implant tissues. Clin Oral Implants Res 27 (2016): 13-21.
- Mombelli A, Oosten M, Schürch E, et al. The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiol Immunol 2 (1987): 145-151.
- Sachdeo A, Haffajee AD, Socransky SS. Biofilms in the edentulous oral cavity. J Prosthodont 17 (2008): 348-356.
- Sousa V, Mardas N, Farias B, et al. A systematic review of implant outcomes in treated periodontitis patients. Clinical oral implants research (2015).
- Theodoridis C, Grigoriadis A, Menexes G, et al. Outcomes of implant therapy in patients with a history of aggressive periodontitis. A systematic review and meta-analysis. Clin Oral Investig 21 (2017): 485-503.
- Smith MM, Knight TE, Al-Harthi L, et al. Chronic periodontitis and implant dentistry. Periodontology 2000 74 (2017): 63-73.
- Caton JG, Armitage G, Berglundh T, et al. A new classification scheme for periodontal and peri-implant diseases and conditions Introduction and key changes from the 1999 classification. J Clin Periodontol 20 (2018): S1-S8.
- Armitage GC. Development of a classification system for periodontal diseases and conditions. Periodontol 4 (1999): 1-6.
- Armitage GC. Periodontal diagnoses and classification of periodontal diseases. Periodontol 2000 34 (2004): 9-21.
- Spear F. Forming an interdisciplinary team. J Am Dent Assoc 136 (2005): 1463-1464.
- Laurell L, Gottlow J, Zybutz M, et al. Treatment of infrabony defects by different surgical procedures. A literature review. J Periodontol 69 (1998): 303-313.
- Lindhe J, Westfelt E, Nyman S, et al. Long-term effect of surgical/non-surgical treatment of periodontal disease. J. Clin. Periodontol 11 (1984): 448-458.
- Isidor F, Karring T. Long-term effect of surgical and nonsurgical periodontal treatment. A 5 year clinical study. Periodontal Res 21 (1986): 462-472.
- Nabers CL. Repositioning the attached gingiva. J Periodontol 25 (1954): 38-39.
- Ariaudo A, Tyrrell HA. Repositioning and increasing the zone of attached gingiva. J Periodontol 28 (1957): 106-110.
- Cirelli JA, Cirelli CC, Holzhausen M, et al. Combined periodontal, orthodontic and restorative treatment of pathologic migration of anterior teeth. A case report. Int J Periodontics Restorative Dent 26 (2006): 501-506.
