Assessment of Inappropriate Prescribing to Elderly Patients in an Internal Medicine Ward According to the 2019 Beers Criteria
Article Information
Cátia Pereira*, Ana Guiomar, Alexandra Cunha, Catarina Alves Cunha, José Pedro Barbosa, Jorge Fortuna
Coimbra University Hospital Center, Coimbra, Portugal
*Corresponding author: Cátia Pereira, Coimbra University Hospital Center, Rua Irmã Lúcia nº2, 3º esquerdo frente, 3030-491, Coimbra, Portugal
Received: 12 May 2020; Accepted: 22 May 2020; Published: 3 June 2020
Citation:
Cátia Pereira, Ana Guiomar, Alexandra Cunha, Catarina Alves Cunha, José Pedro Barbosa, Jorge Fortuna. Assessment of Inappropriate Prescribing to Elderly Patients in an Internal Medicine Ward According to the 2019 Beers Criteria. Archives of Internal Medicine Research 3 (2020): 124-130.
View / Download Pdf Share at FacebookAbstract
Drug prescribing in older adults presents a serious challenge in medical clinical practice as this group of patients is particularly susceptible to drug-related side effects. American Geriatrics Society Beers Criteria serve as guidelines for clinicians to prevent potentially inappropriate prescribing in adults aged 65 years and older. Along with other tools and clinical judgment, these criteria can be used as a prescribing quality indicator. The purpose of this study was to determine the prevalence of potentially inappropriate prescription and the most common potentially inappropriate medications prescribed among older patients at admission in an internal medicine ward, as well as its rate of discontinuation by clinicians by the time of discharge. This assessment was made in light of the American Geriatrics Society 2019 Updated AGS Beers Criteria. Data from three internal medicine wards of the University of Coimbra Hospital Center were analyzed during July 2019, resulting in a total of 153 selected patients. The mean age was 85 (SD 7.32) years and most of the patients were female (58%). On admission, 75% of patients had at least one potentially inappropriate drug prescribed. At discharge, the drug was discontinued in 21% of these patients. One potentially inappropriate drug was introduced in 16% of patients. More than ever, we must acknowledge deprescribing as an important component of a good prescribing continuum. Our results highlight clinicians’ poor recognition of potentially harmful drugs in the elderly and the urge to define a strategy that allows appropriate therapeutic adjustments in this age group.
Keywords
Drug Prescribing, Potentially Inappropriate Medications, Older Adults, Age-Related, Beers Criteria
Drug Prescribing articles, Potentially Inappropriate Medications articles, Older Adults articles, Age-Related articles, Beers Criteria articles
Article Details
Abbreviations:
AGS-American Geriatrics Society; PIMs-Potentially inappropriate medications; SD- Standard Desviation; PPI-Proton-pump inhibitors; NSAID-Nonsteroidal anti-inflammatory drug
1. Introduction
Drug prescribing in the elderly presents unique challenges. Older patients are more likely to have multiple chronic diseases and hence need several medications, which increases the risk of adverse drug reactions and interactions [1]. Age-related changes in pharmacodynamics and pharmacokinetics (such as increased volume of distribution or decreased drug clearance) may lead to larger drug half-lives and therefore prolonged effects of certain drugs [2, 3]. It is well known that some drug classes, such as anticholinergics, benzodiazepines, antipsychotics and opioids, may have significant adverse effects in the elderly population [3]. The American Geriatrics Society (AGS) Beers Criteria compile evidence-based recommendations into a list of potentially inappropriate medications (PIMs) that should be avoided or considered with caution among older adults. This tool aims to guide health professionals in making decisions about therapeutic options but should never dictate how drugs are prescribed [4, 5].
The primary aim of this study was to estimate how frequently clinicians do recognize and suspend potentially inappropriate drugs prescribed among older patients, by determining the frequency of discontinuation at the time of discharge of an internal medicine ward. Discontinuation referred to those patients who had a potentially inappropriate drug prescribed at admission but had this drug suspended at the time of discharge. The secondary aims included the prevalence of PIMs at admission, the frequency of initiation of newly prescribed PIMs by the time of discharge, as well as the relation between the length of hospital stay and the frequency of discontinuation of PIMs. This assessment was made in light of the updated 2019 Beers Criteria.
2. Materials and Methods
An observational retrospective study was conducted involving elderly patients (aged 65 and above) who were admitted in an internal medicine ward at the Coimbra University Hospital Centre during July 2019. Demographic and clinical data were collected from electronic medical records of all elderly patients who were hospitalized during the study period. Clinical variables included dependency status, length of stay, comorbidities and PIMs prescribed at admission and discharge. Exclusion criteria included patients who died before discharge and palliative care patients. Statistical analysis was performed with IBM SPSS® Statistics 26. Normally distributed continuous variables were described by their mean and standard deviation. Other continuous variables were described by their median and range (total and interquartile). Categorical variables were described by the absolute and relative frequencies of each category. Spearman’s correlation coefficient was used to assess the correlation between a pair of non-normal continuous variables. Patients’ medications were reviewed from a medical database at hospital admission and at discharge, according to the recently updated 2019 Beers Criteria.
3. Results
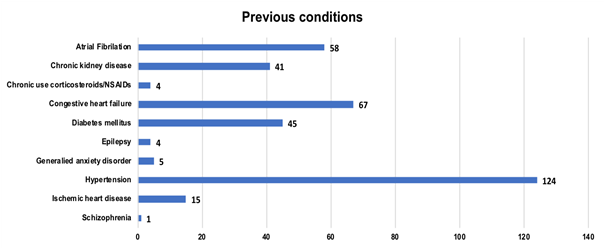
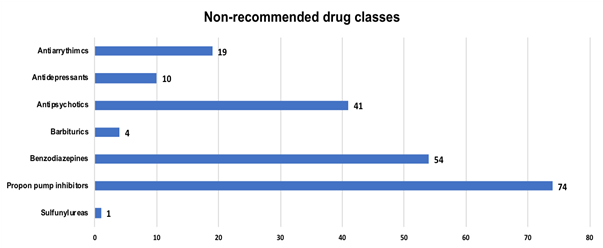
From an initial pool of 163 patients who fulfilled the age criteria, we excluded those who died during the hospital stay (8 patients) and those who had been admitted for palliative care (2 patients). Median length of hospital stay was 8 days; total range was 1-64 days, with an interquartile range of 5-13.5 days. Most of the patients were female (58%), with a mean age of 85 years (SD 7.3). Among the patients under study, 71% were admitted from home, while 29% were admitted from nursing homes. Approximately 35% experienced moderate limitations in daily living activities and 31% were totally dependent. Table 1 summarizes patients’ demographic and clinical characteristics. Various chronic conditions were identified. We decided to report those conditions in which the use of certain drugs was an exception to the Beers Criteria recommendations. Among those, arterial hypertension (n=124), heart failure (n=67), atrial fibrillation (n=58), diabetes mellitus (n=45) and chronic kidney disease (n=41) were the most frequently documented Figure 1. Of the total of 153 patients, 115 (75%) had PIMs among their usual medication on admission and according to Beers Criteria. Proton-pump inhibitors (PPI) were the most prescribed PIMs at admission (48%; n=74), followed by short and intermediate acting benzodiazepines (29%; n=45) and second-generation antipsychotics (25%; n=38) Figure 2. Of a total of 115 patients with PIMs at admission, only 25 (21%) had these drugs discontinued at discharge. Second-generation antipsychotics and short-intermediate acting benzodiazepines were the most commonly discontinued drugs. On admission, 38 patients were taking second-generation antipsychotics and 45 patients were taking short-intermediate acting benzodiazepines. By the time of discharge, second-generation antipsychotics were discontinued in 8 of those patients (21%) and short-intermediate acting benzodiazepines were discontinued in 7 (16%). The frequency of discontinuation of PIMs is presented in Table 2. At discharge, at least one additional potentially inappropriate drug was prescribed to 16% of patients. PPI were the most inadequately drug class newly prescribed at the time of discharge (n=10), followed by second-generation antipsychotic drugs (n=6). From the group of PPI, pantoprazole was the one most frequently prescribed. Spearman's correlation coefficient between the length of stay and the difference in the number of drugs between admission and discharge was weak and not statistically significant (ρ=0.086 and ρ=0.288).
|
Variable |
Measure (n=153) |
|
Age (years) |
|
|
Mean (SD) |
84.59 (7.342) |
|
Range |
67–100 |
|
Gender – n(%) |
|
|
Male |
64 (42%) |
|
Female |
89 (58%) |
|
Length of stay (days) |
|
|
Median |
8 |
|
Range |
1–64 |
|
Interquartile Range |
5–13.5 |
|
Dependence in daily activities – n(%) |
|
|
Totally dependent |
48 (31.4%) |
|
Moderately dependent |
54 (35.3%) |
|
Independent |
51 (33.3%) |
|
Residence – n(%) |
|
|
Independent or with family |
108 (70.6%) |
|
Nursing home |
45 (29.4%) |
Table 1: Demographics and general information.
|
Drug class |
Frequency of prescription at admission |
Out of prescription on discharge |
Discontinued percentage on discharge |
|
Antiarrhythmics |
19 |
2 |
10.5% |
|
Antidepressants |
10 |
1 |
10% |
|
Anti-inflammatory drugs |
3 |
2 |
66.7% |
|
Antipsychotics |
|||
|
First generation |
3 |
1 |
33.3% |
|
Second generation |
38 |
8 |
21.1% |
|
Barbiturics |
4 |
0 |
0% |
|
Benzodiazepines |
|||
|
Short- and intermediate-acting |
45 |
7 |
15.6% |
|
Long-acting |
9 |
5 |
55.6% |
|
Non-benzodiazepine sedative drugs |
1 |
1 |
100% |
|
Proton pump inhibitors |
74 |
3 |
4.1% |
|
Sulfunylureas |
1 |
1 |
100% |
Table 2: Discontinuation of PIM drugs at discharge by drug class.
4. Discussion
The results of this study show that the prescription of potentially inappropriate drugs was highly frequent among older adults (75%) on hospital admission. PPI was the most prescribed drug, followed by short-intermediate acting benzodiazepines and second-generation antipsychotics. Other studies involving the elderly have obtained similar results [6-8]. Khamis et al found that 76.6% of patients were taking at least one potentially inappropriate medication during hospitalization [6]. A previous study in Japan [7] reported that 63% of hospitalized elderly patients were receiving PIMs. In both studies, the most commonly identified PIMs were PPI. Our data is also consistent with findings of a recent portuguese study based on the population of an internal medicine ward indicating that PPI was the most prescribed drug (36%), followed by antihyperglycemic agents (17%), antipsychotics (15.9%) and benzodiazepines (14.6%) [8]. We believe that the high frequency of inappropriate PPI prescription may result from the fact that certain diagnoses such as erosive esophagitis often go unrecorded in patients' clinical records. However, we did not take into account those patients who were considered high risk patients, such as chronic corticosteroid and nonsteroidal anti-inflammatory drug (NSAID) users and therefore we assume that, in the rest of the population studied, these drugs were indeed inappropriately prescribed. Inappropriate benzodiazepine use was also highly frequent, and this may be due to the lack of proper recording of diagnoses such as alcohol and benzodiazepine withdrawal and generalized anxiety disorder. There is a strong recommendation against prescribing antipsychotics and benzodiazepines to older patients, particularly when not indicated, since its use is associated with risk of dependence, cognitive deficits, falls resulting in fractures and overall mortality [9]. In our sample, these two drug classes were frequently used.
Despite being the most discontinued drug classes, antipsychotic medications and benzodiazepines were only discontinued in approximately 20% of cases and we consider these results to be insufficient given the potential side effects of these medications. We observed that PPI prescription remained a frequent practice by the time of discharge, since only 3 of a total of 74 PPI prescribed at admission were discontinued. This is particularly concerning, given the fact that long-term use of PPI has been positively associated with the development of some diseases such as Clostridioides difficile infections, dementia, pneumonia, kidney disease and bone mineral low density [10]. No correlation was found between long-term hospitalization and rate of PIMs discontinuation. Moreover, we observed that 16% patients had been prescribed with at least one new potentially inappropriate drug at discharge and again, PPI were the most inadequately drug class prescribed. Low discontinuation rates independent of hospital length of stay and initiation of PIMs at discharge might reflect clinicians’ inability to distinguish between appropriate and inappropriate drugs. These results should be interpreted in the context of several limitations. As with all retrospective studies, our results may be affected by confoundings. This is a small scale study, limited to a single center and with a small sample size, therefore the results cannot be easily generalised. Probably the main limitation of this study is the fact that drugs classified as PIMs may not be necessarily inappropriate. Regardless the fact that we have excluded potentially inappropriate drugs that were considered appropriate under specific situations according to Beers Criteria, such as in certain diseases or conditions, we observed that more than two-thirds of the patients were taking at least one potentially inappropriate drug at admission. Nevertheless, we must take into account that some PIMs may be appropriately prescribed in certain medical conditions that were not included in patients’ database due to incomplete or incorrect medical records. Prospective studies are needed where drug regimens must be reviewed by multidisciplinary teams who should be able to identify actual inappropriate drugs before a drug is discontinued. Our study did not include potentially clinically important drug-drug interactions to be avoided in older adults neither PIMs based on kidney function. Further studies should be conducted to assess these parameters using a multicenter approach.
The present study highlights the poor recognition of potentially harmful drugs in the elderly. Clinicians often feel uncomfortable discontinuing medications, especially if they did not prescribe them initially and also when the patient seems to be tolerating. At this point, and as suggested in other studies, we should be particularly aware to identify medications that have limited therapeutic benefit and patients at a higher risk of adverse drug effects. Since validated tools that allow for appropriate therapeutic adjustment in this age group are not available, the development of new therapeutic review strategies is needed, possibly with the introduction of multidisciplinary teams for this specific purpose [3]. More than ever, we should recognize the deprescribing process as a chance to identify and discontinue drugs that could cause harm. This is an important part of the good prescribing continuum and should be seen as a positive patient-centered intervention [2].
Conflict of Interest
Without any conflict of interest
References
- Hubbard R, Peel N, Scott I, et al. Polypharmacy among older inpatients in Australia. Med J Aust 202 (2015): 373-377.
- Scott IA, Hilmer SN, Reeve E, et al. Reducing inappropriate polypharmacy: the pro-cess of deprescribing. JAMA Intern Med 175 (2015): 827-834.
- Williams S, Miller G, Khoury R, et al. Rational deprescribing in the elderly. Ann Clin Psychiatry 31 (2019): 144-152.
- American Geriatrics Society 2012 Beers Criteria Update Expert Panel. American Geriatrics Society updated Beers Criteria for potentially inappropriate medication use in older adults. J Am Geriatr Soc 60 (2012): 616-631.
- Roughead EE, Anderson B, Gilbert AL. Potentially inappropriate prescribing among Australian veterans and war widows/widowers. Intern Med J 37 (2007): 402-405.
- Kose E, Hirai T, Seki T, et al. Role of potentially inappropriate medication use in rehabilitation outcomes for geriatric patients after strokes. Geriatr Gerontol Int 18 (2018): 321-328.
- Khamis S, Abdi AM, Uzan A, et al. Applying beers criteria for elderly patients to assess rational drug use at a university hospital in Northern Cyprus. J Pharm Bioallied Sci 11 (2019): 133-141.
- Urzal J, Pedro AB, Oliveira I, et al. Inappropriate Prescribing to Elderly Patients in an Internal Medicine Ward. Acta Med Port 32 (2019): 141-148.
- Markota M, Rummans TA, Bostwick JM, et al. Benzodiazepine use in older adults: dangers, management, and alternative therapies. Mayo Clin Proc 91 (2016): 1632-1639.
- Jaynes M, Kumar AB. The risks of long-term use of proton pump inhibitors: a critical review. Therapeutic Advances in Drug Safety (2019): 1-13.