Granular Cell Tumor of the Breast Imitating a Malignant Tumor: A Case Report and Review of Literature
Article Information
Magdalena Ewa Gumowska2*, Axana Maria Szlenk2, Katarzyna Roszkowska-Purska3, Hanna Piotrzkowska-Wróblewska1, Wojciech Secomski1, Katarzyna Sylwia Dobruch-Sobczak1,2
1Ultrasound Department, Institute of Fundamental Technological Research, Polish Academy of Sciences, Pawi?skiego 5B St., 02-106 Warsaw, Poland
2Radiology Department II, Maria Sk?odowska-Curie National Research Institute of Oncology, Wawelska 15 St., 02-034 Warsaw, Poland
3Pathology Department, Maria Sk?odowska-Curie National Research Institute of Oncology, Wawelska 15 St., 02-034 Warsaw, Poland
*Corresponding Author: Magdalena Ewa Gumowska, Radiology Department II, Maria Sk?odowska-Curie National Research Institute of Oncology, Wawelska 15 St., 02-034 Warsaw, Poland.
Received: 09 August 2022; Accepted: 29 August 2022; Published: 16 September 2022
Citation: Magdalena Ewa Gumowska, Axana Maria Szlenk, Katarzyna Roszkowska-Purska, Hanna Piotrzkowska-Wróblewska, Wojciech Secomski, Katarzyna Sylwia Dobruch-Sobczak. Granular Cell Tumor of the Breast Imitating a Malignant Tumor: A Case Report and Review of Literature. Archives of Clinical and Medical Case Reports 6 (2022): 643-646.
View / Download Pdf Share at FacebookAbstract
A 22 year-old woman with no family history of breast cancer developed a painful breast tumor in the inner lower quadrant of the left breast. After surgical consultation, ultrasound examination was advised. On ultrasound, the mass demonstrated malignant features such as non-parallel orientation, hypoechogenicity, spiculated margins, posterior shadowing, peripheral vessels on color Doppler and increased stiffness in the tissue surrounding the tumor. Before biopsy, mammography was performed. The mass had higher density than fibroglandular tissue, margins were ill-defined (spiculated) and had no microcalcification. BIRADS 5 category was preassigned. Core biopsy revealed granular cell tumor (GCT). The patient is undergoing regular follow-up. Granular cell tumor is rare and generally benign, however, it typically demonstrates malignant features clinically and on obtained diagnostic images. This article highlights the variety of imaging features accompanying benign breast tumors.
Keywords
Breast Cancer; Breast Ultrasound; Granular Cell Tumor; Schwann Cells
Breast Cancer articles; Breast Ultrasound articles; Granular Cell Tumor articles; Schwann Cells articles
Breast Cancer articles Breast Cancer Research articles Breast Cancer review articles Breast Cancer PubMed articles Breast Cancer PubMed Central articles Breast Cancer 2023 articles Breast Cancer 2024 articles Breast Cancer Scopus articles Breast Cancer impact factor journals Breast Cancer Scopus journals Breast Cancer PubMed journals Breast Cancer medical journals Breast Cancer free journals Breast Cancer best journals Breast Cancer top journals Breast Cancer free medical journals Breast Cancer famous journals Breast Cancer Google Scholar indexed journals COVID-19 articles COVID-19 Research articles COVID-19 review articles COVID-19 PubMed articles COVID-19 PubMed Central articles COVID-19 2023 articles COVID-19 2024 articles COVID-19 Scopus articles COVID-19 impact factor journals COVID-19 Scopus journals COVID-19 PubMed journals COVID-19 medical journals COVID-19 free journals COVID-19 best journals COVID-19 top journals COVID-19 free medical journals COVID-19 famous journals COVID-19 Google Scholar indexed journals Breast Ultrasound articles Breast Ultrasound Research articles Breast Ultrasound review articles Breast Ultrasound PubMed articles Breast Ultrasound PubMed Central articles Breast Ultrasound 2023 articles Breast Ultrasound 2024 articles Breast Ultrasound Scopus articles Breast Ultrasound impact factor journals Breast Ultrasound Scopus journals Breast Ultrasound PubMed journals Breast Ultrasound medical journals Breast Ultrasound free journals Breast Ultrasound best journals Breast Ultrasound top journals Breast Ultrasound free medical journals Breast Ultrasound famous journals Breast Ultrasound Google Scholar indexed journals Ultrasound articles Ultrasound Research articles Ultrasound review articles Ultrasound PubMed articles Ultrasound PubMed Central articles Ultrasound 2023 articles Ultrasound 2024 articles Ultrasound Scopus articles Ultrasound impact factor journals Ultrasound Scopus journals Ultrasound PubMed journals Ultrasound medical journals Ultrasound free journals Ultrasound best journals Ultrasound top journals Ultrasound free medical journals Ultrasound famous journals Ultrasound Google Scholar indexed journals Immunotherapy articles Immunotherapy Research articles Immunotherapy review articles Immunotherapy PubMed articles Immunotherapy PubMed Central articles Immunotherapy 2023 articles Immunotherapy 2024 articles Immunotherapy Scopus articles Immunotherapy impact factor journals Immunotherapy Scopus journals Immunotherapy PubMed journals Immunotherapy medical journals Immunotherapy free journals Immunotherapy best journals Immunotherapy top journals Immunotherapy free medical journals Immunotherapy famous journals Immunotherapy Google Scholar indexed journals Schwann Cells articles Schwann Cells Research articles Schwann Cells review articles Schwann Cells PubMed articles Schwann Cells PubMed Central articles Schwann Cells 2023 articles Schwann Cells 2024 articles Schwann Cells Scopus articles Schwann Cells impact factor journals Schwann Cells Scopus journals Schwann Cells PubMed journals Schwann Cells medical journals Schwann Cells free journals Schwann Cells best journals Schwann Cells top journals Schwann Cells free medical journals Schwann Cells famous journals Schwann Cells Google Scholar indexed journals CT articles CT Research articles CT review articles CT PubMed articles CT PubMed Central articles CT 2023 articles CT 2024 articles CT Scopus articles CT impact factor journals CT Scopus journals CT PubMed journals CT medical journals CT free journals CT best journals CT top journals CT free medical journals CT famous journals CT Google Scholar indexed journals Breast Cancer articles Breast Cancer Research articles Breast Cancer review articles Breast Cancer PubMed articles Breast Cancer PubMed Central articles Breast Cancer 2023 articles Breast Cancer 2024 articles Breast Cancer Scopus articles Breast Cancer impact factor journals Breast Cancer Scopus journals Breast Cancer PubMed journals Breast Cancer medical journals Breast Cancer free journals Breast Cancer best journals Breast Cancer top journals Breast Cancer free medical journals Breast Cancer famous journals Breast Cancer Google Scholar indexed journals Granular Cell Tumor articles Granular Cell Tumor Research articles Granular Cell Tumor review articles Granular Cell Tumor PubMed articles Granular Cell Tumor PubMed Central articles Granular Cell Tumor 2023 articles Granular Cell Tumor 2024 articles Granular Cell Tumor Scopus articles Granular Cell Tumor impact factor journals Granular Cell Tumor Scopus journals Granular Cell Tumor PubMed journals Granular Cell Tumor medical journals Granular Cell Tumor free journals Granular Cell Tumor best journals Granular Cell Tumor top journals Granular Cell Tumor free medical journals Granular Cell Tumor famous journals Granular Cell Tumor Google Scholar indexed journals Tumor articles Tumor Research articles Tumor review articles Tumor PubMed articles Tumor PubMed Central articles Tumor 2023 articles Tumor 2024 articles Tumor Scopus articles Tumor impact factor journals Tumor Scopus journals Tumor PubMed journals Tumor medical journals Tumor free journals Tumor best journals Tumor top journals Tumor free medical journals Tumor famous journals Tumor Google Scholar indexed journals
Article Details
1. Introduction
Granular cell tumor is a neuroectodermal tumor derived from Schwann cells [1]. The skin and the subcutaneous tissue are the most common sites, however, it could also arise in the head and neck region, especially in the tongue where it was first described in the 19th century and also in the gastrointestinal and respiratory tracts and extremities. Breast origin is as many as 8% of all cases of granular cell tumors [2] and they represent only 0,1% of all breast tumors (1). Malignant transformation is observed in up to 2% of breast granular cell tumor cases [2]. The patient age with GCT ranges from 19 to 77 years [2,3].
2. Case Report
A 22-year-old woman presented with a 6-months history of a palpable mass in the lower inner quadrant of her left breast and left breast pain without nipple discharge. Physical examination revealed a 2 cm firm mass located at 8 o’clock with normal overlying skin. There was no associated axillary, supraclavicular or infraclavicular adenopathy. About six years prior to the current examination, the patient underwent excision of a benign lesion (fibroadenoma) from the same breast – a postoperative scar at 3 o’clock was noted. Apart from that and a history of anxiety disorders, her past medical history was unremarkable. She had also no family history of breast cancer. Ultrasonography (US) and mammography (full-field digital mammography, FFDM) were performed. Upon ultrasound examination, a deeply hypoechoic lesion with spiculated margins, echogenic halo, irregular shape and very intensive acoustic shadowing (Figure 1), causing difficulties in making exact measurements was demonstrated. Approximate size was 19 x 21mm. Peripheral vascularity was noted (Figure 2), as well as highly increased stiffness in shear wave elastography (E max 300 kPa) on the periphery of the lesion (Figure 3). No axillary, supraclavicular or infraclavicular lymphadenopathy was found, similarly no other lesions in both breasts were identified. The morphology of the postoperative scar in the outer quadrants of the left breast was normal.
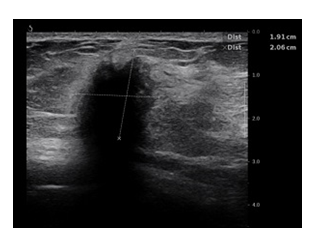
Figure 1: B-mode presentation of the tumor - deeply hypoechoic lesion with spiculated margins, echogenic halo, irregular shape and very intensive acoustic shadowing.
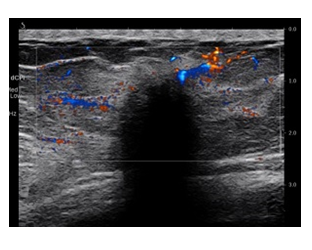
Figure 2: Peripheral vascularity of the lesion is seen.
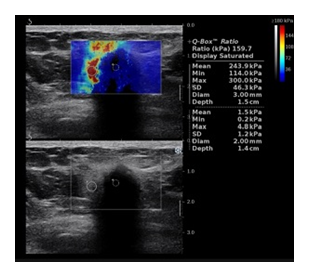
Figure 3: Shear wave elastography – periphery of the lesion is hard (E max 300kPa).
Mammography in mediolateral oblique and craniocaudal projections showed an irregular, spiculated mass in the lower inner quadrant of the left breast, with no associated calcifications (Figure 4).
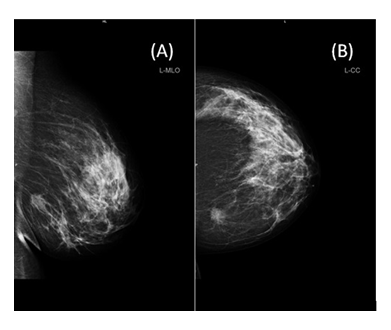
Figure 4: FFDM finding of the lesion in the lower inner quadrant of the left breast. A. Mediolateral oblique projection. B. Craniocaudal projection.
The imaging features were considered as highly suspicious for malignancy in both US and FFDM and BIRADS 5 category was assessed. An ultrasound-guided core needle biopsy was performed with a 14 gauge needle, obtaining three specimens. In the pathology report a granular cell tumor diagnosis was made. The patient was then scheduled for surgery.
3.Discussion
According to the literature, breast cancer among women under 40 years of age is rarely observed. In women younger than 30, the incidence rate is 1 out of 220 patients (0, 45%), which makes it slightly higher than the incidence rate of GCT [4]. Clinically GCT is a breast cancer mimicker, usually presenting as a painless mass, able to cause nipple and skin retraction or infiltrate pectoralis fascia or muscles. Histologically, GCT is composed of sheets of spindle cells, containing abundant eosinophilic cytoplasmic granules (PAS+), with the fibrous tissue interspersed among those cells. The tumor causes the infiltration of the adjacent tissue, which often presents as spicules on diagnostic images (Figure 2, 3, 4). Therefore, on US examination and FFDM it can be mistaken for breast carcinoma. Moreover in biopsy specimens, it could be difficult to distinguish GCT from invasive apocrine cell carcinoma, because both of them contain eosinophilic granules [2]. Franburg-Smith et al. [6] demonstrated six histological features indicating malignancy: necrosis, spindle cell presence, cells with large nuclear bodies, increased mitotic activity, high nuclear to cytoplasmic ratio and pleomorphism. Meeting 2 or more criteria allow to classify the tumor as histologically malignant, 1 or 2 criteria denote the lesion atypical, whereas if only pleomorphism is observed, but none of the other criteria are present, the tumor is described as histologically benign [6].
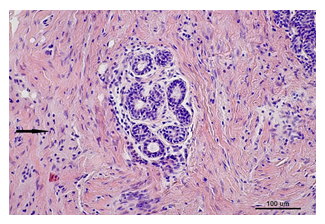
Figure 5: GCT composed of sheets of cells with infiltrative architecture and abundant eosinophilic granular cytoplasm (arrow). Hematoxylin and eosin staining, × 200.
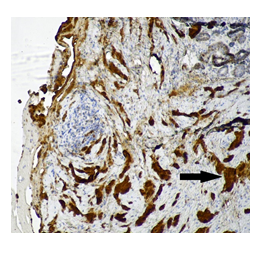
Figure 6: GCT. S-100 positive staining (arrow), × 100.
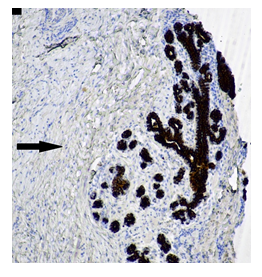
Figure 7: GCT. CKAE1/AE3 negative staining (arrow), x 100.
The US and FFDM findings are not specific for GCT, as we presented in this case. On FFDM most of them display malignant features, having high density, irregular shape and spiculated margins. Same goes with the ultrasound appearance which leads the radiologist to suspect a malignant breast tumor. On US the shape of the tumor is usually elliptical, the margins are not circumscribed, there is lack of capsule and a shadowing behind the tumor is visible. The echogenicity could be various (dominate hypoechoic or anechoic), because of the anisotropic effect. Typically it is avascular on Doppler US. A less common manifestation is a circumscribed mass and an oval shape on US and FFDM. [6] Abreu et al. published a series of five GCT. The FFDM findings were nonspecific, all five lesions presented as masses, 3/5 exhibiting spiculated margins, one showing circumscribed and one indistinct margins. In all the cases evaluated, ultrasound showed nonparallel orientation, irregular shape, heterogenous echogenicity, 3/5 lesions had spiculated margins similarly like on FFDM. On MRI (magnetic resonance imaging) the signal intensity on T1 and T2-weighted images is generally lower than that seen in breast cancer, whereas, the enhancement is heterogenous [7,8]. Our case is clinically and radiologically similar to few reports published in the literature [1,6]. In differential diagnosis, invasive carcinoma, fat necrosis and fibromatosis should be taken into account. While the histology is benign, excision is always advised. Our patient was directed for surgery, with a recommendation from our pathologist to perform wide excision.
4. Conclusion
It is essential to exclude breast cancer before a decision of surgical treatment of GCT is to be made. It is crucial to obtain credible and detailed pathological verification, therefore a core needle biopsy is necessary. To sum it up, clinical and imaging overall view of the tumor tends to mimic malignancy.
Conflict of Interest
All contributing authors declare no conflict of interest.
Funding
This work was financially supported by the National Centre for Research and Development (NCBiR) under the grant agreement LIDER/24/0088/L -11/19/NCBR/2020
References
- Rexeena B, Paul A, Nitish RA, et al. Granular Cell Tumor of Breast: a Case Report and Review of Literature. Indian J Surg Oncol 6 (2015): 446-448.
- Edited by the WHO Classification of Tumours Editorial Board. WHO Classification of tumours. 5Th edition. Breast Tumours (2019).
- Abrikossoff A. Uber Myome, ausgehend von der quergestreiften wilkuerlichen muskulatur. Virchows Arch Pathol Anat 260 (1926): 215-233.
- Paluch-Shimon S, Cardoso F, Partridge AH, et al. ESO-ESMO 4th International Consensus Guidelines for Breast Cancer in Young Women (BCY4). Ann Oncol 31 (2020): 674-696.
- Fanburg-Smith JC, Meis-Kindblom JM, Fante R, et al. Malignant granular cell tumor of soft tissue: diagnostic criteria and clinicopathologic correlation 22 (1998): 779-794.
- Ueki Y, Horimoto Y, Shiraishi A, et al. Granular Cell Tumor of the Breast Coexisting with Ductal Carcinoma in situ: Case Report. Case Rep Oncol 14 (2021): 303-308.
- Zeng Q, Liu L, Wen Q, et al. Imaging features of granular cell tumor in the breast Case report 99 (2020): e23264.
- Abreu N, Filipe J, André S, et al. Granular cell tumor of the breast: correlations between imaging and pathology findings 53 (2020): 105-111.
