A Rare Finding of Clostridium Tertium in an Immunocompetent Patient Following Gynecological Surgery
Article Information
Lauren Leightell-Brown*, Alexander Frost-Younger, Stuart Rundle, Christine Ang
Department of Gynaecological-Oncology, Queen Elizabeth Hospital, Gateshead, United Kindom
*Corresponding Author: Lauren Leightell-Brown, Department of Gynaecological-Oncology, Queen Elizabeth Hospital, Queen Elizabeth Avenue, Gateshead, NE9 6SX, United Kindom
Received: 19 January 2022; Accepted: 27 January 2022; Published: 10 May 2022
Citation: Lauren Leightell-Brown, Alexander Frost-Younger, Stuart Rundle, Christine Ang. A Rare Finding of Clostridium Tertium in an Immunocompetent Patient Following Gynecological Surgery. Obstetrics and Gynecology Research 5 (2022): 131-135.
View / Download Pdf Share at FacebookAbstract
Clostridium tertium (C. tertium) is a Gram-positive, aerotolerant bacillus and a rare human pathogen usually identified in neutropenic patients with hematological malignancy. Limited case reports in non-neutropenic patients suggest the C. tertium is a potential pathogen when associated with risk factors which include intestinal mucosal disruption and beta-lactam antibiotic use. Our case is a 59-year-old woman who developed a post-operative collection containing C.tertium following complete cytoreductive surgery for high-grade serous cancer of tuboovarian origin in the absence of neutropenia. To our knowledge, this is the first documented case of C. tertium infection in a post-operative Gynecological-Oncology patient.
Keywords
<p>Clostridium Tertium, Ovarian Cancer, Post-operative Infection</p>
Clostridium Tertium articles Clostridium Tertium Research articles Clostridium Tertium review articles Clostridium Tertium PubMed articles Clostridium Tertium PubMed Central articles Clostridium Tertium 2023 articles Clostridium Tertium 2024 articles Clostridium Tertium Scopus articles Clostridium Tertium impact factor journals Clostridium Tertium Scopus journals Clostridium Tertium PubMed journals Clostridium Tertium medical journals Clostridium Tertium free journals Clostridium Tertium best journals Clostridium Tertium top journals Clostridium Tertium free medical journals Clostridium Tertium famous journals Clostridium Tertium Google Scholar indexed journals Ovarian Cancer articles Ovarian Cancer Research articles Ovarian Cancer review articles Ovarian Cancer PubMed articles Ovarian Cancer PubMed Central articles Ovarian Cancer 2023 articles Ovarian Cancer 2024 articles Ovarian Cancer Scopus articles Ovarian Cancer impact factor journals Ovarian Cancer Scopus journals Ovarian Cancer PubMed journals Ovarian Cancer medical journals Ovarian Cancer free journals Ovarian Cancer best journals Ovarian Cancer top journals Ovarian Cancer free medical journals Ovarian Cancer famous journals Ovarian Cancer Google Scholar indexed journals Post-operative Infection articles Post-operative Infection Research articles Post-operative Infection review articles Post-operative Infection PubMed articles Post-operative Infection PubMed Central articles Post-operative Infection 2023 articles Post-operative Infection 2024 articles Post-operative Infection Scopus articles Post-operative Infection impact factor journals Post-operative Infection Scopus journals Post-operative Infection PubMed journals Post-operative Infection medical journals Post-operative Infection free journals Post-operative Infection best journals Post-operative Infection top journals Post-operative Infection free medical journals Post-operative Infection famous journals Post-operative Infection Google Scholar indexed journals hematological malignancy articles hematological malignancy Research articles hematological malignancy review articles hematological malignancy PubMed articles hematological malignancy PubMed Central articles hematological malignancy 2023 articles hematological malignancy 2024 articles hematological malignancy Scopus articles hematological malignancy impact factor journals hematological malignancy Scopus journals hematological malignancy PubMed journals hematological malignancy medical journals hematological malignancy free journals hematological malignancy best journals hematological malignancy top journals hematological malignancy free medical journals hematological malignancy famous journals hematological malignancy Google Scholar indexed journals hypertension articles hypertension Research articles hypertension review articles hypertension PubMed articles hypertension PubMed Central articles hypertension 2023 articles hypertension 2024 articles hypertension Scopus articles hypertension impact factor journals hypertension Scopus journals hypertension PubMed journals hypertension medical journals hypertension free journals hypertension best journals hypertension top journals hypertension free medical journals hypertension famous journals hypertension Google Scholar indexed journals abdominal bloating articles abdominal bloating Research articles abdominal bloating review articles abdominal bloating PubMed articles abdominal bloating PubMed Central articles abdominal bloating 2023 articles abdominal bloating 2024 articles abdominal bloating Scopus articles abdominal bloating impact factor journals abdominal bloating Scopus journals abdominal bloating PubMed journals abdominal bloating medical journals abdominal bloating free journals abdominal bloating best journals abdominal bloating top journals abdominal bloating free medical journals abdominal bloating famous journals abdominal bloating Google Scholar indexed journals constipation articles constipation Research articles constipation review articles constipation PubMed articles constipation PubMed Central articles constipation 2023 articles constipation 2024 articles constipation Scopus articles constipation impact factor journals constipation Scopus journals constipation PubMed journals constipation medical journals constipation free journals constipation best journals constipation top journals constipation free medical journals constipation famous journals constipation Google Scholar indexed journals abdominal hysterectomy articles abdominal hysterectomy Research articles abdominal hysterectomy review articles abdominal hysterectomy PubMed articles abdominal hysterectomy PubMed Central articles abdominal hysterectomy 2023 articles abdominal hysterectomy 2024 articles abdominal hysterectomy Scopus articles abdominal hysterectomy impact factor journals abdominal hysterectomy Scopus journals abdominal hysterectomy PubMed journals abdominal hysterectomy medical journals abdominal hysterectomy free journals abdominal hysterectomy best journals abdominal hysterectomy top journals abdominal hysterectomy free medical journals abdominal hysterectomy famous journals abdominal hysterectomy Google Scholar indexed journals ovarian conservation articles ovarian conservation Research articles ovarian conservation review articles ovarian conservation PubMed articles ovarian conservation PubMed Central articles ovarian conservation 2023 articles ovarian conservation 2024 articles ovarian conservation Scopus articles ovarian conservation impact factor journals ovarian conservation Scopus journals ovarian conservation PubMed journals ovarian conservation medical journals ovarian conservation free journals ovarian conservation best journals ovarian conservation top journals ovarian conservation free medical journals ovarian conservation famous journals ovarian conservation Google Scholar indexed journals uterine fibroids articles uterine fibroids Research articles uterine fibroids review articles uterine fibroids PubMed articles uterine fibroids PubMed Central articles uterine fibroids 2023 articles uterine fibroids 2024 articles uterine fibroids Scopus articles uterine fibroids impact factor journals uterine fibroids Scopus journals uterine fibroids PubMed journals uterine fibroids medical journals uterine fibroids free journals uterine fibroids best journals uterine fibroids top journals uterine fibroids free medical journals uterine fibroids famous journals uterine fibroids Google Scholar indexed journals
Article Details
1. Introduction
Clostridia are a diverse group of Gram-positive, spore-forming bacilli found in soil and intestinal tracts of animals and humans. First isolated from war wounds in 1917, C. tertium is an unusual species within this genus, being both aerotolerant and non-toxin producing [1]. It is rarely a pathogen in immunocompetent individuals, being more frequently associated with pathogenic infection in patients with neutropenia and hematological malignancy [2, 3]. A number of presentations are described ranging from soft tissue infection to spontaneous bacterial perit-onitis [2-8]. To date, C.tertium is not reported as a pathogen causing major complications in the post-operative gynecological patient.
2. Case Report
A 59-year-old woman with a past medical history of mild hypertension presented with abdominal bloat-ing, pain and constipation. Previous surgery included abdominal hysterectomy with ovarian conservation for uterine fibroids. Workup included serological CA125 and CA19-9 tumour markers (245 kU/L and 94 kU/L, respectively) and a CT scan showed a pelvic mass with evidence of disseminated peritoneal disease. Flexible sigmoidoscopy failed due to extrin-sica compression from the mass. Ultrasound-guided peritoneal biopsy confirmed the diagnosis as high-grade serous carcinoma of tubo-ovarian origin. The patient was counselled for primary cytoreduction via laparotomy. Intra-operative findings were consistent with the pre-operative imaging results. Complete cytoreduction was achieved by removal of the pelvic mass, contralateral tube and ovary en-bloc with the colon and omentum, as well as total abdomino-pelvic and right diaphragm peritonectomy. An end ileostomy was created and the right upper quadrant and pelvic drains were placed at the end of the operation. Intravenous (IV) piperacillin/tazobactam 4.5 g and metronidazole 500g was administered in the first 24 hours postoperatively according to the preferences of the consultant surgeon.
Following an uncomplicated stay as an elective patient on the surgical high dependency unit, the patient was discharged to ward-based care according to our institution’s enhanced recovery pathway. The pelvic drain was removed on day 4. The patient developed oral candi-diasis on day 5 postoperatively and was commenced on oral nystatin spray. On postoperative day 5, symptomatic ileus was diagnosed after the patient reported mild abdominal cramps, distension and nausea. On day 7, the patient developed acute abdominal pain and feculent discharge per vagina. Blood results revealed an acute rise in inflammatory markers with a white cell count of 20.12 (9.59), neutrophil count 17.77 (7.51), C reactive protein 429 (53.6) and a new stage 2 acute kidney injury. A CT thorax, abdomen and pelvis showed moderate intra-abdominal collections and gas within the pelvis (Figure 1).
Due to concern regarding the patient’s clinical condition, an emergency laparotomy was performed. Intra-operative findings on this occasion included an infected pelvic hematoma with pooling of serous fluid, infected debris and fibrin deposition. As per consultant microbiologist guidance, the patient received intravenous piperacillin/tazobactam 4.5g and metronidazole 400mg three times daily for 24 hours, before being switched to IV Ciprofloxacin 400mg and metronidazole 500 mg on postoperative day 2. On postoperative day 3, surgical specimen bacteriology was reported showing polymicrobial growth including Coliforms, Streptococcus angina-osus, and C. tertium. Clinical status and biochemistry significantly improved and on day 4 the patient was switched to oral ciprofloxacin 500mg and metro-nidazole 400mg, again with Microbiology Consultant advice. This regimen was continued until postopera-tive day 9 when antibiotics were discontinued following sustained clinical improvement. On post-operative day 10, the patient was discharged home. Blood cultures and surgical wound swabs grew no organisms.
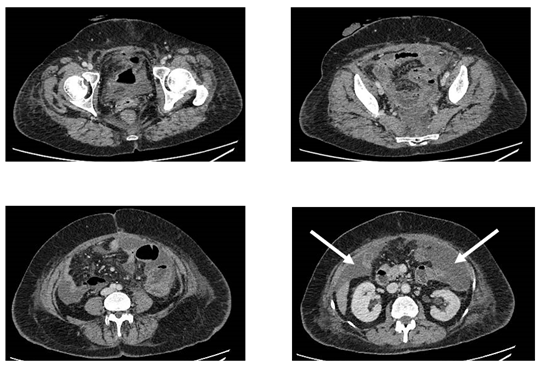
Figure 1: Radiologic imaging confirming post-operative changes. White arrow demonstrates moderate size collections within the pelvis. No evidence of bowel injury.
3. Discussion
Risk factors for C.tertium infection include neut-ropenia, intestinal mucosal injury, severe liver disease and use of beta-lactam antibiotics [2] Over 90% of cases of pathogenic C.tertium infections involve neutropenic patients [2]. C. Tertium invol-ving non-neutropenic patients is rare and almost all reported cases involve gastrointestinal pathology. Two cases of C.tertium have been reported in the post-operative patient. Hepatic abscess and C.tert-ium bacteremia following emergency appendectomy [8] and C.tertium lung empyema post right hemi-colectomy [9]. In our case, numerous risk factors were identified including recent bowel resection, peri-operative administration of beta-lactam antibio-tics and a possible impaired immune system from prolonged poor nutrition. Additionally, in this case, a solid-state hemostatic agent was used to aid hemo-stasis before closure. These agents have previously been reported to be a risk factor for the development of postoperative pelvic collection in gynecological patients undergoing pelvic exenteration for recurrent malignancy [10].
Post gynecological surgery pelvic collections are mostly polymicrobial due to contamination from the skin, vaginal opening or bowel resection [11]. Organisms commonly found include Coliforms, Enterococcus, Streptococcus and Anaerobes. Due to its aerotolerant characteristics, C.tertium is some-times falsely identified as Gram-positive aerobic organisms/bacilli, and these are often judged to be a contaminant such as Lactobacillus spp. or Bacillus spp. [12]. In some cases, this has led to delays in the initiation of correct treatment. Antimicrobial guide-lines for the management of C.tertium are not standardised. Typically, the organism is resistant to beta-lactams, including cephalosporins and clinda-mycin. Common susceptibilities and successful treat-ment has been described with vancomycin, quin-olones, imipenems and trimethoprim [3, 13-15]. C. tertium bacteremia has been successfully treated with Metronidazole, yet we understand metronidazole resistant strains have been reported. In our case, this particular C.tertium strain was sensitive to peni-cillins, co-amoxiclav and metronidazole.
In conclusion, we present the first case of a post-operative polymicrobial pelvic collection containing C. tertium in a tertiary Gyne-Oncology unit. Numerous identifiable risk factors were found for C. tertium infection and for developing a post-operative pelvic collection. A combination of bowel surgery, exposure to perioperative beta-lactam antibiotics and use of fibrin hemostat agents were likely to be contributing factors. By reporting this case we hope to contribute to the limited literature available regarding C.tertium pathogenicity and successful management. Given its potential for misidentify-cation, C.tertium should be considered in the post-operative Gynecological Oncology patient who has been exposed to known risk factors.
Disclosure
The authors declare no conflict of interest.
References
- Henry CH. An investigation of the cultural reactions of certain anaerobes found in wounds. The Journal of Pathology and Bacteriology 21 (1918).
- Miller DL, Brazer S, Murdoch D, et al. Significance of Clostridium tertium bacter-emia in neutropenic and nonneutropenic patients: review of 32 cases. Clinical Infectious Diseases 32 (2001).
- Valtonen M, Sivonen A, Elonen E. A cluster of seven cases of Clostridium tertium septicemia in neutropenic patients. European journal of clinical microbiology & infectious diseases 9 (1990): 40-42.
- Kourtis AP, Weiner R, Belson K, et al. Clostridium tertium meningitis as the presenting sign of a meningocele in a twelve-year-old child. Pediatric infectious diseases Journal 16 (1997): 527-529.
- Gredlein CM, Silverman ML, Downey MS. Polymicrobial septic arthritis due to clostridium species: case report and review. Clinical infectious diseases 30 (2000)
- Butler T, Pitt S. Spontaneous bacterial peritonitis due to Clostridium tertium. Gastroenterology 82 (1982).
- Lew JF, Wiedermann BL, Sneed J, et al. Aerotolerant Clostridium tertium brain abscess following a lawn dart injury. Journal of Clinical Microbiology 28 (1990).
- Milano V, Biehle L, Patel S, et al. Clostridium tertium bacteremia and hepatic abscess in a non-neutropenic patient. ID Cases 15 (2019).
- Alroumi F, Giaccotto J, Sarwar A, et al. Clostridium tertium Empyema after a Hemi-Colectomy and Repair of Incarcerated Hernia. Surgical Infections Case Reports 1 (2016): 146-148.
- Fagotti A, Costantini B, Fanfani F, et al. Risk of postoperative pelvic abscess in major gynecologic oncology surgery: one-year sing-le-institution experience. Ann Surg Oncol 17(2010): 2452-2458.
- Lachiewicz MP, Moulton LJ, Jaiyeoba O. Pelvic surgical site infections in gynecologic surgery. Infectious Diseases in Obstetrics and Gynecology 2015 (2015): 614950-614950.
- Gosbell IB, Johnson CG, Newton PJ, et al. Clostridium tertium bacteremia: 2 cases and review. Pathology 28 (1996): 70-73.
- Coleman N, Speirs G, Khan J, et al. Neutropenic enterocolitis associated with Clostridium tertium. Journal of Clinical Pathology 46 (1993).
- Thaler M, Gill V, Pizzo PA. Emergence of Clostridium tertium as a pathogen in neutropenic patients. The American Journal of Medicine 81 (1986): 596-600.
- Speirs G, Warren R E, Ramp A. Clostridium tertium septicemia in patients with neutropenia. The Journal of Infectious Disease 158 (1988): 1336-1340.
