Effect of a Sodium Fluoride-Releasing Rubber Cup on Hydroxyapatite Crystallinity of Human Enamel: FTIR Spectroscopy Analysis
Article Information
Giulia Orilisi1, Riccardo Monterubbianesi1, Vincenzo Tosco1, Carla Conti2, Maurizio Procaccini1, Angelo Putignano1*, Giovanna Orsini1*
1Department of Clinical Sciences and Stomatology (DISCO), Polytechnic University of Marche, Ancona, Italy
2Department of Materials, Environmental Science and Urban Planning (SIMAU), Polytechnic University of Marche, Ancona, Italy
*Corresponding Authors: Giovanna Orsini, Department of Clinical Sciences and Stomatology (DISCO), Polytechnic University of Marche, Via Tronto 10, 60126, Ancona, Italy.
Angelo Putignano, Department of Clinical Sciences and Stomatology (DISCO), Polytechnic University of Marche, Via Tronto 10, 60126, Ancona, Italy
Received: 06 February 2020; Accepted: 15 February 2020; Published: 12 March 2020
Citation: Giulia Orilisi, Riccardo Monterubbianesi, Vincenzo Tosco, Carla Conti, Maurizio Procaccini, Angelo Putignano, Giovanna Orsini. Effect of a Sodium Fluoride-Releasing Rubber Cup on Hydroxyapatite Crystallinity of Human Enamel: FTIR Spectroscopy Analysis. Dental Research and Oral Health 3 (2020): 024-034.
View / Download Pdf Share at FacebookAbstract
Fluoride application is an important strategy to reduce demineralization and enhance remineralization in human teeth. This study aimed to evaluate the effect on enamel hydroxyapatite (HA) crystallinity (C) of a sodium fluoride-releasing rubber cup compared to a non-fluoride rubber cup, using Fourier Transformed Mid Infrared Spectroscopy (FTMIR) analysis. First class direct composite restorations were performed in ten sound extracted molars. Teeth were then divided into two groups (n=5): Control group, polished with non-fluoride rubber cup (noFHA), for 10 s; Tested group, polished with a sodium fluoride-releasing rubber cup (FHA), for 10 s. Samples were scraped off on the treated surfaces with abrasive paper and the dust was analyzed using FTMIR. Spectra were acquired in the range of 4000-400 cm-1 and each spectrum represented the average of 5 measurements. Phosphate (PO4) vibration at 604 cm-1 was used to analyze C: the full width at half maximum (FWHM) of noFHA was lower than the one of FHA; thus, sodium fluoride, contained in the rubber cup, increased C. The absorption at 1090 cm-1 can be considered an additional marker of C, indeed the peak of FHA was higher than the one of HA and noFHA, thus suggesting increasing and stabilizing of the enamel C. In conclusion, the tested sodium fluoride-releasing rubber cup could be an effective polishing system since it not only allows to polish the tooth surface, but also improves the C of enamel HA, thanks to the quick bond done by fluoride.
Keywords
<p>Hydroxyapatite, Enamel Crystallinity, Sodium Fluoride, Dental Enamel, Fourier Transform Infrared Spectroscopy, Polishing System</p>
Hydroxyapatite articles, Enamel Crystallinity articles, Sodium Fluoride articles, Dental Enamel articles, Fourier Transform Infrared Spectroscopy articles, Polishing System articles
Hydroxyapatite articles Hydroxyapatite Research articles Hydroxyapatite review articles Hydroxyapatite PubMed articles Hydroxyapatite PubMed Central articles Hydroxyapatite 2023 articles Hydroxyapatite 2024 articles Hydroxyapatite Scopus articles Hydroxyapatite impact factor journals Hydroxyapatite Scopus journals Hydroxyapatite PubMed journals Hydroxyapatite medical journals Hydroxyapatite free journals Hydroxyapatite best journals Hydroxyapatite top journals Hydroxyapatite free medical journals Hydroxyapatite famous journals Hydroxyapatite Google Scholar indexed journals Enamel Crystallinity articles Enamel Crystallinity Research articles Enamel Crystallinity review articles Enamel Crystallinity PubMed articles Enamel Crystallinity PubMed Central articles Enamel Crystallinity 2023 articles Enamel Crystallinity 2024 articles Enamel Crystallinity Scopus articles Enamel Crystallinity impact factor journals Enamel Crystallinity Scopus journals Enamel Crystallinity PubMed journals Enamel Crystallinity medical journals Enamel Crystallinity free journals Enamel Crystallinity best journals Enamel Crystallinity top journals Enamel Crystallinity free medical journals Enamel Crystallinity famous journals Enamel Crystallinity Google Scholar indexed journals Sodium Fluoride articles Sodium Fluoride Research articles Sodium Fluoride review articles Sodium Fluoride PubMed articles Sodium Fluoride PubMed Central articles Sodium Fluoride 2023 articles Sodium Fluoride 2024 articles Sodium Fluoride Scopus articles Sodium Fluoride impact factor journals Sodium Fluoride Scopus journals Sodium Fluoride PubMed journals Sodium Fluoride medical journals Sodium Fluoride free journals Sodium Fluoride best journals Sodium Fluoride top journals Sodium Fluoride free medical journals Sodium Fluoride famous journals Sodium Fluoride Google Scholar indexed journals Dental Enamel articles Dental Enamel Research articles Dental Enamel review articles Dental Enamel PubMed articles Dental Enamel PubMed Central articles Dental Enamel 2023 articles Dental Enamel 2024 articles Dental Enamel Scopus articles Dental Enamel impact factor journals Dental Enamel Scopus journals Dental Enamel PubMed journals Dental Enamel medical journals Dental Enamel free journals Dental Enamel best journals Dental Enamel top journals Dental Enamel free medical journals Dental Enamel famous journals Dental Enamel Google Scholar indexed journals Fourier Transform Infrared Spectroscopy articles Fourier Transform Infrared Spectroscopy Research articles Fourier Transform Infrared Spectroscopy review articles Fourier Transform Infrared Spectroscopy PubMed articles Fourier Transform Infrared Spectroscopy PubMed Central articles Fourier Transform Infrared Spectroscopy 2023 articles Fourier Transform Infrared Spectroscopy 2024 articles Fourier Transform Infrared Spectroscopy Scopus articles Fourier Transform Infrared Spectroscopy impact factor journals Fourier Transform Infrared Spectroscopy Scopus journals Fourier Transform Infrared Spectroscopy PubMed journals Fourier Transform Infrared Spectroscopy medical journals Fourier Transform Infrared Spectroscopy free journals Fourier Transform Infrared Spectroscopy best journals Fourier Transform Infrared Spectroscopy top journals Fourier Transform Infrared Spectroscopy free medical journals Fourier Transform Infrared Spectroscopy famous journals Fourier Transform Infrared Spectroscopy Google Scholar indexed journals Polishing System articles Polishing System Research articles Polishing System review articles Polishing System PubMed articles Polishing System PubMed Central articles Polishing System 2023 articles Polishing System 2024 articles Polishing System Scopus articles Polishing System impact factor journals Polishing System Scopus journals Polishing System PubMed journals Polishing System medical journals Polishing System free journals Polishing System best journals Polishing System top journals Polishing System free medical journals Polishing System famous journals Polishing System Google Scholar indexed journals dentin articles dentin Research articles dentin review articles dentin PubMed articles dentin PubMed Central articles dentin 2023 articles dentin 2024 articles dentin Scopus articles dentin impact factor journals dentin Scopus journals dentin PubMed journals dentin medical journals dentin free journals dentin best journals dentin top journals dentin free medical journals dentin famous journals dentin Google Scholar indexed journals
Article Details
1. Introduction
Despite all the efforts and advances made in the prevention of tooth demineralization and decays, these pathologies still affect a large number of patients [1]. Dental tissues are continuously undergoing cycles of demineralization and remineralization [2] and caries occurs when demineralization exceeds remineralization [3]. However, the progression of dental decays is a slow process, and, during early stages, non-invasive procedures allow to prevent demineralization, converting the lesion to inactive state from an active state [4, 5], thus enhancing remineralization [6, 7]. In the past decades, various remineralizing agents containing fluoride, calcium, and phosphate ions in various forms and concentrations, were introduced [8-10]. Among these preventive measurements, there are several fluoride-containing products for professional applications with anticariogenic effects [4, 7, 11]. The role of fluoride in the prevention and treatment of erosion and teeth demineralization has long been questioned [12, 13]. Traditional fluoride applications, using monovalent fluorides in low-to-moderate concentrations, such as in toothpastes and mouth rinses, were observed to have preventive effect [12, 14]. Sodium fluoride (NaF) varnish is one of the most concentrated fluoride products commercially available and it has been widely used in Europe for decades [15].
Rubber cups, in combination with prophylaxis pastes, are commonly used for supragingival professional tooth cleaning and polishing. Recently, fluoride-releasing rubber cups were introduced, in order to simultaneously fluoridate the enamel, without a prophylaxis paste, and polish the tooth after a restorative procedure [16, 17]. The two major aspects of fluoride action are: (i) the inhibition of demineralization, and (ii) the enhancement of subsurface remineralization of enamel surface [15]. Fluoride, in the aqueous phase at the apatite crystal surface, plays a determining role in the inhibition of enamel or dentin demineralization [4, 18]. As the pH rises, new and larger crystals that contain more fluoride in form of fluorohydroxyapatite crystals are formed, reducing the enamel demineralization with an increase of remineralization [19, 20]. Hydroxyapatite (HA) is composed of calcium, phosphorous, oxygen and hydrogen atoms with the chemical formula Ca10(PO4)6(OH)2, characterized by a hexagonal unit cell. Its study and description are of great importance in the field of biomaterials, because HA is the main constituent of bone, enamel and dentine [21]. The crystallinity (C) is correlated to the degree of order within the crystals. In the scientific literature, two ways are reported to measure the C: X-ray diffraction and Infrared Spectroscopy [21, 22]. The ions substitution introduces distortions in the apatite and the C of HA can be modified: in the case of F-, replacing OH-, the C is increased, due to the F- small ionic radius, producing a tiny unit cell volume [23, 24]. The present study is the first report evaluating the effect on enamel hydroxyapatite C of a rubber cup, releasing sodium fluoride at 0.9% used to polish teeth after resin-based composite restorations. The effectiveness of the tested material was compared with a non-fluoride rubber cup, by means of Fourier Transformed Mid Infrared Spectroscopy (FTMIR). The null hypothesis was that sodium fluoride, contained in the tested rubber cup, is able to improve the C of human enamel HA.
2. Materials and Methods
After routinely performed extractions of third molars for orthodontic or prosthetic reasons at the Section of Stomatology of the Polytechnic University of Marche, ten sound teeth were collected. Teeth were washed in an ultrasonic bath with distilled water for 2 minutes in order to remove blood and biological remains, and then carefully examined to exclude the presence of lesions and decays, including hypoplastic defects and cracks; elements exhibiting any of these features were excluded. Afterwards, teeth were stored in artificial saliva. On each tooth, a class I cavity was created using a diamond burr (FG755F-5, Kerr, U.S.) and the restoration performed using a simplified adhesive (Scotchbond Universal Adhesive, 3M ESPE, St. Paul, MN), followed by a nanohybrid resin-composite (Filtek Supreme XTE, 3M ESPE, St. Paul, MN), polymerized with the lamp Elipar DeepCure S (3M ESPE, Seefeld, Germany) for 40 s. Subsequently, teeth were divided into the following two groups (n=5):
- • Control group: teeth polished for 10 s, using a non-fluoride rubber cup, with the same shape of the ones, used in the tested group (noFHA).
- • Tested group: teeth polished for 10 s, using a fluoride-releasing rubber cup (Pasteless Prophy®, Kerr, U.S.; FHA).
The rubber cup was used with a slow handpiece at 6000 rounds/min, one for each sample. All the procedures were performed by single dental operator to minimize operator changes in variability. Then, the samples were washed with distilled water, dried and analyzed in order to evaluate the C of HA in enamel, using FTMIR spectroscopy [25]. Samples were scraped off on the treated surfaces with abrasive paper, transparent in the infrared, and were analyzed using a Perkin Elmer Spectrum GX1 spectrometer, equipped with a Universal attenuated Total Reflectance (U-ATR) accessory. The spectra were acquired in the range of 4000-500 cm-1, 64 scans and 4 cm-1 spectral resolution, and each spectrum represents the average of 5 measurements.
3. Results
All samples showed comparable spectra in each group in the region 4000-500 cm-1 (Figure 1). In order to evaluate C, the vibrations between 1200-500 cm-1, corresponding to the stretching modes of PO4 of HA, were considered [26]. For data handling, Spectrum v.6.3.1 and Grams AI 7.02 software packages were
used. After curve-fitting of the obtained spectra, position, height, full width at half maximum (FWHM) and area under the curves were measured (Figure 2). The most intense band of PO4 was found at 1090 cm–1 in FHA, while, in noFHA it was at 1040 cm–1 [27]. Moreover, other spectra were obtained and compared: the spectrum of syntetic HA (pureHA) and the spectrum obtained from the dust, derived from noFHA, mixed with NaF and water, at pH=6, in order to simulate the saliva effects (Mix) (Figure 3).
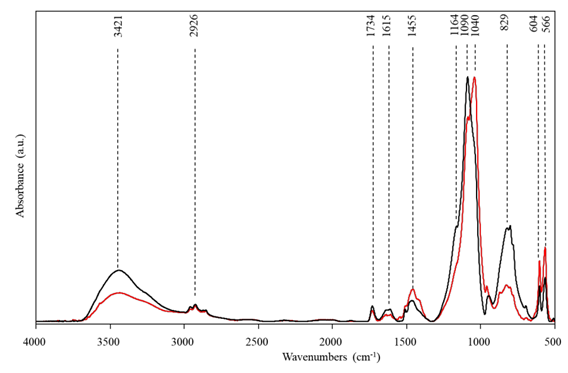
Figure 1: Averaged infrared spectra of noFHA (red) and FHA (black) samples between 4000 - 500 cm-1.
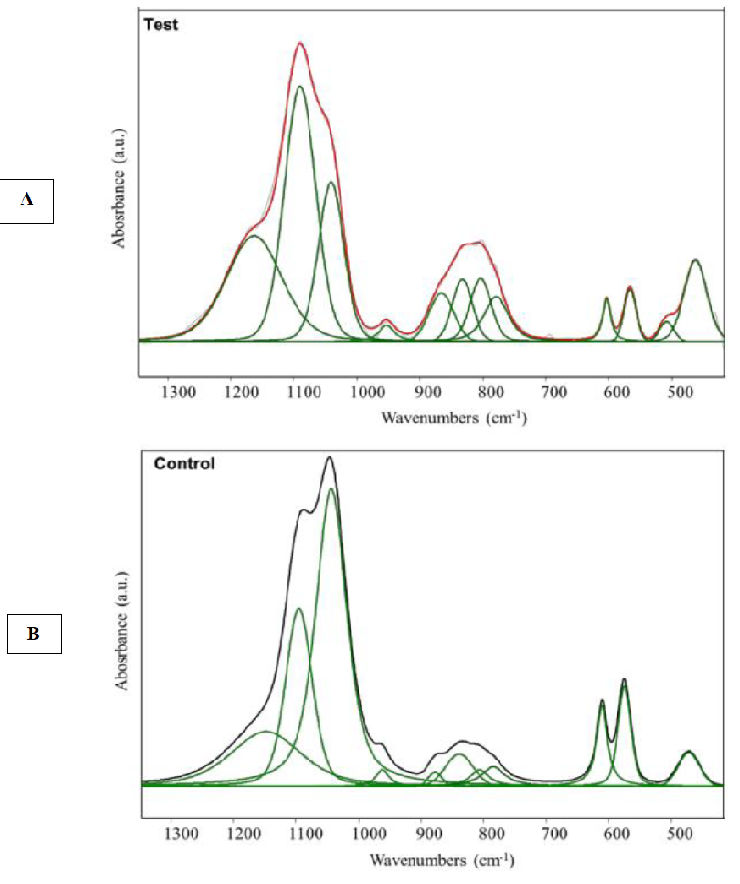
Figure 2: Mixed Gaussian-Lorenzian curve-fitting for FHA (Test, A) and noFHA (Control, B) samples. In FHA (A), the red curve and in noFHA (B) the black one represented the average curve deriving from the obtained spectra.
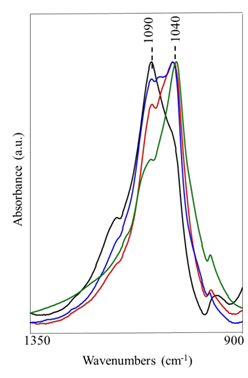
Figure 3: (Blu spectrum): mixture of noFHA dust with NaF and water at pH=6 (Mix); (Red Spectrum): HA (pureHA); (Green Spectrum): noFHA; (Black Spectrum): FHA. The analyzed peaks are found at 1090 cm–1 and 1040 cm–1.
4. Discussion
Enamel consists of 96% (wt%) inorganic matrix and 4% (w/w) organic material (mainly lipids and noncollagenous proteins), as well as water, which occupies the free spaces between HA crystals [28]. HA has a hexagonal crystal structure, consisting on isolated PO43− tetrahedra connected by a network of distorted octahedra and twisted trigonal prisms, both of which accommodate Ca2+, whereas OH− are located at the corners [28-30]. FTIR is a technique providing information especially about bonds of molecules. Chemical groups (e.g., hydroxyl, phosphate, amide) can be identified by their specific absorption at different wavenumbers. Because the spectra of these mineral components are quite distinct, vibrational spectroscopy has been extensively used to study all of these tissues, providing information on the nature of the present mineral phases, as well as quantitative information on the changes in mineral and matrix composition as mineralization occurs, and the nature and amounts of substituents in the mineral [25]. In particular, PO4 vibration at 650-500 cm-1 has been used to analyze the C of the apatite domains by FTMIR, using the method proposed by Shemesh et al. [31]. According to his study, the apatite C is inversely proportional to the FWHM of the peak at 604 cm-1, assigned to the phosphate ions [21, 31-33]. In this study, the FWHM of the peak at 604 cm–1 of noFHA is around 22.9, while of FHA is around 16.8. The C of noFHA is lower than the one of FHA; thus, NaF, contained in the rubber cup, results to increase the C of HA, being our results in agreement with the conclusions reported in Shemesh’s study [31]. Moreover, the absorption at 1090 cm-1 can be considered an additional marker of HA, while the peak at 1040 cm-1 is a marker of HA amorphous structure [27, 34]. In Figure 3, the height of the peaks at 1090 cm-1 shows different trends. C decreases as follows: FHA>Mix>pureHA>noFHA. This is probably because, using a non-releasing rubber cup during polishing, the amount of HA, contained in enamel, is reduced. On the contrary, if a fluoride-releasing rubber cup is used, fluoride could bind to HA, forming fluorohydroxyapatite, which is a more resistant compound than the HA [35-38]. Thus, as showed in Figure 3, the peak at 1090 cm-1 related to FHA is the highest, increasing and stabilizing enamel C. To confirm this finding, the height of the band of FHA at 1040 cm-1 is the lowest, because the component of amorphous HA is less than in the other samples. Dental prophylaxis involves the placement of pumice or an abrasive paste in a rubber cup to the clinical crowns of the teeth, in order to remove plaque, salivary pellicle and extrinsic stains before fluoride application [39]. This fact could result in a greater amount of fluoride contacting the enamel surface, thus enhancing its anti-cariogenic property. Therefore, a polishing treatment, such as the one tested in our study, based on the simultaneous action of cleaning/smoothen dental surface, in adjunction with fluoride bonding, can be helpful in the inhibition of dental caries as well as in the prevention of secondary caries in the restored tooth [40]. According to this, the use of topical fluoride within the polishing rubber cup, as routine part of the final step of many restorative procedures, could enormously simplify the clinical practice, allowing to fluoridate enamel and contemporary polish the restoration. Previous studies analyzed the effect on the surface roughness and surface gloss of tooth enamel and composite resin, when exposed to a paste-free prophylaxis polishing cup, as well as a conventional prophylaxis polishing paste [41]. They reported that the conventional prophylaxis pastes increased surface roughness and decreased the gloss of the composite resin and tooth enamel, while the paste-free cups did not significantly affect the surface roughness of the enamel or the restorative materials. According to these last acquisitions it would be interesting to perform a further analysis investigating whether the fluoridated tested polishing cups would affect the roughness and the gloss of the enamel and composite surfaces, as previously performed using other specific polishing systems [42].
5. Conclusions
The null hypothesis that fluoride-releasing rubber cup may improve enamel HA crystallinity was not rejected, suggesting that this polishing system allows to simultaneously polish the restored tooth surface and increase C of enamel HA, without using an additional prophylaxis paste, by quickly bonding the fluoride for stabilizing HA structure. Within the limits of the present study, which is an in vitro evaluation with a limited sample size, our findings provide the first demonstration that a fluoride-releasing rubber cup may chemically improve HA structure. Therefore, it can be suggested that the tested rubber cups are an effective way for clinicians to polish the teeth after restorative procedures, because they enhance enamel structure strength, being more advantageous, in term of caries prevention, than traditional non-fluoride releasing rubber cups. To better understand the mechanism of action of NaF related to the C of HA, it would be interesting to plan future investigations that will evaluate both in vitro and in vivo the exact amount of fluoride uptake by enamel.
Acknowledgments
The authors thank Professor Giorgio Tosi for his valuable contribution in drafting this manuscript and Alessandro Lorenzini for samples preparation.
Author Contributions
- Orilisi and R. Monterubbianesi contributed to the acquisition and interpretation of data and manuscript discussion. V. Tosco and M. Procaccini contributed to the study design and data interpretation. C. Conti performed the FTMIR analysis and contributed to data interpretation. A. Putignano and G. Orsini contributed to the research plan, data interpretation and supervised the entire project. All authors participated to the writing of the present manuscript.
Financial Disclosure
No financial relationships relevant to this article.
Conflicts of Interest
The authors declare that there is no conflict of interest regarding the publication of this article.
References
- Lussi A, Schlueter N, Rakhmatullina E, et al. Dental erosion-an overview with emphasis on chemical and histopathological aspects. Caries Res 45 (2011): 2-12.
- Hannig M, Hannig C. Nanotechnology and Its Role in Caries Therapy. Advances in Dental Research 24 (2012): 53-57.
- Wagle M, D'Antonio F, Reierth E, et al. Dental caries and preterm birth: a systematic review and meta-analysis. BMJ Open 8 (2018): e018556.
- Rao R, Jain A, Verma M, et al. Comparative evaluation of remineralizing potential of Fluoride using three different remineralizing protocols: An in vitro study. J Conserv Dent 20 (2017): 463-466.
- Viana ÍEL, Lopes RM, Silva FRO, et al. Novel fluoride and stannous -functionalized β-tricalcium phosphate nanoparticles for the management of dental erosion. J Dent 92 (2020): 103263.
- Carvalho JC, Scaramucci T, Aimée NR, et al. Early diagnosis and daily practice management of erosive tooth wear lesions. Br Dent J 224 (2018): 311-318.
- Li X, Wang J, Joiner A, et al. The remineralisation of enamel: a review of the literature. J Dent 42 (2014): S12-S20.
- Tasios T, Papageorgiou SN, Papadopoulos MA, et al. Prevention of orthodontic enamel demineralization: A systematic review with meta-analyses. Orthod Craniofac Res 22 (2019): 225-235.
- Rao A, Malhotra N. The role of remineralizing agents in dentistry: a review. Compend Contin Educ Dent 32 (2011): 26-33.
- Bandekar S, Patil S, Dudulwar D, et al. Remineralization potential of fluoride, amorphous calcium phosphate-casein phosphopeptide, and combination of hydroxylapatite and fluoride on enamel lesions: An in vitro comparative evaluation. J Conserv Dent 22 (2019): 305-309.
- Lopes C de CA, Soares CJ, Lara VC, et al. Effect of fluoride application during radiotherapy on enamel demineralization. J Appl Oral Sci 27 (2018): e20180044.
- Huysmans M-C, Young A, Ganss C. The role of fluoride in erosion therapy. Monogr Oral Sci 25 (2014): 230-243.
- Ten Cate JM, Buijs MJ, Miller CC, et al. Elevated fluoride products enhance remineralization of advanced enamel lesions. J Dent Res 87 (2008): 943-947.
- Lussi A, Megert B, Eggenberger D, et al. Impact of different toothpastes on the prevention of erosion. Caries Res 42 (2008): 62-67.
- Lata S, Varghese NO, Varughese JM. Remineralization potential of fluoride and amorphous calcium phosphate-casein phospho peptide on enamel lesions: An in vitro comparative evaluation. J Conserv Dent 13 (2010): 42-46.
- Zimmer S, Barthel CR, Schemehorn BR, et al. A new fluoride-releasing rubber cup for professional oral hygiene. J Clin Dent 13 (2002): 253-257.
- Zimmer S, Barthel CR, Koehler C, et al. Enamel fluoride retention after application of fluoride-containing rubber cups. Am J Dent 15 (2002): 11-14.
- Fulmer MT, Ison IC, Hankermayer CR, et al. Measurements of the solubilities and dissolution rates of several hydroxyapatites. Biomaterials 23 (2002): 751-755.
- Clarkson BH, Exterkate R a. Noninvasive dentistry: a dream or reality?. Caries Res 49 (2015): 11-17.
- Tschoppe P, Zandim DL, Martus P, et al. Enamel and dentine remineralization by nano-hydroxyapatite toothpastes. J Dent 39 (2011): 430-437.
- Reyes-Gasga J, Martínez-Piñeiro EL, Rodríguez-Álvarez G, et al. XRD and FTIR crystallinity indices in sound human tooth enamel and synthetic hydroxyapatite. Mater Sci Eng C Mater Biol Appl 33 (2013): 4568-4574.
- Pleshko N, Boskey A, Mendelsohn R. Novel infrared spectroscopic method for the determination of crystallinity of hydroxyapatite minerals. Biophys J 60 (1991): 786-793.
- Grynpas MD. Fluoride effects on bone crystals. J Bone Miner Res 5 (1990): S169-S175.
- Farlay D, Panczer G, Rey C, et al. Mineral maturity and crystallinity index are distinct characteristics of bone mineral. J Bone Miner Metab 28 (2010): 433-445.
- Giorgini E, Conti C, Rocchetti R, et al. Study of oral cavity lesions by infrared spectroscopy. J Biol Regul Homeost Agents 30 (2016): 309-314.
- Termine JD, Lundy DR. Vibrational spectra of some phosphate salts amorphous to X-ray diffraction. Calcif Tissue Res 15 (1974): 55-70.
- Gadaleta SJ, Paschalis EP, Betts F, et al. Fourier transform infrared spectroscopy of the solution-mediated conversion of amorphous calcium phosphate to hydroxyapatite: new correlations between X-ray diffraction and infrared data. Calcif Tissue Int 58 (1996): 9-16.
- Ortiz-Ruiz AJ, Teruel-Fernández J de D, Alcolea-Rubio LA, et al. Structural differences in enamel and dentin in human, bovine, porcine, and ovine teeth. Ann Anat 218 (2018): 7-17.
- Boskey AL, Moore DJ, Amling M, et al. Infrared analysis of the mineral and matrix in bones of osteonectin-null mice and their wildtype controls. J Bone Miner Res 18 (2003): 1005-1011.
- Boskey AL, Mendelsohn R. Infrared spectroscopic characterization of mineralized tissues. Vib Spectrosc 38 (2005): 107-114.
- Shemesh A. Crystallinity and diagenesis of sedimentary apatites. Geochimica et Cosmochimica Acta 54 (1990): 2433-2438.
- Miller LM, Dumas P. Chemical imaging of biological tissue with synchrotron infrared light. Biochimica et Biophysica Acta (BBA) - Biomembranes 1758 (2006): 846-857.
- Pucéat E, Reynard B, Lécuyer C. Can crystallinity be used to determine the degree of chemical alteration of biogenic apatites?. Chemical Geology 205 (2004): 83-97.
- Boskey AL, DiCarlo E, Paschalis E, et al. Comparison of mineral quality and quantity in iliac crest biopsies from high- and low-turnover osteoporosis: an FT-IR microspectroscopic investigation. Osteoporos Int 16 (2005): 2031-2038.
- Manara S, Paolucci F, Palazzo B, et al. Electrochemically-assisted deposition of biomimetic hydroxyapatite–collagen coatings on titanium plate. Inorganica Chimica Acta 361 (2008): 1634-1645.
- Nasker P, Samanta A, Rudra S, et al. Effect of fluorine substitution on sintering behaviour, mechanical and bioactivity of hydroxyapatite. J Mech Behav Biomed Mater 95 (2019): 136-142.
- Colceriu Burtea L, Prejmerean C, Prodan D, et al. New Pre-reacted Glass Containing Dental Composites (giomers) with Improved Fluoride Release and Biocompatibility. Materials (Basel) 12 (2019).
- Rintoul L, Wentrup-Byrne E, Suzuki S, et al. FT-IR spectroscopy of fluoro-substituted hydroxyapatite: strengths and limitations. J Mater Sci Mater Med 18 (2007): 1701-1709.
- Azarpazhooh A, Main PA. Efficacy of dental prophylaxis (rubber cup) for the prevention of caries and gingivitis: a systematic review of literature. Br Dent J 207 (2009): 328-329.
- Nigam AG, Jaiswal J, Murthy R, et al. Estimation of Fluoride Release from Various Dental Materials in Different Media-An In Vitro Study. Int J Clin Pediatr Dent 2 (2009): 1-8.
- Covey DA, Barnes C, Watanabe H, et al. Effects of a paste-free prophylaxis polishing cup and various prophylaxis polishing pastes on tooth enamel and restorative materials. Gen Dent 59 (2011): 466-473.
- Tosco V, Monterubbianesi R, Orilisi G, et al. Effect of four different finishing and polishing systems on resin composites: roughness surface and gloss retention evaluations. Minerva Stomatol (2019).
