Nailfold Changes as a Sign of Underlying Systemic Illnesses
Article Information
Muhammad Sohaib Asghar1*, Abubakar Tauseef1, Muhammad Sohaib Qamar2, Saad Aslam1, Mohammed Akram3, Basmah Fayaz3, Uzma Rasheed3, Maryam Zafar1, Gul Muhammad Memon3, Iftekhar Ahmed1
1Dow University Hospital, Dow University of Health Sciences, Karachi, Pakistan
2Ozarks Medical Center, Missouri, USA
3Liaquat National Hospital and Medical College, Karachi, Pakistan
*Corresponding Author: Muhammad Sohaib Asghar, Dow University Hospital, Dow University of Health Sciences, Karachi, Pakistan
Received: 08 March 2020; Accepted: 20 March 2020; Published: 27 March 2020
Citation:
Muhammad Sohaib Asghar, Abubakar Tauseef, Muhammad Sohaib Qamar, Saad Aslam, Mohammed Akram, Basmah Fayaz, Uzma Rasheed, Maryam Zafar, Gul Muhammad Memon, Iftekhar Ahmed. Nailfold Changes as a Sign of Underlying Systemic Illnesses. Fortune Journal of Rheumatology 2 (2020): 042-060.
View / Download Pdf Share at FacebookAbstract
This review article summarizes nail fold changes witnessed in local as well as systemic diseases and differentiation among these diseases according to the occurrence of particular nail fold manifestation and examination. Raynaud’s phenomenon is the main clinical manifestation encountered and capillaroscopy is used to examine nail bed changes found in capillary loops. Data prevailing within this review article is obtained by utilization of PubMed search engine and terminologies like nail fold, nail fold changes, paronychia, leukonychia, Raynaud's phenomenon, and onycholysis are used as Mesh Major Topic. A total of 14 papers of review articles were reviewed from 1983 till 2019. Data is entered in tabulated form in order to define the type of study and highlight the outcome. This review article based on nail fold changes as a clinical finding of numerous local and systemic illnesses is of great help to physicians and provides an important clue in the care of the patient if not neglected. This review article enlightens us with precise information and knowledge about nail changes in the form of shape, color and appearance to distinguish one disease from another and further simplifying the workup and treatment modalities opted for diseases.
Keywords
Review, Nailfold, Capillary, Systemic, Raynaud’s
Review articles, Nailfold articles, Capillary articles, Systemic articles
Review articles Review Research articles Review review articles Review PubMed articles Review PubMed Central articles Review 2023 articles Review 2024 articles Review Scopus articles Review impact factor journals Review Scopus journals Review PubMed journals Review medical journals Review free journals Review best journals Review top journals Review free medical journals Review famous journals Review Google Scholar indexed journals Nailfold articles Nailfold Research articles Nailfold review articles Nailfold PubMed articles Nailfold PubMed Central articles Nailfold 2023 articles Nailfold 2024 articles Nailfold Scopus articles Nailfold impact factor journals Nailfold Scopus journals Nailfold PubMed journals Nailfold medical journals Nailfold free journals Nailfold best journals Nailfold top journals Nailfold free medical journals Nailfold famous journals Nailfold Google Scholar indexed journals Capillary articles Capillary Research articles Capillary review articles Capillary PubMed articles Capillary PubMed Central articles Capillary 2023 articles Capillary 2024 articles Capillary Scopus articles Capillary impact factor journals Capillary Scopus journals Capillary PubMed journals Capillary medical journals Capillary free journals Capillary best journals Capillary top journals Capillary free medical journals Capillary famous journals Capillary Google Scholar indexed journals Systemic articles Systemic Research articles Systemic review articles Systemic PubMed articles Systemic PubMed Central articles Systemic 2023 articles Systemic 2024 articles Systemic Scopus articles Systemic impact factor journals Systemic Scopus journals Systemic PubMed journals Systemic medical journals Systemic free journals Systemic best journals Systemic top journals Systemic free medical journals Systemic famous journals Systemic Google Scholar indexed journals Raynaud’s articles Raynaud’s Research articles Raynaud’s review articles Raynaud’s PubMed articles Raynaud’s PubMed Central articles Raynaud’s 2023 articles Raynaud’s 2024 articles Raynaud’s Scopus articles Raynaud’s impact factor journals Raynaud’s Scopus journals Raynaud’s PubMed journals Raynaud’s medical journals Raynaud’s free journals Raynaud’s best journals Raynaud’s top journals Raynaud’s free medical journals Raynaud’s famous journals Raynaud’s Google Scholar indexed journals capillaroscopy articles capillaroscopy Research articles capillaroscopy review articles capillaroscopy PubMed articles capillaroscopy PubMed Central articles capillaroscopy 2023 articles capillaroscopy 2024 articles capillaroscopy Scopus articles capillaroscopy impact factor journals capillaroscopy Scopus journals capillaroscopy PubMed journals capillaroscopy medical journals capillaroscopy free journals capillaroscopy best journals capillaroscopy top journals capillaroscopy free medical journals capillaroscopy famous journals capillaroscopy Google Scholar indexed journals capillary loops articles capillary loops Research articles capillary loops review articles capillary loops PubMed articles capillary loops PubMed Central articles capillary loops 2023 articles capillary loops 2024 articles capillary loops Scopus articles capillary loops impact factor journals capillary loops Scopus journals capillary loops PubMed journals capillary loops medical journals capillary loops free journals capillary loops best journals capillary loops top journals capillary loops free medical journals capillary loops famous journals capillary loops Google Scholar indexed journals onycholysis articles onycholysis Research articles onycholysis review articles onycholysis PubMed articles onycholysis PubMed Central articles onycholysis 2023 articles onycholysis 2024 articles onycholysis Scopus articles onycholysis impact factor journals onycholysis Scopus journals onycholysis PubMed journals onycholysis medical journals onycholysis free journals onycholysis best journals onycholysis top journals onycholysis free medical journals onycholysis famous journals onycholysis Google Scholar indexed journals terminologies articles terminologies Research articles terminologies review articles terminologies PubMed articles terminologies PubMed Central articles terminologies 2023 articles terminologies 2024 articles terminologies Scopus articles terminologies impact factor journals terminologies Scopus journals terminologies PubMed journals terminologies medical journals terminologies free journals terminologies best journals terminologies top journals terminologies free medical journals terminologies famous journals terminologies Google Scholar indexed journals leukonychia articles leukonychia Research articles leukonychia review articles leukonychia PubMed articles leukonychia PubMed Central articles leukonychia 2023 articles leukonychia 2024 articles leukonychia Scopus articles leukonychia impact factor journals leukonychia Scopus journals leukonychia PubMed journals leukonychia medical journals leukonychia free journals leukonychia best journals leukonychia top journals leukonychia free medical journals leukonychia famous journals leukonychia Google Scholar indexed journals
Article Details
1. Introduction
Nailfold changes have been observed in many systemic diseases affecting the multiorgan system or a single organ. Nailfold examination assists in distinguishing different systemic diseases as well. Different procedures have been introduced in recent years that help us identify skin changes as well as capillary changes. Nailfold and nail bed abnormalities have been noted and described in the literature pertaining to different systemic diseases that may be associated with or without the presence of connective tissue disease. Raynaud’s phenomenon is one of many clinical findings observed and capillaroscopy is performed to see nailbed changes in capillary loops which will be described in this article as well.
1.1 Objectives
The objective of this study is to summarize nail fold findings found in different diseases that either have a localized pattern or their systemic involvement and their manifestations affecting nail fold in a particular pattern indicating the degree of disease activity.
2. Methods
Data mining for this review article was done using the PubMed search engine using similar medical terms for Nailfold changes as a sign of underlying systemic illnesses. Our review aimed to describe nailfold changes and its findings in different underlying systemic diseases which may point towards it. We also used terms such as “nailfold, nailfold changes, paronychia, leukonychia, Raynaud’s phenomenon, onycholysis” as Mesh Major Topic. A total of 14 papers were selected and went through by four independent reviewers. All of these papers were reviewed thoroughly by each individual reviewer. The papers included were from 1983 till 2019. The information gathered from each publication was systematically arranged in ascending order of the year of publication and information was extracted to be included in our review. A tabulated form of arrangement was done in order to rectify the type of study and the outcome of it and if any device was employed as well. The final outcome of the study was also included in the table for ease of understanding of outcomes.
|
S.No. |
Author |
Topic |
Outcome/Conclusion |
|
1. |
Spencer-Green G, et al. [1] |
Nailfold capillary changes in pediatric rheumatic conditions. |
Compared Dermatomyositis, Scleroderma, MCTD, Juvenile RA for nailfold capillary abnormalities. |
|
2. |
Thompson, et al. [2] |
Findings in Scleroderma and associated syndromes of Nailfold Biopsy. |
There was a correlation with decrease capillary count and severity of the disease. |
|
3. |
Fawset S, et al. [3] |
Nailfold abnormalities as a clue for systemic diseases. |
Many nail abnormalities can help in the workup of underlying diseases. |
|
4. |
Park JW, et al. [4] |
Response of tadalafil in cutaneous microcirculatory function with patients of coronary artery disease and erectile dysfunction. |
Tadalafil was used in 20 patients with co-occuring CAD and ED. It did improved ED patients with cardiovascular risk with respect to the endothelial function but patients reported successful sexual intercourse in the 48 hour period per single dose. Its function could be assessed by nailfold capillaroscopy by measuring DpH and vRBC. |
|
5. |
Nicole Fett, et al. [5] |
Update of Morphea. |
Generalized morphea is differentiated from systemic sclerosis where patients may develop sclerosis of the fingers, but typically don’t exhibit ulcerations, phalanx resorption, changes in capillaries of the nail fold or Raynaud's phenomenon, all of which happens in systemic sclerosis. |
|
6. |
Slavica Pavlov-Dolijanovic, et al. [6] |
Primary Raynaud's Phenomenon associated with nailfold capillary changes in Scleroderma pattern. |
The sensitivity and specificity of Scleroderma type of nailfold capillary modifications were greater in primary Raynaud's phenomenon developing systemic sclerosis than those with other connective tissue diseases. |
|
7. |
Darryn Rennie, et al. [7] |
Nailfold Dermatoscopy in General Practise. |
Nailfold dermatoscopy approach considers Morphology, Diameter, Architecture, and Density. Dermatoscopes are useful devices helping in examining nailfold capillaries. |
|
8. |
Mahnaz Etehad Tavakol, et al. [8] |
Use of Nailfold capillaroscopy in Rheumatology. |
Scleroderma spectrum disorders should be evaluated with nailfold capillaroscopy which is quite inexpensive and non-invasive. |
|
9. |
Violeta Higuera, et al. [9] |
Nailfold changes associated with Systemic Lupus Erythematosus. |
The presence of Nail Dystrophy and related organ damage were compared in this study. It was found that the presence of nail dystrophy increases the likelihood of organ/microvascular damage. |
|
10. |
Ines Poveda-Montoyo, et al. [10] |
A case report of retronychia/ paronychia |
Two cases of retronychia managed with nail avulsion resulting in complete resolution of symptoms, also that there was no recurrence of paronychia. |
|
11. |
Samad Ghaffari, et al. [11] |
Koilonychia in Iron- Deficiency Anemia |
A case report of a 57-year old woman with a complaint of intermittent hemorrhoidal bleeding for 7 years, and showing koilonychia. Oral supplementation of iron improved the overall fatigue but didn’t affect nail changes. |
|
12. |
Chi-Feng Yen, et al. [12] |
Use of nail braces in severe paronychia caused by Epidermal growth factor inhibitors . |
Epidermal Growth Factor inhibitors are known to cause severe paronychia. The condition is often treated with surgical. Nail brace was used the patient was on afatinib during the entire period with resolution of paronychia. |
|
13. |
Fabiana M Damasco, et al. [13] |
Nailfold abnormalities in Sezary Syndrome. |
The nail changes outlined above were compatible with the preceding literature. Onychauxis, anonychia, distal notching, and onychoschizia were the most specific nail changes in SzS. |
|
14. |
Maurizio Cutolo, et al. [14] |
Nailfold capillaroscopy and its careful use in rheumatic diseases. |
Standardization of assessment of the morphology of single capillaroscopic shapes has been followed up by a unanimous multicenter algorithm by the EULAR SG-MC in rheumatic diseases, also defined a simple way make it easier for inexperienced and proficient capillaroscopists to identify them. |
Table 1: Review of Articles.
2.1 George Spencer Green, et al. [1]
This study [1] included 118 pediatric patients, 34 normal subjects (15 males and 19 females) which served as controls in this study for the purpose of comparing, while 84 patients were divided into groups pertaining to their connective tissue diseases. The conditions which existed in the patients were used as study groups and were children with Childhood Dermatomyositis (21 Females, 11 Males), Juvenile Rheumatoid Arthritis (16 Females, 6 Males), Scleroderma (19 patients, further subdivided into 9 with systemic disease and 10 with localized disease), Mixed Connective Tissue Disease (3 Females, 1 Male), and Systemic Lupus Erythematosus (7 females).
Nailfold capillaroscopy was done in these patients and its findings were correlated with localized or systemic disease. A normal capillaroscopy was identified with uniformity in the appearance and corresponding distribution of the capillary loops. A dropout of the capillary vascular bed, avascularity, nonuniform appearance, tortuous, arborized capillary loop clusters were abnormally found. Out of the 118 subjects which included controls and patients both, 29 showed Nailfold capillary abnormalities which were found solely in subjects with dermatomyositis and scleroderma.
Patients with scleroderma and dermatomyositis revealed similar morphological capillary nailfold abnormalities. The capillary pattern alone could not serve as a foundation for the distinction between the two conditions. However, dermatomyositis was seen to have highly arborized capillary loop clusters more frequently, although one patient was noted to have them in scleroderma. Biopsy specimens of Twenty-Five patients with dermatomyositis were available which correlated with nailfold capillary abnormalities, showing extensive loss of capillary bed and non-necrotizing vasculitis along with abnormal nailfold pattern. Out of 32 patients with dermatomyositis, 20 exhibited dilation and/or drop out of nailfold capillary loops. 7 of the 20 patients had arborized capillary loop clusters that were highly tortuous. Patients with Localized scleroderma surprisingly didn’t have capillary findings neither their affected skin exhibited any changes. The 9 subjects with systemic disease all displayed nailfold capillary abnormalities. Capillary dropout and dilatation were seen around the edge of the skin lesions in 3 subjects with skin ulcers and systemic sclerosis.
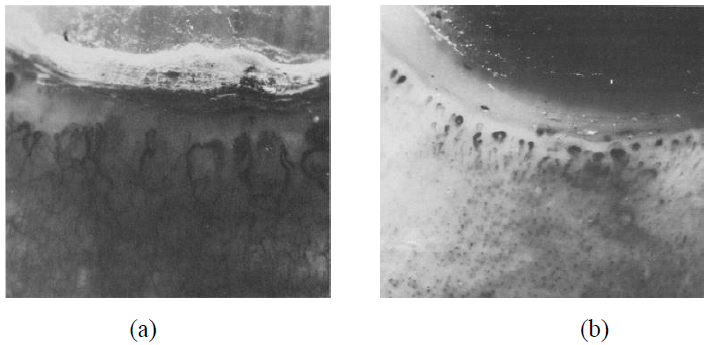
Figure 1: (a) Abnormal nailfold pattern with dilated loops, arborization of dilated capillary loops (systemic sclerosis); (b) Abnormal nailfold pattern with distinct population and redundancy, giving the appearance of neovascularization (dermatomyositis).
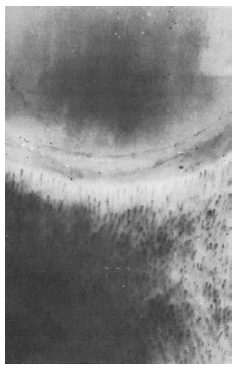
Figure 2: Normal nailfold pattern with homogenous distribution and uniform appearance of loops (normal control).
2.2 Thompson, et al. [2]
This research [2] included 15 patients: 9 of whom were diagnosed with scleroderma (systemic sclerosis) according to the major criteria of the American rheumatism association, and 6 patients with closely related disorders: 2 with CREST syndrome and UTCD (Undifferentiated connective tissue disease). The chosen patients served with a range of varying degrees of different skin and visceral organ involvement seen in the scleroderma variety of syndromes. The duration of ailment in these patients oscillated from 3 months to 9 years. A control group was made by acquiring biopsies from 9 healthy volunteers. The histological inspection unveiled the presence of many eosinophilic, PAS-positive amorphous, unshapely globules in the nail cuticles of all patients but one. Patient biopsies displayed endothelial inflammation and growth with thickening of the basement membrane occasionally. Capillary dilatation with thinning of the basement membrane was present a lot more frequently in the apical papillae. Well distributed PAS staining in the ground substance of apical dermis was prominent in several biopsies coming across more evidently in those patients with extensive cuticle deposits. Nailfold photomicrographs showed that capillary count corresponded with the capillary loss sections. Mast cells found in close proximity to small vessels were effortlessly recognized by their PAS-positive stained granules and were twice as rampant in the control group than in the patient group. Interstitial fibroblasts in the patients were scarce in comparison to those identified in the control group. Capillary damage was well associated with cuticular deposits which seem to comprise mainly of plasma proteins signifying increased capillary permeability or frank hemorrhage. There seems to be a correlation with decrease capillary count and severity of the disease. Two patients reportedly died two months after biopsy specimens were taken, they had the lowest capillary counts of all.
2.3 Fawcett M.D, et al. [3]
There are many nail abnormalities reported in this study [3] that can help in the workup of underlying diseases. Nail findings can be growth-related or change in color of the nail. We are reporting a few findings from the paper; Clubbing (seen in Inflammatory bowel disease, COPD, lung cancer, chronic bronchitis, arteriovenous fistula, congenital cyanotic heart disease, subacute bacterial endocarditis), Pitting (Psoriasis, alopecia areata, eczema, Reiter’s syndrome), Beau’s lines (Raynaud’s disease, syphilis, hypoparathyroidism, pemphigus, trauma), Yellow Nail (Lymphedema, pleural effusion, immunodeficiency syndromes, rheumatoid arthritis, bronchiectasis, sinusitis), Onycholysis (Psoriasis, Onychomycosis and other infectious entities, hyperthyroidism, sarcoidosis, amyloidosis), Terry’s nails (Liver insufficiency, cirrhosis, diabetes mellitus, congestive heart failure, hyperthyroidism, malnutrition), Azure lunula (Wilson’s disease, silver poisoning, excessive Fluoride consumption, quinacrine therapy), Half-and-Half Nails (Chronic renal failure), Muehrcke’s lines (hypoalbuminemia), and Mees’ lines (Arsenic poisoning, Hodgkin’s disease, leprosy, malaria, Carbon Monoxide poisoning).
2.4 J-W Park, et al. [4]
Nailfold capillary microscopy has been employed to determine the efficacy of using tadalafil (a phosphodiesterase inhibitor) in patients with co-occurrence of Coronary Artery Disease and Erectile Dysfunction [4]. The function and impact of tadalafil were evaluated by the International Index of Erectile Function (IIEF). The velocity of RBC at rest and after 3 minutes of ischemia was substantially decreased in patients with CAD and ED when equaled with the age-matched control group. To judge the duration of post-ischemic hyperemia, which is a measure for vascular reactivity, a blood pressure cuff was adorned and inflated to 300 mmHg on the upper arm for 3 minutes. DpH is specified as the time interlude between the unloosening of the bloodstream and the re-establishment of baseline values for the rest of the erythrocytic velocity in carefully chosen capillaries of the nailfold. Among 20 patients who responded to TAD 10 patients had productive sexual intercourse during the 48 hr period after taking 20mg tadalafil. Among these 10 patients, six patients had intercourse twice, three patients had it thrice and one patient had it four times.
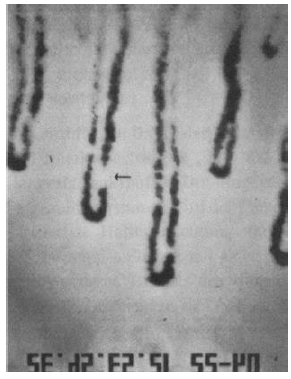
Figure 3: Arrow pointing towards capillaries having a plasma gap.
Penis has microvessels more than 10 to 20 folds as compared to vasculature around nailfold capillaries. Monitoring nailfold capillary vasculature can help identify the probability of changes to occur in the penile vasculature. Nailfold capillaroscopy is an inexpensive and noninvasive tool that can predict the microvascular effect of tadalafil in patients with concomitant ED and CAD.
2.5 Nicole Fett, et al. [5]
Morphea is a rare, inflammatory, fibrosing skin condition that results in the sclerosis of the dermis and subcutaneous tissue but could also extend to the fascia, muscle, and bone. The pathogenesis of morphea remains inadequately analyzed and is probably multifactorial; genetic predilection, immune dysregulation, and environmental influences have all been implicated in the process. Morphea is also known as localized scleroderma because on clinical examination, morphea has an irregular dispersal of lesions and is usually restricted to one body area. Generalized morphea is differentiated from systemic sclerosis where patients may develop sclerosis of the fingers, but typically don’t exhibit ulcerations, phalanx resorption, changes in capillaries of the nail fold or Raynaud's phenomenon, all of which happens in systemic sclerosis. The face is usually exempted. Furthermore, the existence of flexion contractures of the joints and muscle-joint indicators are common. Morphea and systemic sclerosis have overlapping aspects with graft versus host disease (GVHD), both histologically and clinically.
2.6 Slavika Pavlov-Dolijanovic, et al. [6]
This was a prospective study of 10 years in which 3,029 patients diagnosed with Primary Raynaud’s Phenomenon (in accordant with the criteria proposed by LeRoy and Medsger) were registered [6]. At the primary visit, all patients had symmetric occurrences verified as color changes in the hand and/or foot digits as a reaction to cold stimuli or emotional stress; standard erythrocyte sedimentation rate; ordinary appearing nailfold capillaries; negative test for antinuclear antibody; absence of tissue necrosis or gangrene, and lack of a supplemental, underlying cause for the phenomenon to be explained based on the patient’s history and general physical examination. Enlisted patients had consistent follow-up visits every 6 months. Nailfold capillaroscopy alterations in patients with primary raynaud’s phenomenon were not perceived at the commencement of the study. After successive nailfold capillaroscopy at regular 6-month intervals, results were recorded as normal, nonspecific, or scleroderma-like. In patients with Raynaud’s phenomenon developing Systemic sclerosis, the sensitivity (94%) and the specificity (92%) of SD type of nailfold capillary modifications were greater than those in the other connective tissue diseases.
2.7 Rennie, et al. [7]
Raynaud phenomenon is described as reduced blood flow and transient vasoconstriction of the arteries and arterioles of the digits in response to emotional strain or cold temperatures which presents as an alteration of the skin color of the affected area [7]. Raynaud’s phenomena characteristically involve the fingers and start with a single digit and then extend to other digits proportionally on both hands. The thumb is usually spared. An attack generally follows a pattern of three stages: first, is skin pallor as the fingers show a demarcated white area, followed by cyanotic skin changes which are observed to be blue in color; followed by erythematous changes due to vascular reperfusion (reactive hyperemia). Primary Raynaud's phenomenon and second Raynaud's phenomenon (linked with connective tissue diseases) can be differentiated with the aid of nailfold capillary examination.
The article delivers an outline of the utility of nailfold capillary dermatoscopy in various diseases and features the MDAD (morphology, diameter, architecture, and density) methodology of nailfold dermatoscopy (Figure 4). Dermatoscopes are useful devices in examining nailfold capillaries. The average nailfold capillary density is seven per millimeter, and the pattern of distribution and coil-shaped morphology can be appreciated on nailfold capillaroscopy. The presence of hemorrhage and avascular areas with engorged loops or without capillary loops can be observed. Capillaries can be seen with dermatoscopes that are polarised and non-polarised. A thorough history including questions about pertinent symptoms of an underlying disease, occupational use of tools, smoking and medications should be prudently taken. The examination must be concentrated on fingers, joints, skin, and nailfold examination with dermatoscope. Laboratory results of ANA (anti-nuclear antibody) assist in diagnosing an underlying connective tissue disorder. Patients with Systemic Sclerosis, Polymyositis, dermatomyositis, and other connective diseases develop Raynaud’s phenomenon accompanied by nailfold capillary abnormalities.
Midst Non-rheumatic diseases, Cardiac syndrome X comprises of angina, exertional ischemic ST-segment irregularities and normal coronary arteries on angiogram; dermatoscopy in these patients revealed morphological changes comparable to systemic inflammatory diseases. A study reportedly found the presence of capillary changes in 91% of known cases of Primary Biliary Cirrhosis and 54% in systemic sclerosis.
2.8 Mahnaz Etehad Tavakol, et al. [8]
Patients with Raynaud’s phenomenon have been prompted for capillaroscopic studies under the suspicion of microcirculation defect [8]. Nailfold capillaroscopy has been proven vital especially in the timely diagnosis of systemic sclerosis and it is also used as a classification criterion. The chief benefit of capillaroscopy as seen by many rheumatologists lies in the recognition of microvascular nailfold variations that can arise in some inflammatory connective tissue diseases. Capillaroscope and autoantibodies together are acknowledged as an effective instrument in identifying developing Connective tissue Diseases in patients with Raynaud’s phenomenon. Parameters such as ANA, amount of capillaries and the presence of enlarged capillaries have been established in a system named PRINCESS (Prognostic Rule-Based Instructions using Nailfold Capillaroscopy Examination and Scleroderma-Related Serology). This has been used for a collection of Scleroderma-spectrum disorders which provides support in discriminating between Primary and Secondary Raynaud’s Phenomenon. Changes are also observed in CTDs such as MCTDs, overlap syndromes, dermatomyositis, and polymyositis.
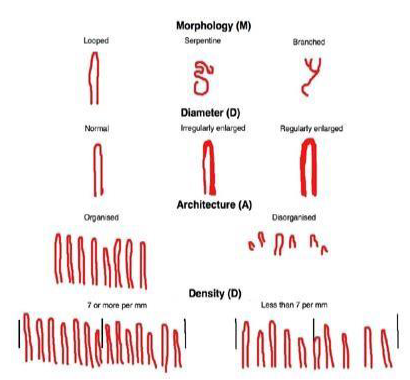
Figure 4: The MDAD approach to nailfold dermatoscopy.
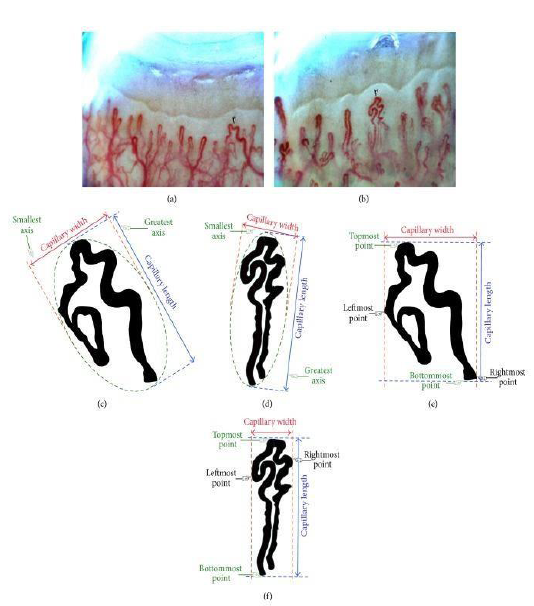
Figure 5: (a, b) Two different images acquired by a digital capillaroscope with 200x magnification from two young healthy females to extract the features of capillaries marked with arrows; (c, d) Automated measuring of capillary width and height (PCA method); (e, f) Manual measuring of capillary width and height.
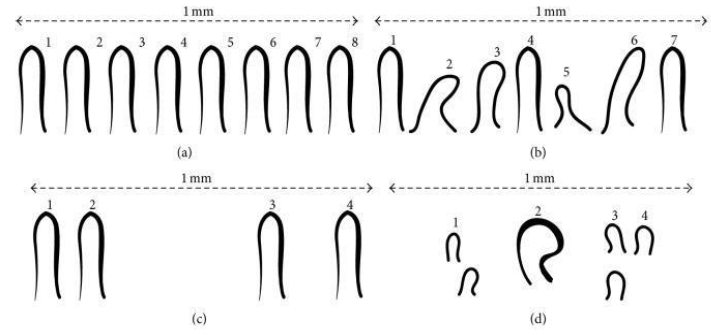
Figure 6: Distribution of capillary per mm; (a) normal capillary arrangement, (b) capillary disarrangement (c) avascular areas (a local paucity); (d) an enlarged capillary and avascular areas.
2.9 Violeta Higuera, et al. [9]
In this cross-sectional study of SLE patients [9], individuals were assigned in groups, according to the existence or nonexistence of nail dystrophy. The patients involved all fulfilled the 1982 American College of Rheumatology (ACR) reviewed criteria for the grouping of SLE and appeared at the Rheumatology department at the Instituto Nacional de Cardiologia Ignacio Chavez in Mexico City, between April 2012 and December 2012. Initially, 63 patients had been enrolled in the study but two patients were omitted because of the presence of culture-proven onychomycosis; Trichophyton species was isolated in both cases. Fifty (82%) of the 61 remaining patients were female. Complete history and examination were done with baseline laboratory tests along with ANA, anti-dsDNA, Antiextractable nuclear antigen antibodies (including anti-SSA/Ro, anti-SSB/La, anti-Sm, and anti-U1 RNP) Anticardiolipin antibodies, and anti-β2 glycoprotein I antibodies was measured by ELISA. The plasma concentrations of ET-1 were measured by a quantitative ELISA. The most frequent nail changes found in the 32 patients with ND were onycholysis, reported in 13 patients and longitudinal ridging, observed in 8 patients. Other changes were yellow nails, leukonychia, longitudinal pigmented bands, and periungual erythema. Nail abnormalities were present in several nails. Patients with Nail dystrophy also had organ damage and skin damage was reported than in patients with ND (Figure 7). SLICC/ACR index was used with values of 0.5 (median) where O=minimum and 6=max. Skin ulceration, scarring chronic alopecia was also found. Capillaroscopy changes were observed in both ND and ND groups.
2.10 Ines Poveda-Montoyo, et al. [10]
Retronychia is a chronic paronychia caused by the nail embedding into the proximal nailfold, and typically impacts the big toe one-sidedly. It often goes undiagnosed clinically and is confused for classical paronychia which can lead to needless long-term treatment with oral antibiotics. This article is a case report where 2 cases have been reported of a 14 and 16-year old girl [10] (Figure 8 and 9). Both cases had a chronic history of pain, erythema, and tenderness of the proximal nailfold suggesting paronychia. They both were treated with oral and topical antibiotics. X-ray and ultrasound evaluations revealed a radiolucent image of the first phalange and soft tissue inflammation suggesting osteomyelitis of the 14-year old. The patient was admitted in the hospital and given cefazolin intravenously. Blood tests and cultures were negative but skin culture exposed the presence of Pseudomonas Aeruginosa. Cefazolin was withdrawn and ciprofloxacin was started. It did not improve the condition. Then nail avulsion was performed under anesthesia. An underlying nail plate was apparent in the proximal nailfold of the affected left great toe. Similarly, the 16-year old had a much more prolonged history of 6 months of the pain of both great toes as well as conspicuous signs of inflammation with unremarkable exudate in proximal nailfolds with yellowish discoloration and distal onycholysis. No bone involvement was found on Xray but skin culture came back positive for penicillin-resistant Staphylococcus lugdunensis and Corynebacterium striatum. Treatment with oral ciprofloxacin was acquainted, to no avail. Retronychia is usually misdiagnosed as paronychia on a clinical exam. It causes aggravation of symptoms and prolonged antibiotic failure extends its diagnosis. Retronychia has been reported in adolescents but very rarely in children with a mean age of diagnosis of around 25, predominantly found in young females.
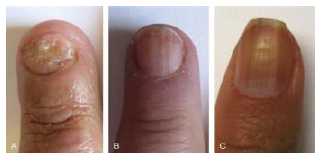
Figure 7: Nail Dystrophy in 3 patients with SLE: Onycholysis (A) Longitudinal Ridging; (B) and Longitudinal Pigmented Bands (C).
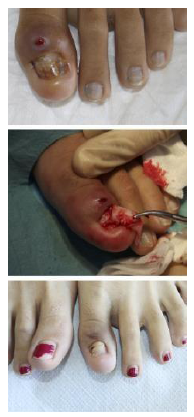
Figure 8: (A) The patient presented with a history of chronic proximal paronychia affecting the left first toe; an attempt to drain the lesions had been performed but failed; (B) During avulsion of the nail plate, the proximal nail fold growth has been observed; (C) One and a half months after surgery, the patient remained asymptomatic, with new nail plate regrowth.
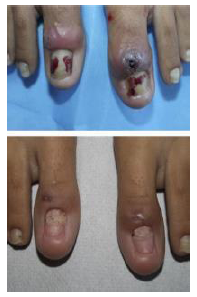
Figure 9: (A) Both great toes showing prominent inflammatory signs in the proximal nail fold; (B) One and a half months after surgery, the nail plate of both great toes, regrown.
2.11 Samad Ghaffari, et al. [11]
A case report of a 57-year old woman with a complaint of intermittent hemorrhoidal bleeding for 7 years [11] (Figure 10). She appeared pale with koilonychia on second, third fingers and thumbs of both hands. Her lab evaluation revealed Hemoglobin of 7.8 g/dL a decreased MCV of 66fl, a platelet count of five hundred and fifty thousand. Her Iron profile revealed a decreased serum iron level of 23 microgram/dL, a ferritin level of 3 nanogram/mL and a total iron-binding capacity of 270 microgram/dL. Upper Gastrointestinal endoscopy was unremarkable while colonoscopy was unremarkable too except for the presence of hemorrhoids which was the cause of bleeding. Hemorrhoids do not normally cause this significant bleeding that would lead to this degree of anemia. Stool tests for ova, parasites, celiac disease were also negative. This finding of hemorrhoids leading to anemia is a rare finding. Koilonychia usually occurs in the first 3 digits. The patient was treated with oral iron supplementation and followed at the 3-month interval where her Hemoglobin improved and was found out to be 11.2g/dL and her fatigue had lessened however her nails appeared unchanged.
2.12 Chi-Feng Yen, et al. [12]
In patients with severe EGFR inhibitor-induced paronychia a noninvasive substitute to nail extraction is displayed in this paper [12] (Figure 11). Patients’ quality of life and acquiescence can be improved by nail braces, and inappropriate dose cutbacks can be avoided. Severe paronychia is usually brought on by epidermal growth factor receptor inhibitors which frequently need surgical extraction or reducing the doses or discontinuation of EGFR inhibitors which can lead to post-extraction septicity, bleeding and damage of adjoining tissue. A new alternative has been described here. Nail braces were secured at the nail edges to decrease the compression of the arch with adjustments in every 8 weeks. This resulted in immediate pain relief and eliminated pyogenic lesions that were present. It did not require lowering the dose of afatinib before or after the procedure and it resulted in complete resolution with no recurrence of paronychia following subsequent year.
2.13 Fabiana M. Damasco, et al. [13]
Onychodystrophies related with Sézary syndrome (SzS) have hardly ever been defined in the literature. Cutaneous T-cell lymphoma (CTCL) encompasses a group of extranodal non-Hodgkin lymphomas. Mycosis fungoides (MF) and Sézary syndrome are the most prevalent types of CTCL. SzS is an uncommon and destructive type, which is mostly characterized by exfoliating erythroderma often with extreme pruritus, global lymphadenopathy, and leukocytic count of Sézary cells in the blood. Alopecia, palmoplantar hyperkeratosis and nail deformities are other clinical findings that can be noted. A reflective analysis of SzS patients at an institute was applied and data were compared with prior publications. The medical records and clinical photographs of patients with SzS seen between 1989 and 2017 were studied [13] (Figures 12 and 13). The Nail Psoriasis Severity Index (NAPSI) was put to use for the assessment of how severe the condition of the psoriatic nail was by computing the entire area of contribution in the nail division. Illustrations of the nails of 19 patients of which 9 were males and the rest females were gauged analyzable from the 535 cases which were nominated for the study. Nail changes of varying degrees were appreciable in all patients. Nail manifestations (and percentage of incidence) were as follows:
- paronychia (63.16%)
- leukonychia (42.10%)
- onycholysis (8/19, 42.10%)
- trachyonychia (31.58%)
- subungual hyperkeratosis (26.31%)
- splinter hemorrhages (26.31%)
- onychauxis (26.31%)
- yellow discoloration (21.05%)
- distal yellow-brown discoloration (21.05%)
- distal notching nail (15.79%)
- onychoschizia (15.79%)
- onychomadesis (10.52%)
- longitudinal melanonychia (5.26%)
- anonychia (5.26%).
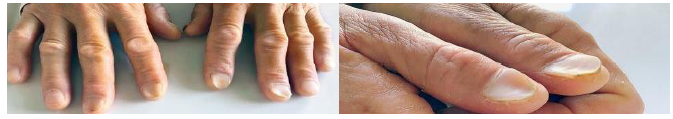
Figure 10: Koilonychia in Iron-Deficiency Anemia.
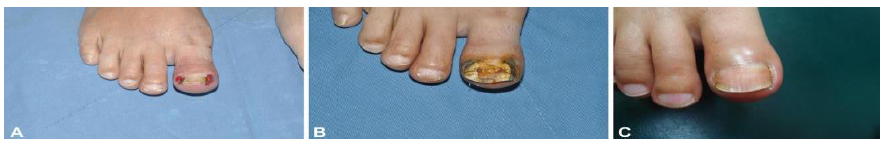
Figure 11: Nail braces for severe paronychia induced by epidermal growth.
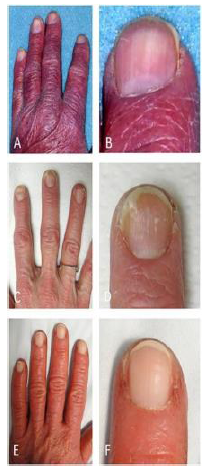
Figure 12: (A, B) (in detail), paronychia, distal yellow-brown discoloration and leukonychia; (C, D) (in detail), onycholysis and (E, F) Onychoschizia trachyonychia.
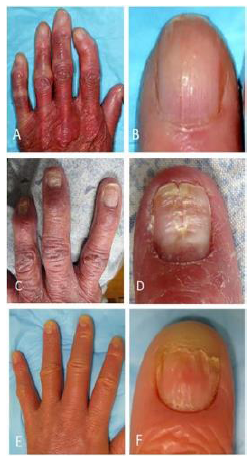
Figure 13: (A, B) Onychauxis; (C, D) Distal Notching; (E, F) (in detail), leukonychia.
The nail changes outlined above were compatible with the preceding literature. Onychauxis, anonychia, distal notching, and onychoschizia were the most specific nail changes in SzS.
2.14 Maurizio Cutolo, et al. [14]
Standardization of assessment of the morphology of single capillaroscopic shapes has been followed up by a unanimous multicenter algorithm by the EULAR SG-MC in rheumatic diseases. The microscopic findings spotted qualitatively by NVC in SSc patients fall into three clearly distinct patterns that deviate from the regular: Early, Active, and the Late. The analysis of the physical changes detected at NVC today is broadly endorsed and programmed systems for obtaining capillary counts are also accessible. Not only have newer studies presented by EULAR agreed to a standard language to label general capillaroscopy and the prevailing capillaroscopic script in a standardized, uniform way, (capillary count [density], dimension, uncharacteristic shapes [morphology], presence/occurrence of hemorrhages) but also defined a simple way to separate scleroderma from non-scleroderma arrays and therefore, made it easier for inexperienced and proficient capillaroscopists to identify them [14].
3. How can this article help clinically?
Nailfold findings articulate a disease process, they may not be considered a significant clue to many physicians and negligence can compromise patient care if not considered earlier on. This article comprehensively provides a review of findings in different systemic, connective tissue diseases. Nailfold capillaroscopy reportedly is a useful tool in identifying the severity and progression of disease activity. A few pictures have been obtained and added here with a description for the purpose of ease of identification.
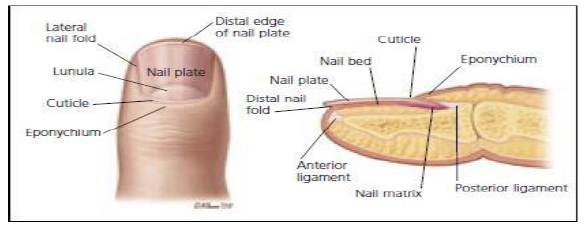
Figure 14: Anatomy of the Nail.
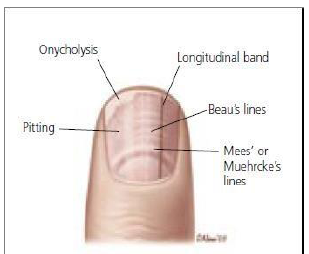
Figure 15: Pathologic Nail Findings associated with underlying diseases.
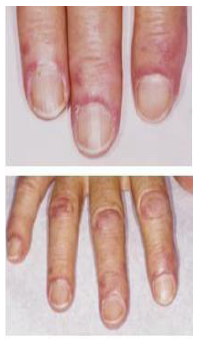
Figure 16: Dermatomyositis (Top). Twisted and dilated capillaries, Just proximal to the cuticle give a blush to the skin of the eponychychium and may signal SLE, Dermatomyositis or scleroderma; (Bottom) The blush and pathognomic finding of Gottron’s papules (i.e., thickened skin over the interphalangeal joints) indicate a diagnosis of dermatomyositis.
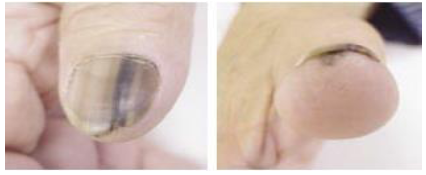
Figure 17: Longitudinal Bands (Left) Common in dark-skinned persons, when these bands are condition accompanied by the pigmentation of underlying skin and disruption of nail growth also results from (right) affected patients should undergo a biopsy to rule out melanoma.
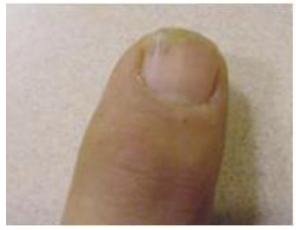
Figure 18: Onycholysis and splinter hemorrhage. This may result from trauma; onycholysis Hyperthyroidism, warts, and onychomycosis.
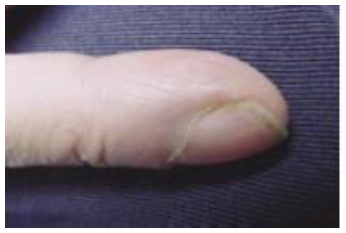
Figure 19: Clubbing. This condition may accompany neoplastic and other lung diseases, atrioventricular malformations, congenital heart disease, celiac disease, and Inflammatory.
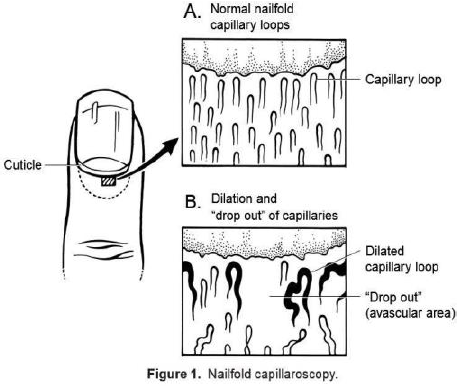
Figure 20: Nailfold capillaroscopy.
These findings are likely consistent with clinically and can be correlated. Terry’s nails, a ground glass appearance white in color which originating from the nail bed can be correlated to cirrhosis in 80% of cases. Similarly, Beau’s lines (transverse linear depressions-trauma, Raynaud’s Disease), Mees’ lines (suggest arsenic poisoning) and Muehrckes lines (indicate Hypoalbuminemia) all have clinical significance and direct patient workup in a certain direction [3]. Dermatoscopy in GP practice should be learned and exercised frequently to assess disease severity by observing the nailfold capillary loop morphology using the MDAD approach [7]. Nailfold capillary abnormalities are also found in autoimmune disease patients such as Primary Biliary Cirrhosis [7]. Capillary Dermatoscopy findings can be assessed and used for its predictability of effectiveness of tadalafil in patients with concomitant CAD and ED. Improved ED and successful sexual intercourse were observed in such patients and nailfold dermatoscopy showed improved blood flow in capillary bed [4]. Nailfold dermatoscopy has a great implication which was never commonly known, while it is a non-invasive and inexpensive testing tool, it helps to predict patient’s disease progression and outcome collectively with laboratory support.
4. Discussion
The reason for this article was to present concise data and knowledge of nail findings and their underlying disease patterns causing those changes which may be a change in growth size or color, its appearance, and change in its shape [4]. These findings help in identifying the disease and help in further directing the workup and treatment [1]. There are many variations of nail findings related to growth and change in color of nails, including onycholysis, clubbing, pitting, yellow nail, Beau's line, Azure lunula, Terry (white) nail, Mees line, Muehrcke’s line and Half and Half nails [3]. Nailfold capillary abnormalities are common in pediatric rheumatic disease, reported with different vascular lesions found in biopsies of childhood dermatomyositis and scleroderma. Similar diseases such as CREST syndrome and UCTD also involve skin, nailfold and visceral lesions correlating with scleroderma [2]. The time interval of suffering from these diseases among patients varied from 3 months to 9 years. Histological findings were suggestive of the presence of abundant PAS-positive amorphous globules in cuticles along with capillary ectasia and decline in capillary count in many patients of scleroderma and similar diseases determining the severity of the disease. There is a striking difference between systemic sclerosis and the clinically rare disease called Morphea on the basis of the absence of Raynauds phenomenon, sclerodactyly, and capillary nailfold variations [5].
Systemic sclerosis and Morphea are similar to graft vs host disease (GVHD). Primary Raynaud's phenomenon exhibits attacks with changes in the color of hand and feet with normal ESR, normal nailfold capillary changes and negative antinuclear antibodies along with no appearances of gangrene and ulcerations. After 6 months of nailfold capillary examinations, outcomes of the patient were normal, scleroderma-like or non-specific [6]. The manifestations of nail dystrophy in SLE include onycholysis, longitudinal ridging, yellow nails, longitudinal pigmented bands, and periungual erythema. The presence of severe nail dystrophy denoted severe organ damage [9]. Nailfold dermatoscopy is utilized in order to differentiate between rheumatic and non-rheumatic skin diseases in parameters of morphology, diameter, architecture, and density (MDAD). This device is used to measure capillary folds. It also helps in differentiating between the primary and secondary types of Raynaud's phenomenon [7].
There are beneficial effects of capillaroscope for examining nail fold for early detection of diseases like Raynaud's phenomenon and systemic sclerosis. It detects microcirculation changes in capillaries and it is widely sighted finding fulfilling the criterion of diseases [8]. Retronychia is a chronic proximal paronychia mostly diagnosed clinically and often confused with paronychia resulting in extended treatment with systemic antibiotics with no beneficial effects of drugs thus resulting in worsening of the condition [10]. Paronychia is induced due to the consumption of epidermal growth factor inhibitors (EGFI) and a substitute for nail extraction in the form of nail braces can eliminate the utilization of nail extraction and provide immediate pain relief and allows the continuation of drugs [12]. Onychodystrophies manifested in Sezary syndrome are estimated by a criterion known as Nail psoriasis severity index (NPSI), which includes paronychia, leukonychia, trachonychia, subungual hyperkeratosis, onycholysis, and yellow nails. Patients can also suffer from intense pruritis, generalized lymphadenopathy, and waxy erythema. The differentiating features of Sezary syndrome from psoriasis are onychauxis, anonychia, distal notching, and onychoschizia [13]. The microvascular changes occurring in nail fold capillaries prove progressive functional and structural changes of nailfold capillaries in autoimmune diseases and systemic sclerosis [11, 14].
5. Conclusion
Our review article is composed of theories, findings, and outcomes obtained from 14 review articles based on nail fold changes involving their appearance, color, size, and shape. Every review article quoted in this article has different outcomes yet they are united in highlighting a single purpose to differentiate local diseases from systemic illnesses with or without damaging connective tissues [15, 16].
References
- Spencer-Green G, Schlesinger M, Bove KE, et al. Nailfold capillary abnormalities in childhood rheumatic diseases. J Pediatr 102 (1983): 341-346.
- Robert PT, Frank EH, John CM, et al. Nailfold Biopsy in Scleroderma and Related Disorders. Arthritis Rheum 27 (1984): 97-103.
- Fawcett S, Hart T, Linford S, et al. Nail Abnormalities: Clues to Systemic Disease. Am Fam Physician 69 (2004): 1417-1424.
- Park JW, Leithauser B, Mrowietz C, et al. Cutaneous microcirculatory function predicts the responsiveness to tadalafil in patients with erectile dysfunction and coronary artery disease. Int J Impot Res 20 (2008): 150-156.
- Fett N, Werth V. Update on Morphea. J Am Academy Dermatology 64 (2011): 217-228.
- Pavlov-Dolijanovic S, Damjanov NS, Stojanovic RM, et al. Scleroderma pattern of nailfold changes as predictive value for the development of a connective tissue disease: a follow-up study of 3,029 patients with primary Raynaud’s phenomenon. Rheumatol Int 32 (2012): 3039-3045.
- Rennie D. Nailfold Dermatoscopy in General Practise. Aust Fam Physician 44 (2015): 809-812.
- Etehad Tavakol M, Fatemi A, Karbalaie A, et al. Nailfold Capillaroscopy in Rheumatic Diseases: Which Parameters should be evaluated. Biomed Res Int (2015): 974530.
- Higuera V, Amezcua-Guerra LM, Montoya H, et al. Association of Nail Dystrophy with Accrued Damage and Capillaroscopic Abnormalities in Systemic Lupus Erythematosis. J Clin Rheumatol 22 (2016): 13-18.
- Poveda-Montoyo I, Vergara-de Caso E, Romero-Pérez D, et al. Retronychia a little known cause of paronychia: A report of two cases in adolescent patients. Pediatr Dermatol 35 (2018): 144-146.
- Ghaffari S, Pourafkari L. Koilonychia in Iron-Deficiency Anemia. N Engl J Med 379 (2018): 13.
- Yen CF, Lee YY. Nail Braces for severe paronychia induced by epidermal growth factor receptor inhibitors: An alternative to nail extraction. J Am Acad Dermato 78 (2018): 89-90.
- Damasco FM, Geskin LJ, Akilov OE. Nail changes in Sezary Syndrome: A single center study and review of the literature. J Cutan Med Surg 23 (2019): 380-387.
- Cutolo M, Paolino S, Smith V. Nailfold capillaroscopy in rheumatology: ready for use daily but with care in terminology. Clin Rheumatol 38 (2019): 2293-2297.
- Karbalaie A, Emrani Z, Fatemi A, et al. Practical issues in assessing nailfold capillaroscopic images: a summary. Clin Rheumatol 38 (2019): 2343-2354.
- Zufferey P, Depairon M, Chamot AM, et al. Prognostic Significance of nailfold capillary microscopy in patients with Raynaud’s phenomenon and scleroderma-pattern abnormalities, A six-year follow-up study. Clin Rheumatol 11 (1992): 536-541.
