A Smart Treatment for Sprains around Ankle with Platelet Rich Plasma
Article Information
r Ashok Naidu1 , Dr Sunil T2 , Dr Satya Kumar Koduru1,*
1Prof and Hod-Orthopaedics, Nri Academy of Sciences, Andhra Pradesh, India
2Asst.Prof of Orthopaedics, Nri Academy of Sciences, Andhra Pradesh, India
*Corresponding Author: Dr Satya Kumar Koduru, Hod-Orthopaedics, Nri Academy of Sciences, Andhra Pradesh, India
Received: 28 February 2020; Accepted: 11 March 2020; Published: 31 March 2020
Citation: Dr Ashok Naidu, Dr Sunil T, Dr Satya Kumar Koduru. A Smart Treatment for Sprains around Ankle with Platelet Rich Plasma. Journal of Orthopaedics and Sports Medicine 2 (2020): 55-60.
View / Download Pdf Share at FacebookAbstract
Sprains of ankle are one of the most common injuries in sports and also in normal life. Normally, they are treated with time and basic ligament care techniques. Most sprains will heal without surgery.
The aim: Is to evaluate the role of autologous prp for acute ankle injuries. Our analysis evaluates the recent literature on prp use in the management of acute, traumatic ankle injuries and also to report the effects of autologous prp injections on time to return to work or play.
Keywords
<p>Ankle Injuries; Prp; Platelet Rich Plasma; Autologous Prp; Ankle Ligamentous Injuries</p>
Platelet-rich plasma articles Platelet-rich plasma Research articles Platelet-rich plasma review articles Platelet-rich plasma PubMed articles Platelet-rich plasma PubMed Central articles Platelet-rich plasma 2023 articles Platelet-rich plasma 2024 articles Platelet-rich plasma Scopus articles Platelet-rich plasma impact factor journals Platelet-rich plasma Scopus journals Platelet-rich plasma PubMed journals Platelet-rich plasma medical journals Platelet-rich plasma free journals Platelet-rich plasma best journals Platelet-rich plasma top journals Platelet-rich plasma free medical journals Platelet-rich plasma famous journals Platelet-rich plasma Google Scholar indexed journals Orthopaedics articles Orthopaedics Research articles Orthopaedics review articles Orthopaedics PubMed articles Orthopaedics PubMed Central articles Orthopaedics 2023 articles Orthopaedics 2024 articles Orthopaedics Scopus articles Orthopaedics impact factor journals Orthopaedics Scopus journals Orthopaedics PubMed journals Orthopaedics medical journals Orthopaedics free journals Orthopaedics best journals Orthopaedics top journals Orthopaedics free medical journals Orthopaedics famous journals Orthopaedics Google Scholar indexed journals Sports medicine articles Sports medicine Research articles Sports medicine review articles Sports medicine PubMed articles Sports medicine PubMed Central articles Sports medicine 2023 articles Sports medicine 2024 articles Sports medicine Scopus articles Sports medicine impact factor journals Sports medicine Scopus journals Sports medicine PubMed journals Sports medicine medical journals Sports medicine free journals Sports medicine best journals Sports medicine top journals Sports medicine free medical journals Sports medicine famous journals Sports medicine Google Scholar indexed journals Ankle injuries articles Ankle injuries Research articles Ankle injuries review articles Ankle injuries PubMed articles Ankle injuries PubMed Central articles Ankle injuries 2023 articles Ankle injuries 2024 articles Ankle injuries Scopus articles Ankle injuries impact factor journals Ankle injuries Scopus journals Ankle injuries PubMed journals Ankle injuries medical journals Ankle injuries free journals Ankle injuries best journals Ankle injuries top journals Ankle injuries free medical journals Ankle injuries famous journals Ankle injuries Google Scholar indexed journals Musculoskeletal tissues articles Musculoskeletal tissues Research articles Musculoskeletal tissues review articles Musculoskeletal tissues PubMed articles Musculoskeletal tissues PubMed Central articles Musculoskeletal tissues 2023 articles Musculoskeletal tissues 2024 articles Musculoskeletal tissues Scopus articles Musculoskeletal tissues impact factor journals Musculoskeletal tissues Scopus journals Musculoskeletal tissues PubMed journals Musculoskeletal tissues medical journals Musculoskeletal tissues free journals Musculoskeletal tissues best journals Musculoskeletal tissues top journals Musculoskeletal tissues free medical journals Musculoskeletal tissues famous journals Musculoskeletal tissues Google Scholar indexed journals Joint articles Joint Research articles Joint review articles Joint PubMed articles Joint PubMed Central articles Joint 2023 articles Joint 2024 articles Joint Scopus articles Joint impact factor journals Joint Scopus journals Joint PubMed journals Joint medical journals Joint free journals Joint best journals Joint top journals Joint free medical journals Joint famous journals Joint Google Scholar indexed journals Osteoarthritis articles Osteoarthritis Research articles Osteoarthritis review articles Osteoarthritis PubMed articles Osteoarthritis PubMed Central articles Osteoarthritis 2023 articles Osteoarthritis 2024 articles Osteoarthritis Scopus articles Osteoarthritis impact factor journals Osteoarthritis Scopus journals Osteoarthritis PubMed journals Osteoarthritis medical journals Osteoarthritis free journals Osteoarthritis best journals Osteoarthritis top journals Osteoarthritis free medical journals Osteoarthritis famous journals Osteoarthritis Google Scholar indexed journals Rheumatoid arthritis articles Rheumatoid arthritis Research articles Rheumatoid arthritis review articles Rheumatoid arthritis PubMed articles Rheumatoid arthritis PubMed Central articles Rheumatoid arthritis 2023 articles Rheumatoid arthritis 2024 articles Rheumatoid arthritis Scopus articles Rheumatoid arthritis impact factor journals Rheumatoid arthritis Scopus journals Rheumatoid arthritis PubMed journals Rheumatoid arthritis medical journals Rheumatoid arthritis free journals Rheumatoid arthritis best journals Rheumatoid arthritis top journals Rheumatoid arthritis free medical journals Rheumatoid arthritis famous journals Rheumatoid arthritis Google Scholar indexed journals Foot and ankle articles Foot and ankle Research articles Foot and ankle review articles Foot and ankle PubMed articles Foot and ankle PubMed Central articles Foot and ankle 2023 articles Foot and ankle 2024 articles Foot and ankle Scopus articles Foot and ankle impact factor journals Foot and ankle Scopus journals Foot and ankle PubMed journals Foot and ankle medical journals Foot and ankle free journals Foot and ankle best journals Foot and ankle top journals Foot and ankle free medical journals Foot and ankle famous journals Foot and ankle Google Scholar indexed journals Anterior talofibular ligament articles Anterior talofibular ligament Research articles Anterior talofibular ligament review articles Anterior talofibular ligament PubMed articles Anterior talofibular ligament PubMed Central articles Anterior talofibular ligament 2023 articles Anterior talofibular ligament 2024 articles Anterior talofibular ligament Scopus articles Anterior talofibular ligament impact factor journals Anterior talofibular ligament Scopus journals Anterior talofibular ligament PubMed journals Anterior talofibular ligament medical journals Anterior talofibular ligament free journals Anterior talofibular ligament best journals Anterior talofibular ligament top journals Anterior talofibular ligament free medical journals Anterior talofibular ligament famous journals Anterior talofibular ligament Google Scholar indexed journals Pain articles Pain Research articles Pain review articles Pain PubMed articles Pain PubMed Central articles Pain 2023 articles Pain 2024 articles Pain Scopus articles Pain impact factor journals Pain Scopus journals Pain PubMed journals Pain medical journals Pain free journals Pain best journals Pain top journals Pain free medical journals Pain famous journals Pain Google Scholar indexed journals Cytokines articles Cytokines Research articles Cytokines review articles Cytokines PubMed articles Cytokines PubMed Central articles Cytokines 2023 articles Cytokines 2024 articles Cytokines Scopus articles Cytokines impact factor journals Cytokines Scopus journals Cytokines PubMed journals Cytokines medical journals Cytokines free journals Cytokines best journals Cytokines top journals Cytokines free medical journals Cytokines famous journals Cytokines Google Scholar indexed journals Inflammation angiogenesis articles Inflammation angiogenesis Research articles Inflammation angiogenesis review articles Inflammation angiogenesis PubMed articles Inflammation angiogenesis PubMed Central articles Inflammation angiogenesis 2023 articles Inflammation angiogenesis 2024 articles Inflammation angiogenesis Scopus articles Inflammation angiogenesis impact factor journals Inflammation angiogenesis Scopus journals Inflammation angiogenesis PubMed journals Inflammation angiogenesis medical journals Inflammation angiogenesis free journals Inflammation angiogenesis best journals Inflammation angiogenesis top journals Inflammation angiogenesis free medical journals Inflammation angiogenesis famous journals Inflammation angiogenesis Google Scholar indexed journals Prp injections articles Prp injections Research articles Prp injections review articles Prp injections PubMed articles Prp injections PubMed Central articles Prp injections 2023 articles Prp injections 2024 articles Prp injections Scopus articles Prp injections impact factor journals Prp injections Scopus journals Prp injections PubMed journals Prp injections medical journals Prp injections free journals Prp injections best journals Prp injections top journals Prp injections free medical journals Prp injections famous journals Prp injections Google Scholar indexed journals Soft tissue articles Soft tissue Research articles Soft tissue review articles Soft tissue PubMed articles Soft tissue PubMed Central articles Soft tissue 2023 articles Soft tissue 2024 articles Soft tissue Scopus articles Soft tissue impact factor journals Soft tissue Scopus journals Soft tissue PubMed journals Soft tissue medical journals Soft tissue free journals Soft tissue best journals Soft tissue top journals Soft tissue free medical journals Soft tissue famous journals Soft tissue Google Scholar indexed journals
Article Details
1. Introduction
Lateral sprains of ankle are one of the most common in sports medicine and in orthopaedic practice, considering the sprains; they represent an 85% of the ankle injuries.
The objective of the treatment is to normalize the joint function and allow the patient to return to his or her normal activities and improve quality of life as early as possible. Prp treatment helps create a biological environment internally that is most conducive for restoration of injured tissue by providing numerous signaling cytokines and growth factors that are important in repair of the damaged tissue by diverse mechanisms including the regulation of inflammation angiogenesis and remodeling of new tissue.
Conclusion - treatment with platelet-rich plasma (prp) is a widely used alternative option which is safe because of its autologous nature.
Prp contains numerous growth factors responsible for its potential to heal ankle injuries effectively. Though treatment with platelet-rich plasma is a promising option, there is only limited clinical evidence supporting its use in acute traumatic ankle injuries. § one of the most common injuries in sports& in daily life are ankle sprains. Normally, they are treated with time and basic ligament care techniques. Most sprains will heal without surgery.
1.1 Purpose of review
Platelet-rich plasma has become popular treatment option within the orthopedic community to biologically enhance and stimulate difficult-to-heal musculoskeletal tissues.
1.2 The aim
Is to evaluate the role of autologous prp for acute ankle injuries. Our analysis evaluates the recent literature on prp use in the management of acute, traumatic ankle injuries and also to report the effects of autologous prp injections on time to return to work or play.
1.3 Introduction
Lateral ankle sprains account for 85% of the injuries in sports and in daily life.
1.4 The objective of the treatment
Is to normalize the joint function and allow the patient to return to daily activities and improve quality of life as early as possible. Prp treatment helps create a biological environment [1] internally that is very conducive for restoration of injured tissue by providing numerous signaling cytokines and growth factors [2, 3] that are important in repair of the damaged tissue by diverse mechanisms including the regulation of inflammation angiogenesis and remodeling of new tissue [4-7].
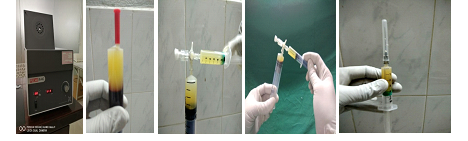
1.5 Prp preparation [8-12]
- 17 ml of venous blood is drawn into one 20 cc syringe containing 3 ml of acd (acid citrate dextrose) to finally get 4 ml of platelet rich plasma.
- It is centrifuged (1st) for 15 minutes with a setting of 1500 rpm along with counterbalance to the syringe.
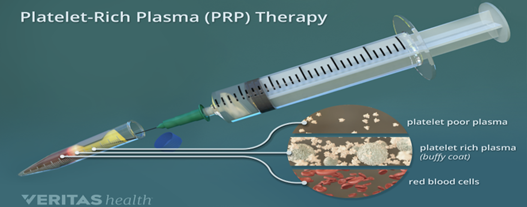
- Three layers were formed upper being the platelets containing plasma, middle being the buffy coat layer, lower being the RBC.
- Upper layer was drawn out into another syringe.
- It is centrifuged (2nd) for 7-8 minutes with a setting of 3500 rpm which is very rapid, essential for platelets to sediment along with the counterbalance.
- High concentration of platelets, were sedimented at the bottom of the test tube with platelet poor plasma being on the top.
- Platelet poor plasma was discarded with 2-3ml of prp left in the syringe.
2. Materials and Methods
Materials and methods a study of 36 cases done in nri
medical college and orthocare, Vijayawada over last 18 months. Single dose of prp along with walking cast application in acute ankle sprains showed reduction in vas score at 3 weeks interval.
2.1 Inclusion criteria
- Acute lateral and medial ankle sprains with no more of 48 hours of evolution,
- First time ankle sprain,
- Grade 2 or 3.
2.2 Exclusion criteria
- Associated pathologies like osteoarthritis, rheumatoid arthritis,
- Pregnant women,
- Previous surgery around the ankle,
- Blood dyscrasias.
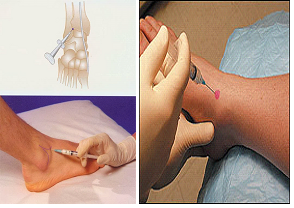
The patients will receive a single dose of autologous platelet-rich plasma, and will be immobilized with a walking cast for 3 weeks post walking cast removal, they will be evaluated with American orthopedic foot and ankle society's ankle hind foot scale, vas and foot and ankle disability index. § Platelet-rich plasma will be injected (3-4ml) under the lateral malleolus, over the anterior talofibular ligament or around deltoid ligamentous region for medial injuries.
3. Results
Results were based on following criteria
- American orthopedic foot and ankle society ankle-hind foot scale (aofas) time frame: six months evaluates pain, function and alignment of foot. The best score is 100 points, and the worst score is 0 points.
- Visual analogue scale time frame: six months evaluate the pain in a scale of 0 to 10, when 0 is no pain and 10 is the worst pain
- Foot and ankle disability index (fadi) time frame: six months assesses activities such as standing, walking on flat or uneven surfaces, walking on inclines, and the length of time of walking without difficulty. It also includes a section for sports activities and ankle or foot pain (or both). The highest score is 136 points, indicating the best clinical situation, free of pain and limitations, while the lowest score is 0.
3.1 Results
- Out of 36 patients -28 cases were lateral ankle injuries, 08 cases are medial deltoid ligamentous injuries.
- Male - 22,female -14
- Right side -20,
- Left side 16
- Age group -18-30= 20, 30-50=12, 50 and above=04
- Aofas scale - 96-100 points in 28 cases
- Vas score - 0-2 - in 28 cases
- Fadi score - 130 points in 28 cases
- 6 cases came back late for follow up with removal of walking cast elsewhere so we didn't include them in the result
- Remaining 2 cases lost follow up.
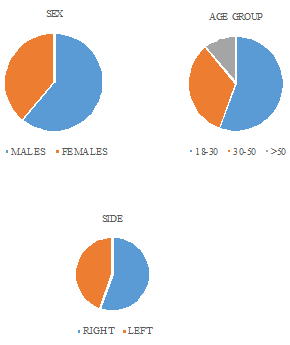
4. Discussion
Prp treatment helps create a biological environment internally that is very conducive for restoration of injured tissue by providing numerous signaling cytokines and growth factors that are important in repair of the damaged tissue by diverse mechanisms including the regulation of inflammation angiogenesis and remodeling of new tissue.
The utilization of prp for the treatment of musculoskeletal conditions has become more prevalent in recent years. Current literature has established that prp injections are safe and accelerate the soft tissue healing process.
5. Conclusion
Prp can be used as an alternative treatment that is safe due to its autologous nature. Prp contains numerous growth factors that have potential to repair ankle injuries effectively. Prp may be a promising treatment option, but at present, there are only limited clinical studies supporting its use in acute traumatic ankle injuries.
Conflict of Interest
None.
References
- Administration Fad. Regulatory considerations for human cells, tissues, and cellular and tissue-based products. Minimal manipulation and homologous use. In: services Usdohah, editor. Maryland: U.S. Department of Health and Human Services (2017).
- Hall Mp, Band Pa, Meislin Rj, et al. Platelet-rich plasma: current concepts and application in sports medicine. J Am Acad Orthop Surg 17 (2009): 602-608.
- Iqbal J, Pepkowitz Sh, Klapper E. Platelet-rich plasma for the replenishment of bone. Curr Osteoporos Rep 9 (2011): 258-263.
- Mishra A, Tummala P, King A, et al. Buffered platelet-rich plasma enhances mesenchymal stem cell proliferation and chondrogenic differentiation. Tissue Engineering Part C, Methods 15 (2009): 431-435.
- Murray Ir, Laprade Rf. Platelet-rich plasma: renewed scientific understanding must guide appropriate use. Bone Joint Res 5 (2016): 92-94.
- Prins Hj, Rozemuller H, Vonk-Griffioen S, et al. Bone-forming capacity of mesenchymal stromal cells when cultured in the presence of human platelet lysate as substitute for fetal bovine serum. Tissue Eng A 15 (2009): 3741-3751.
- Zaky Sh, Ottonello A, Strada P, et al. Platelet lysate favours in vitro expansion of human bone marrow stromal cells for bone and cartilage engineering. J Tissue Eng Regen Med 2 (2008): 472-481.
- Alves R, Grimalt R. A review of platelet-rich plasma: history, biology, mechanism of action, and classification. Skin Appendage Disord 4 (2018): 18-24.
- Castillo Tn, Pouliot Ma, Kim Hj, et al. Comparison of growth factor and platelet concentration from commercial platelet-rich plasma separation systems. Am J Sports Med 39 (2011): 266-271.
- Fitzpatrick J, Bulsara Mk, Mccrory Pr, et al. Analysis of platelet-rich plasma extraction: variations in platelet and blood components between 4 common commercial kits. Orthop J Sports Med 5 (2017).
- Sundman Ea, Cole Bj, Fortier La. Growth factor and catabolic cytokine concentrations are influenced by the cellular composition of platelet-rich plasma. Am J Sports Med 39 (2011): 2135-2140.
- Mazzocca Ad, Mccarthy Mb, Chowaniec Dm, et al. Platelet-rich plasma differs according to preparation method and human variability. J Bone Joint Surg Am 94 (2012): 308-316.
