Acquired Cryptorchidism in a 12-Year-old with X-Linked Ichthyosis (XLI)
Article Information
Fjolla Hyseni1, Ali Guy2, Guri Hyseni3, Breta Kotorri4, Blerona Shaipi5, Ermira Aliu6, Valon Vokshi 7, Loran Rakovica8, Essa A Mohamed9, Ibrahim A Bajwa10, Mumin M Omar11, Juna Musa12
1Medical Resercher, NYU Langone Health, New York, USA
2Clinical Assistant Professor, Department of Rehabilitation Medicine, NYU Grossman School of Medicine, New York, USA
3Department of Pediatric Surgery, Hospital and University Clinical Service of Kosova, Prishtina, Kosova
4Medical Doctor, University of Prishtina, Faculty of Medicine, Kosovo
5Medical Doctor, University of Medicine, Tirana, Albania
6Medical Doctor, Radiologist, Department of Radiology, General Hospital, Gjilan, Kosovo
7Department of Anesthesiology and Reanimation, University Clinical Center of Kosovo
8Department of Gastroenterology and Hepatology, University Clinic Hospital of Kosova
9Department of Cardiovascular diseases, Mayo Clinic, Rochester, MN, USA
10FU Medical College, Foundation University Islamabad, Punjab, Pakistan
11University of Minnesota, Rochester, MN, USA
12Department of General Surgery, Mayo Clinic, Rochester, MN, USA
*Corresponding Author: Fjolla Hyseni Vokshi, Medical Resercher, NYU Langone Health, New York, USA
Received: 05 September 2021; Accepted: 23 September 2021; Published: 08 October 2021
Citation: Fjolla Hyseni, Ali Guy, Guri Hyseni, Breta Kotorri, Blerona Shaipi, Ermira Aliu, Valon Vokshi, Loran Rakovica, Essa A Mohamed, Ibrahim A Bajwa, Mumin M Omar, Juna Musa. Acquired Cryptorchidism in a 12-Year-old with X-Linked Ichthyosis (XLI). Archives of Clinical and Medical Case Reports 5 (2021): 680-684.
View / Download Pdf Share at FacebookAbstract
Cryptorchidism is a broad term encompassing several distinct entities. True, false cryptorchidism and ectopia testis are congenital disorders. Rarely, cryptorchidism has acquired character. Testicular ascent is also sometimes known as acquired cryptorchidism with an unclear association. Various extracutaneous abnormalities have been reported in some patients with an increased incidence of testicular cryptorchidism. X-linked ichthyosis is a genetic disorder of keratinization characterized by a generalized desquamation of large, adherent, dark brown scales. Steroid sulfatase (STS) deficiency is one of the causes of ichthyoses. STS genes on the X chromosome is responsible for this disease. Herein we report a case of STS deficiency complicated with an acquired cryptorchidism. A 12-yearold- boy with STS deficiency was referred to our hospital because of emptiness of his right scrotum. In early childhood at 5 years of age his skin was excessively dry and scaly by visible scaling and/or hyperkeratosis of most or all the skin in the lower extremity. The child underwent immediate orchiopexy via a groin approach and the testis was successfully mobilized into the scrotum.
Keywords
Cryptorchidism; STS gene; X-linked ichthyosis; Orchiopexy; Acquired
Cryptorchidism articles; STS gene articles; X-linked ichthyosis articles; Orchiopexy articles; Acquired articles
Cryptorchidism articles Cryptorchidism Research articles Cryptorchidism review articles Cryptorchidism PubMed articles Cryptorchidism PubMed Central articles Cryptorchidism 2023 articles Cryptorchidism 2024 articles Cryptorchidism Scopus articles Cryptorchidism impact factor journals Cryptorchidism Scopus journals Cryptorchidism PubMed journals Cryptorchidism medical journals Cryptorchidism free journals Cryptorchidism best journals Cryptorchidism top journals Cryptorchidism free medical journals Cryptorchidism famous journals Cryptorchidism Google Scholar indexed journals COVID-19 articles COVID-19 Research articles COVID-19 review articles COVID-19 PubMed articles COVID-19 PubMed Central articles COVID-19 2023 articles COVID-19 2024 articles COVID-19 Scopus articles COVID-19 impact factor journals COVID-19 Scopus journals COVID-19 PubMed journals COVID-19 medical journals COVID-19 free journals COVID-19 best journals COVID-19 top journals COVID-19 free medical journals COVID-19 famous journals COVID-19 Google Scholar indexed journals STS gene articles STS gene Research articles STS gene review articles STS gene PubMed articles STS gene PubMed Central articles STS gene 2023 articles STS gene 2024 articles STS gene Scopus articles STS gene impact factor journals STS gene Scopus journals STS gene PubMed journals STS gene medical journals STS gene free journals STS gene best journals STS gene top journals STS gene free medical journals STS gene famous journals STS gene Google Scholar indexed journals X-linked ichthyosis articles X-linked ichthyosis Research articles X-linked ichthyosis review articles X-linked ichthyosis PubMed articles X-linked ichthyosis PubMed Central articles X-linked ichthyosis 2023 articles X-linked ichthyosis 2024 articles X-linked ichthyosis Scopus articles X-linked ichthyosis impact factor journals X-linked ichthyosis Scopus journals X-linked ichthyosis PubMed journals X-linked ichthyosis medical journals X-linked ichthyosis free journals X-linked ichthyosis best journals X-linked ichthyosis top journals X-linked ichthyosis free medical journals X-linked ichthyosis famous journals X-linked ichthyosis Google Scholar indexed journals Orchiopexy articles Orchiopexy Research articles Orchiopexy review articles Orchiopexy PubMed articles Orchiopexy PubMed Central articles Orchiopexy 2023 articles Orchiopexy 2024 articles Orchiopexy Scopus articles Orchiopexy impact factor journals Orchiopexy Scopus journals Orchiopexy PubMed journals Orchiopexy medical journals Orchiopexy free journals Orchiopexy best journals Orchiopexy top journals Orchiopexy free medical journals Orchiopexy famous journals Orchiopexy Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals CT articles CT Research articles CT review articles CT PubMed articles CT PubMed Central articles CT 2023 articles CT 2024 articles CT Scopus articles CT impact factor journals CT Scopus journals CT PubMed journals CT medical journals CT free journals CT best journals CT top journals CT free medical journals CT famous journals CT Google Scholar indexed journals Hydrocortisone articles Hydrocortisone Research articles Hydrocortisone review articles Hydrocortisone PubMed articles Hydrocortisone PubMed Central articles Hydrocortisone 2023 articles Hydrocortisone 2024 articles Hydrocortisone Scopus articles Hydrocortisone impact factor journals Hydrocortisone Scopus journals Hydrocortisone PubMed journals Hydrocortisone medical journals Hydrocortisone free journals Hydrocortisone best journals Hydrocortisone top journals Hydrocortisone free medical journals Hydrocortisone famous journals Hydrocortisone Google Scholar indexed journals Tuberculomas articles Tuberculomas Research articles Tuberculomas review articles Tuberculomas PubMed articles Tuberculomas PubMed Central articles Tuberculomas 2023 articles Tuberculomas 2024 articles Tuberculomas Scopus articles Tuberculomas impact factor journals Tuberculomas Scopus journals Tuberculomas PubMed journals Tuberculomas medical journals Tuberculomas free journals Tuberculomas best journals Tuberculomas top journals Tuberculomas free medical journals Tuberculomas famous journals Tuberculomas Google Scholar indexed journals Undescended testis articles Undescended testis Research articles Undescended testis review articles Undescended testis PubMed articles Undescended testis PubMed Central articles Undescended testis 2023 articles Undescended testis 2024 articles Undescended testis Scopus articles Undescended testis impact factor journals Undescended testis Scopus journals Undescended testis PubMed journals Undescended testis medical journals Undescended testis free journals Undescended testis best journals Undescended testis top journals Undescended testis free medical journals Undescended testis famous journals Undescended testis Google Scholar indexed journals
Article Details
1. Introduction
UDT is one of most common pediatric disorders at birth among male children. Undescended testis (UDT) could present during later into childhood years when the child is between one and 10 years old. This phenomenon is named as acquired UDT (35%) which is manifested with the absence of one or both testes in normal scrotal position. An ascending testicle or acquire undescended testicle, that has returned to the groin and can be easily guided by hand into the scrotum. Based on the routine examination, the physician determines this illness. Since the etiology remains unclear and the disorder is very well-known, testes at birth have descended at 96% rate therefore 1 year old boys the incidence reaches 0.8% which usually occurs on the right 50% and on the left 35% as well as at a bilateral rate of 10-15%. Determine whether the testis is palpable or not, is crucial when contemplating the differential diagnosis for cryptorchidism. Early detection is crucial to prevent high risk of Acquired UDT which is linked to testicular cancer in adulthood (though the risk is still less than 1 in 100). Whereas Testicular torsion (twisting of the chord that brings blood to the scrotum) developing a hernia near the groin [2-4].
2. Case Report
A 12-year-old boy was referred to our hospital by his pediatrician because of emptiness of his right scrotum. He was born at term with no significant medical history. At admission vital signs were normal. His heart, lung, and abdominal examination was normal. Laboratory: hemoglobin 14.1 gm%, white blood cell counts 11.4/mm3, uranalysis was normal. Physical examination revealed an empty right hemi-scrotum and a mass over the midpoint of the inguinal canal. The left testicle resides, shape, and consistency was in the scrotum with a normal size. The right hypotrophic testis was palpable in the middle of the inguinal canal. Ultrasound examination reveals a right testis with homogeneous low-to medium- level echogenicity and was spherical in shape. The testis measures 3 to 5 cm in length and 2 to 3 cm in depth. Also, pulsed wave Doppler testicular flow was normal. In addition, he presented with severe, hyperkeratotic plaques of the lower extremities. In early childhood at 5 years of age his skin was excessively dry and scaly by visible scaling and/or hyperkeratosis of most or all the skin in the lower extremity. Family was counseled about the disease and possible precipitating factors. There was no family history of similar kind of illness. There was no history of any drug intake prior to the scaling. Further evaluation through STS assay and PCR amplification of 5'-3' ends of the STS gene were analyzed. Undetectable levels of STS activity and complete deletion of the STS gene were found, and the patient was diagnosed with XLR ichthyosis. The child underwent immediate orchiopexy via a groin approach and the testis was successfully mobilized into the scrotum. The postoperative recovery was uneventful. Follow-up six month later the right testis was into the scrotum with normal ultrasound examination.
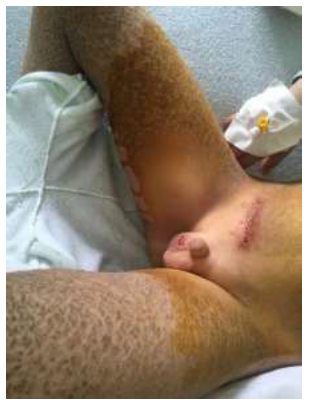
Figure 1: Immediate postoperative appearance following right orchiopexy. Lower extremities keratinization’s are characterized by a generalized desquamation of large, adherent, dark brown scales.
3. Discussion
The failure of testis descent in the scrotum is known as cryptorchidism or UDT. It is more frequent in premature male neonates, with an incidence varying from 1-4 % in full-term and 1-45% in preterm male [1]. Cryptorchidism is a rare but significant defect that occurs when the testis does not descend properly. It usually affects male neonates and is characterized by spontaneous descent. The defect is linked to various genetic and environmental factors. 60% of newborns experience spontaneous descent by the age of six months. Down syndrome, Klinefelter syndrome, and prune-belly syndrome are all linked to cryptorchidism. It can also be found in disorders like posterior urethral valve, abdominal wall defects such as omphalocele and gastroschisis, and neural tube anomalies like myelomeningocele, spigelian hernia, and cerebral palsy. The UDT has a higher risk of cancer than contralateral descended testis. The contralateral testis is a type of testis that shows an increased risk of developing cancer. The unusual environment in cryptorchidism causes gonocytes to accumulate within the seminiferous cords and undergo mutations. The contralateral descended testis is a known risk factor for cryptorchidism. The high temperature environment which can inhibit the development of gonocyte stem cells and trigger subsequent apoptosis are some of the factors that contribute to this risk. Gonocytes accumulate within the seminiferous cords and develop into cancer cells. They can become the source of these cells through mutations [2]. The testis develops in relation to the posterior abdominal wall. They reach the iliac fossa in the third month of intrauterine life and the deep inguinal ring in the seventh month.
During the seventh month, they move through the inguinal canal and are in the scrotum by the end of the eighth month. The descent of testis is carried out in two phases [3]. The first phase involves moving across the abdomen to the inguinal canal- Sertoli cells secrete anti-Mullerian hormone, which influences this phase. The second phase involves moving through the inguinal canal. The normal attachment of gubernaculum to the scrotal ligament plays a crucial role in the complete descent of testes, especially in the second phase.
In some cases, the ligament is attached to the pubic region, undescended testis on the right could be the result of this. The incidence of undescended testis in men ranges from one in 1,000 to one in 2,500 [4]. Testicular torsion and inguinal hernia are two frequent side effects of an undescended testis. The condition usually affects males and can lead to poor sperm quality [5]. Determine whether the testis is palpable or not, is crucial when contemplating the differential diagnosis for cryptorchidism. If palpable, It could be one of three diagnosis:
- A real palpable undescended testis that may be felt in the inguinal canal all the way to the external ring [6].
- The testis is placed somewhere outside the typical anatomical line of descent, but not within the scrotum [6]. The suprapubic, perineal, and femoral regions are the most prevalent locations [7].
- A retractile testis is the third factor to evaluate with palpable cryptorchidism.
This happens when the testis is missing from the scrotum due to an abnormally strong cremasteric reflex, but it may be brought back into place during your physical exam by overriding that reaction. It is not always easy to tell the difference between a real undescended testis and a retractile one. Undescended testes are linked to the same difficulties as retractile testes. While most cases of cryptorchidism present unilaterally, up to one-third of cases present bilaterally. Congenital absence of the vas deferens (CAVD) can be unilateral (CUAVD) or bilateral (CBAVD), and it accounts for 1-2 percent of male infertility. In this way, in patients with cryptorchidism, the presence of vas deferens ought to be assessed during scrotal palpation and stomach ultrasound study is additionally prescribed to assess some other coinciding irregularities like renal agenesis.Additionaly more, CFTR quality investigation may be additionally useful to assess the presence of inactive cystic fibrosis [8].
4. Conclusion
Our case report highlights the importance of a periodic testicular evaluation in XLI due to the association with acquired cryptorchidism. In addition, we suggest that this case report will result to provide more information for genetic counselling reinforce the need for multidisciplinary medical counseling, even though the association of cryptorchidism and X-linked recessive ichthyosis are not mutually exclusive, but rather may both contribute to this association.
References
- Docimo SG. The results of surgical therapy for cryptorchidism: a literature review and analysis. J Urol 154 (1995): 1148-1152.
- Ong C, Hasthorpe S, Hutson JM. Germ cell development in the descended and cryptorchid testis and the effects of hormonal manipulation. Pediatr Surg Int 21 (2005): 240-254.
- Bailey and love’s, short practice of surgery, 24th edition (2004):1404.
- Kolon TF, Patel RP, Huff DS. Cryptorchidism: diagnosis, treatment, and long- term prognosis". Urol. Clin. North Am. 31 (2004): 469-480.
- Pinczowski D, McLaughlin JK, Lackgren G, et al. Occurrence of testicular cancer in patients operated on for cryptorchidism and inguinal hernia. J Urol 146 (1991): 1291-1294.
- Braga LH, Lorenzo AJ, Romao RL. Canadian Urological Association-Pediatric Urologists of Canada (CUA-PUC) guideline for the diagnosis, management, and follow- up of cryptorchidism. Canadian Urological Association Journal 11 (2017): E251.
- Celayir AC, Sander S, Elicevik M. Timing of surgery in perineal ectopic testes: analysis of 16 cases. Pediatric Surgery International 17 (2001): 167-168.
- Daudin M, Bieth E, Bujan L, et al. Congenital bilateral absence of the vas deferens: clinical characteristics, biological parameters, cystic fibrosis transmembrane conductance regulator gene mutations, and implications for genetic counseling. Fertility and Sterility 74 (2000): 1164-1174, 2000.
