Dynamic Orthosis for the Entire Spine
Article Information
Herman J Traven*
Faculty of Medicine, University of Ljubljana, Ljubljana, Slovenia
*Corresponding Author: Herman J Traven, Dr. Med., chirurg, Faculty of Medicine, University of Ljubljana, SI-1000 Ljubljana, Kongresni trg 12, Slovenia
Received: 05 March 2020; Accepted: 16 March 2020; Published: 30 March 2020
Citation:
Herman J Traven. Dynamic Orthosis for the Entire Spine. Journal of Spine Research and Surgery 2 (2020): 017-022.
View / Download Pdf Share at FacebookKeywords
<p>Spine Injuries, Orthosis, Spine, Dynamic Immobilization</p>
Spine Injuries articles Spine Injuries Research articles Spine Injuries review articles Spine Injuries PubMed articles Spine Injuries PubMed Central articles Spine Injuries 2023 articles Spine Injuries 2024 articles Spine Injuries Scopus articles Spine Injuries impact factor journals Spine Injuries Scopus journals Spine Injuries PubMed journals Spine Injuries medical journals Spine Injuries free journals Spine Injuries best journals Spine Injuries top journals Spine Injuries free medical journals Spine Injuries famous journals Spine Injuries Google Scholar indexed journals Orthosis articles Orthosis Research articles Orthosis review articles Orthosis PubMed articles Orthosis PubMed Central articles Orthosis 2023 articles Orthosis 2024 articles Orthosis Scopus articles Orthosis impact factor journals Orthosis Scopus journals Orthosis PubMed journals Orthosis medical journals Orthosis free journals Orthosis best journals Orthosis top journals Orthosis free medical journals Orthosis famous journals Orthosis Google Scholar indexed journals Spine articles Spine Research articles Spine review articles Spine PubMed articles Spine PubMed Central articles Spine 2023 articles Spine 2024 articles Spine Scopus articles Spine impact factor journals Spine Scopus journals Spine PubMed journals Spine medical journals Spine free journals Spine best journals Spine top journals Spine free medical journals Spine famous journals Spine Google Scholar indexed journals Dynamic Immobilization articles Dynamic Immobilization Research articles Dynamic Immobilization review articles Dynamic Immobilization PubMed articles Dynamic Immobilization PubMed Central articles Dynamic Immobilization 2023 articles Dynamic Immobilization 2024 articles Dynamic Immobilization Scopus articles Dynamic Immobilization impact factor journals Dynamic Immobilization Scopus journals Dynamic Immobilization PubMed journals Dynamic Immobilization medical journals Dynamic Immobilization free journals Dynamic Immobilization best journals Dynamic Immobilization top journals Dynamic Immobilization free medical journals Dynamic Immobilization famous journals Dynamic Immobilization Google Scholar indexed journals sinusoid curves articles sinusoid curves Research articles sinusoid curves review articles sinusoid curves PubMed articles sinusoid curves PubMed Central articles sinusoid curves 2023 articles sinusoid curves 2024 articles sinusoid curves Scopus articles sinusoid curves impact factor journals sinusoid curves Scopus journals sinusoid curves PubMed journals sinusoid curves medical journals sinusoid curves free journals sinusoid curves best journals sinusoid curves top journals sinusoid curves free medical journals sinusoid curves famous journals sinusoid curves Google Scholar indexed journals biomechanical chain joint articles biomechanical chain joint Research articles biomechanical chain joint review articles biomechanical chain joint PubMed articles biomechanical chain joint PubMed Central articles biomechanical chain joint 2023 articles biomechanical chain joint 2024 articles biomechanical chain joint Scopus articles biomechanical chain joint impact factor journals biomechanical chain joint Scopus journals biomechanical chain joint PubMed journals biomechanical chain joint medical journals biomechanical chain joint free journals biomechanical chain joint best journals biomechanical chain joint top journals biomechanical chain joint free medical journals biomechanical chain joint famous journals biomechanical chain joint Google Scholar indexed journals osteoporosis fractures articles osteoporosis fractures Research articles osteoporosis fractures review articles osteoporosis fractures PubMed articles osteoporosis fractures PubMed Central articles osteoporosis fractures 2023 articles osteoporosis fractures 2024 articles osteoporosis fractures Scopus articles osteoporosis fractures impact factor journals osteoporosis fractures Scopus journals osteoporosis fractures PubMed journals osteoporosis fractures medical journals osteoporosis fractures free journals osteoporosis fractures best journals osteoporosis fractures top journals osteoporosis fractures free medical journals osteoporosis fractures famous journals osteoporosis fractures Google Scholar indexed journals scoliosis articles scoliosis Research articles scoliosis review articles scoliosis PubMed articles scoliosis PubMed Central articles scoliosis 2023 articles scoliosis 2024 articles scoliosis Scopus articles scoliosis impact factor journals scoliosis Scopus journals scoliosis PubMed journals scoliosis medical journals scoliosis free journals scoliosis best journals scoliosis top journals scoliosis free medical journals scoliosis famous journals scoliosis Google Scholar indexed journals spine surgeon articles spine surgeon Research articles spine surgeon review articles spine surgeon PubMed articles spine surgeon PubMed Central articles spine surgeon 2023 articles spine surgeon 2024 articles spine surgeon Scopus articles spine surgeon impact factor journals spine surgeon Scopus journals spine surgeon PubMed journals spine surgeon medical journals spine surgeon free journals spine surgeon best journals spine surgeon top journals spine surgeon free medical journals spine surgeon famous journals spine surgeon Google Scholar indexed journals
Article Details
1. Introduction
To date, accidents and injuries have reached epidemic proportions. In polytrauma, individual segments of the spine are often affected. At that time, the emergency physician must determine whether the spinal injury is stable or unstable. This is followed by surgical or conservative therapy. The old realisation that in fractures require the immobilisation of the affected bone and the two adjacent joints, unless osteosynthesis has been performed, has been well-established. Massages are forbidden. I observed that in the case of stable spinal injuries, segmentational orthosis is administered in practice, because there is no suitable dynamic apparatus for the necessary immobilisation of the entire spine. However, doing so neglects the facts that the spine is a biomechanical chain joint, which can be divided into segments only anatomically, and not physiologically. An injury of one segment affects the statics of the entire spine. Altough the osteosynthesis of vertebrae or implantation achieves a relatively stable consolidation, many problems may occur in the postoperative period, outside the knowledge of the surgeon, due to premature mobilization. I offer a solution to surgeons in the accompanying article. I myself have carried out a medical survey of a support apparatus that I developed in a critical situation at a certain point in time [1-8].
2. Medical Case
A 46-year-old man of asthenic constitution fell backwards from the height of 4 metres while working in the garden due to a break in the side of a wodden ladder. He fell on two parallel 5 cm thick concrete curbs and hit his cervical and lumbar spine segments. A head injury did not occur. Due to the impact to his neck, he experienced forceful paraesthesia lasting several seconds in all exremities, as characteristic of an electric shock with several thousand Volts. Fully conscious without dyspnoea he realised that his lungs are not being ventilated, i. e. he was not breathing. Therefore, he moved and fell a further ten centimeters down. Now he could breathe in air. When he recovered and because the pain was still tolerable, he quickly ran, bent forwards, to the 15 m remote living room and lay on wood floors for 4 days in home care. The first week he took diazepame, chlorzoxason/paracetamol.
The strong hardening of the abdominal muscle (defanse) loosend after three days. On the fourth day he was taken on a stretcher to the Orthopaedic Clinic. An X-ray ivestigation found injury of the C6, 7 Th5, and L1, 2 vertebrae. Because the injuries of the vertebrae appeared stable, a plaster corset with a Minerva cast was indicated. The patient decided against hospitalisation because with the help of the plaster immobilisation he became partially mobile. At home, the plaster deformed in the lying down position due to summer heat and sweating. Paresthesia of the lower extremities apeared. Therefore, we removed his 7, 5 kg heavy plaster 9 days after the injury and replaced it with an innovative prototype of a dynamic support device for the entire spine. The biggest challenge then was to exactly form the sinusoid curves on the brace. The patient was able to walk to the restroom. In the standing position, the brace also relieves the gravitational pressures. Three weeks after the injury; during a shorter drive with the city bus, the patient had to stand on his toes due to painful vertical jolts. After four weeks of 24 hours a day use of the device a rigidity of the spine was detected. In the fifth week, progressive phasing out of the orthosis followed, and then 14 days everyday the patient received physiotherapy in a warm sea water pool. Half a year after the accident unpleasant neuralgic pain was occasionally present in the right dermatome C8. It has now been 30 years from this event. The injured man is 77 years old and has stated that he has had no problems with his spine. He was performing various physical work, but he did not do sports.
3. Characteristics
The orthosis is a 2, 30 kg heavy apparatus consisting of:
A: a dorsal metal support, extending from the back of the neck to the sacral bone.
B: a thoracic + abdominal pelot
C: a Shanz kravat.
The construction enables the regulation of the individual components with each other within a length of 4 cm. This solves the issue of serial production in the sizes S, L, X, XL, as a kit.

Figure 1: Frontal view.
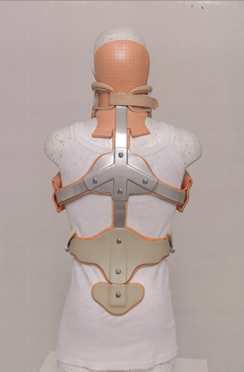
Figure 2: Dorsal view.

Figure 3: View from the left.

Figure 4: View from the right.
4. Application
In the abdominal position of the patient, the sinusoid curves of the spine are copied by means of a handy universal stencil. The dedicated tools are then used to accurately form the dorsal longitudinal metal strip. A 3D scan is not required. The so-called Shanz kravat can be individually adjusted in volume. A removable piece is integrated into the underchin that can be removed prior to eating to allow for the chewing of food. Perspiration of the cervical area is guaranteed.
- The armpit pads affect the muscle tone of the shoulder ring.
- The pressure of the brace on the spinous processes is neutralised with the surrouding area.
- In the lying down position, the brace easily dips into the bed mattress.
- The redressing of metal strips is always possible due to the internal elasticity of the aluminium alloy.
Each case of application is formed strictly individually post-injury or prior to surgery. The indication is determined by the surgeon. The mental stability of the injured person is also important. In post-surgical convalescence, this method restricts unwantend bending between vertebrae along the entire spine. which are subsequently often the cause of insufficient restitution ad integrum, even though a stable osteosynthesis was performed on time.
5. Material
- Straps-(aluminium alloy with appropriate internal elasticity)-6 pcs
- Plastazote
- Stainless steel screws M6 with lens head(hex key system)-6 pcs
- Detachable threes-part Shanz cravat(Velcro system)
- Tensioning metal spring clips(4 pcs)
- Pull straps(4 pcs)
- Plastics and aluminium pelots(5pcs)
- Two plastazote axillary pads
- Glue
- Rivets
6. Discussion
A phobia of this kind of immobilisation is redundant. Also due to the public exposure in domestic care. The original purpose was to allow the professional immobilisation of the injured spine in the hospital with the aim of the patient continuing their treatment in domestic and outpatient care. Further research on the importance of the correct immobilisation of this biomechanical chain joint will confirm the importance of the correct post-traumatic easing of streched tissues due to the sudden effects of physical force. The formation of individual sinusoid forms from case to case is made possible with dental-technical accuracy. If necessary, appropriate redressing is possible if the treatment lasts for a longer time. I note that after injuries, there is an exaggerated push for premature inclusion of mobilisation and such offers. The injury must be treated properly and in line with the doctrine. Analgesic are not recomended. Extensions of the indications for this type of orthosis have not been investigated. By extensions I mean juvenile scoliosis, osteoporosis fractures, broom-shaped fractures of vertebrae due to blast effects on pilot of jets, soldiers, etc.
7. Conclusion
For establishment in practice, the consensus of experts of the profession and other important stakeholders is necessary, with the aim of not harming the affected.
References
- Gyton Arthur C. Textbook of Medical Physiology. Fourth Edition, Saunders Company, Philadelphia, London, Toronto (1957).
- Allgöver M. Allgemeine und spezielle Chirurgie. Springer Verlag Berlin, Heidelberg GmbH (2013).
- Müller M E, Allgöwer M, Willenegger H, et al. Manual der Osteosynthese. Springer Verlag Berlin, Heidelberg, New York (1977).
- Böhler Lorenz. Die Technik der Knochenbehandlung Band I. II. Auflage 1963, Nachdruck 1996. Verlag Wilhelm Maudrich Wien, München, Bern (1937).
- Saegesser Max. Spezielle chirurgische Therapie, achte vollständig neu bearbeitete Auflage mit 3343 Abbildungen. Jahr 1972 Verlag Hans Huber Bern, Stuttgart, Wien.
- Saegesser Max. Chirurgische Operationslehre. Springer Verlag Berlin, Heidelberg (1935).
- Pernkopf Eduard. Atlas of Topographical and Applied Human Anatomie. Urban & Schwarzenberg, Edited by Helmut Ferner MD (1979).
- Hartmann W&Co GmbH&CoKG. Aluminium Legierungen, Grundlagewissen.
