Biomarkers of Allogeneic Cell Therapy in Acute Steroid-Refractory Graftversus- Host Disease
Article Information
Gil Gonen-Yaacovi, PhD*, and Oscar Segurado, MD, PhD
ASC Therapeutics, Milpitas, CA, USA
*Corresponding Author: Gil Gonen-Yaacovi, PhD, Associate Director, Clinical and Regulatory Affairs, ASC Therapeutics, 521 Cottonwood Dr, Milpitas, CA 95035, USA
Received: 27 September 2021; Accepted: 11 October 2021; Published: 22 October 2021
Citation: Gil Gonen-Yaacovi, Oscar Segurado. Biomarkers of Allogeneic Cell Therapy in Acute Steroid-Refractory Graftversus-Host Disease. Archives of Clinical and Medical Case Reports 5 (2021): 724-732.
View / Download Pdf Share at FacebookAbstract
Cell therapy requires precise screening and monitoring of patients to ensure that the transfer of either autologous or allogeneic cells to a patient results in a therapeutic effect to targeted organs or tissues. One well-established application of cell therapy is allogeneic hematopoietic stem cell transplantation (allo-HSCT) to treat hematologic conditions. A common complication following allo-HSCT, however, is the development of acute graft-versus-host disease (aGVHD), which leads to substantial morbidity and mortality. There is currently no widely effective treatment for aGVHD, but cell therapy using decidua stromal cells (DSCs) has shown success in academic-driven clinical studies. The introduction of selective biomarkers of cellular, immune, and disease response to DSCs can help select the right patient, the right treatment, and the right monitoring in the treatment of aGVHD. In this article, we discuss the relevance of precision medicine as an essential approach to leverage biomarkers as well as other clinical aspects that optimize safety and efficacy of cell therapy in aGVHD.
Keywords
Acute graft-versus-host disease; Allogeneic hematopoietic stem cell transplantation; Cell therapy; Decidua stromal cells
Acute graft-versus-host disease articles; Allogeneic hematopoietic stem cell transplantation articles; Cell therapy articles; Decidua stromal cells articles
Acute graft-versus-host disease articles Acute graft-versus-host disease Research articles Acute graft-versus-host disease review articles Acute graft-versus-host disease PubMed articles Acute graft-versus-host disease PubMed Central articles Acute graft-versus-host disease 2023 articles Acute graft-versus-host disease 2024 articles Acute graft-versus-host disease Scopus articles Acute graft-versus-host disease impact factor journals Acute graft-versus-host disease Scopus journals Acute graft-versus-host disease PubMed journals Acute graft-versus-host disease medical journals Acute graft-versus-host disease free journals Acute graft-versus-host disease best journals Acute graft-versus-host disease top journals Acute graft-versus-host disease free medical journals Acute graft-versus-host disease famous journals Acute graft-versus-host disease Google Scholar indexed journals disease articles disease Research articles disease review articles disease PubMed articles disease PubMed Central articles disease 2023 articles disease 2024 articles disease Scopus articles disease impact factor journals disease Scopus journals disease PubMed journals disease medical journals disease free journals disease best journals disease top journals disease free medical journals disease famous journals disease Google Scholar indexed journals Allogeneic hematopoietic stem cell transplantation articles Allogeneic hematopoietic stem cell transplantation Research articles Allogeneic hematopoietic stem cell transplantation review articles Allogeneic hematopoietic stem cell transplantation PubMed articles Allogeneic hematopoietic stem cell transplantation PubMed Central articles Allogeneic hematopoietic stem cell transplantation 2023 articles Allogeneic hematopoietic stem cell transplantation 2024 articles Allogeneic hematopoietic stem cell transplantation Scopus articles Allogeneic hematopoietic stem cell transplantation impact factor journals Allogeneic hematopoietic stem cell transplantation Scopus journals Allogeneic hematopoietic stem cell transplantation PubMed journals Allogeneic hematopoietic stem cell transplantation medical journals Allogeneic hematopoietic stem cell transplantation free journals Allogeneic hematopoietic stem cell transplantation best journals Allogeneic hematopoietic stem cell transplantation top journals Allogeneic hematopoietic stem cell transplantation free medical journals Allogeneic hematopoietic stem cell transplantation famous journals Allogeneic hematopoietic stem cell transplantation Google Scholar indexed journals Gastrointestinal articles Gastrointestinal Research articles Gastrointestinal review articles Gastrointestinal PubMed articles Gastrointestinal PubMed Central articles Gastrointestinal 2023 articles Gastrointestinal 2024 articles Gastrointestinal Scopus articles Gastrointestinal impact factor journals Gastrointestinal Scopus journals Gastrointestinal PubMed journals Gastrointestinal medical journals Gastrointestinal free journals Gastrointestinal best journals Gastrointestinal top journals Gastrointestinal free medical journals Gastrointestinal famous journals Gastrointestinal Google Scholar indexed journals hematopoietic stem cell articles hematopoietic stem cell Research articles hematopoietic stem cell review articles hematopoietic stem cell PubMed articles hematopoietic stem cell PubMed Central articles hematopoietic stem cell 2023 articles hematopoietic stem cell 2024 articles hematopoietic stem cell Scopus articles hematopoietic stem cell impact factor journals hematopoietic stem cell Scopus journals hematopoietic stem cell PubMed journals hematopoietic stem cell medical journals hematopoietic stem cell free journals hematopoietic stem cell best journals hematopoietic stem cell top journals hematopoietic stem cell free medical journals hematopoietic stem cell famous journals hematopoietic stem cell Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals CT articles CT Research articles CT review articles CT PubMed articles CT PubMed Central articles CT 2023 articles CT 2024 articles CT Scopus articles CT impact factor journals CT Scopus journals CT PubMed journals CT medical journals CT free journals CT best journals CT top journals CT free medical journals CT famous journals CT Google Scholar indexed journals Cell therapy articles Cell therapy Research articles Cell therapy review articles Cell therapy PubMed articles Cell therapy PubMed Central articles Cell therapy 2023 articles Cell therapy 2024 articles Cell therapy Scopus articles Cell therapy impact factor journals Cell therapy Scopus journals Cell therapy PubMed journals Cell therapy medical journals Cell therapy free journals Cell therapy best journals Cell therapy top journals Cell therapy free medical journals Cell therapy famous journals Cell therapy Google Scholar indexed journals Radioembolization articles Radioembolization Research articles Radioembolization review articles Radioembolization PubMed articles Radioembolization PubMed Central articles Radioembolization 2023 articles Radioembolization 2024 articles Radioembolization Scopus articles Radioembolization impact factor journals Radioembolization Scopus journals Radioembolization PubMed journals Radioembolization medical journals Radioembolization free journals Radioembolization best journals Radioembolization top journals Radioembolization free medical journals Radioembolization famous journals Radioembolization Google Scholar indexed journals Decidua stromal cells articles Decidua stromal cells Research articles Decidua stromal cells review articles Decidua stromal cells PubMed articles Decidua stromal cells PubMed Central articles Decidua stromal cells 2023 articles Decidua stromal cells 2024 articles Decidua stromal cells Scopus articles Decidua stromal cells impact factor journals Decidua stromal cells Scopus journals Decidua stromal cells PubMed journals Decidua stromal cells medical journals Decidua stromal cells free journals Decidua stromal cells best journals Decidua stromal cells top journals Decidua stromal cells free medical journals Decidua stromal cells famous journals Decidua stromal cells Google Scholar indexed journals
Article Details
Abbreviations:
aGVHD- acute graft-versus-host disease; allo-HSCT- allogeneic hematopoietic stem cell transplantation; BSA- body surface area; dd-cfDNA- donor-derived cell-free DNA; DSC- decidua stromal cell; IFN-γ- interferon gamma; IL- interleukin; MSC- mesenchymal stromal cell; REG3α- regenerating islet-derived protein 3-α; ST2- suppressor of tumorigenicity-2
1. Introduction
Allogeneic cell therapies are an important type of precision medicine–an approach to disease treatment and prevention offering tailored, individualized care that considers a patient’s genetics, lifestyle, and environment [1]. Allogeneic cell therapy involves the transfer of whole donor cells to a patient, with the aim of restoring or altering his or her own diseased or damaged cells, delivering treatment to a specific organ or tissue, or providing immunoregulatory functionality. Myriad cell types are available for cell therapies, with hematopoietic stem cell transplantation for the treatment of hematologic diseases being among the most common [2-4].
The transfer of new cells to a patient imposes toxicity and immune-related concerns, which are evidenced by the development of acute graft-versus-host disease (aGVHD) following allogeneic hematopoietic stem cell transplantation (allo-HSCT). Decidua stromal cells (DSCs) are used in cell therapy technologies that have shown promise in many diseases, including aGVHD; markers that describe how the transferred cells behave in the body, how the immune system responds to the new cells, and how the patient responds to the treatment.
2. Acute Graft-Versus-Host Disease and Decidua Stromal Cells
Allo-HSCT is the first-line treatment for several benign and malignant hematopoietic cancers and diseases [5]. Following allo-HSCT, aGVHD is the most frequent comorbidity [6, 7] and may cause considerable mortality [8-10]. Approximately half of patients who receive allo-HSCT develop aGVHD [9, 11, 12]; the disorder is fatal in up to 10% of these individuals [12], making it the second leading cause of death (after disease relapse) for allo-HSCT recipients [13]. Simply, in aGVHD, donor blood cells target the neoplastic cells, but they also mount an immune response against healthy cells and tissues in the host. This response usually appears within the first three months after allo-HSCT and primarily affects the skin, gastrointestinal tract, and liver with rash, secretory diarrhea, and abnormal cholestatic liver function, which present as the prominent signs of disease [9, 14].
Acute GVHD is staged according to the number of organs affected and the extent of involvement [9]. Treatment for aGVHD usually consists of steroids with or without calcineurin inhibitors, but only about half of patients respond to this treatment [7, 9]. Currently, only one second-line therapy is approved for treatment of steroid-refractory aGVHD: ruxolitinib, a selective inhibitor of members of the Janus tyrosine kinase family (JAK1 and JAK2), it has demonstrated improved overall response and failure-free survival compared with other therapies [15]. Simply, JAK proteins are important signal tranducers and activators of transcription that impact the development, proliferation, and activation of immune cell types that are important in the progression of aGVHD [16]. Other treatment attempts with cytostatic agents, immunomodulatory agents, and biologic therapies have demonstrated low response rates and only short-term survival, often only a few months [6, 7, 17, 18].
Several other second-line cell therapies have been developed for treating steroid-refractory aGVHD, including mesenchymal stromal cells (MSCs) and DSCs [8]. MSCs, which are present in adult and fetal tissues, are multipotent, non-hematopoietic stem cells that can differentiate into various cell types. They are often isolated from bone marrow [19], but can also be found in adipose tissue, peripheral blood, dental pulp, endometrium, amniotic fluid, fetal membranes, the placenta, and the umbilical cord as well as other tissues and secretions [20-22]. MSCs possess immunomodulatory and anti-inflammatory processes and are able to avoid triggering an immune response. These characteristics make MSCs successful components of treatments for many diseases, but they have not been effective in preventing relapse or mortality in aGVHD [19, 23].
DSCs are similar to MSCs, but they are uniquely derived from fetal membranes of the maternal placenta [24]. Compared with MSCs, DSCs display more potent immunosuppressive properties and do not display any differentiation potential [8], which are key benefits in the treatment of aGVHD. Specifically, DSCs exhibit decreased production of interferon gamma (IFN-γ) and interleukin (IL)-17, increased secretion of anti-inflammatory IL-10, and higher expression of integrins [3, 4]. They suppress alloreactivity, enhance expression of programmed cell death ligands 1 and 2, and increase the frequency of regulatory T cells [23, 25, 26]. Furthermore, they do not upregulate human leukocyte antigen-II after IFN-γ stimulation [8]. Together, these features make DSCs ideal candidates for treating aGVHD (Figure 1).
Several studies have been conducted using DSCs in aGVHD and chronic GVHD (cGVHD), and promising results have been achieved (Table 1) [4, 8, 17, 27, 28]. Additionally, the studies have demonstrated that treatment with DSCs is safe and effective. During the long-term follow-up of an academic-driven study, patients receiving DSCs for steroid-refractory aGVHD achieved survival rates that were substantially greater than those achieved with traditional treatments, including MSCs, with a 1-year survival rate close to 80% and a 4-year survival rate near 60% [17].
|
Author and year of study |
Objective |
Population |
Dose |
Results |
|
Ringden, 2013 [4] |
Test initial efficacy of DSCs |
9 patients with acute GVHD |
2x106 |
Efficacy: 75% ORR Safety: DSCs were safe to infuse with no acute toxic effects |
|
Erkers, 2015 [8] |
Test efficacy and biodistribution of DSCs in humans |
3 patients with chronic GVHD |
1-2.8x106 |
Efficacy: 2 patients achieved PR, and 1 patient did not respond; DSCs were initially located in the lungs, followed by dissemination to the liver and spleen Safety: No adverse events were reported |
|
Baygan, 2017 [27] |
Test safety and adverse events of DSCs |
44 patients with aGVHD in the DSC group and 40 with aGVHD in the control group |
0.9-2.9 x106 |
Safety: DSCs are safe to use in aGVHD with no major adverse events; no differences between DSCs and control in the frequency of infections, relapse, or cause of death |
|
Ringden, 2018 [17] |
Test efficacy of DSCs in different supplements |
38 patients with aGVHD (24 with SR-aGVHD) |
0.9-2.9 x106 |
Efficacy: ORR at Day 28 was 82% and 1-year OS was 63% Safety: no major adverse events were reported |
|
Sadeghi, 2019 [28] |
Test long-term safety of DSCs |
21 patients with aGVHD |
0.9-2.9 x106 |
Efficacy: DSCs are efficient in the long run with 66% 4-year OS Safety: no major adverse events or serious infections were reported |
|
ASC930 in Patients With Steroid-Refractory Acute Graft Versus Host Disease (SR-aGVHD) [41] |
To evaluate efficacy of ASC930 in participants with SR-aGVHD |
Planned for ~60 participants |
Planned for 0.9-2.9 x106 |
TBD |
aGVHD, acute graft-versus-host disease; DSCs, decidua stromal cells; ORR, overall response rate; OS, overall survival; PR, partial response; SR, steroid-refractory.
Table 1: Clinical studies conducted to date and planned [4, 8, 15, 27, 28].
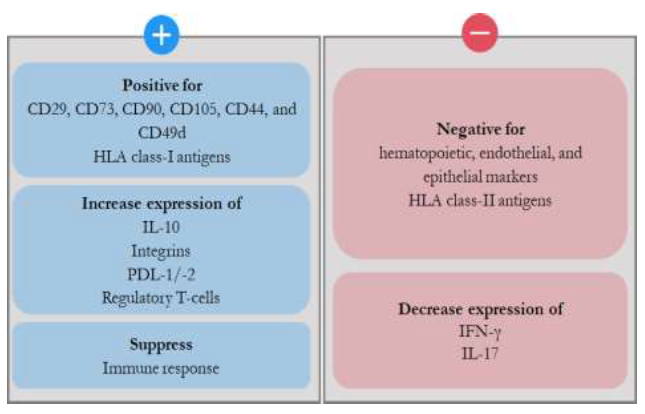
Figure 1: Properties and mechanisms of action of DSCs [3, 4, 8, 23-26].
CD, cluster of differentiation biomarkers; HLA, human leukocyte antigen; IL, interleukin; IFN, interferon; PDL, programmed cell death ligand
3. Biomarkers of Cell Therapy
A limitation of using DSCs in aGVHD is a lack of understanding of how the cells behave in the body and how they affect the immune system of the host. Biomarkers are an essential component to clarify the mechanisms of the treatment regimens. Infused DSCs can be radiolabeled to measure their presence in various organs over time. In a pilot study of three patients with severe cGVHD after stem cell transplantation, DSCs were labeled with 111indium and their distribution was tracked for 48 hours. DSCs traveled to the lungs, then to the spleen and liver [8]; they did not appear to travel to the organs typically affected by cGVHD such as the intestine, esophagus, or skin. This method of assessing the effect of DSCs might be applied to larger populations and used as a basis for further clinical study, but its invasive nature makes it cumbersome for routine use.
An alternative means of measuring DSCs in the body is the quantification of donor-derived cell-free DNA (dd-cfDNA), which is viable as a surveillance tool to describe the behavior of DSCs. After allo-HSCT, dd-cfDNA is detectable and quantifiable in the recipient’s blood. The ability to detect and differentiate donor and recipient DNA exploits differences between the genotypes of the donor and the recipient. This noninvasive test can detect precursors to organ injury following transplantation by measuring the progression of inflammation [29–31]. Quantification of dd-cfDNA can predict organ rejection as well as direct personalized immunotherapeutic treatment. Currently, dd-cfDNA is primarily used in solid-organ transplants, but work is underway to validate its application in allo-HSCT. There is no recognized threshold for the concentration of dd-cfDNA that indicates the onset of aGVHD, and more work is required to clarify the timing and measurement of dd-cfDNA relative to allo-HSCT [29].
4. Biomarkers of Immune Response
Immune response to DSCs can be measured with flow cytometry, which estimates immune response by simultaneously identifying and quantifying cellular systems and measuring the functional attributes of individual cells [32]. Mass cytometry pairs flow cytometry with mass spectrometry, offering high dimensional and unbiased examination of the immune system that is not limited by the number of parameters that can be analyzed at once [33]. Mass cytometry has been critical in elucidating how the immune system reconstitutes after allo-HSCT: it and allows individual cells to be described according to phenotype and function on the basis of cell-surface and intracellular proteins [5, 34]. Patterns of immune reconstitution and post-transplant complications, including aGVHD, have been recognized using mass cytometry, leading to an appreciation of the complex, individualized biological processes that occur after allo-HSCT and the discovery of prognostic immune biomarkers [5]. Related technologies, including proteomics, multiomics, and single-cell “omics,” are also important to understand the effects of cell-therapy expression in individual cells [35-37], and these technologies could be applied in assessing immune response to DSC therapy.
5. Biomarkers of Disease Response
Disease response in aGVHD can be measured using surrogate safety and efficacy endpoints. Two biomarkers of endothelial dysfunction, which predict long-term outcomes, can be estimated from whole blood: suppressor of tumorigenicity-2 (ST2) and regenerating islet-derived protein 3-α (REG3α) [38, 39]. Both proteins have been identified in high concentrations in the blood of patients with aGVHD and are predictors of increased mortality. REG3α is produced in the pancreas and small intestine and displays enhanced expression during inflammation and is thought to be directly related to endothelial damage caused by aGVHD. REG3α is specifically useful in aGVHD that presents in the gastrointestinal system because this protein can distinguish between aGVHD-related and other causes of diarrhea. ST2 is part of the IL-1 family that is secreted by endothelial and epithelial cells as well as fibroblasts and has been associated with treatment-resistant aGVHD [40].
Both ST2 and REG3α are incorporated into the MAGIC (Mount Sinai Acute GVHD International Consortium) algorithm probability [39], which is a tool for assessing mortality after aGVHD treatment. The timing, methods, and cut-off values of laboratory measurement of these biomarkers need to be clarified and standardized to increase their application in aGVHD.
6. Conclusions
The prediction, diagnosis, and treatment of aGVHD after allo-HSCT is a clinical need that can be met with cell therapy that uses DSCs. To ensure the safe and effective use of cell therapies, though, sensitive, specific, and standardized boimarkers are needed to guide treatment and to assess response. We must understand how the cells behave in the body, how the immune system responds to the cells, and how the patient responds to the treatment. Finding the the right treatment for the right patient and employing the right monitoring will ensure the success of cell therapy.
References
- US Food and Drug Administration. Precision medicine. September 27, 2018. https://www.fda.gov/medical-devices/in-vitro-diagnostics/precision-medicine. Accessed (2021).
- Xie M, Viviani M, Fussenegger M. Engineering precision therapies: lessons and motivations from the clinic. Synth Biol 6 (2020): ysaa024.
- Karlsson H, Erkers T, Nava S, et al. Stromal cells from term fetal membrane are highly suppressive in allogeneic settings in vitro. Clin Exp Immunol 167 (2012): 543-555.
- Ringdén O, Erkers T, Nava S, et al. Fetal membrane cells for treatment of steroid-refractory acute graft-versus-host disease. Stem Cells 31 (2013): 592-601.
- Stern L, McGuire H, Avdic S, et al. Mass cytometry for the assessment of immune reconstitution after hematopoietic stem cell transplantation. Front Immunol 9 (2018): 1672.
- Berger M, Biasin E, Saglio F, et al. Innovative approaches to treat steroid-resistant or steroid refractory GVHD. Bone Marrow Transplant 42 (2008): S101-S105.
- Malard F, Huang X-J, Sim JPY. Treatment and unmet needs in steroid-refractory acute graft-verus-host disease. Leukemia 34 (2020): 1229-1240.
- Erkers T, Kaipe H, Nava S, et al. Treatment of severe chronic graft-versus-host disease with decidual stromal cells and tracing with (111) indium radiolabeling. Stem Cells Dev 24 (2015): 253-263.
- Jacobsohn DA, Vogelsang GB. Acute graft versus host disease. Orphanet J Rare Dis 2 (2007): 35.
- Srinagesh HK, Ferrera JLM. MAGIC biomarkers of acute graft-versus-host disease: biology and clinical application. Best Pract Res Clin Haematol 32 (2019): 101111.
- Ferrara JLM, Levine JE, Reddy P, et al. Graft-versus-host disease. Lancet 373 (2009): 1550-1561.
- Jamil MO, Mineishi S. State-of-the-art acute and chronic GVHD treatment. Int J Hematol 101 (2015): 452-466.
- Nassereddine S, Rafei H, Elbahesh E, et al. Acute graft versus host disease: a comprehensive review. Anticancer Res 37 (2017): 1547-1555.
- Gooptu M, Antin JH. GVHD prophylaxis 2020. Front Immunol 12 (2021): 605726.
- Huarte E, Peel M, Juvekar A, et al. Ruxolitinib, a JAK1/JAK2 selective inhibitor, ameliorates acute and chronic steroid-refractory GvHD mouse models. Immunotherapy 13 (2021): 977-987.
- Schroeder MA, Choi J, Staser K, et al. The role of Janus kinase signaling in graft-versus-host disease and graft versus leukemia. Biol Blood MaroowMarrow Transplant 24 (2018): 1125-1134.
- Ringden O, Baygan A, Remberger M, et al. Placenta-derived decidua stromal cells for treatment of severe acute graft-versus-host disease. Stem Cells Transl Med7 (2018): 325-331.
- Roddy JVF, Haverkos BM, McBride A, et al. Tocilizumab for steroid refractory acute graft-versus-host disease. Leuk Lymphoma 57 (2016): 81-85.
- Li T, Luo C, Zhang J, et al. Efficacy and safety of mesenchymal stem cells co-infusion in allogeneic hematopoietic stem cell transplantation: a systematic review and meta-analysis. Stem Cell Res Ther12 (2021): 246.
- Horwitz EM, Andreef M, Frassoni F. Mesenchymal stem cells. Curr Opin Hematol13 (2006): 419-425.
- Murray IR, Peault B. Q&A: mesenchymal stem cells where do they come from and is it important? BMC Biol13 (2015): 99.
- Andrzejewska A, Lukomska B, Janowski M. Concise review: mesenchymal stem cells: from roots to boost. Stem Cells37 (2019): 855-864.
- Introna M, Golay J. Tolerance to bone marrow transplantation: do mesenchymal stromal cells still have a future for acute or chronic GvHD? Front Immunol11 (2020): 609063.
- Hass R, Kasper C, Bohm S, et al. Different populations and sources of human mesenchymal stem cells (MSC): a comparison of adult and neonatal tissue-derived MSC. Cell Commun Signal9 (2011): 12.
- Peyvandi F, Kunicki T, Lillicrap D. Genetic sequence analysis of inherited bleeding diseases. Blood122 (2013): 3423-3431.
- Meggyes M, Miko E, Szigeti B, et al. The importance of the PD-1/PD-L1 pathway at the maternal-fetal interface. BMC Pregnancy Childbirth19 (2019): 74.
- Baygan A, Aronsson-Kurttila W, Moretti G, et al. Safety and side effects of using placenta-derived decidual stromal cells for graft-versus-host disease and hemorrhagic cystitis. Front Immunol8 (2017): 795.
- Sadeghi B, Remberger M, Gustafsson B, et al. Long-term follow-up of a pilot study using placenta-derived decidua stromal cells for severe acute graft-versus-host disease. Biol Blood Marrow Transplant25 (2019): 1965-1969.
- Bloom RD, Bromberg JS, Poggio ED, et al. Cell-free DNA and active rejection in kidney allografts. J Am Soc Nephrol 28 (2017): 2221-2232.
- Grskovic M, Hiller DJ, Eubank LA, et al. Validation of a clinical-grade assay to measure donor-derived cell-free DNA in solid organ transplant recipients. J Mol Diagn18 (2016): 890-902.
- Seeto RK, Fleming JN, Dholakia S, et al. Understanding and using Allosure donor derived cell-free DNA. Biophys Rev12 (2020): 917-924.
- Zhang T, Warden AR, Li Y, et al. Progress and applications of mass cytometry in sketching immune landscapes. Clin Transl Med 10 (2020): e206.
- Gadalla R, Noamani B, MacLeod BL, et al. Validation of CyTOF against flow cytometry for immunological studies and monitoring of human cancer clinical trials. Front Oncol9 (2019): 415.
- Spitzer MH, Nolan GP. Mass cytometry: single cells, many features. Cell165 (2016): 780-791.
- Jing Y, Liu J, Ye Y, et al. Multi-omics prediction of immune-related advserse events during checkpoint immunotherapy. Nat Commun 11 (2020): 4946.
- Linnarsson S, Teichmann SA. Single-cell genomics: coming of age. Genome Biol 17 (2016): 97.
- Rabilloud T, Potier D, Pankaew S, et al. Single-cell profiling identified pre-existing CD19-negative subclones in a B-ALL patient with CD19-negative relapse after CAR-T therapy. Nat Commun12 (2021): 865.
- Nomura S, Ishii K, Fujita S, et al. Associations between acute GVHD-related biomarkers and endothelial cell activation after allogeneic hematopoietic stem cell transplantation. Transpl Immunol 44 (2017): 27-32.
- Srinagesh HK, Ferrera JLM. MAGIC biomarkers of acute graft-versus-host disease: Biology and clinical application. Best Pract Res Clin Haematol 32 (2019): 101111.
- Solan L, Kwon M, Carbonell D, et al. ST2 and REG3α as predictive biomarkers after haploidentical stem cell transplantation using post-transplantation high-dose cyclophosphamide. Front Immunol 10 (2019): 2338.
- https://clinicaltrials.gov/ct2/show/NCT04883918
