CADASIL or MS? Consider “Red Flags” but Avoid a Misdiagnosis: Case Series of a Concomitant Diagnosis
Article Information
Morena Emanuele1, Lucchini Matteo2, Romano Carmela1, Petrucci Simona3, Tartaglia Matteo4, Morosetti Roberta2, Conte Antonella4,5, Buscarinu Maria Chiara1,6, Romano Silvia1, Salvetti Marco1,5, Mirabella Massimiliano2, Ristori Giovanni1,6
1Centre for Experimental Neurological Therapies (CENTERS), Department of Neurosciences, Mental Health and Sensory Organs, Sapienza University of Rome, Rome, Italy
2Fondazione Policlinico Universitario "A. Gemelli" IRCCS, Istituto di Neurologia, Università Cattolica del Sacro Cuore, Rome, Italy
3Department of Neurology and Psychiatry, Sapienza University of Rome, Rome, Italy
4Department of Human Neurosciences, Sapienza University of Rome, Rome, Italy
5Istituto di Ricovero e Cura a Carattere Scientifico (IRCCS) Istituto Neurologico Mediterraneo Neuromed, Pozzilli, Italy
6Neuroimmunology Unit, Istituto di Ricovero e Cura a Carattere Scientifico (IRCCS) Fondazione Santa Lucia, Rome, Italy
*Corresponding Author: Morena Emanuele, Centre for Experimental Neurological Therapies (CENTERS), Department of Neurosciences, Mental Health and Sensory Organs, Sapienza University of Rome, Rome, Italy.
Received: 11 July 2022; Accepted: 12 August 2022; Published: 05 September 2022
Citation: Morena Emanuele, Lucchini Matteo, Romano Carmela, Petrucci Simona, Tartaglia Matteo, Morosetti Roberta, Conte Antonella, Buscarinu Maria Chiara, Romano Silvia, Salvetti Marco, Mirabella Massimiliano, Ristori Giovanni. CADASIL or MS? Consider “Red Flags” but Avoid a Misdiagnosis: Case Series of a Concomitant Diagnosis. Archives of Clinical and Medical Case Reports 6 (2022): 618-621.
View / Download Pdf Share at FacebookAbstract
Cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy (CADASIL) is a monogenic autosome-dominant disease with chronic clinical course. Rarely, CADASIL may present with atypical relapsing-remitting manifestations, cerebral and spinal white matter lesions, mimicking inflammatory CNS disease as multiple sclerosis (MS). The rarely co-occurrence of MS and CADASIL may represent a hard challenging diagnosis even for an expert neurologist. Here, we present a case series of two patients with CADASIL showing MRI pattern overlapping MS. They were the only case of co-occurrence of CADASIL and MS in their own family. Both patients were treated with anti-inflammatory and anti-platelet drugs, mostly with good response. Pathogenic hypothesis highlights that genetic events, related to monogenic disease, may expose CNS antigens with a consequent self-immune attack. In CADASIL, the function of Notch3 receptor showed a consistent interplay with immune system activity. Indeed, certain mutations of Notch3 receptor show abnormal upregulation of specific pro-inflammatory patterns. However, even if it is not possible to determinate if the proinflammatory activity may be promoted by pathogenic mutations in Notch3, the "apparent" difference between MS and “inflammatory CADASIL” could be considered more semantic than etiologic.
Keywords
<p>CADASIL; CNS Inflammation; Inflammatory CADASIL; Multiple Sclerosis; Monogenetic Disease; Neurodegeneration</p>
CADASIL articles; CNS Inflammation articles; Inflammatory CADASIL articles; Multiple Sclerosis articles; Monogenetic Disease articles; Neurodegeneration articles
CADASIL articles CADASIL Research articles CADASIL review articles CADASIL PubMed articles CADASIL PubMed Central articles CADASIL 2023 articles CADASIL 2024 articles CADASIL Scopus articles CADASIL impact factor journals CADASIL Scopus journals CADASIL PubMed journals CADASIL medical journals CADASIL free journals CADASIL best journals CADASIL top journals CADASIL free medical journals CADASIL famous journals CADASIL Google Scholar indexed journals COVID-19 articles COVID-19 Research articles COVID-19 review articles COVID-19 PubMed articles COVID-19 PubMed Central articles COVID-19 2023 articles COVID-19 2024 articles COVID-19 Scopus articles COVID-19 impact factor journals COVID-19 Scopus journals COVID-19 PubMed journals COVID-19 medical journals COVID-19 free journals COVID-19 best journals COVID-19 top journals COVID-19 free medical journals COVID-19 famous journals COVID-19 Google Scholar indexed journals CNS Inflammation articles CNS Inflammation Research articles CNS Inflammation review articles CNS Inflammation PubMed articles CNS Inflammation PubMed Central articles CNS Inflammation 2023 articles CNS Inflammation 2024 articles CNS Inflammation Scopus articles CNS Inflammation impact factor journals CNS Inflammation Scopus journals CNS Inflammation PubMed journals CNS Inflammation medical journals CNS Inflammation free journals CNS Inflammation best journals CNS Inflammation top journals CNS Inflammation free medical journals CNS Inflammation famous journals CNS Inflammation Google Scholar indexed journals Sarcoidosis articles Sarcoidosis Research articles Sarcoidosis review articles Sarcoidosis PubMed articles Sarcoidosis PubMed Central articles Sarcoidosis 2023 articles Sarcoidosis 2024 articles Sarcoidosis Scopus articles Sarcoidosis impact factor journals Sarcoidosis Scopus journals Sarcoidosis PubMed journals Sarcoidosis medical journals Sarcoidosis free journals Sarcoidosis best journals Sarcoidosis top journals Sarcoidosis free medical journals Sarcoidosis famous journals Sarcoidosis Google Scholar indexed journals Inflammatory CADASI articles Inflammatory CADASI Research articles Inflammatory CADASI review articles Inflammatory CADASI PubMed articles Inflammatory CADASI PubMed Central articles Inflammatory CADASI 2023 articles Inflammatory CADASI 2024 articles Inflammatory CADASI Scopus articles Inflammatory CADASI impact factor journals Inflammatory CADASI Scopus journals Inflammatory CADASI PubMed journals Inflammatory CADASI medical journals Inflammatory CADASI free journals Inflammatory CADASI best journals Inflammatory CADASI top journals Inflammatory CADASI free medical journals Inflammatory CADASI famous journals Inflammatory CADASI Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals CT articles CT Research articles CT review articles CT PubMed articles CT PubMed Central articles CT 2023 articles CT 2024 articles CT Scopus articles CT impact factor journals CT Scopus journals CT PubMed journals CT medical journals CT free journals CT best journals CT top journals CT free medical journals CT famous journals CT Google Scholar indexed journals Breast Cancer articles Breast Cancer Research articles Breast Cancer review articles Breast Cancer PubMed articles Breast Cancer PubMed Central articles Breast Cancer 2023 articles Breast Cancer 2024 articles Breast Cancer Scopus articles Breast Cancer impact factor journals Breast Cancer Scopus journals Breast Cancer PubMed journals Breast Cancer medical journals Breast Cancer free journals Breast Cancer best journals Breast Cancer top journals Breast Cancer free medical journals Breast Cancer famous journals Breast Cancer Google Scholar indexed journals Multiple Sclerosis articles Multiple Sclerosis Research articles Multiple Sclerosis review articles Multiple Sclerosis PubMed articles Multiple Sclerosis PubMed Central articles Multiple Sclerosis 2023 articles Multiple Sclerosis 2024 articles Multiple Sclerosis Scopus articles Multiple Sclerosis impact factor journals Multiple Sclerosis Scopus journals Multiple Sclerosis PubMed journals Multiple Sclerosis medical journals Multiple Sclerosis free journals Multiple Sclerosis best journals Multiple Sclerosis top journals Multiple Sclerosis free medical journals Multiple Sclerosis famous journals Multiple Sclerosis Google Scholar indexed journals Neurodegeneration articles Neurodegeneration Research articles Neurodegeneration review articles Neurodegeneration PubMed articles Neurodegeneration PubMed Central articles Neurodegeneration 2023 articles Neurodegeneration 2024 articles Neurodegeneration Scopus articles Neurodegeneration impact factor journals Neurodegeneration Scopus journals Neurodegeneration PubMed journals Neurodegeneration medical journals Neurodegeneration free journals Neurodegeneration best journals Neurodegeneration top journals Neurodegeneration free medical journals Neurodegeneration famous journals Neurodegeneration Google Scholar indexed journals
Article Details
1. Background
Cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy (CADASIL) is an autosomal-dominant, small-vessel disease, clinically characterized by transient ischemic attacks and/or strokes, migraine and cognitive impairment possibly leading to pseudobulbar paralysis and progressive dementia. CADASIL is caused by pathogenic mutations in NOTCH3 gene, located on chromosome 19p13, which encodes a large single-pass transmembrane receptor expressed in vascular smooth muscle cells. More than 200 different pathogenic mutations, localized throughout exons 2-24 of the NOTCH3 gene have been already described in CADASIL patients [1]. Most of them lead to a variation in the number of cysteine aminoacidic residues in one of the 34 epidermal growth factor-like repeats (EGFrs) domains of the Notch3 protein. In patients the Notch3 receptor extracellular domain has been demonstrated to accumulate in the vessel wall with a direct or indirect toxic effect on vascular smooth muscle cells, leading to degeneration [2]. A clinical diagnosis of CADASIL is supposed when the patient shows the typical clinical manifestations associated with a specific magnetic resonance imagining (MRI) pattern of the brain: 1) diffuse white matter lesions involving in particular the temporal pole, 2) microbleeds in the semioval center, thalamus, basal ganglia and pons and 3) lacunar infarcts [3]. The clinical suspect, complicated by the extreme phenotypic variability, may be supported by the identification of GOM (Granular Osmiophilic Material) on skin biopsy (specificity of 100%, and variable sensitivity from 45% to 100%) [4]. However, only the genetic test can confirm the diagnosis. CADASIL may present with a relapsing-remitting course and with cerebral and brainstem white-matter lesions, being among the several white matter diseases mimicking multiple sclerosis (MS) [5]. The co-occurrence of MS and CADASIL, that are known rarely to co-exist [6], represents a hard challenge for the diagnostic process even for an expert neurologist.
2. Case1
A 38 years-old woman came to our attention in April 2011 for rigidity and numbness in right hand and leg. She had no familial history of neurological diseases. Her medical history was unremarkable except for celiac disease, diagnosed in 2010 by esophagogastroduodenoscopy (EGDS) and digiunal biopsy (Marsh IIIC *) [7]. She performed a lumbar puncture that showed an increased cellularity in the absence of oligoclonal bands, and a brain and spinal MRI that showed multiple T2/FLAIR hyperintense lesions in periventricular white matter, semioval centrum, bilateral putamen, frontal white matter and spinal cord with no enhancement after gadolinium contrast. Autoantibody panel for vasculitis resulted negative. Somatosensory and Visual Evoked Potentials were normal, while Motor Evoked Potentials evidenced a delay of central nervous system motor conduction in right leg. When she came at our board, the neurological examination evidenced Babinski sign, brisk tendon reflexes and light spastic hypertonus on her right side. In May 2011, after a gastrointestinal infection, the patient presented acute stiffness in right leg; a new MRI revealed three additional lesions (two cerebral and one new spinal lesions), without contrast enhancement. A diagnosis of MS was posed based on McDonald Criteria 2010 [8] and a therapy with Glatiramer Acetate three times a week was started. In February 2012, the patient presented a new clinical relapse with hypoesthesia on her left side and was given intravenous high dose corticosteroids treatment with subsequent complete regression of symptoms. After three months, she manifested a new relapse characterized by paresthesia in both hands and Lhermitte sign. Spinal MRI showed a new cervical (C4-C5) lesion with contrast-enhancement. Symptoms partially regressed after a new treatment with i.v. corticosteroids. Considering the progression of the disease course, she switched to a second-line therapy with Natalizumab with a good clinical response for three years, without changes in neurologic examination (EDSS 1) and MRI. Following JCV seroconversion, the patient stopped natalizumab on June 2015 and started dimethylfumarate after 5 weeks. Clinical examinations and MRI were stable in the next years, but an important decrease of lymphocyte count appeared in February 2017, leading to a new switch to interferon beta (IFN) i.m. once a week, which was started in August 2017. In December 2017, her mother had a stroke at the age of 62. The absence of conventional cerebrovascular risk factors and the brain MRI pattern (a recent capsular infarct, associated to multiple lacunar infarcts, severe diffused white matter hyperintensities involving temporal lobes and several microbleeds on gradient echo images – T2 weighted imaging) were strongly suggestive for CADASIL. The suspect was subsequently confirmed by the identification of the heterozygous c.421C>T, p. (Arg141Cys) substitution in NOTCH3 gene (rs1174625611). The same pathogenetic variant was detected in our patient by Sanger sequencing in February 2018. Given this result and the stability of the clinical-MRI conditions, we decided to stop the Disease-modifying therapy (DMT). However, three months later the patient developed hyposthenia in her lower limbs, and her spinal cord MRI showed a new enhancing lesion (Figure 1). This new clinical and radiological activity prompted to perform a new lumbar puncture: we found unmatched oligoclonal bands (OCBs) in the CSF and an elevated Kappa Free Light Chain Index (KFLC) index [9]. Considering the coexistence of MS and CADASIL and the report of side effects to INF beta and acetylsalicylic acid, we started treatment with subcutaneous glatiramer acetate 40 mg three times a week and antiplatelet therapy with clopidogrel 75 mg a day. The patient has been clinically and radiologically stable during the last two years of follow-up, and she remains currently worsening-free.
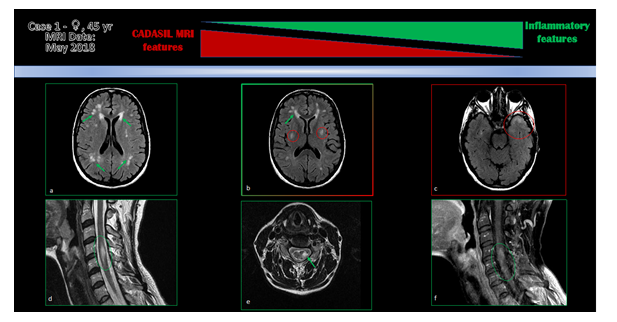
Figure 1: MRI images. T2/FLAIR (a,b,c): a. Centrum Semiovale (CSO); b. Deep basal ganglia; c. Anterior temporal lobe. T2-weighted images (d,e): d. Sagittal section; e. Axial section. T1 post gadolinium-enhancement: f. Sagittal section. Green arrow: inflamation lesions; Red circle: CADASIL features.
3. Case 2
In 2016 a 49-year old healthy man experienced progressive bilateral legs weakness, with gait limitation. He performed a brain MRI showing confluent hyperintensities in T2 sequences in periventricular, deep white matter and basal ganglia areas. After contrast injection, some small lesions got enhancement. Multiple spinal hyperintensities in T2 sequences were found at C2, C2-C3, C4-C5, between D3-D6 and D8-D9, without any enhancement. Clinical and MRI investigations allowed to pose diagnosis of MS, referring to revised McDonald’s criteria of 2010 [8]. At that time, the patient presented a EDSS of 4.0 and he started oral therapy with Teriflunomide. Due to radiological disease activity without clinical worsening (stable EDSS 4.0), he shifted to higher efficacy DMT in May 2019, starting fingolimod. Further MRI activity, along with clinical disease progression in July 2020 (EDSS 5.0) and in September 2020 (EDSS 6.0), required further vertical therapy shift to ocrelizumab in 2020. When his dizygotic twin showed a symptomatology characterized by recurrent migraine and memory loss episodes, a brain MRI was performed and a diagnosis of CADASIL was considered. The molecular analysis of NOTCH3 identified the heterozygous c.3226C>T (p.Arg1076Cys) pathogenic variant in NOTCH3 (rs1438626607), confirming the clinical diagnosis of CADASIL. The case 2 thus came at our neurogenetics unit for a genetic counseling about CADASIL in 2020. He had never reported CADASIL-related clinical features such as migraine, stroke, cognitive impairment, epilepsy, gate disturbances or other symptoms. However, considering his family history, he underwent molecular analysis to investigate the presence of the familial variant on his DNA. As in his brother, the NOTCH3 c.3226C>T (p.Arg1076Cys) substitution was confirmed in the heterozygous state also in our patient. At that point, we decided to deepen his previous MS diagnosis performing a lumbar puncture and a new brain and spine MRI (Figure 2), 5 months far from the last ocrelizumab infusion. The CSF analysis showed the presence of 14 OCB, with a unique intracranial synthesis pattern, and a high G-globulin antibody concentration (308.8 mg/dL, with a normal value < 34.0). Considering the co-occurrence of MS and CADASIL, we decided to continue the DMT with Ocrelizumab and we started an antiplatelet therapy with acetylsalicylic acid 100 mg/die. To date, patient repeated a new brain and spinal MRI in 2021 showing absence of inflammatory activity and is clinically stable (EDSS 6.0).
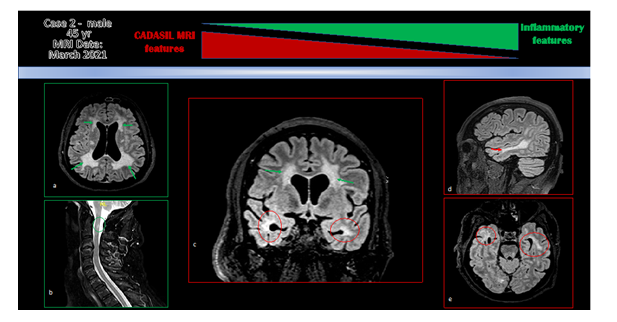
Figure 2: MRI images. T2/FLAIR: a. Centrum Semiovale (CSO); b. Tervical spinal cord; c. CSO and polar lobe. d. Temporal lobe, sagittal section; f. Temporal lobe, axial section. Green arrow: inflammatory lesions; Red circle: CASASIL features.
4. Conclusion
We observed two cases of CNS inflammatory disease with a concomitant diagnosis of CADASIL. These cases may be difficult to diagnose considering the rarity of CADASIL condition, the poor genotype-phenotype correlation, the heterogeneity of symptoms and age of onset of this inherited disease. The first case of co-occurrence of CADASIL and MS was reported by Carone et al. as an atypical presentation of CADASIL, misdiagnosed with MS [10]. A diagnosis of MS, according to the McDonald’s criteria, requires evidence of spatial and temporal dissemination of the disease, but also “no better explanation” for other etiologies [8]. Instead, migraine and familial history are two feature guides for CADASIL diagnostic suspect. In both our cases, the clinical presentation, the MRI pattern and the excellent clinical response to i.v. steroid therapy favored an inflammatory diagnostic hypothesis. No clinical features instead leaned for a CADASIL diagnosis except for the positive familial history. Concerning MRI findings, they were of difficult interpretation for the differential diagnosis. In both cases, some atypical features for MS, like hyperintensities in deep basal ganglia or in anterior temporal lobe, that seemed more typical for CADASIL, co-existed with brain and spinal cord lesions (that are rarely seen in CADASIL [11]), supporting the diagnosis of MS (Figure 1, 2). The description of CADASIL and MS co-existence cases increased in the recent years, opening a debate about a possible relationship between monogenic diseases and inflammatory disease of CNS [12]. Pathogenic hypotheses highlight that genetic defects, like mutation of Notch3 protein [13], or cytopathies such as Leber’s disease [14], or POLG mutations [15], could promote demyelinating-like diseases, suggesting a key role of the exposure of CNS antigens with a consequent self-immune attack [16]. Notably, the function of Notch3 receptor in CADASIL disease showed a consistent interplay with immune system activity. Notch3 appears involved in T cell response regulation, specifically in myelin reactive T-cells, contributing to the encephalitogenic potential of autoreactive T cells [13]. Moreover, its abnormal upregulation showed a pro-inflammatory activity [17]. It is known that the Notch3 receptor activity favors the activation of the Nuclear Factor kappa B (NF-κB), promoting pro-inflammatory gene expression in activated macrophages, and its inhibition can reduce myelin-activated T-cell response [18]. Taking these data into account, it might be expected that mutations which increase, or do not change, Notch3 activity can predispose to inflammation. Intriguingly, functional studies in CADASIL patient with NOTCH3 p.R1076C mutation showed an abnormal upregulation of pro-inflammatory NF-κB target genes in VSMCs, partly attributed to constitutive activation of Notch3 signalling [17]. This mutation, present in patient of case 2, is localized in the EGFr 27 domain and it has been already described in further 7 unrelated CADASIL families worldwide [17], [19], [20]. Conversely, the more common pathogenic c.421C>T (p.Arg141Cys) variant in the EGFr 3 domain, identified in our case 1 and in many other families with CADASIL worldwide, causes a reduced expression of the Notch3 receptor on the cell surface, higher intracellular aggregates but no alteration of Notch3 signalling, suggesting that the pathology may be due to abnormal Notch3 trafficking and localization rather than signalling dysfunction [21]. Overall, to our knowledge, this is the first time that inflammatory phenotypic features have been described in patients carrying these two variants. To date it is not possible to determinate if the proinflammatory activity may be promoted only by the pathogenic mutations in NOTCH3 or need the contemporary intervention of other genetic and non-genetic modifier factors. Nevertheless, the relevant role for NOTCH3 in inflammation has been already proven. Maybe the presence of modifier factors could explain the intrafamilial phenotypic variability described in the two reported families. Considering these hypothesis, the "apparent" difference between MS and “inflammatory CADASIL” could be semantic rather than etiologic. In this perspective DMTs used in MS might be beneficial for these patients [7] and, reciprocally, the selective modulation of Notch3-dependent pathways may represent a possible therapeutic option in MS [13].
References
- Mizuno T, Mizuta I, Watanabe-Hosomi et al. Clinical and Genetic Aspects of CADASIL. Front. Aging Neurosci 12 (2020): 91.
- Rutten JW, Haan J, Terwindt GM, et al. Interpretation of NOTCH3 mutations in the diagnosis of CADASIL. Expert Rev. Mol. Diagn 14 (2014): 593-603.
- Stojanov D, Aracki-Trenkic A, Vojinovic S, et al. Imaging characteristics of cerebral autosomal dominant arteriopathy with subcortical infarcts and leucoencephalopathy (CADASIL). Bosn. J. Basic Med. Sci 15 (2015): 1-8.
- Morroni M, Marzioni D, Ragno M, et al. Role of Electron Microscopy in the Diagnosis of Cadasil Syndrome: A Study of 32 Patients. PLoS ONE 8 (2013).
- Di Donato I, Bianchi S, De Stefano N, et al. Cerebral Autosomal Dominant Arteriopathy with Subcortical Infarcts and Leukoencephalopathy (CADASIL) as a model of small vessel disease: update on clinical, diagnostic, and management aspects. BMC Med 15 (2017): 41.
- Schiess N, Huether K, Szolics M, et al. Multiple sclerosis or ‘inflammatory CADASIL?: Case Report and review of the literature. Clin. Neurol. Neurosurg 173 (2018): 196-199.
- Rubio-Tapia A, Hill ID, Kelly CP, et al. ACG clinical guidelines: diagnosis and management of celiac disease. Am. J. Gastroenterol 108 (2013): 656-676.
- Polman CH, Reingold SC, Banwell B, et al. Diagnostic criteria for multiple sclerosis: 2010 Revisions to the McDonald criteria. Ann. Neurol 69 (2011): 292-302.
- Rosenstein I, Rasch S, Axelsson M, et al. Kappa free light chain index as a diagnostic biomarker in multiple sclerosis: A real-world investigation, J. Neurochem 159 (2021): 618-628.
- Carone DA, CADASIL and multiple sclerosis: A case report of prolonged misdiagnosis. Appl. Neuropsychol. Adult 24 (2017): 294-297.
- Motolese F, Rossi M, Gangemi E, et al. CADASIL as Multiple Sclerosis Mimic: A 48-year-old man with severe leukoencephalopathy and spinal cord involvement. Mult. Scler. Relat. Disord 41 (2020): 102014.
- Abedi KV, Li J, Malik MT, et al. CADASIL vs. Multiple Sclerosis: Is It Misdiagnosis or Concomitant? A Case Series. Front. Neurol 11 (2020): 860.
- Jurynczyk M, Jurewicz A, Raine CS, et al. Notch3 Inhibition in Myelin-Reactive T Cells Down-Regulates Protein Kinase Cθ and Attenuates Experimental Autoimmune Encephalomyelitis. The Journal of Immunology 180 (2008): 2634-2640.
- La Russa et al. Leber’s hereditary optic neuropathy associated with a multiple-sclerosis-like picture in a man. Mult. Scler. Houndmills Basingstoke Engl 17 (2011): 763-766.
- Echaniz-Laguna A, Chassagne M, de Sèze J, et al. POLG1 variations presenting as multiple sclerosis. Arch. Neurol 67 (2010).
- Collongues N, Derache N, Blanc F, et al. Inflammatory-like presentation of CADASIL: a diagnostic challenge. BMC Neurol 12 (2012): 78.
- Ling Y, De Guio F, Jouvent E, et al. Clinical correlates of longitudinal MRI changes in CADASIL. J. Cereb. Blood Flow Metab 39 (2019): 1299-1305.
- López-López S, Monsalve EM, de Ávila MJR, et al. NOTCH3 signaling is essential for NF-κB activation in TLR-activated macrophages. Sci. Rep 10 (2020).
- Bianchi S, Zicari E, Carluccio A, et al. CADASIL in central Italy: a retrospective clinical and genetic study in 229 patients. J. Neurol 262 (2015): 134-141.
- Liao YC et al. Characterization of CADASIL among the Han Chinese in Taiwan: Distinct Genotypic and Phenotypic Profiles. PloS One 10 (2015): e0136501.
- Karlström H, Beatus P, Dannaeus K, et al. A CADASIL-mutated Notch 3 receptor exhibits impaired intracellular trafficking and maturation but normal ligand-induced signaling. Proc. Natl. Acad. Sci. U. S. A 99 (2002): 17119-17124.
