Hyperpigmentation after Full Thickness Skin Grafts–A Case Report
Article Information
Staubach R*, Koehler P, Glosse H, Loff S
Klinikum Stuttgart/ Olgahospital, Department for Pediatric Surgery Kriegsbergstraße 60/62, 70174 Stuttgart, Germany
*Corresponding Author: Raphael Staubach, Klinikum Stuttgart/ Olgahospital, Department for Pediatric Surgery Kriegsbergstraße 60/62, 70174 Stuttgart, Germany
Received: 25 May 2023; Accepted: 12 June 2023; Published: 03 July 2023
Citation: Staubach R, Koehler P, Glosse H, Loff S. Hyperpigmentation after Full Thickness Skin Grafts–A Case Report. Archives of Clinical and Medical Case Reports. 7 (2023): 302-303.
View / Download Pdf Share at FacebookAbstract
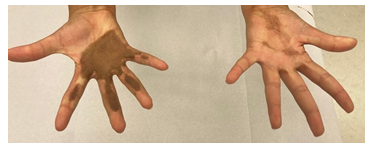
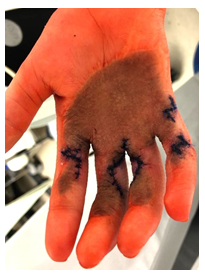
We report on an eight-year-old female patient of our department of pediatric surgery. In 2015 she was admitted to the emergency department at the age of one for burns she suffered from a barbecue accident. The admitting personnel were told that the child grabbed a piece of glowing charcoal with both hands burning a considerable part of her palms' and forearms' skin. The burnt surface showed partial blistering and made up approximately 1.5% of the child’s body surface. Primary treatment included covering with UrgoTul and Polyhexanide followed by a Suprathel skin substitution. Eighteen days after the accident a split thickness skin transplantation from the head to both palms was performed. Despite adequate wound healing supported by compression and extension therapy restrictive scarring occurred followed by a full thickness skin transplantation from the groin to the right hand. 24 months after the initial autotransplantation a dark discoloration of the right hand's transplant was noted (Figure 1). Five years after the full skin autotransplantation multiple scar releases were performed: a jumping man plasty and two z-plasties (Figure 2).
Keywords
Tissue damage; Hyperpigmentation; Skin graft
Article Details
1. Case Report
A punch biopsy of the dark discoloration was performed for further examination. On histology, however, no pathological changes were found: the skin specimen was described as keratinizing squamous epithelium without an increase in the number of melanocytes. Usually, abnormal pigmentation in skin grafts is caused by changes of epidermal melanin content [1, 2]. Under normal circumstances, more melanin means increased pigmentation of the skin. In transplanted skin the degree of pigmentation is not only a result of quantitative changes, but also due to variation in distribution, degradation pattern, and size of the melanosomes within the keratinocytes [3]. Hyperpigmented skin grafts show an increased number of melanosomes within the epidermal layer [4] and usually appear 7-14 days after transplantation. This is supposed to be the sequel of melanocyte injury and abnormal melanocyte control after reinnervation of the graft eventually leading to hyperpigmentation [1-4]. Although the melanogenesis regulation gene MC-1R was identified as a key player in the development of hyperpigmentation of human skin grafts, the exact pathogenetic mechanism has not yet been identified and the true pathogenesis of skin dyspigmentation under these circumstances has remained obscure [5].
It is hypothesized that various types of tissue damage - such as ultraviolet radiation and bacterial infection - but also hypertrophic scarring, and the associated inflammatory process can induce increased pigmentation of skin autografts [5]. Hyperpigmentation of skin grafts is more commonly seen in patients with naturally darker skin such as those with Arabic or Hispanic heritage. In addition, after burns of the palms this phenomenon is also seen more frequently [6].
Treatment of the hyperpigmentation of a skin graft can be indicated for cosmetic or cultural reasons. Maintaining the function of the hand, however, remains of utmost importance. In most cases application of camouflage make-up or bleaching agents bring about unsatisfactory results. Effective treatment requires excision of the hyperpigmented skin and transplantation of a new autologous split thickness skin graft [2, 6]. A study of donor sites for hyperpigmentation would be of great interest.
Conflict of Interest
There are no conflicts of interests.
References
- Tyack ZF, Pegg S, Ziviani J. Postburn dyspigmentation: its assessment, management, and relationship to scarring--a review of the literature. J Burn Care Rehabil 18 (1997): 435- 440.
- Al-Qattan MM. Surgical management of post-burn skin dyspigmentation of the upper limb. Burns 26 (2000): 581-586.
- Tsukada S. Studies on the pigmentation of skin grafts: the ultrastructure of epidermal melanoxytes. Plast Reconstr Surg 59 (1977): 98-106.
- Kim JS, Park SW, Choi TH, et al. The evaluation of relevant factors influencing skin graft changes in color over time. Dermatol Surg 34 (2008): 32-39.
- Xue CY, Dai HY, Li L, et al. Involvement of melanocortin-1 receptor in the hyperpigmentation of human skin autografts. J Dermatol 39 (2012): 705-710.
- Teles G, Bastos V, Mello G. Correction of hypercromic palmar graft with split-thickness instep plantar graft: case report. J Burn Care Res 29 (2008): 403-405.